Assessing and Improving Children’s Rights in Hospitals: Case Studies from Kyrgyzstan, Tajikistan, and Moldova
Ana Isabel Fernandes Guerreiro, Aigul Kuttumuratova, Kubanychbek Monolbaev, Larisa Boderscova, Zulfiya Pirova, and Martin W. Weber
Health and Human Rights 18/1 PDF
Published June 2016
Abstract
There is a recognized need to raise evidence on how to adopt human rights-based approaches (HRBAs) to health and to assess their impact. In 2013 and 2014, the World Health Organization (WHO) Regional Office for Europe used a set of tools to assess and improve the situation of children’s rights in 11 hospitals in Kyrgyzstan, 10 hospitals in Tajikistan, and 21 hospitals in Moldova, by applying a HRBA to health, taking as a reference the Convention on the Rights of the Child (CRC). The assessment results show a similar situation across countries in some areas, and more or less significant variation in others. Common gaps include the need to improve adolescent-friendly health services, the rights to privacy and play; and infrastructure and equipment. In Kyrgyzstan and Tajikistan, a second round of assessment, was carried out, which showed an effective change in several areas, whilst other areas showed persistent gaps. Moldova did not carry out a second round of assessment. Involving children and parents in the assessment was crucial to obtain more reliable data; the project showed how to use the CRC as a framework to improve quality of care for children (QoC); and the tools were proven useful for self-assessment.
Introduction
The CRC is not merely a legal text; it is a framework for states and professionals working for and with children to guide them on how to enable children to reach their full potential. As such, the CRC should be applied in all of children’s life settings, by all relevant institutions. Fulfilling children’s rights in the health care sector, particularly in hospitals, can be a vehicle to improve children’s experience of health care, to enhance children’s and parents’ involvement in their own care and in the development of services and, importantly, to improve the QoC provided to children. The importance of adopting an HRBA to health was reinforced in the recently adopted WHO European Child and Adolescent Health Strategy 2015–2020.1
In line with its adopted strategies, WHO provides continuous technical support to member states in developing innovative policies and improving QoC. Strengthening child rights in health has become a focus of WHO work in the European region in recent years. In particular, the WHO has applied a set of existing tools for the assessment and improvement of child rights in hospital and integrated the process in ongoing efforts for improving quality of hospital care for children. The adopted set of tools—the Manual and Tools for the assessment and improvement of children’s rights in hospital (2012)—was prepared by the Task Force on Health Promotion for Children and Adolescents in and by Hospitals, a working group of the International Network of Health Promoting Hospitals and Health Services, in collaboration with hospitals and international partners, including WHO.2
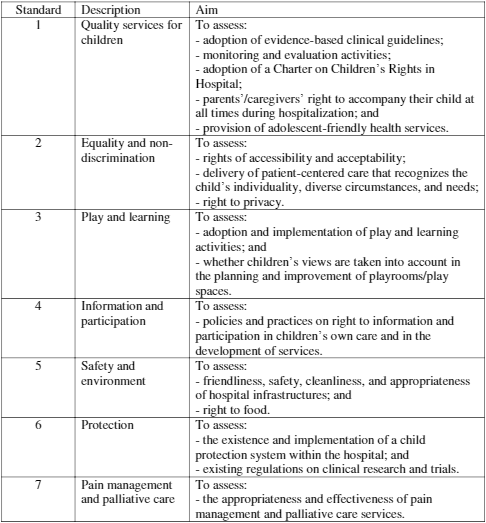
The tools are based on seven standards, which derive from the CRC, charters and working documents, and the findings from an earlier pilot. The standards translate the rights enshrined in the CRC and related dimensions into concrete measures and activities that health professionals and managers can apply in the delivery of healthcare for children (Table 1). The Manual and Tools consists of a guide for assessment and improvement and five assessment tools on children’s rights targeting hospital management, health professionals, parents/caregivers, 12- to 18-year-old children and adolescents, and 6- to 11-year-old children. The first four tools assess the eight standards through 22 sub-standards and approximately 72 measurable items each (statements or questions) for each group of stakeholders. The tool for 6- to 11-year-old children consists of a short questionnaire. A template for focus group discussions with parents/caregivers and 12- to 18-year-old children and adolescents is also provided. The questions are adapted to each group, but they aim to address and collect information on the same issues in order to gather complementary and reliable data.
Table 1. Description and aim of the standards, Manual and Tools for the assessment and improvement of children’s rights in hospitals (2012).
Quality of care: the overall aim of the tools is to assess children’s right to health and related rights as a means to improve QoC delivery (article 24 of the CRC); The tools implement an HRBA to health and address the following elements specifically: 3
Participation: children, parents, health professionals, and managers participate in the assessment of standards and identification of gaps for improvement. Standard 4, on information and participation, assesses children’s participation in their own care and in the design, development, and assessment of services (article 12 of the CRC);
Access: Standard 2, on equality and non-discrimination, assesses the dimensions of access (Article 2 of the CRC);
Accountability: the tools enable to verify the implementation of the national programs and hospital policies in place against actual delivery of care for children; and to facilitate a monitoring and evaluation system of QoC for children;
Capacity building: the tools facilitate awareness raising of stakeholders, both duty-bearers and rights-holders on children’s rights in health.
In 2012, the WHO Regional Office for Europe adopted the Manual and Tools, translated them into Russian, and field-tested them in two Kyrgyzstan hospitals. The tool was used as an external quality assessment in two ways: focus groups with hospital managers, health workers, and parents/caregivers; and individual interviews. This trial showed that the tools cover major aspects of child rights in hospitals and was well accepted by hospital managers, health staff, and parents/caregivers. From the hospital administration’s point of view, the tools helped them to look at child/patient rights in a new way. Based on the field test results, the translated tool was edited, adapted to local terminology, and peer reviewed.
In 2013, WHO facilitated the assessment of children’s rights in hospitals in Kyrgyzstan and Tajikistan. Funded by the Russian Federation, the assessment was done in the framework of a WHO project to support the improvement of QoC for children. The project sought to reduce childhood mortality through strengthening national health systems capacity in improving QoC for common childhood illnesses in first-level referral hospitals. This work was also part of the broader initiative by the WHO/Europe to strengthen children’s rights in health services.
The assessment of the respect of children’s rights in hospitals in Moldova was carried out upon recommendation by WHO/Europe with the aim to strengthen evidence and overall recommendations to the Ministry of Health (MoH) on improving QoC for children in hospitals and, in particular, children’s and parents’/caregivers’ rights. The Manual and Tools were reviewed and translated into Romanian by national QoC and health experts and used for the assessment and improvement of the respect of children’s rights in hospitals.
Methods
First assessment
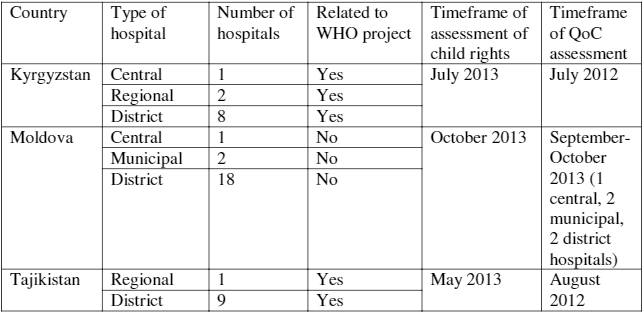
The assessment of children’s rights was conducted in hospitals in three regions of Kyrgyzstan (Thalas, Chiu,and Issyk-Kul); in hospitals in the Khatlon region of Tajikistan; and in hospitals from most districts of Moldova, covering 54% of all country hospitals in Moldova. Hospitals in all three countries were a mix of national, regional, and district hospitals (seeTable 2). Hospitals in Kyrgyzstan and Tajikistan were identified by the Ministries of Health (MoH) as project health facilities covered by the above mentioned WHO project on improving QoC.
Table 2. Hospital characteristics and timeframe.
In Kyrgyzstan and Tajikistan, two national experts were assigned to overall data collection. They travelled to participating hospitals and conducted briefings with respective hospital staff or focal points on the self-assessment process. Prior to this visit, each hospital assigned two staff members to carry out the self-assessment. The number of participants varied according to hospital size and number of patients hospitalized at the time of the study.4
In Moldova, the national focal point was responsible for distributing questionnaires, explaining how to work with them, and presenting the information; this person also conducted data collection. In every hospital, the director was responsible for coordinating the process at the facility level.5
Participants in the three countries included hospital management, doctors and nurses, parents/caregivers, and 6- to 18-year-old children and adolescents. Doctors and nurses represented a variety of departments, including paediatrics, surgery, resuscitation, somatic, infectious diseases, endocrinology, and urology.
In every hospital, group discussions and individual interviews took place. All children were interviewed individually. Some parents/caregivers were interviewed, whilst others participated in group discussions. Once the data collection process was completed, the data were forwarded to the Child and Adolescent Health Program at WHO/Europe for analysis and preparation of a final report.
Patient interviews in all three countries were confidential and prior consent to participation was obtained, in oral form.
Second assessment
Following the first assessment, the hospital managers in Kyrgyzstan and Tajikistan initiated several changes to address identified gaps in child rights. In Tajikistan, the improvement process was also supported by the project steering group, composed of national experts and MoH representatives, whose role was to oversee, support, and monitor implementation of the WHO project on improving paediatric hospital care.
In Kyrgyzstan and Tajikistan, the tools for assessment and improvement of children’s rights in hospital were used to assess improvement results approximately one year after the first assessment. All hospitals that had participated in the first round of assessment also participated in the second round. All participating hospitals in both countries carried out group discussions and individual interviews to assess the respect of children’s rights.
In Moldova, the MoH used the findings and recommendations from the first round of assessment to develop a national plan of actions to improve QoC in paediatric hospitals but did not proceed with a second round of assessment of children’s rights in hospital.
Results
First assessment
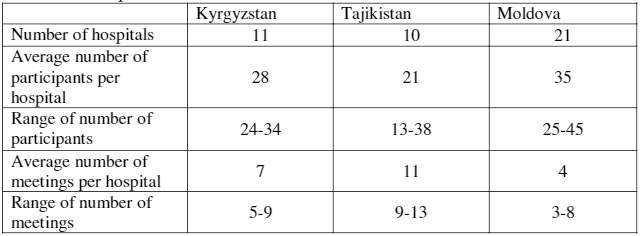
Eleven hospitals in Kyrgyzstan, 10 hospitals in Tajikistan, and 21 hospitals in Moldova participated in the assessment on children’s rights in hospitals. Tajikistan gathered the smallest number of participants per hospital, ranging from 13 in one hospital to 38 in another, but had the highest number of meetings per hospital (average n=11). Moldova collected information from the widest number of stakeholders, ranging from 25 participants in one hospital to 45 participants in another, but had the smallest number of meetings per hospital (average n=4). These results are described in Table 3.
Table 3. Participation in first assessment.
Standard 1: Quality services for children
Next, we present findings by standard in the three countries. The information gathers the inputs from the five groups of stakeholders and provides a specific account of results per sub-standard. Unless otherwise stated, the data in the tables reports information gathered from the different groups of stakeholders.
In the three participating countries, self-evaluation teams in all hospitals stated that care was delivered based on national and international guidelines. In Moldova, the guidelines were developed nationally through ad hoc committees made up of university staff and health professionals, in partnership with the MoH. Subsequently, all hospitals adapted the national protocols to their own context. In Moldova, the main related gap identified by the self-evaluation teams was that some of the national guidelines were not in line with the international ones and thus should be adjusted, based on evidence-based medicine. No gaps were identified in Tajikistan and Kyrgyzstan.
The question posed to parents/caregivers and 12- to 18-year old children and adolescents by the self-evaluation team was, “Do you think you/your child received the best possible care?” All parents/caregivers and children and adolescents in the three countries stated that they were satisfied with the care received.
In terms of training, there were some differences between the participating countries. In Moldova, all medical doctors and nurses working in paediatric care had a specialization in paediatrics; in Kyrgyzstan, in eight hospitals, doctors and nurses working with children were trained in paediatric care; and in Tajikistan, in seven hospitals, doctors were trained in paediatric care and in one hospital the doctors were graduates of paediatrics. Only one of the hospitals in Tajikistan had nurses trained in paediatrics.
Self-evaluation teams in all hospitals in participating countries stated that there were regular monitoring and evaluation activities, including audits and patient satisfaction surveys. In Moldova, relevant statistical data that require continuous improvement was available at the MoH’s website.
The self-evaluation teams identified several main actions for improvement of monitoring and evaluation activities: to establish an effective system for collecting and presenting patient satisfaction surveys (all countries), to promote audits to ensure that health care services are in line with the organizational policy (Kyrgyzstan and Moldova), and to revise the statistical forms and the corresponding set of indicators (Moldova).
At the time of the assessment, Kyrgyzstan was the only country that had adopted, disseminated, and implemented a Charter on Children’s Rights in Hospital. Self-assessment teams in 10 of the 11 participating hospitals stated that a Charter on Children’s Rights in Hospital had been adopted either in 2008 (n=1), in 2009 (n=4), or 2010 (n=5), and that it was displayed in between 30% and 86% of hospital wards. This variation was dependent on the work carried out by each hospital. However, upon further analysis, there is evidence showing that in five participating hospitals, a Charter on Children’s Rights had effectively not been adopted and was not displayed in all wards; in one hospital it was only partially adopted and partially displayed.
Inputs from stakeholders in the three countries demonstrate that there was attention to parents’/caregivers’ right to stay with children during their hospitalization, although with some limitations. In Kyrgyzstan, the self-evaluation teams reported that 10 hospitals allowed parents/caregivers to stay with children during their hospitalization, including overnight stays; and in three hospitals, parents/caregivers were also allowed to stay with their child during procedures, except anaesthesia induction. However, in practice, one hospital only allowed parents/caregivers to stay overnight with children younger than 7, one hospital charged parents/caregivers a fee to stay overnight, and in at least five hospitals, children and parents/caregivers reported that the parent was not allowed to stay overnight, although they wanted to.
In Tajikistan, the limitations were insufficient room and the child’s age. Self-assessment teams in nine hospitals stated that parents/caregivers were allowed to stay with children during procedures, including anaesthesia induction in some hospitals. The feedback from children and parents/caregivers regarding this right was mostly very positive. Six- to 11-year-old and 12- to 18-year-old children and adolescents in nine hospitals reported that their parents had stayed with them and that they felt comfortable when their mother accompanied them at all times.
In Moldova, inputs from the self-evaluation teams showed that parents/caregivers were allowed, in principle, to stay with the child during procedures, including anaesthesia induction in all hospitals. However, no feedback from children, adolescents, or parents was reported, which makes it difficult to assess whether this right was respected effectively.
In the three participating countries, Adolescent-Friendly Health Services (AFHS) were partially implemented: there was a specific AFHS in seven hospitals in Kyrgyzstan, four hospitals in Tajikistan, and 12 hospitals in Moldova. In Tajikistan, two hospitals also had a center for adolescents seeking confidential counseling. There was no additional information provided in the three countries as to what services were included or their effectiveness.
Standard 2: Equality and non-discrimination
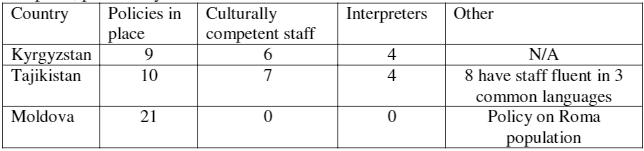
Self-assessment teams in most hospitals in participating countries stated that there were policies and practices in place to ensure that children had the right to access health care services without discrimination. In Moldova, all hospitals had also endorsed and implemented a policy on non-discrimination of the Roma population. Table 4 presents the availability of policies, culturally competent staff—interpreters and other—in the three countries.
Table 4. Availability of culturally competent staff, interpreters, and other, by number of hospitals, per country.
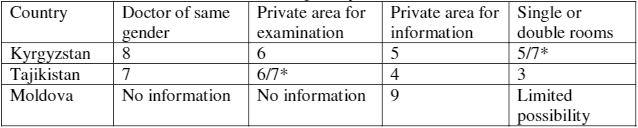
In terms of children’s right to privacy, there were some enabling conditions in the three countries, but more needed to be done. There was a demonstrated need to guarantee that all children are informed privately; this was done in less than half of the hospitals across the countries. Table 5 presents elements on children’s privacy that were assessed in the three countries.
Table 5. Assessed elements on children’s privacy.
*Data provided by self-assessment teams and parents/caregivers and children and adolescents, respectively.
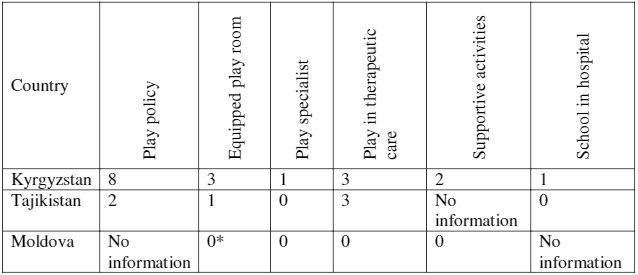
Standard 3: Play and learning
Children’s right to play and learning needed greater attention in all three countries. As shown in Table 6, there are little opportunities for children to play or continue their education while in hospital. There were some positive findings: three hospitals in Kyrgyzstan and Tajikistan had introduced play during therapeutic care (in one hospital in Kyrgyzstan, the play was based on the WHO Integrated Management of Childhood Illness Guidelines); two hospitals in Kyrgyzstan provided supportive activities, such as clown, music, and art therapy; and two hospitals in Kyrgyzstan had consulted with children for the planning and improvement of playrooms and play spaces.
Table 6. Availability of play and learning opportunities in hospitals.
*Eight hospitals had a space where children can play, but there were no properly equipped play rooms.
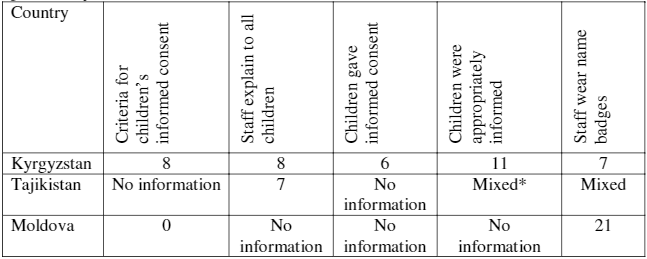
Standard 4: Information and participation
The assessment of children’s right to information and participation provided distinct results in the participating countries. This right received significant attention in Kyrgyzstan and little attention in Moldova; in Tajikistan, there was diversity of policies and practices. Table 7 summarizes the findings on policies and practices on information and participation in the three countries.
Table 7. Policies and practices on information and participation, by number of hospitals, per country.
*“Mixed” refers to the variation of findings within the same hospital, i.e., some children had been informed appropriately and others had not. Note: Columns 1, 2 and 5 are based on inputs from the self-assessment teams, while columns 3 and 4 are based on inputs from parents/caregivers and children and adolescents, with the exception of information related to staff wearing badges in Moldova, which is based on the inputs provided by the assessment teams.
In terms of the engagement of children and adolescents for the development and improvement of health care services, self-assessment teams in Kyrgyzstan and Tajikistan stated that they engaged children and adolescents, who received feedback, in three hospitals each. In Moldova, self-assessment teams in all hospitals stated only that children’s participation either partly or does not influence decision‐making in relation to improvement of health care services.
Standard 5: Safety and environment
The cross-cutting analysis showed a need to improve infrastructure and equipment in all participating countries. In Tajikistan, parents/caregivers called attention to the great need to renovate hospitals, including the need for appropriate facilities such as toilets and more modern equipment. In four hospitals, the self-assessment teams identified the need to allocate a budget to ensure that air conditioning and a functioning sewage system were implemented.
Concerning children’s right to food, the results show significant attention in Kyrgyzstan and Moldova and a need for improvement in Tajikistan. In Kyrgyzstan and Moldova, all participating hospitals provided free food for children. However, food was not available to children of all age groups. In all hospitals in both countries except one in Kyrgyzstan, a nutrition specialist planned the menu. In Kyrgyzstan, the children interviewed in all hospitals stated: “I received free food in a timely manner in the hospital and the food was healthy and tasty.” In Moldova, inputs from the stakeholders also show that food is served punctually in all hospitals. In Tajikistan, free food was provided to children in five hospitals and with limitations, and a nutrition specialist planned the menu in just two hospitals.
The results on the provision of effective cleaning services for children showed a mixed picture across the countries. In Kyrgyzstan, all hospitals ensured effective cleaning services, and children and families were satisfied with the services. In Tajikistan, in nine hospitals, staff are encouraged to follow strict cleaning procedures. In practice, inputs by children and parents/caregivers show a mixed picture. In Moldova, although there seemed to be attention as to ensuring effective and cleaning services, the situation was not uniform and some hospitals were, in fact, lacking sufficient number and adequate toilets, hot water and bathrooms for mothers and children.
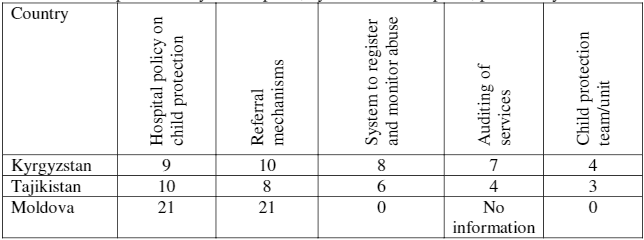
Standard 6: Protection
The assessments show attention to child protection across the three countries, as demonstrated in Table 8. The main gaps include the need to set up child protection teams in hospitals and enhance auditing of services. The assessment also showed a need to train health professionals on a) how to identify and examine children who have been abused, and b) on existing protocols and referral mechanisms. In Kyrgyzstan, health professionals had been trained in three hospitals, and partially trained in another three, on how to identify and examine children who have been abused, and on existing protocols and referral mechanisms based on a handbook. In Tajikistan, health professionals in four hospitals had been trained on existing protocols and referral mechanisms; in Moldova, no professionals were trained. Also in Moldova, self-assessment teams stated that most protection work is done at the primary health care level.
Table 8. Child protection system in place, by number of hospitals, per country.
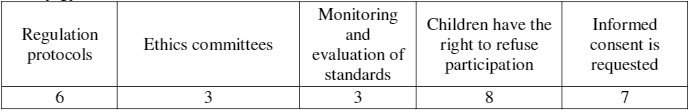
In terms of children’s involvement in clinical research and trials, there are no activities taking place in Tajikistan. In Moldova—as far as it is possible to gather—clinical research is only carried out in two hospitals, and children and families have the option to refuse or not be involved in the teaching activities; one of those hospitals has an ethics committee for clinical research and trials. The findings from Kyrgyzstan are presented in Table 9.
Table 9. System in place for clinical research and trials, by number of hospitals, in Kyrgyzstan.
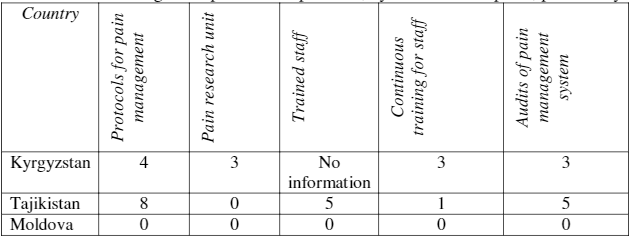
The assessments on the provision of pain management show different situations in the countries, from attention in some hospitals in Kyrgyzstan, to attention in at least half of participating hospitals in Tajikistan and no protocols or other activities in Moldova. In fact, the protocols were being prepared at national level by the MoH at the time of assessment, in Moldova. Table 10 presents the findings in detail.
Standard 7: Pain management and palliative care
In Kyrgyzstan, in most hospitals where children were interviewed,they had been asked by health professionals whether they felt pain and were given medicines for pain relief.
In Tajikistan, children, adolescents and parents/caregivers gave very positive feedback on this right for all hospitals, with very few exceptions. It is also important to mention that children and parents/caregivers valued greatly the attentive and caring staff.
Table 10.Pain management policies and practices, by number of hospitals, per country.
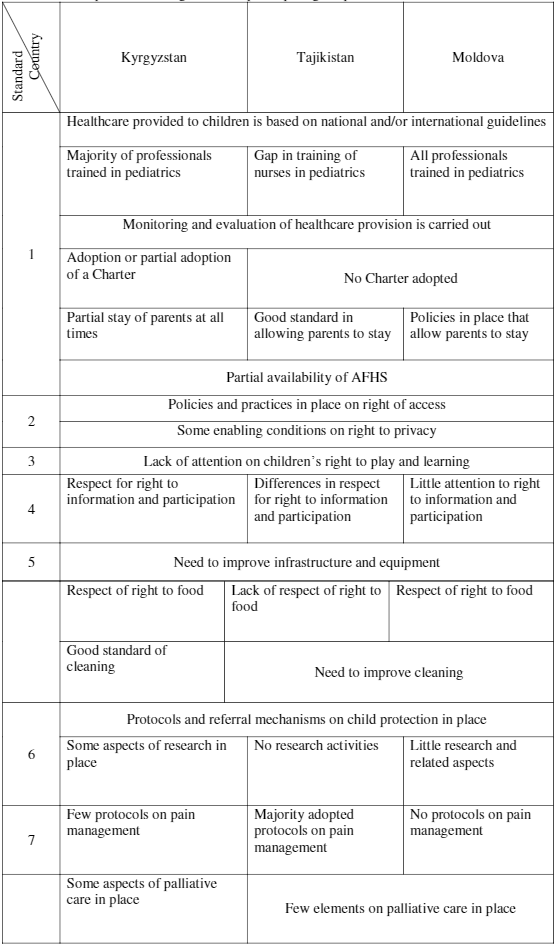
If we now take a general overview of the cross-cutting results between the three countries, it is possible to observe several standards or sub-standards with a similar situation and other areas where there is more or less significant variation (Table 11). In terms of policies and protocols, all countries provided health care based on national and/or international evidence-based guidelines and carried out monitoring and evaluation (standard 1); there were policies and practices in place on right of access (standard 2); and protocols and referral mechanisms on child protection in place (standard 6). Common gaps included the need to enhance AFHS (standard 1), conditions on right to privacy (standard 2), right to play and learning (standard 3) and the need to improve infrastructure and equipment (standard 5). Some of the rights with significant variation between the three countries included information and participation, food and pain management.In terms of palliative care, assessment teams in Tajikistan and Moldova only mentioned that palliative care includes psychological support to the child’s family, in five hospitals, in both countries. In Kyrgyzstan, palliative care begins when the illness is diagnosed and continues throughout in six hospitals, it includes psychological support to the child’s family in seven hospitals and there are partnerships in place to provide palliative care in the community or at home in five hospitals.
Table 11.Comparative findings between participating hospitals in the three countries.
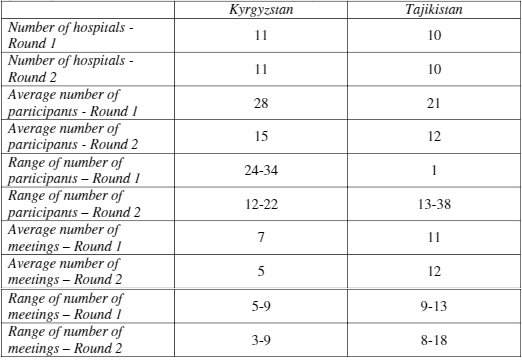
The second round of assessments in Kyrgyzstan and Tajikistan were carried out in the same hospitals as in the first round of assessment. As shown in Table 12, the average number of participants and meetings decreased from the first to the second round, with the exception of the average number of meetings carried out in Tajikistan, which increased by one.
Second round of assessments
Table 12. Number of hospitals; range and average number of participants and meetings, per hospital in the two rounds of assessment in Kyrgyzstan and Tajikistan
Overall, the results of the second round of assessment show an effective change in many of the gaps identified in the first round of assessments in Kyrgyzstan and Tajikistan. Between the first and second round of assessment, hospital managers initiated changes in several areas. For example, in Tajikistan, regarding right to food, the administration of several hospitals increased the average expenditure of food per patient by redistributing existing hospital funds, the menu was revised, the frequency of meals was increased, new kitchens, as well as, facilities for parents/caregivers and convenient conditions to cook or warm up food were established. Regarding parents’/caregivers’ stay, some of the hospitals reorganized children’s wards in a way that allowed overnight stay. Hospitals also reported that after the first assessment they ensured that in waiting areas different videos with health messages such as prevention of acute respiratory infections, diarrhea, support and promotion of breastfeeding and proper care seeking were shown to enhance parents’ knowledge of child health. The project steering group disseminated banners and brochures with relevant CRC-related information in all the participating hospitals.
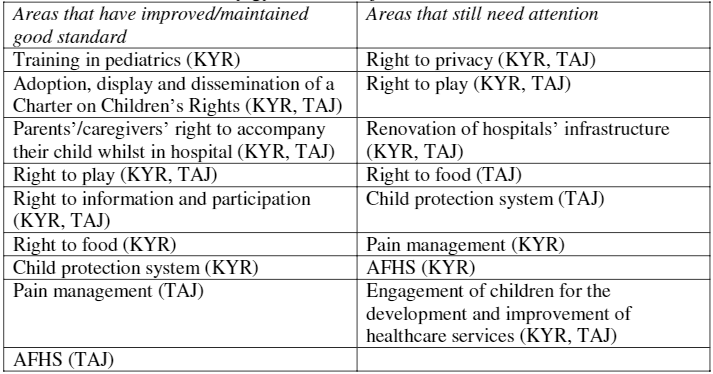
Several of the areas that have improved or that still need attention are common to both countries, as demonstrated in Table 13. Areas where significant change was shown include the adoption, display and dissemination of a Charter on Children’s Rights in Hospital; parents’/caregivers’ right to accompany their child whilst in hospital; and right to information and participation. Additionally, in Kyrgyzstan, the number of professionals working in participating hospitals that have been trained in pediatrics has increased and the right to food and the child protection system have maintained a good standard. In Tajikistan, the inputs by the stakeholders show a good standard of pain management, including training of all professionals in nine out of ten participating hospitals and there is one additional hospital providing AFHS.
The main areas that still need attention in both countries are children’s right to privacy, renovation of hospitals’ infrastructure, particularly in Tajikistan; and the engagement of children for the development and improvement of healthcare services. In terms of complementary training, in both countries health professionals have not received training on how to effectively communicate with children and families and on how to identify and examine a child who has been a victim of abuse. In Kyrgyzstan, in comparison to the first round of assessment, there has been a decrease in the number of hospitals where audits are carried out, by two and there are no improvements in terms of AFHS. In Tajikistan, children’s right to food and the child protection system are still an issue to address, as well.
In terms of right to play, in both countries there have been initiatives to adopt related hospital policies, to provide a space where children can play and, in some cases, to recruit play specialists or psychologists. However, there is still a need to provide a properly equipped playroom, with trained specialists and games adapted to all age groups; and to include play in therapeutic care in most hospitals in Kyrgyzstan and Tajikistan. Finally, there is insufficient information on the adoption and implementation of evidence-based guidelines and children’s access to health care services without discrimination in both countries.
Table 13. Children’s rights that have improved or maintained a good standard and areas that still need attention, in Kyrgyzstan and Tajikistan
The assessment of children’s rights in hospitals presented here demonstrates how to apply a HRBA to health, by taking as a reference the CRC. We will now discuss what has been the impact of adopting a HRBA to children’s health in terms of the elements highlighted in the introduction and the findings; and how to enhance such approaches.
Discussion
The participation of children and parents in the hospital assessments provided crucial information about the fulfillment of certain rights, which would have been difficult to gather otherwise. This reinforces the importance of involving children and parents in the design, development and assessment of services.
For most of the sub-standards analyzed, there were practices in place across the three countries, including areas that are more pertinent to the ‘rights’ sphere, as opposed to the ‘clinical’ sphere, such as parents’/caregivers’ right to accompany their children during hospitalization, children’s right to information and participation, the adoption of Charters on Children’s Rights in Hospital and the right to food. This means that elements of a HRBA to health were already present, which may have facilitated the improvements achieved in the short period between the first and second rounds of assessment in Kyrgyzstan and Tajikistan. Hospitals used their own resources or collaborated with WHO Country Offices for this. Most of the areas where no change was reported are those that require more substantial budgets (i.e. infrastructure-related).
The process of assessment is ‘educational’ for all stakeholders and, importantly, it translates the principles of the CRC into actions that professionals can relate to in their clinical practice and rights that children and parents can understand and claim. Although there has been no assessment of a change of attitudes by health professionals, the second round of assessments suggests enhanced skills (i.e. in informing and enabling children to participate in their own care).
In terms of equality and non-discrimination, the assessments have not been able to generate significant information about policies and practices, nor any changes between the first and second round of assessments. This takes us to two main weaknesses of the process. Firstly, the tools cannot cover the complexity and variation of factors that influence child health outcomes in every hospital and context, globally. Consequently, the reliability and impact of the use of the tools and the assessment process at large, is highly connected to the adaptation to the tools to the local context, based on the national regulatory framework; and the knowledge and sensitivity of facilitators and how they are able to explore each of the standards.
A second consideration is the sensitivity of some rights to biases, which in some cases is also tied to the inability of the questions and statements of the standards to produce detailed and reliable information. For example, whilst in parents’/caregivers’ right to accompany their child during hospitalization or children’s right to privacy, it is possible to cross the information provided by the different groups of stakeholders to gather reliable information, for others it is not. For example, in Kyrgyzstan and Tajikistan, self-evaluation teams in all hospitals stated that care is delivered based on national and international guidelines. However, a parallel assessment on QoC in Kyrgyzstan demonstrated that the adoption and implementation of guidelines must follow a stricter method; and in Tajikistan, the assessment of QoC demonstrated that case-management did not follow national or international guidelines and that most of the medical workers were not acquainted with national clinical protocols.6
Consequently, in addition to the local adaptation of the tools and a strong component of capacity building, we believe that future assessments should be complemented with the use of the WHO tools on QoC and AFHS and a more systematic programming cycle. The tools can be used as self-assessment and integrated into hospitals’ monitoring and evaluation systems of QoC and improvements can be initiated internally.
Subsequent to the programs in Kyrgyzstan, Tajikistan and Moldova, the WHO Regional Office for Europe has developed assessment tools on children’s rights in primary health care and is working with partners to enhance the process of improving QoC for children by implementing a HRBA to health. In specific, WHO is developing a framework, which member states can apply, on how to use the CRC to improve QoC for children.
Conclusion
Despite the weaknesses of the process described before, we believe that the use of the tools for the assessment of children’s rights in hospital shows some promising results and has a huge potential to improve the QoC delivered to children. However, we need to strengthen the process of assessment and improvement in line with the HRBA to health and to gather more evidence.
We therefore recommend that WHO continues this area of work; that it promotes further assessments and scaling-up in the pilot countries and other countries in the region; and that it facilitates a more comprehensive approach on how to use the CRC to improve QoC for children.
We recommend governments to set up a national steering committee made up of key institutions (i.e. MoH, national human rights institution, etc), to review the national regulatory framework taking into account the HRBA to health and to collaborate with the Ministry of Higher Education or equivalent to progressively integrate child rights and QoC in medical curricula. MoH should also make budgets available to the extent of their resources, in line with CRC provisions, to promote improvements.
We recommend the international research community to undertake a randomized control trial of the use of the assessment tools and to measure its impact on QoC and child health outcomes.
We believe this process should be linked to and would enhance the periodic reporting to the Committee on the Rights of the Child, in the context of Article 24 on children’s right to the highest attainable standard of health, as provided in General Comment No 15 of the Committee.7
Acknowledgments
The authors would like to thank Elnura Boronbaeva, Chief Pediatrician of the Ministry of Health of Kyrgyzstan; Rodica Skutelnic, Head of Mother and Child Department, Ministry of Health of the Republic of Moldova; and Dr Pavel Ursu, WHO Representative/Head of WHO Country Office and Sherali Rakhmatuloev, Head of Mother and Child Department, Ministry of Health of Tajikistan for their support with the assessments; the national coordinators involved in data collection: Gulsun Rakova, Aigul Jailoobaeva, and Bubualime Musurkulova (Kyrgyzstan); Dr Ala Cojocaru (Moldova); Dr Nargiz Nuralieva, Dr Obidjon Aminov, and Dr Holbozor Tursunov (Tajikistan); all the hospital assessment teams; and the staff, children, adolescents, and parents who participated in these assessments.
Disclaimer: Aigul Kuttumuratova, Kubanychbek Monolbaev, Larisa Boderscova, Zulfiya Pirova and Martin W. Weber are staff members of the World Health Organization. The opinions expressed in the paper are theirs and do not necessarily reflect the positions and policies of the World Health Organization.
Ethical considerations: Oral consent was obtained by the children and parents involved in the research.
Competing interests: None declared.
Copyright: © Guerreiro, Kuttumuratova, Monolbaev, Boderscova, Pirova, and Weber
Ana Isabel Fernandes Guerreiro, MA, is Independent Consultant on children’s rights, Albufeira, Portugal, WHO Regional Office for Europe, Copenhagen, Denmark
Aigul Kuttumuratova, Programme, PhD, MBA, is Officer, Child and Adolescent Health, Division of Non-communicable Diseases and Promoting Health through the Life-Course, WHO Regional Office for Europe, Copenhagen, Denmark
Larisa Boderscova, PhD, is National Professional Officer, WHO Country Office, Republic of Moldova, Chisinau, Republic of Moldova
Zulfiya Pirova, MPH, is National Professional Officer, WHO Country Office, Tajikistan, Dushanbe, Tajikistan
Martin W. Weber, MD, PhD, is ProgrammeManager, Child and Adolescent Health, Division of Non-communicable Diseases and Promoting Health through the Life-Course, WHO Regional Office for Europe, Copenhagen, Denmark
Please address correspondence to the authors c/o Ana Isabel F. Guerreiro, Estrada da Galé, Sesmarias Cx300H, 8200-385 Albufeira, Portugal.
Email: ana_isabel_guerreiro@hotmail.com.
References
1. World Health Organization, Investing in children: the European child and adolescent health strategy 2015–2020 (World Health Organization Regional Office for Europe, 2014), Available at: http://www.euro.who.int/__data/assets/pdf_file/0010/253729/64wd12e_InvestCAHstrategy_140440.pdf?ua=1
2. International Network of Health Promoting Hospitals and Health Services, Manual and Tools for the assessment and improvement of children’s rights in hospitals (International Network of Health Promoting Hospitals and Health Services, 2012). Available at: http://www.hphnet.org/index.php?option=com_content&view=article&id=1551:hp-for-children-a-adolescents-in-a-by-hospitals-&catid=20
3. Bustreo, F. et al., Women’s and Children’s Health: Evidence of Impact of Human Rights (World Health Organization,2013)
4. World Health Organization, Assessing the respect of children’s rights in hospitals in Kyrgyzstan and Tajikistan. WHO project: Improving the quality of paediatric care in the first level referral hospitals in selected countries of central Asia (World Health Organization, 2014). Available at: http://www.euro.who.int/__data/assets/pdf_file/0020/252542/Assessing-the-respect-of-childrens-rights-in-hospitals-in-Kyrgyzstan-and-Tajikistan-Eng.pdf?ua=1
5. World Health Organization, Assessing the respect of children’s rights in hospital in the Republic of Moldova (World Health Organization, 2014). Available at: http://www.euro.who.int/__data/assets/pdf_file/0006/260349/Assessing-the-respect-of-childrens-rights-in-hospital-in-the-Republic-of-Moldova.pdf
6. Lazzerini M. (2012) Assessment of pediatric hospital care in Kyrgyzstan 24th July – 4th August 2012: Mission report. WHO; available at: http://www.euro.who.int/__data/assets/pdf_file/0004/180706/e96733.pdf?ua=1 last accessed: 17 June 2015; Stasii E. (2012) Assessment of pediatric hospital care in Tajikistan 2-18 July 2012: Mission report. WHO; available at: http://www.euro.who.int/__data/assets/pdf_file/0005/181796/e96753-Eng.pdf last accessed 17 June 2015
7. Committee on the Rights on the Child, General Comment nº 15 on the right of the child to the enjoyment of the highest attainable standard of health, (Committee on the Rights on the Child, 2013)