Eugene T. Richardson, Mohamed Bailor Barrie, J. Daniel Kelly, Yusupha Dibba, Songor Koedoyoma, and Paul E. Farmer
Abstract
Despite more than 25 documented outbreaks of Ebola since 1976, our understanding of the disease is limited, in particular the social, political, ecological, and economic forces that promote (or limit) its spread.
In the following study, we seek to provide new ways of understanding the 2013-2016 Ebola pandemic. We use the term, ‘pandemic,’ instead of ‘epidemic,’ so as not to elide the global forces that shape every localized outbreak of infectious disease. By situating life histories via a biosocial approach, the forces promoting or retarding Ebola transmission come into sharper focus.
We conclude that biomedical and culturalist claims of causality have helped obscure the role of human rights failings (colonial legacies, structural adjustment, exploitative mining companies, enabled civil war, rural poverty, and the near absence of quality health care to name but a few) in the genesis of the 2013-16 pandemic. From early 20th century smallpox and influenza outbreaks to 21st century Ebola, transnational relations of inequality continue to be embodied as viral disease in West Africa, resulting in the preventable deaths of hundreds of thousands of people.
To tear treasure out of the bowels of the land was their desire, with no more moral purpose at the back of it than there is in burglars breaking into a safe. Who paid the expenses of the noble enterprise I don’t know…
Joseph Conrad, Heart of Darkness (1902)
Introduction
The 2013-2016 Ebola pandemic is the largest and longest in recorded history, with more than 28,600 reported cases as of December 13, 2015.1 The proximal determinants of the outbreak in West Africa have been well described: dysfunctional health services, a highly mobile and interconnected population, debilitated government institutions, burial practices that involve contact with contagious Ebola-infected corpses, and unsafe and poor quality provision of care to infected individuals.2 More distal determinants, including slave-trading, exploitative colonialism, enabled civil war, resource extraction, and unethical pharmaceutical trials on African people, have received scant attention.3 These centuries of extractive activities and rights violations have led to regional and global population movements which occur against a backdrop of rapid ecological change in the increasingly deforested regions of the three most affected countries—Sierra Leone, Liberia, and Guinea.
Despite more than 25 documented outbreaks since 1976—and, likely, uncounted others prior to the identification of the virus—our understanding of Ebola is limited, particularly concerning the social, political, ecological, and economic forces that promote its spread.4 For the most part, analytic attempts have had the effect of removing health and illness from the social and political context in which they are produced.5
Biosocial analyses of disease burdens increasingly recognize the limitations of biomedical and epidemiological studies, which often ignore the economic and political factors resulting in poor health outcomes.6 Biomedical culture’s linear notion of progress can be contrasted with the interactive and systems orientation of more biosocial paradigms.7 These paradigms provide a lens with which to view “the swirling political and economic relationships that dialectically produce levees and slums, soils and dams, tourism and hunger, energy and climate,” health systems and pandemics.8 Like studies of structural or symbolic violence, they can integrate “power into the understanding of disease dynamics.”9
In the following study, we provide a broadly biosocial analysis of the 2013-16 Ebola pandemic, one that leads us “from the large-scale to the local and from the social to the molecular.”10 By situating life histories in a biosocial approach, the forces promoting Ebola transmission come into sharper focus.
Brief background on Sierra Leone
Sierra Leone is a West African nation of 6.1 million people with a gross national income per capita of US$710 and a life expectancy at birth of 45 years.11 Referred to as “the white man’s grave,” the country was established by Britain as a repatriation colony for former slaves in 1787.12 It gained independence from the United Kingdom in 1961 after more than 150 years of colonial rule.
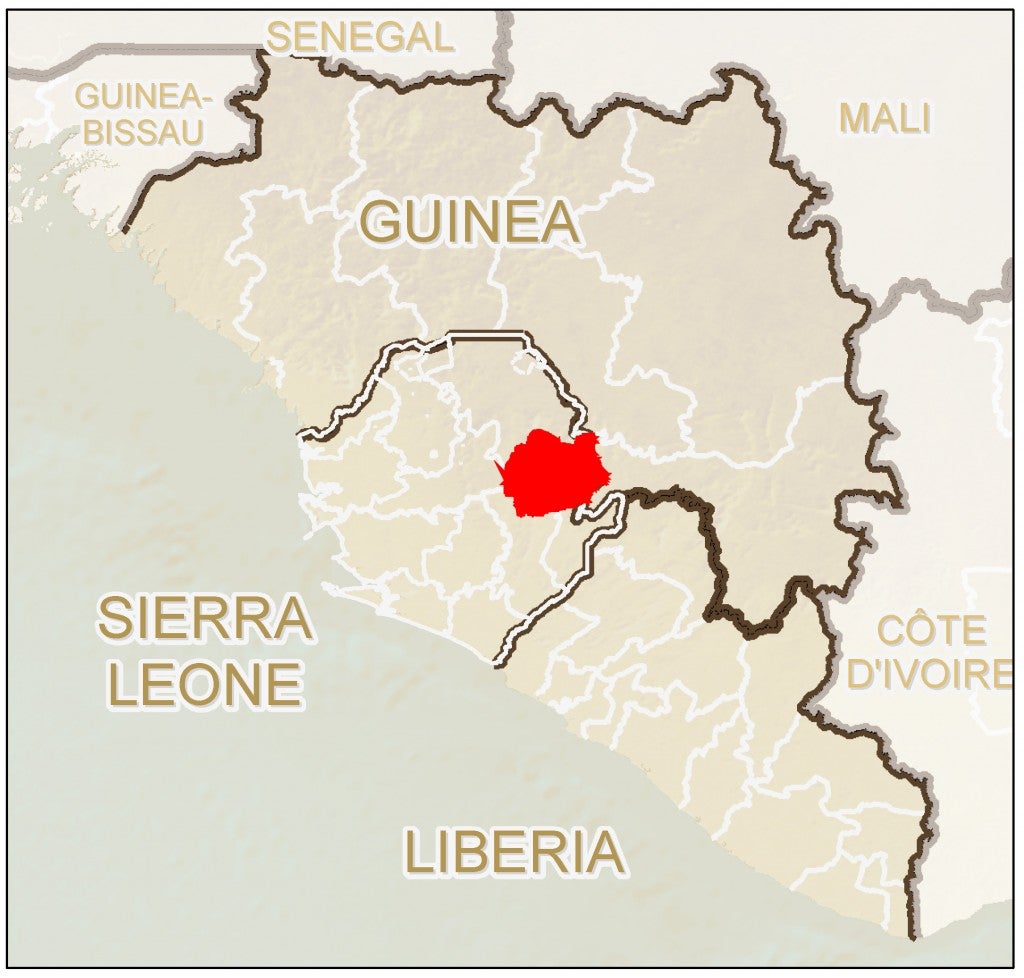
The country is divided into 14 districts and 149 chiefdoms, the latter traditionally ruled by Paramount Chiefs. Kono District (Figure 1) borders Guinea and is notable for diamond mining, thus attracting a significant amount of migrant labor. The district was also one of the major theaters of the Sierra Leone civil war (1991-2002), a conflict that resulted in more than 70,000 casualties and 2.6 million displaced people, many of them across the borders with Guinea and Liberia.13
Materials and methods
PF designed the study, which was conducted from December 2014 to March 2015. ETR and JDK first gathered systematic observations of triage, isolation, treatment, discharge, and burial while working as clinicians at the Koidu Government Hospital holding center for Ebola and in four Ebola Community Care Centers run by Partners in Health (PIH) in Kono District, Sierra Leone. ETR compiled field notes nightly.
ETR and MBB then conducted open-ended, in-depth, semi-structured interviews with four Ebola survivors from Kono District. Survivors were recruited by contacting the director of the Kono Survivors’ Group and requesting that she identify a miner, student, farmer, and health care worker who would be interested in being interviewed. Written informed consent was obtained and participants were reimbursed 50,000 Leones (US$10) for their participation. Interviews were conducted in Krio and audio-recorded. Members of the research team discussed findings and interpretations until consensus was reached on the dominant themes. Ethnographic data was then integrated with historical, political, economic, and ecological evidence to provide a biosocial account of the pandemic.
Ethics approval was not obtained, as the Stanford Institutional Review Board does not require protocol submission for research data from less than five participants. Names have been changed to protect confidentiality.
Results
- Sahr (miner)
“Lei dem nor kam nia mi.” (Don’t let them near me.)
Sahr G. was born in Kono District in 1984 but spent most of his early years in the nearby district of Bombali. When his father died in 1994, he moved back to Kono to begin work as a child miner. In 1996, at 12 years old, he was captured during the Revolutionary United Front’s (RUF) siege of Koidu (the capital of Kono District) and forced to join the fighting. The RUF’s policy of capturing and enlisting child soldiers during the Sierra Leone Civil War is well documented, with one post-war survey suggesting that 88 percent of all RUF combatants were recruited via abduction.14 Sahr was shot during a battle with government troops but survived. In 2002, he participated in the Disarmament, Demobilization and Reintegration (DDR) process, turned in his prized German submachine gun, and was given 300,000 Leones with which he planted a palm farm that has yet to turn an adequate profit.
Sahr resumed mining after the war, finding several large alluvial diamonds in the Sewa River. He invested his earnings in what turned out to be a Nigerian investment scam called “Wealth Builders.” He had planned to migrate to Europe with his earnings, but instead was obliged to resume panning the region’s rivers and streams.
In December 2014, Sahr’s uncle became gravely ill with acute fever and gastrointestinal symptoms and was brought to Koidu Government Hospital (KGH). At triage, he was misdiagnosed as being Ebola-negative and sent home. Due to an Ebola “sensitization” campaign in the district, Sahr knew the risks associated with touching suspected Ebola cases but was confident in the hospital’s judgment that his uncle was negative: “A grip di pa; a fid am sup.” (I held my uncle; I fed him soup.) Sahr cared for his uncle and started showing similar symptoms himself the day his uncle passed away. By then, he was suspicious enough that Ebola was the culprit to warn his family, “Lei dem nor kam nia mi.”
Sahr then hired a motorcycle, rode to KGH, was admitted, and tested positive for Ebola. He was sent to the Ebola treatment unit (ETU) in Kenema since Kono still lacked such a facility. The ambulance was packed with seven positive patients; two died en route. On arrival at the Kenema ETU, he panicked when he saw the red fences surrounding the suspect/confirmed zone: the rebels had attached red cloths to their weapons during live battles. Of the 14 patients sent to Kenema that day, only two survived. Sahr described it as the worst experience of his life, worse than any battle he had fought in the civil war: “Insai di war, yu kin si yu enimi; Ebola yu nor dae si am.” (During the war, you could see your enemy; Ebola can’t be seen.)
- Aminata (student)
“Wetman no dae get Ebola bikos i dae tek meresin.” (White people can’t get Ebola because they are protected by their medicines.)
Aminata K. was born in Sandor Chiefdom, Kono District, in 1993. She spent her childhood going to school and helping her father farm his small plot. She and her family were forced to flee to Guinea during the third RUF campaign in 1998.15 For over a week, they trekked by night and hid in the bush by day, eating bananas and rice their father brought, traveling toward the refugee camps in Guinea. Camp life across the border proved very difficult: her family was forced to sleep outside until her father gathered enough materials to build them a hut. Food was also scarce, and her father eked out an income by gathering firewood from local forests. After a year and a half in the camp, they returned to their village, which had been completely razed. Her father had hidden a drum of rice in the forest prior to their exodus, and it fed them until they could replant and harvest their farm.
When Aminata was 13, her mother died from an unknown illness. Her elder sister died in childbirth the same year. Even before Ebola spread west across the country in 2014, Sierra Leone had the highest maternal mortality ratio in the world.16 The lifetime risk of maternal death in Sierra Leone is 1 in 21; by comparison, the same figure in Spain is 1 in 15,000.17
After Aminata’s father remarried, conflict developed between Aminata and her stepmother, so her father moved Aminata to Koidu to finish her education. On account of schools closing during the war— when some 70% of educational institutions in Sierra Leone were destroyed—Aminata entered her final year of high school when she was 21.18 Due to Ebola, all schools in Sierra Leone were closed from June 2014 to April 2015; a notable rise in teenage pregnancies ensued.19 During this period, Aminata started a relationship with a 38-year-old pastor. They planned to wed, Aminata said, but she knew to stay away when 10 of the 15 people in his household came down with Ebola. The pastor was symptom-free during this catastrophe, but decided to jump in the back of the ambulance when his sick mother was being transferred to the ETU in Kenema, partly in order to get himself tested. After two negative Ebola tests, he went to a friend’s house in Koidu to avoid quarantine in his home. Three days later he fell ill with symptoms typical of Ebola. Aminata decided to care for him, reassured by his negative results (and the accompanying document certifying them). Shortly thereafter, the pastor was admitted to the Kono ETU (which opened in January 2015) and tested positive for Ebola. Aminata was admitted with similar symptoms five days later, and tested positive, but was separated from the pastor by a double boundary of red fencing. When asked why Aminata didn’t request to join her fiancé, she replied, “Usai dem put mi, na dae a dae.” (Where they put me, that’s where I should be.)
Both Aminata and the pastor were discharged as survivors, and they followed the instructions of the discharge nurses not to engage in sexual relations. The pastor died from apparent liver failure 10 days after he was discharged. Like most Ebola survivors, he had received little in the way of immediate clinical follow-up (in spite of mounting evidence of near- and long-term sequelae). When he became jaundiced, they consulted an herbalist, believing that he had been cured of Ebola, and was now “kontri sik.” That is, his discharge certificate verified that he was a survivor of Ebola—a foreign illness or construct; the subsequent jaundice was thought to be a result of witchcraft. Since her own discharge, Aminata has developed post-Ebola uveitis, an increasingly recognized sequela.20
- Tamba (farmer)
“Dem nor dae kam nia yu cos yu bin get Ebola. Dem say, ‘wi no wan yu na wi ples agen.’” (People don’t come near you when you’ve had Ebola. They say, ‘We don’t want you near our place again.’)
Tamba L. was born in Kambia District (on the border of Guinea) in 1949. His father was a ‘master farmer,’ producing more than 100 bushels of rice per year. When Tamba was 10 years old, he and his elder sister moved to Nimikoro Chiefdom in Kono District, and she trained him as a tailor. He married in 1971 and had five children. He began farming, producing about three bushels of rice per year. His father was well connected to the Paramount Chief in Kambia and was thus able to get farm support (for example, access to a tractor and fertilizer) via the patronage system, or ‘clientelistic exchange.’21 Tamba lamented that “big man” partnerships in Kono revolved around mining, and because of this, he was never able to enter the patrimonial system of politics there.
Like much of Kono’s population, Tamba was displaced during the civil war and fled to Makeni, then Kambia, and finally to Freetown. When he returned to Kono after the war, he had to start over: “A don los evri tin.” (I lost everything.)
Ebola struck Tamba’s village of Bumpe iatrogenically, and was then amplified through funeral practices. A well-respected taxi driver from Bumpe ferried a sick woman to KGH from the heavily afflicted village of Ndogboi. Around 10 days later, the driver suffered a stroke and was brought to KGH. At that time, the hospital was not taking admissions—the wards were being decontaminated—so the doctors in triage had two options for all presenting patients: 1) send them as Ebola suspects to the Kenema ETU, four hours away, or 2) send them closer to home to receive care in small health posts known as Peripheral Health Units. Hospital records indicate that the driver did not meet suspect criteria and was thus sent back to his village. He died several days later, and the District Ebola Response Center (DERC) was then called. The DERC sent a team to swab the body for Ebola polymerase chain reaction (PCR) testing; the body was left in the village pending the results. The results took three days to come back; this, combined with the driver’s dismissal from the hospital, led many villagers to believe he did not die from Ebola. They held a funeral: “Alman kam na di berrin.” (Everyone came to the burial.) The Ebola swab came back positive, and the subsequent village outbreak killed more than 40 people, including Tamba’s wife and their nursing child. Tamba tested positive shortly after, showing symptoms, and was quickly transported to the Kenema ETU with four friends, all of whom died.
When Tamba was asked about the reception he received in his village after discharge, he said: “Dem nor dae kam nia yu cos yu bin get Ebola. Dem say, ‘wi no wan yu na wi ples agen.’” Soon after returning home, he was employed as a community health educator as part of the Partners In Health Survivors’ Program. Tamba believes community sensitization campaigns are the key to controlling future outbreaks; he says, “Patna Pa Welbodi don gi mi wok fo go tich di villej pipul dem. Naw wi dae it wan ples…en do evri tin in komon.” (Partners In Health gave me work to educate the community. Now we eat in one place…we do everything together.)
- Esther (nurse)
“Usai dem tai kaw, na dae i dae it.” (Where you tie the cow, that’s where it eats.)
Esther B. was born in Nimiyama Chiefdom, Kono District, in 1986. Her father died before she was born, and she grew up as an only child with her mother, a typist for the chiefdom. During the war, Esther and her mother sought refuge in Freetown, where she completed secondary schooling. In 2006, she returned to Kono to work as a volunteer nurse’s aide at KGH. For seven years, she lived on handouts from staff nurses, and was finally invited to attend nursing school in 2012. This is a common path for young people interested in nursing in Sierra Leone. When asked why individuals would tolerate such hard work without steady pay, she replied, “Usai dem tai kaw, na dae i dae it.” Figuratively speaking, she explained, this means that if one works as a nurse, this is how she should gain her livelihood; she should not be expected to beg outside the hospital (that is, cut the tie and go look elsewhere for food) but rather within it. Even ‘fully employed’ nurses are so underpaid that they are forced to charge patients for otherwise free drugs and services. Instead of recognizing nurses’ salaries as insufficient to live on, the government (and even more non-Sierra Leonean commentators in the aid industry) terms this behavior “corruption.” (Figure 2)
In October 2014, Esther responded to a job request from the district to work as a nurse at the Ebola holding center at KGH. She was promised USD 100 per week (the standard Sierra Leone Ebola hazard pay) for ten weeks of work. To date, she has received USD 20. On a single day in December, we witnessed conditions at their worst: over 20 corpses lying in the ward, hygienists spraying moribund patients in the face with bleach to see if they were alive or not, hundreds of pounds of contaminated personal protective equipment lying about, and heroic nurses doing their best despite the deplorable conditions.
As elsewhere, such conditions led to nosocomial infections. By January 2015, all nine of the nurses who worked in the center had contracted Ebola; seven died. After recovering from her illness, PIH hired Esther as a nurse at one of their Community Care Centers. These centers are part of a decentralizing strategy, bringing small Ebola treatment units to relatively underserved communities—and employing survivors.
Discussion
Biosocial analysis represents a fluid space between the disciplines of economics, anthropology, political science, history, ecology, epidemiology, and physiology.22 In the case of the 2013-16 Ebola pandemic, it allows us to interrogate claims of causality while insisting on the importance of the right to health. We use the term, ‘pandemic,’ and avoid ‘epidemic,’ so as not to elide the global forces that shape every localized outbreak of infectious disease.
Political economy
The survivors’ experiences outlined above offer evidence of an abysmal public health infrastructure in Sierra Leone, as well as a near absence of clinical care. It thus seems germane to ask why health services—and government institutions in general—are so impoverished.
As Englebert has shown, the arbitrariness of a country’s boundaries in Africa correlate with poor development outcomes.23 The boundaries of Sierra Leone have had little to do with cohesive self-determination, but rather were determined by the interests of colonial powers.24 In short, the Republic of Sierra Leone inherited a flawed, exploitative polity from colonial rulers.25
The heterogeneity of identities lassoed within such contrived boundaries help set the climate for patrimonial rule.26 Patrimonialism, as highlighted in Tamba’s narrative, is a “style of governance where politicians control power through a system of personal relationships where policies/favors are distributed in exchange for political support.”27 It is has been the de facto form of rule in Sierra Leone since independence was declared, and has been potentiated by minerals as a ready source of patronage.28 Diamonds, for example, have been central to transnational corporate profiteering and underdevelopment in Sierra Leone.29 They also triggered and sustained horrific brutality in the Sierra Leone civil war (1991-2002) and have come to be seen as a ‘resource curse.’30 What would it take to help remedy the situation in Kono, where billions of dollars have been extracted from the ground (Figure 3), yet roads, hospitals, and schools are absent or woefully underfunded? For example, while KGH lacked x-ray capability—making care for conditions ranging from tuberculosis to fractures suboptimal at best—the nearby mining company had a perfectly functional, if rarely used, x-ray machine.31
Patrimonialism as a system of rule is said to be counterproductive to economic development, representative government, and accountable institutions. As a violation of the right to health, resources that could be devoted to public works for the poor are instead funneled to elite coffers—hence the “public health desert” found in today’s Sierra Leone.32 The resulting dysfunctional health facilities then amplify transmission in infectious disease outbreaks: as of December 13, 2015, Sierra Leone reported 14,122 cases of Ebola.33 Indeed, Esther’s tally of nine out of nine nurses infected at the KGH holding center demonstrates the parlous risk dysfunctional health facilities pose.
As an example of the lack of checks and balances associated with patrimonial governance, and because of weak public institutions, Sierra Leone did not have an analytic platform capable of accounting for all the money allocated to fight Ebola, most of which went to international NGOs and contractors. A 2015 report by national auditors found that almost a third of these funds were unaccounted for.34 When we asked our national staff where the money went, many replied, “Dem don it di moni.” (The government elites ate [stole] the money.) We witnessed the patrimonial system at work as foreign aid was channeled through the National Ebola Response Center, then on to District Ebola Response Centers, some headed by Paramount Chiefs. Resources (for example, vehicles) were meted out according to informal arrangements, rather than actual UN- and donor-written allocations. Esther’s unresolved hazard pay was another casualty of such a system.
But government institutions are not solely to blame. The paradigm of infectious disease exceptionalism, whereby international aid is funneled into intensive responses for exceptional conditions (HIV, for example), reorients the donor gaze from strengthening health systems in general to mopping up preventable pandemics.35 The aid industry thus serves as an “anti-politics machine,” which effectively casts problems of outbreak containment in apolitical, ahistorical, techno-managerial terms, while disguising the underlying political and economic causes.36 Another way of saying this is that purposeful underdevelopment in West Africa and trans-hemispheric relations of inequality are the real pathologies—not Ebola.
This leads us to question: Is current Ebola aid from the World Bank, the United Kingdom Department for International Development, and the United States Agency for International Development enough to redress the path-dependent influence of colonial institutions that have facilitated the current pandemic?37 Is this aid a form of reparations disguised as altruism? Will this outpouring of Ebola aid lead to sustainable investments and health-systems strengthening in Sierra Leone? The huge reductions in aid (now that West Africa has been declared ‘Ebola free’) suggest otherwise. As Sahr observed, “Wei di ren dae kam, yuba sae i go bil os; wei san komot, i foget.” (When it’s raining, the vulture says he’ll build a house; when the sun comes out, he forgets.)
Human and peoples’ rights
The 1981 African Charter on Human and Peoples’ Rights (also known as the Banjul Charter) is a rather novel instrument in that it not only includes rights for individuals but also for people.38 The promulgation of the right to an environment conducive to satisfactory collective development (Article 24) provides a moral language for biosocial analyses, in that it transcends the liberal focus on ‘bounded’ individuals and pays special recognition to human interconnectedness.39 Esther’s narrative demonstrates that health care workers (HCWs) have risks that are structured by their group identity. When the term “caregiver” is extended to include people like Sahr, Aminata, and Esther—all of whom provided care for infected people—we see that Ebola is fundamentally a disease of people who care about others, but lack the staff, stuff, space, and systems to do so safely.
Relational human rights in West Africa are not solely promoted by a mere exposé of how the fruits of scientific advances are stockpiled for some and denied to others.40 Rather, there must be a praxis component. It forces us to ask: Will the rebuilding of the country’s economy and health infrastructure occur in pragmatic solidarity with the people of Sierra Leone—as in the case of Tamba? Or will Western aid continue to manage “inequality with the latest tools from economists and technocrats”?41
Using the Banjul Charter as a guide, we witnessed relational human rights violations throughout the Ebola outbreak: in WHO’s initial mishandling of the public health threat; in dysfunctional health systems; in quarantined villages that lacked adequate food supplies; in extractive biomedical and social science research programs lacking clinical delivery platforms; and in the limited use of intravenous resuscitation—the only hope to save those with significant loss of fluids and electrolytes—throughout the brunt of the outbreak. Even MSF, recipient of the Lasker-Bloomberg Public Service Award in recognition of their work in the Ebola-affected countries, remarked, “the prolonged reluctance of placing IV-lines to severely dehydrated patients will remain a symbol of the inadequate clinical care during MSF’s Ebola intervention in West Africa.”42 All of the NGOs on the ground had the responsibility to provide good supportive care to those suffering from Ebola.
Ecology
Several authors have posited ecological forces in sparking outbreaks of Ebola. Bausch and Schwarz describe a three-tiered cascade that results in sustained outbreaks: 1) poverty drives individuals to encroach deeper into forests, making zoonotic transmission more probable; 2) infections are then amplified by a dysfunctional health system; and 3) containment is hampered by poorly resourced governments.43 Such a thesis is plausible and far better buttressed by evidence than are culturalist claims, but more could be said. When Tamba was presented with this line of reasoning, he remarked, “Wi don dae go na bush fo yia, pan di wa…en di ospital dem bin bad. So wai naw?” (We’ve been going deep in the forest for ages, especially during the war…and the hospitals have always been bad. So why now?) While Tamba is not aware of recent evidence that demonstrates circulating Ebola prior to this outbreak, he is prescient to ask, “Why now?”44
Another important question is by what mechanisms has international agribusiness shaped and taken advantage of the 2013-2016 Ebola pandemic. Wallace and colleagues posit that capital-intense industrial palm oil farms have increased human interaction with frugivorous bats (Pteropodidae), a putative Ebola reservoir, and may explain the association of outbreak peaks at the start of the dry season, when oil palm picking is at its height.45 Alarmingly, a recent report by Global Witness documents the way Golden Veroleum Liberia (a subsidiary of Golden Agri-Resources, a palm oil plantation company based in Indonesia) has taken advantage of pandemonium and the scaling back of advocacy by environmental NGOs during the pandemic to double its landholdings for palm oil plantations.46 The dependence on subsistence farming, which Aminata describes, should stimulate interrogation of trade deals that often undermine food security.
Climate change may be another ecological mechanism that contributes to Ebola outbreaks. Alexander and colleagues suggest that increasing climate variability can alter fruiting patterns in West African flora, potentially concentrating reservoir and susceptible host species in areas of increased foraging opportunity. This can lead to increased Ebola transmission in wildlife, which may result in a higher probability of spillover to humans. The authors thus conclude, “research into Ebola reservoir and transmission dynamics will be essential to refining surveillance approaches.”47
Like the environment itself, ecological claims are fragile and uncertain. Fairhead and Leach provide a compelling challenge to straightforward models of ecological change, arguing that deforestation has consistently been exaggerated in this region which has long been densely populated and farmed and in which many of the forests are actually anthropogenic in origin.48
Do inequitable trade agreements facilitate the ecological conditions conducive to pandemic disease? Is it possible to tie unsustainable consumption and carbon emissions in industrialized countries to increased outbreaks of viral hemorrhagic fevers? Do anthropogenic forests create further facilitate spillover? We agree with other authors that ecological analysis and policy need to be reframed towards addressing the problems of socially vulnerable people, like Tamba, Aminata, and Sahr.49
“Culture” and claims of causality
The term “culture” is perhaps the most vexed in anthropology, and in the social sciences in general; it admits to multiple meanings in discussions of serious illness, where it serves as a black box with extraordinary (and often contradictory) explanatory power. It is certain that the cultural traditions of the people most affected by Ebola, and those charged with responding to it, have shaped the current pandemic in significant ways; these traditions have included ways of understanding illness, of seeking care in the absence of a functioning health system, and in funerary practice in the absence of almost anything in the way of assistance for family members. But much more can be said about the influence of rapidly changing social institutions and ecological conditions on what are loosely (and inaccurately) termed “traditional beliefs.” One classic example is the fetishization of bushmeat and bats. The inordinate amount of attention focused on bushmeat and bats in radio programs, pamphlets, billboards (Figure 4), and other media culturalizes and de-historicizes the political and economic forces that have promoted the pandemic. It should be remembered that only one of the more than 28,000 reported cases in West Africa is thought to have come from bushmeat or bats.50
Concerning bushmeat, Rizkalla and colleagues argue, “Despite efforts to change the eating habits of African villagers, many believe occult forces are behind Ebola. They do not understand that they could limit their exposure by avoiding dead or sick animals.”51 Many of the patient histories we took while working at the Community Care Centers are at odds with the view that intractable behaviors amplify transmission. These histories are corroborated by the in-depth interviews with Sahr, Aminanta, and Tamba, each of whom indicated they were aware of no-touch policies, but were dissuaded by the ambiguous—in their view—discharge certificates that signaled their contacts were Ebola-free. They also stepped in where professional caregivers were unavailable, beleaguered, or dead.
The cultures of distinctly transnational institutions have also shaped the Ebola pandemic. As we observed at inter-agency meetings, providers of foreign aid clamored to publish the number of ETUs built, patients triaged, lab specimens processed, calls made to 117 (the national Ebola alert number), and so on, while often failing to ask critical questions such as: Is chronic poverty obscured by international interventions that fetishize epidemiological statistics and ‘performance’ indicators?52 Such statistics, and their exaggerated precision, evoke the power of scientific claims and make it “difficult to distinguish an emergency [outbreak] from chronic poverty.”53 In addition, with the input of anthropologists, these statistics tend to reify culture “as an ensemble of measurable factors with deterministic power over specific aspects of illness.”54 In other words, the emphasis on ‘deliverables’ in the emergency setting obfuscates the relationship between human rights failings and outbreaks of infectious disease.
A final example is biomedical culture’s focus on Ebola as a freestanding biological entity, which disguises its existence as a social phenomenon.55 As an illustration, we observed that Ebola ‘survivors’—that is, those who are symptomatic, test positive, and survive—were sometimes given benefits in the form of food, clothing, and employment, even if they were the only ones in their families affected. Suspect cases who were discharged negative from an ETU were given nothing, even if all their family members perished on account of the disease. In short, the biomedical notion of individual symptomatic viremia determined whether or not “an individual” received international aid, which may subvert Sierra Leonean collectivist psychologies.56 In recognition of these relational rights, some NGOs provide social support for Ebola-affected persons and their networks, whether an individual tests positive or not.
Points of departure
From early 20th century smallpox and influenza outbreaks to 21st century Ebola, transnational relations of inequality continue to be embodied as viral disease in West Africa, resulting in the preventable deaths of hundreds of thousands of individuals.57 Then and now, biomedical and culturalist claims of causality help obscure the role of human rights failings in the genesis of infectious disease outbreaks. We submit that an analytic framework based on radical relationality, including webs of power relations at the political, economic, ecological, and cultural levels, is necessary to provide an adequate account of the re-emergence of Ebola in West Africa.58 These webs stretch back in time and across the region and link it to distant continents, as a more comprehensive account of the current pandemic will one day reveal—and as Sahr’s, Aminata’s, Tamba’s, and Esther’s accounts already suggest. An historically grounded, biosocial approach can foster a change towards a more reflexive understanding of outbreak responses in general, one that provides a corrective lens for biomedical tunnel vision.
Acknowledgments
The authors would like to express their gratitude to and admiration for the Kono Survivors’ Group. We would also like to thank the staff of Wellbody Alliance and Partners In Health for their dedication to health equity in Sierra Leone, in particular, Corrado Cancedda, Kerry Dierberg, Jonathan Lascher, Kathryn Barron, Gabriel Warren Schlough, Michael Drasher, and Gina Lamin.
Eugene Richardson, MD, is a PhD Candidate in the Department of Anthropology at Stanford University, Stanford, CA, USA, and a Research Scientist at Partners In Health, Freetown, Sierra Leone.
Mohamed Bailor Barrie, MBChB, is co-founder of Wellbody Alliance, Koidu, Sierra Leone; an MMSc Candidate in the Department of Global Health and Social Medicine at Harvard Medical School, Boston, MA, USA; and Strategic Adviser to Partners In Health, Freetown, Sierra Leone.
Daniel Kelly, MD, is co-founder of Wellbody Alliance, Koidu, Sierra Leone, and a Lecturer in the Division of Global Health Equity at Brigham and Women’s Hospital, Boston, MA, USA.
Yusupha Dibba, MBChB, is Medical Director of Wellbody Alliance, Koidu, Sierra Leone.
Songor Koedoyoma, MBChB, is Chief of Staff of the Kono District Ebola Response Center (DERC), Koidu, Sierra Leone.
Paul E. Farmer, MD, PhD, is co-founder of Partners In Health, Boston, MA, USA, Kolokotrones University Professor of Global Health and Social Medicine at Harvard Medical School, Boston, MA, USA, and Chief of the Division of Global Health Equity at Brigham and Women’s Hospital, Boston, MA, USA. He is editor-in-chief of Health and Human Rights Journal.
Please address correspondence to Eugene T. Richardson, MD, Department of Anthropology, Stanford University, 450 Serra Mall, Main Quadrangle, Building 50, Stanford, CA 94305-2034, USA. Email: etr@stanford.edu
References
- P. Piot, J-J. Muyembe, and W. J. Edmunds,”Ebola in west Africa: From disease outbreak to humanitarian crisis,”Lancet Infectious Diseases 14/11 (2014), pp. 1034-1035; and World Health Organization, Ebola situation report — 16 December 2015 (Geneva: WHO, 2015). Available at http://apps.who.int/ebola/current-situation/ebola-situation-reports
- M. Chan, “Ebola virus disease in west Africa — No early end to the outbreak,” New England Journal of Medicine 371/13 (2014), pp. 1183-1185; D. M. Pigott, N. Golding, A. Mylne, et al., “Mapping the zoonotic niche of Ebola virus disease in Africa,” Elife 3 (2014), pp. e04395; J. A. Robinson, Governance and political economy constraints to World Bank CAS priorities in Sierra Leone (Washington, DC: World Bank, October 2008); P. Richards, J. Amara, M. C. Ferme, et al., “Social pathways for Ebola virus disease in rural Sierra Leone, and some implications for containment,” PLoS Neglected Tropical Diseases 9/4 (2015), pp. e0003567; and P. Farmer, “Diary,” London Review of Books 36/20 (2014), pp. 38-39.
- W. Rodney, How Europe underdeveloped Africa (London: Bogle-L’Ouverture, 1972); I. Abdullah (ed), Between democracy and terror: The Sierra Leone civil war (Dakar: Codesria, 2000); A. Wilkinson and M. Leach, “Briefing: Ebola-myths, realities, and structural violence,” African Affairs 114 (2014), pp. 136-148; and J. Martin-Moreno, “Ebola, or the messy cocktail of public health and globalisation in post-colonial Africa,” Lancet Global Health Blog (2014). Available at http://globalhealth.thelancet.com/2014/09/04/ebola-or-messy-cocktail-public-health-and-globalisation-post-colonial-africa; S. Philpott and U Schüklenk, ” A study that should not have been done,” (Garrison: Hastings Center, 2010). Available at http://www.thehastingscenter.org/Bioethicsforum/Post.aspx?id=4626#ixzz3imwzfeUJ; P. Farmer, “New malaise: Medical ethics and social rights in the global era,” Pathologies of power: Health, human rights, and the new war on the poor (Berkeley: University of California Press, 2004), pp. 196-212; and E. R. Ezeome and C. Simon, ”Ethical problems in conducting research in acute epidemics: the Pfizer meningitis study in Nigeria as an illustration,” Developing World Bioethics 10/1 (2010), pp. 1-10.
- Centers for Disease Control and Prevention, Outbreaks chronology: Ebola hemorrhagic fever (Atlanta: CDC, 2014). Available at http://www.cdc.gov/vhf/ebola/resources/outbreak-table.html; Ebola Response Anthropology Platform. Available at http://www.ebola-anthropology.net
- M. Vaughan, Curing their ills: Colonial power and African illness (Redwood City: Stanford University Press, 1991); E. K. Akyeampong, “Disease in West African history,” in E. K. Akyeampong (ed), Themes in West African History (Oxford: James Currey, 2006); P. Farmer, AIDS and accusation: Haiti and the geography of blame (Berkeley: University of California Press, 1992); M. Lock and V-K. Nguyen, An anthropology of biomedicine (Chichester: Wiley-Blackwell, 2010).
- R. M. Packard, B. Wisner, and T. Bossert, “Introduction,” Social Science & Medicine 28/5 (1989), pp. 405-414; P. Farmer. “Social inequalities and emerging infectious diseases,” Emerging Infectious Diseases 2/4 (1996), pp. 259-269; P. Farmer, “Social scientists and the new tuberculosis,” Social Science & Medicine 44/3 (1997), pp. 347-358; D. Fassin, When bodies remember: Experiences and politics of AIDS in South Africa (Berkeley: University of California Press, 2007); and J. Biehl and A. Petryna, “Critical global health,” in J. Biehl and A. Petryna (eds), When people come first: Critical studies in global health (Princeton: Princeton University Press, 2013), pp. 1-22.
- R. Kearns, “Place and health: Towards a reformed medical geography,” Professional Geographer 45/2 (1993), pp. 139-147; E. T. Richardson and A. Polyakova, “The illusion of scientific objectivity and the death of the investigator,” European Journal of Clinical Investigation 42/2 (2012), pp. 213-215.
- P. Robbins, Political ecology: A critical introduction, 2nd ed. (West Sussex: John Wiley & Sons, 2012).
- P. Farmer, “An anthropology of structural violence,” Current Anthropology 45/3 (2004), pp. 305-325; P. Bourdieu and J-C. Passeron, Reproduction in education, society and culture (London: Sage, 1977); quote from J. Mayer, “The political ecology of disease as one new focus for medical geography,” Progress in Human Geography 20/4 (1996), pp. 441-456.
- P.E. Farmer, “Preface,” in P. Farmer, A. Kleinman, J. Kim, and M. Basilico (eds), Reimagining global health: An introduction (Berkeley: University of California Press, 2013), pp. xiii-xxiii.
- World Bank, World development indicators (Washington, DC: World Bank, 2013).
- F.H. Rankin, The white man’s grave: A visit to Sierra Leone in 1834 (London: Richard Bentley, 1836).
- M. Kaldor and J. Vincent, Case study Sierra Leone (New York: UNDP, 2006).
- I. Beah, A long way gone: Memoirs of a boy soldier (New York: Sarah Crichton Books, 2007); M. Humphreys and J. M. Weinstein, “Who fights? The determinants of participation in civil war,” American Journal of Political Science 52/2 (2008), pp. 436-455.
- L. Gberie, A dirty war in west Africa: The RUF and the destruction of Sierra Leone (Bloomington: Indiana University Press, 2005).
- United Nations Population Fund, Breaking the silence about maternal death in Sierra Leone (New York: UNFPA, 2010).
- United Nations Children’s Fund, Maternal mortality (New York: UNICEF, 2013). Available at http://data.unicef.org/maternal-health/maternal-mortality.
- Gberie (see note 19).
- Plan, “Teenage pregnancy rates rise in Ebola-stricken West Africa,” (2014). Available at https://plan-international.org/about-plan/resources/news/teenage-pregnancy-rates-rise-in-ebola-stricken-west-africa/.
- D. V. Clark, H. Kibuuka, M. Millard, et al., “Long-term sequelae after Ebola virus disease in Bundibugyo, Uganda: a retrospective cohort study,” Lancet Infectious Diseases 15/8 (2015), pp. 905-912.
- Robinson (see note 2).
- A. Biersack and J. B. Greenberg, Reimagining political ecology (Durham: Duke University Press, 2006).
- P. Englebert, State legitimacy and development in Africa (Boulder: Lynne Rienner, 2000).
- F. N. Le Mesurier and L. P. Schwartz, Agreement between Great Britain and France respecting the boundary between Sierra Leone and French Guinea (London, 1913). Available at http://ocid.nacse.org/tfdd/tfdddocs/49ENG.pdf; and A. A. Boahen, Africa under colonial domination, 1880-1935, Vol. 7 (Berkeley: University of California Press, 1990).
- B. Davidson, Black man’s burden: Africa and the curse of the nation-state (New York: Random House, 1992); S. Meyer, Sierra Leone: Reconstructing a patrimonial state (Madrid: FRIDE, 2007).
- G. Padró-i-Miquel, “The control of politicians in divided societies: The politics of fear,” Review of Economic Studies 74 (2007), pp. 1259-1274.
- Robinson (see note 2).
- W. Reno, “Liberia and Sierra Leone: The competition for patronage in resource-rich economies,” in E. W. Nafziger, F. Stewart, and R. Väyrynen (eds), Weak states and vulnerable economies: Humanitarian emergencies in developing countries, Vol. 2, (Oxford: Oxford University Press, 2000).
- A. Zack-Williams, Tributors, supporters and merchant capital: Mining and underdevelopment in Sierra Leone (Brookfield: Avebury, 1995); I. Smillie, “Getting to the heart of the matter: Sierra Leone, diamonds, and human security,” Social Justice 27/4 (2000), pp. 24-31.
- V. A. B. Davies, “Sierra Leone: Ironic tragedy,” Journal of African Economies 9/3 (200), pp. 349-369.
- P. R. Keefe, “Buried secrets,” The New Yorker (July 8, 2013) and P. R. Keefe, “Two mining bohemoths battle an Israeli billionaire,” The New Yorker (June 2, 2014).
- A. Sen, Development as freedom (New York: Anchor Books, 1999); quote from P. Farmer, “Who lives and who dies,” London Review of Books 37/3 (2015).
- World Health Organization (see note 1).
- Audit Service Sierra Leone. Report on the audit of the management of the Ebola funds, May to October 2014 (Freetown, 2015).
- A. Benton, HIV exceptionalism (Minneapolis: University of Minnesota Press, 2015).
- J. Ferguson, The anti-politics machine: development, depoliticization, and bureaucratic power in Lesotho (Minneapolis: University of Minnesota Press, 1994).
- S. L. Engerman and K. L. Sokoloff, “Factor endowments, institutions, and differential growth paths among new world economies,” in S. Haber (ed), How Latin America fell behind (Palo Alto: Stanford University Press, 1997); and D. Acemoglu, S. Johnson, and J. A. Robinson, “Colonial origins of comparative development: An empirical investigation,” American Economic Review 91 (2001), pp. 1369-1401.
- African Charter on Human and Peoples’ Rights, (1981). Available at http://www.achpr.org/instruments/achpr/.
- M. Heintz (ed), The anthropology of moralities (New York: Berghahn, 2009).
- N. Vaisman, “Relational human rights: Shed-DNA and the identification of the ‘living disappeared’ in Argentina,” Journal of Law and Society 41/3 (2014), pp. 391-415.
- P. Farmer with N. Gastineau, Rethinking health and human rights,” S. Gruskin, M. A. Grodin, G. J. Annas, and S. P. Marks (eds), Perspectives on health and human tights (New York: Routledge, 2005), pp. 73-94.
- Ebola: a challenge to our humanitarian identity. A letter to the MSF movement. Dec 4, 2014.
- D. G. Bausch and L. Schwarz, “Outbreak of Ebola virus disease in Guinea: Where ecology meets economy,” PLoS Neglected Tropical Diseases 8/7 (2014), pp. e3056.
- R. J. Schoepp, C. A. Rossi, S. H. Khan, et al, “Undiagnosed acute viral febrile illnesses, Sierra Leone,” Emerging Infectious Diseases 20/7 (2014), pp. 1176-1182.
- R. G. Wallace, M. Gilbert, R. Wallace, et al., “Did Ebola emerge in west Africa by a policy-driven phase change in agroecology?” Environment and Planning A 46 (2014), pp. 2533-2542; R. Wallace, “Neoliberal Ebola: palm oil, logging, land grabs, ecological havoc and disease,” Ecologist (July 25, 2015). Available at http://www.theecologist.org/News/news_analysis/2964412/neoliberal_ebola_palm_oil_logging_land_grabs_ecological_havoc_and_disease.html; and R. Carrere, Oil palm in Africa: Past, present and future scenarios (Montevideo: World Rainforest Movement, 2010).
- Global Witness, The new snake oil? The violence, threats, and false promises driving rapid palm oil expansion in Liberia (London: Global Witness, July 2015).
- K. A. Alexander, C. E. Sanderson , M. Marathe, et al., “What factors might have led to the emergence of Ebola in West Africa?” PLOS Medical Journals’ Community Blog (November 11, 2014). Available at http://blogs.plos.org/speakingofmedicine/2014/11/11/factors-might-led-emergence-ebola-west-africa/.
- J. Fairhead and M. Leach, Misreading the African landscape: Society and ecology in a forest-savanna mosaic (Cambridge: Cambridge University Press, 1996).
- T. Forsyth, “Political ecology and the epistemology of social justice,” Geoforum 39/2 (2008), pp. 756-764; and H. Baer and M. Singer, Global warming and the political ecology of health (Walnut Creek: Left Coast Press, 2009).
- D. J. Park, G. Dudas, S. Wohl, et al. “Ebola virus epidemiology, transmission, and evolution during seven months in Sierra Leone,” Cell 161 (2015), pp. 1516-26
- C. Rizkalla, F. Blanco-Silva, and S. Gruver, “Modeling the impact of Ebola and bushmeat hunting on western lowland gorillas,” Ecohealth 4/2 (2007), pp. 151-155.
- V. Adams, “Subjects, profits, erasures,” in Biehl and Petryna (eds), (note 9), pp. 79.
- M. Foucault, Discipline and punish: The birth of the prison (New York: Knopf Doubleday, 1979); quote from R. Rottenburg, “Social and public experiments and new figurations of science and politics in postcolonial Africa,” Postcolonial Studies 12/4 (2009), pp. 423-440.
- J. Jones, “Ebola, emerging: The limitations of culturalist discourses in epidemiology,” Journal of Global Health 1/1 (2011), pp. 1-6; quote from S. M. DiGiacomo, “Can there be a “cultural epidemiology”?” Medical Anthropology Quarterly 13/4 (1999), pp. 436-457.
- M. T. Taussig, “Reification and the consciousness of the patient,” Social Science Medicine 14B/1 (1980), pp. 3-13.
- G. Millar, An ethnographic approach to peacebuilding: Understanding local experiences in transitional states (New York: Routledge, 2014).
- I. Rashid, “Epidemics and resistance in colonial Sierra Leone during the First World War,” Canadian Journal of African Studies 45/3 (2011), pp. 415-439.
- R. Braidotti, The posthuman (Cambridge: Polity, 2013) and T. L. Goldberg and J. A. Patz, “The need for a global health ethic,” Lancet 386/10007 (2015), pp. e37-e39.
Figure 1. Sierra Leone and surrounds. Kono District in red. Source: Centers for Disease Control and Prevention.
Figure 2. Billboard at Koidu Government Hospital. Photo credit: ET Richardson.

Figure 4. Bushmeat billboard, Liberia. Photo credit: Paul E. Farmer