Climate Change and the Right to Health for Māori in Aotearoa/New Zealand
Rhys Jones, Hayley Bennett, Gay Keating, Alison Blaiklock
Health and Human Rights 2014, 16/1
Abstract
Climate change is widely regarded as one of the most serious global health threats of the 21st century. Its impacts will be disproportionately borne by the most disadvantaged populations, including indigenous peoples. For Māori in Aotearoa/New Zealand, as with other indigenous peoples worldwide, colonization has led to dispossession of land, destabilization of cultural foundations, and social, economic, and political marginalization. Climate change threatens to exacerbate these processes, adding future insult to historical and contemporary injury. Yet the challenges posed by climate change are accompanied by considerable opportunities to advance indigenous rights and reduce health disparities. In this paper, we examine issues related to climate change and Māori health using a right to health analytical framework, which identifies obligations for the New Zealand government.
Introduction
Climate change is widely regarded as a serious threat to public health globally.1 It is already causing significant morbidity and mortality, with impacts predicted to increase markedly over coming decades.2 Leading health threats include water and food shortages, extreme weather events, changing patterns of infectious disease, and mental/psychological stress. In Aotearoa/New Zealand, there will also be new health and social pressures relating to the arrival of climate migrant and refugee populations and flow-on health impacts from changes in global and local economies and policies in response to climate change.3
Vulnerability to the health effects of climate change varies considerably between different populations, being influenced by geographic location, demographics including socioeconomic status, background burden of climate-related health conditions, health system capability, and capacity to adapt.4 Adverse impacts will be disproportionately borne by the most disadvantaged populations, including indigenous peoples.5 As noted in the UNESA State of Worlds Indigenous Peoples 2009, “For many indigenous peoples, climate change is a potential threat to their very existence and a major issue of human rights and equity.”6
Aotearoa/New Zealand is a country of just over 4 million people, with Māori, the indigenous people, comprising 14.9% of the total population.7 As with many other indigenous peoples worldwide, colonization has led to dispossession of land and destabilization of cultural foundations as well as social, economic, and political marginalization.8 These processes are perpetuated through colonial systems and structures that maintain an inequitable distribution of the determinants of health. As a result, Māori are disproportionately exposed to adverse social and economic conditions, with consequent higher morbidity and mortality. Life expectancy for Māori is over seven years lower than for non-Māori, and Māori have significantly higher rates of most major diseases, such as cardiovascular disease, cancers, chronic respiratory disease, and diabetes, as well as experiencing poorer access to and quality of health care.9 These factors all increase vulnerability to the health effects of climate change for Māori in Aotearoa/New Zealand.
It is critical that public health and equity are positioned at the centre of climate change policy.10 A rights-based approach is a helpful way to consider these issues in order to achieve optimal outcomes for indigenous populations. Climate change is inextricably linked to the right to the highest attainable standard of health; realization of this right depends on a liveable environment and a stable climate.11 The right to health has been clearly associated with climate change for the childhood population; the Committee on the Rights of the Child, in its recent General Comment on the right to health, described climate change as one of the biggest threats to child health and one that exacerbates inequalities.12
This paper begins by describing the impacts of climate change on health and the determinants of health for Māori, as well as the health co-benefits of climate action. We then use a right to health analytical framework to examine issues related to climate change and Māori health.
The impacts of climate change on Māori health
Māori concepts of health
Māori concepts of health extend beyond physical interpretations to conceptualize health as a collective and individual continuum that traverses generations. In common with other indigenous peoples, Māori understandings of health emphasize a holistic perspective that incorporates spiritual, intellectual, physical, social, and emotional dimensions, and includes relationships with the natural environment.13 The United Nations Development Group, in its guidelines on indigenous issues, says, “A healthy indigenous community is one in which the community as a whole enjoys harmonious relations with its environment.”14
Indigenous concepts of health have parallels with concepts of the determinants of health and the indivisibility and interdependence of human rights. Indigenous peoples have, however, long extended such ideas with the emphasis they place on comprehending the dependence of humans on the natural environment for health and well-being. In addition to the physical/mental impacts of climate change on human health described below, for Māori (and in fact all peoples), climate change also has important implications for cultural, social, and economic determinants of health.15
Physical and mental health impacts
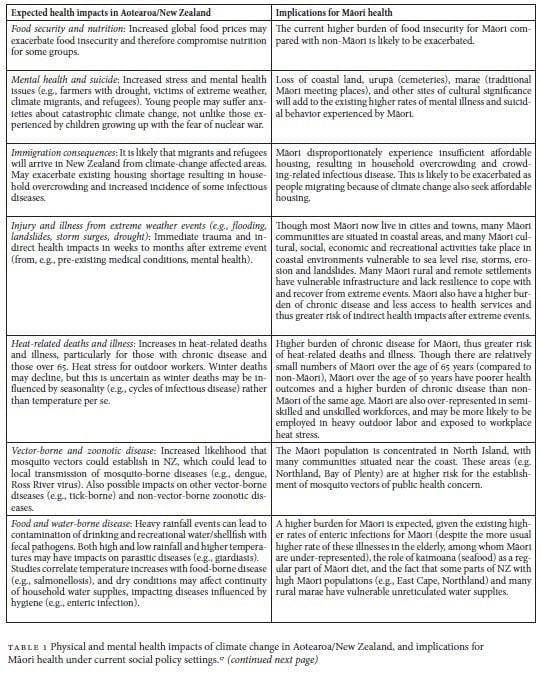
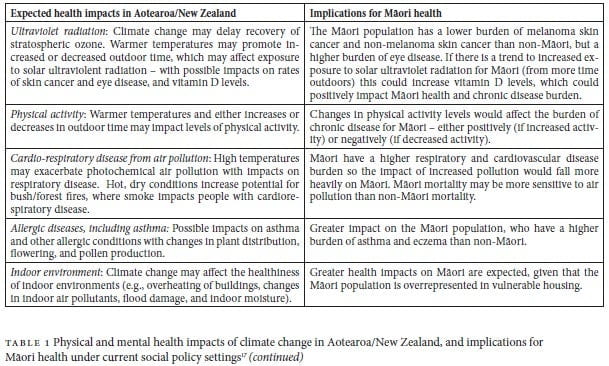
Table 1 outlines some of the expected physical and mental health impacts of climate change for New Zealanders, with a specific focus on the implications for Māori health. The effects described here are not intended to be exhaustive, but rather provide examples of the major mechanisms by which climate change can be expected to impact health and well-being. This information is derived from an extensive literature review and analysis undertaken by the New Zealand College of Public Health Medicine in the production of their 2013 Policy Statement on Climate Change.16
Wider impacts on the determinants of health
There are a number of ways in which climate change impacts on the wider cultural, social, and economic determinants of health for Māori. It is possible that these indirect impacts, mediated through the determinants of health, will become a more significant factor than the direct physical health impacts.18 Experience in recent decades shows that Māori and other socially disadvantaged groups tend to experience disproportionately adverse health outcomes from economic changes that increase social inequality.19
Firstly, indigenous relationships with the natural environment are significant, and Māori explicitly consider a healthy environment to be a prerequisite for good health.20 As with other indigenous peoples, the loss of identity due to displacement and dispossession of lands, resources, and waters (likely to occur with climate change) is intimately linked to adverse physical and mental health outcomes.21
The Māori economy is disproportionately invested in climate-sensitive primary industries, and is likely to experience significant adverse effects from global environmental and socioeconomic trends as a result of climate change.22 Losses in the Māori economy will increase unemployment and reduce average income, thereby affecting the capacity of households to secure the resources necessary for good health.
Poorly planned responses to climate change could also impact health equity through changes in the economic determinants of health. For example, climate change policies that raise costs for fuel and energy (and therefore increase costs of goods and services) without counter-balancing measures, could place extra financial burden on low-income families – disproportionately Māori – affecting ability to afford the basics for good health.23
Health co-benefits from climate action
The challenges posed by climate change are accompanied by considerable opportunities to improve Māori health and reduce health disparities. Many of the actions required by governments and private entities to mitigate and adapt to climate change can have concomitant health benefits in the short to medium term. Measures such as increasing active transport, reducing dietary red meat and animal fat consumption, and improving energy-efficiency in homes could contribute to reductions in heart disease, cancer, obesity, osteoarthritis, Type 2 diabetes, respiratory disease, motor vehicle injuries, and to improvements in mental health.24 However, health co-benefits will not automatically flow from climate action, nor will such benefits inevitably improve equity unless policies and interventions are designed so that the health-related benefits accrue preferentially to those who are most disadvantaged and negative consequences for these groups are avoided or minimized.
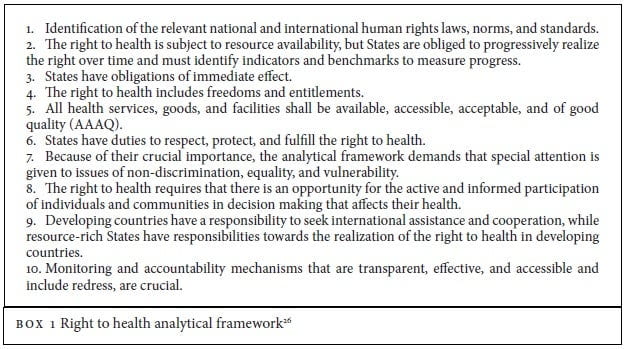
Analysis using a right to health analytical framework
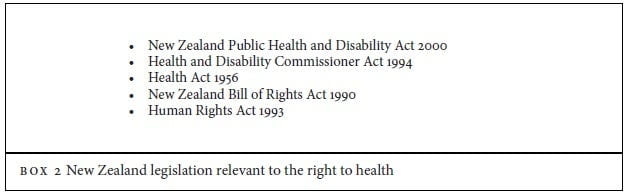
We examined issues related to climate change and Māori health using the right-to-health analytical framework developed by Hunt et al.25 The scope for this analysis included the effects of climate change itself, approaches to minimize climate change by limiting greenhouse gas emissions (mitigation) and future adaptations to a warmer climate (adaptation). The framework applies to all aspects of the right to the highest attainable standard of health, including the determinants of health, and articulates States’ obligations arising from the right to health (Box 1).
The following section considers the obligations of the New Zealand government towards each of the elements of the analytical framework, as it applies to the right to health for Māori in relation to climate change. Some issues apply to more than one element of the framework; in these situations the issue is primarily discussed under the most relevant part of the framework with linkages to other elements identified as appropriate.
1. National and international human rights laws, norms, and standards:
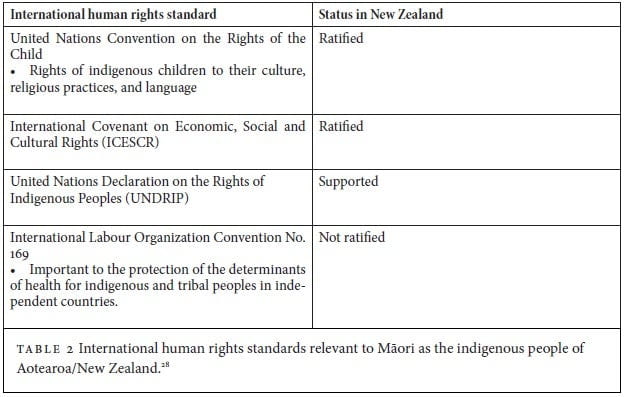
The rights of Māori as indigenous peoples are recognized in Te Tiriti o Waitangi (the 1840 treaty between Māori and the British Crown allowing settlement of Aotearoa/New Zealand), and various domestic laws, including the New Zealand Public Health and Disability Act 2000, which recognizes the principles of the Treaty of Waitangi and establishes mechanisms for Māori participation in decision making about health services.27 There are also a number of international human rights standards that apply to Māori as the indigenous people of Aotearoa/New Zealand (Table 2).
New Zealand has recognized the right to health in its ratification of core human rights treaties, including conventions about racism and the rights of women, children, and persons with disabilities. There are also a number of acts in New Zealand legislation that articulate the right to health (Table 3).29 In particular, the Human Rights Act prohibits direct or indirect discrimination in relation to health status or health services, or in relation to key determinants of health such as employment, housing, and education.
New Zealand is one of 195 parties to the UN Framework Convention on Climate Change (UNFCCC), which originated at the Rio de Janeiro “Earth Summit” in 1992 and entered into force in 1994. The ultimate objective of the UNFCCC is to stabilize greenhouse gas concentrations “at a level that would prevent dangerous anthropogenic (human induced) interference with the climate system.”30 New Zealand is also a member of the Intergovernmental Panel on Climate Change (IPCC), and by endorsing its reports, the New Zealand government acknowledges its scientific authority.
2. Resource constraints, progressive realization, and indicators
Notwithstanding resource constraints, States have an obligation to move as quickly as possible towards the full realization of Article 12 of ICESCR (the right of everyone to the enjoyment of the highest attainable standard of physical and mental health).31 Retrogressive measures—that is, a worsening of health indicators—are not permissible. The equal right to health of indigenous people is explicit in UNDRIP.32 Any deterioration in health-related outcomes, or increase in inequities, needs to be justified.
There are several implications of progressive realization for Māori. New Zealand should be taking active measures to improve the health of Māori, irrespective of climate change. Because climate change is likely to be retrogressive (significantly worsen Māori health and exacerbate inequities), governments should take all possible steps within resource constraints to limit the extent of climate change. These mitigation measures should be carried out in such a way as to support the progressive realization of the right to health of Māori, including policies that have direct, pro-equity, health benefits. Any steps that are taken to adapt to climate change (such as relocation of coastal communities prone to sea level rise or storm surges) should be accompanied by measures to mitigate any negative effects on Māori wellbeing. Measuring progress requires systems to monitor Māori health outcomes for climate-sensitive conditions, as discussed further in the section “Monitoring and accountability.”
3. Obligations of immediate effect
Some obligations arising from the right to health are subject to neither resource constraints nor progressive realization, but are of immediate effect. Hunt and Khosla argue that climate change is such an extremely grave risk to health that States have a core obligation to take immediate action to slow down and reverse climate change.33 The duty to avoid discrimination on the basis of characteristics such as race, sex, language, religion, political views, and disability is also effective immediately. This obligation requires the New Zealand government to urgently address any climate-related policies or practices that discriminate against Māori.
The Emissions Trading Scheme (ETS), which has been the main policy tool chosen by successive governments to address climate change in Aotearoa/New Zealand, was relatively weak at its inception and has been successively amended such that taxpayers now subsidize 95% of emissions for large industrial polluters, and the agricultural sector is excluded from the scheme.34 The weak ETS and lack of other effective policy tools, combined with a number of exacerbating factors, mean that gross domestic greenhouse gas emissions are continuing to rise in New Zealand. This represents a failure to meet the obligation of immediate action in response to the threat posed by climate change.
4. Freedoms and entitlements
This includes freedom from discrimination in the design and implementation of climate policies (including freedom from barriers to adaptation), as well as entitlement to protection from climate change-related harm and an adequate quality of health care.35 For Māori in Aotearoa/New Zealand, entitlements include protection from climate-related destruction of taonga (treasured things, whether tangible or intangible) that support positive health outcomes.
These requirements signal the need for much more comprehensive risk assessment methods to identify climate risks for Māori communities and develop appropriate adaptation measures. Māori communities face a number of barriers to adaptation including lack of access to quality technical advice, exclusion from local and regional planning processes, lack of capital to invest in climate-resilient infrastructure, and other constraints on the ability to modify resource use such as the regulatory, legal, and quota regimes imposed on Māori land and resource use.36 These adaptation barriers increase the risk of harm to health and the determinants of health from climate change.
Indigenous rights also include an entitlement to self-determination (UNDRIP Article 3), including in relation to climate change-related issues.37 This requires provision for meaningful engagement in political and other processes that have a bearing on the right to health (UNDRIP Article 18).38 In Aotearoa/New Zealand, this means that iwi (Māori tribal organizations) need to be fully engaged in decision making on issues that affect their taonga, including health. In relation to climate change, this includes fossil fuel exploration, agricultural intensification, transport projects, the ETS, and other policy proposals to address climate change.
UNDRIP recognizes the rights of indigenous peoples to their ongoing spiritual relationship with their traditional lands, territories, seas, coastal waters, and resources (Article 25), and the conservation and protection of the environment (Article 29).39 These rights are among the underpinnings of the health of indigenous peoples (see below, under “Active and informed participation”) and will be violated profoundly by climate change.
5. Available, accessible, acceptable, and of good quality (AAAQ)
Current inequities in access to, acceptability of, and quality of care need to be addressed; the New Zealand government must be held accountable for progressively reducing and eliminating these inequities. Projected climate change impacts need to be considered in future health system design to ensure that it has the capacity to achieve the AAAQ requirements in the face of increased need. Health service development must be prioritized to ensure these rights are achieved for Māori and other populations likely to be hardest hit by climate change.
The lack of an effective ETS, as discussed under “Obligations of immediate effect,” has significant implications for New Zealand’s ability to meet these health sector needs. The opportunity cost of having an ETS that is largely taxpayer subsidized means that there are reduced public funds available for critical health and social services and constraints on the ability of the government to address current health and social inequities for Māori.
Another missed opportunity is the current failure of New Zealand’s health system to save costs by lowering carbon use. Several analyses show that it is possible to make significant cost savings by implementing sustainability/low carbon initiatives in health care systems. Cost savings could then be reinvested in health services and initiatives to reduce health inequities for Māori.40
6. Respect, protect, fulfill
Respecting the right to health involves ensuring that government action or inaction does not undermine the rights of Māori in relation to health. Dramatic and urgent action is required by all governments, individually and collectively, to reduce the risk of catastrophic climate change. For many societies, including Aotearoa/New Zealand, such action will require fundamental changes to the way we live. There is no way of avoiding significant impact on the determinants of health, but positive effects can be promoted and negative effects minimized. It is possible for the New Zealand government to take a responsible approach to emissions reduction while at the same time meeting its obligations in regards to health and human rights for Māori (and everyone else). In order to uphold the right to health, emissions reductions are needed, and these reductions need to be managed in a way that upholds the right to health.
Protecting the right to health means ensuring that third parties do not interfere with attainment of this right. Global greenhouse gas emissions, if allowed to continue unabated, clearly pose a threat to Māori health (as they do to everyone’s health). If the New Zealand government fails to restrict domestic greenhouse gas emissions to a level commensurate with an acceptable degree of risk, it is neglecting its obligation to protect the right to health. If it is not a responsible partner in the development of strong international agreements to mitigate climate change, it is further neglecting this obligation.
Fulfilling the right to health means States must ensure (among other things) provision of health care and equitable access to the determinants of health. This has important implications for the New Zealand government in relation to preventing or mitigating adverse impacts of climate change on Māori. For example, climate change is likely to impact on primary industries including fisheries in which Māori have considerable economic interests. Without appropriate action, this could result in negative socioeconomic consequences for Māori communities, thereby undermining the right to health. Fulfilling the right to health also implies a contribution towards climate change adaptation for Māori communities.
7. Non-discrimination, equality, and vulnerability
Responses to climate change require urgent measures to substantially reduce the burning of fossil fuels. Economic instruments to achieve this, such as the ETS, have the potential to be regressive, adversely affecting the most vulnerable. Effective increases in the cost of carbon generally flow through into higher costs for goods and services, placing a particular burden on those with the lowest disposable incomes.41 Without explicit attention, Māori will be disproportionately affected, which constitutes discrimination in access to key determinants of health and will be retrogressive rather than achieving progressive realization to the right to the determinants of health.
Other climate change policies have the potential to discriminate against Māori, as noted in a series of meetings with Māori in 2007. Large emitters in the agricultural and transport sectors are not liable for their emissions whilst iwi are potentially disadvantaged in a number of ways. For example, iwi who had forested land returned to them as part of a Treaty of Waitangi settlement could be penalized for changing the land use. Pre-1990 forests, many of which are on Māori land, are not eligible for carbon credits under the ETS, while “new” forests are eligible.42
Further, the lack of effective action to reduce emissions has significant implications for intergenerational equity. There are likely to be overwhelming carbon budget fiscal issues for future governments and for younger New Zealanders as the nation is left behind in the global transition to a low-carbon economy. Māori, along with many other indigenous peoples, place high value on future generations. These indigenous values call for action in the current generation to avoid placing an excessive burden on future generations. Māori make up an increasing proportion of New Zealand’s young people and stand to bear an unfair burden as a result of recent and current governments’ failure to adequately respond to climate change.43
Obligations to avoid discrimination and to achieve progressive realization of the right to health require States to align climate, health, and equity goals. Policies to avoid regressive outcomes are required, both to avoid penalizing the poor and to maximize health co-benefits for low-income population groups. Experience elsewhere shows that this is possible.44 An example of a government initiative seeking to achieve positive impacts for Māori health (and which will concomitantly impact on climate change) is the Warm Up New Zealand: Healthy Homes Programme. Under the program, the Energy Efficiency Conservation Authority will provide grants for up to 60% of the cost of home insulation and project partners (e.g., trusts, primary health organizations, and iwi) will top up the government grants. The program will be targeted at households (including renters) with high health risk, including those with children and/or elderly members. In addition to energy efficiency gains, insulating homes protects against the effects of heat waves and reduces health problems associated with cold, damp housing, which is prevalent in Aotearoa/New Zealand and which disproportionately affects the Māori population.45
8. Active and informed participation
This means that Māori should be actively involved in setting priorities about climate change and health, decision-making processes, delivery of mitigation and adaptation programs, and holding duty-bearers to account. Participation is a key human rights concept, signifying a need to address political marginalization of Māori and give expression to tino rangatiratanga (self-determination), as stated in Te Tiriti o Waitangi and obligations under the Declaration on the Rights of Indigenous Peoples. There is evidence that these obligations have not been met; in a series of consultation meetings in 2007, Māori noted that climate change policy development in the early 2000s lacked a Treaty of Waitangi context, and that there was a lack of partnership with Māori in developing climate change policy.46
Meaningful participation, and respect for Māori rights to self-determination under the Declaration on the Rights of Indigenous Peoples, requires recognizing Māori concepts of health. Māori and other indigenous peoples have a long history of natural resource management, as well as having clear kaitiakitanga (guardianship) rights and responsibilities. Their traditional ecological knowledge and expertise means they have much to contribute to developing and implementing effective, sustainable mitigation and adaptation strategies. In the 2007 consultation between the Ministry for the Environment and Māori, Māori emphasized that the government could make better use of Māori knowledge on sustainability and environmental stewardship. Concern was also expressed about the use of economic instruments such as carbon trading and the commodification of resources to address climate change, noting that this approach was not a good fit with Māori worldviews on the environment and the kaitiakitanga role.47
9. International assistance and cooperation
The implications of this obligation in respect to climate change are twofold. First, New Zealand is currently violating the right to health in other countries, particularly developing countries, by contributing to unsafe concentrations of atmospheric greenhouse gases. New Zealand is a relatively high emitter of greenhouse gases, with the fifth highest per capita emissions among developed countries that took on commitments under the UNFCCC.48 Its disproportionately high historical contribution means that the onus is on New Zealand to urgently and substantially reduce its emissions.
Second, with regard to its participation in international forums, New Zealand must ensure that due account is taken of the right to health, particularly for people in developing countries. Its role in international climate negotiations needs to include advocacy for fair and equitable approaches to the allocation of emissions reductions amongst countries which take into account overall carbon budgets, historical responsibility, and capability to mitigate.49 New Zealand is well placed to support and assist development of international linkages between indigenous peoples in resource-rich as well as low- and middle-income countries. These actions are important for the well-being of all people, and especially so for indigenous peoples and other groups who will be most seriously affected by climate change.
10. Monitoring and accountability
Hunt and Khosla explain that accountability mechanisms in relation to climate change are urgently needed. Climate change is already leading to the dispossession of land for indigenous peoples in small island nations.50 States have obligations under UNDRIP to provide mechanisms for redress when indigenous peoples are deprived of their lands and resources (Article 2) as well as obligations of redress for serious violations of the right to health, including its determinants.51
In order to ensure that the determinants of health are not being adversely affected, indicators are also required to monitor climate-sensitive economic and social outcomes for Māori. To date, there has been little work to identify the relevant indicator sets or to monitor progress, despite New Zealand having excellent datasets that could be used. Systems to monitor these indicators must be effective and transparent, and must include accountability mechanisms that apply to all relevant public and private interests.52
Conclusion
There is very little international literature on the impact of climate change on indigenous peoples’ health. This is also evident in Aotearoa/New Zealand; despite being a comparatively well-resourced country, the New Zealand College of Public Health Medicine policy on climate change is the first health-focused assessment of climate change impacts on Māori.53 Our analysis extends this assessment by using a right to health analytical framework to examine the implications of climate change for Māori as the indigenous population of Aotearoa/New Zealand.
One of the limitations of this paper is that, as a case study of Māori in Aotearoa/New Zealand, it does not reflect the diversity of issues affecting indigenous populations worldwide. We have used a general analytical framework that was not specifically developed to consider the needs of indigenous peoples. However, given similarities in the underlying conditions that drive health outcomes and in rights-based instruments, our analysis is likely to have relevance for indigenous peoples internationally.54
New Zealand, having ratified human rights treaties that include the right to health, must be accountable to its obligations within a right to health framework. It is clear that climate change and both mitigation and adaptation to climate change pose serious threats to the right to health for Māori in Aotearoa/New Zealand. The New Zealand government has obligations arising from this right to address a broad range of issues at many different levels. The analysis we have conducted identifies a number of important areas where the government is currently failing to meet these obligations, as well as future measures that are required in order to avoid further encroaching on the right to health.
Systems for monitoring and accountability are conspicuously lacking: no specific indicators for Māori exist and the ability to conduct an equity-focused health impact assessment is limited. Indeed, no government agency has undertaken a comprehensive assessment of the health effects of climate change for Māori. When compared with the range and quality of data and the processes for accountability that exist generally in the health sector, New Zealand’s performance in relation to this aspect of the right to health is a significant cause for concern.
Another area in which the government response has been particularly inadequate is in relation to active participation and self-determination. To date, there has been extremely limited engagement with Māori in the development of climate change policy, either for mitigation or adaptation. Again, this compares poorly with acknowledgment of the need for active participation of Māori in health sector legislation, policies, and provision of health services.
Overall, the Aotearoa/New Zealand government is not currently meeting its obligations in relation to progressive realization. Even without considering the likely impacts of climate change, Māori health and social outcomes in some areas are static or deteriorating. Unless explicit attention is paid to mitigation policies with health co-benefits that reduce inequities, New Zealand climate change policies risk worsening the state of Māori health.
Our right to health analysis highlights implications for adoption of climate policies and interventions. Some approaches to climate change mitigation have clear health co-benefits and align with equity goals, and should be adopted immediately with appropriate monitoring and evaluation. Other strategies designed to reduce greenhouse gas emissions do not have automatic co-benefits for health or are potentially regressive. Such interventions need to be designed, implemented, and evaluated carefully in partnership with indigenous communities in order to promote equity and achieve progressive realization of the right to health.
Climate change, if allowed to continue unchecked, is incompatible with progressive realization of the right to health. This implies an obligation on the New Zealand government and other States to: (1) actively, dramatically, and urgently reduce domestic greenhouse gas emissions, and; (2) take all possible steps to achieve a dramatic and urgent reduction in global greenhouse gas emissions through international negotiations and other mechanisms. Further, given that some degree of global warming is now unavoidable, all governments and States have obligations to prepare for the impact of climate change and to support indigenous communities with adaptation. Research and tools to assess equity and health impacts of climate change, and of policies to address climate change, are urgently needed.
In responding to the threat of climate change, it is essential to not only provide for indigenous self-determination, but also to recognize the contribution indigenous peoples can make to climate change mitigation and adaptation approaches that benefit all people. Climate change can be seen as the result of an excessive emphasis on Western development and a devaluing of indigenous ways of knowing and ways of relating to the environment. Upholding indigenous rights to guardianship of the natural environment has the potential to provide solutions to the challenge of climate change for all of humanity.
Rhys Jones, MBChB, MPH, is a Public Health Physician and Senior Lecturer in Te Kupenga Hauora Māori, Faculty of Medical and Health Sciences, University of Auckland, Auckland, New Zealand.
Hayley Bennett, MBChB, MPH, is a Public Health Physician in Rotorua, New Zealand.
Gay Keating, MBChB, is a Public Health Physician at Eru Pōmare Māori Health Research Centre, Department of Public Health, University of Otago Wellington School of Medicine and Health Sciences, New Zealand.
Alison Blaiklock, MBChB, MPHTM is a Public Health Physician and Honorary Senior Clinical Lecturer, Department of Public Health, University of Otago Wellington, New Zealand.
Corresponding author: Rhys Jones, email: rg.jones@auckland.ac.nz.
References
1. A.J. McMichael, “Globalization, climate change, and human health,” New England Journal of Medicine 368/14 (2013), pp.1335-1343. Available at http://www.nejm.org/doi/full/10.1056/NEJMra1109341; C.D. Butler and D. Harley, “Primary, secondary and tertiary effects of eco-climatic change: the medical response,” Postgrad Med J 86 (2010), pp.230-234; A. Costello, M. Abbas, A. Allen et al., “Managing the health effects of climate change,” Lancet 373 (2009), pp.1693-1733. Available at http://www.thelancet.com/journals/lancet/article/PIIS0104-6736(09)60935-1/fulltext; K. R. Smith, A. Woodward, D. Campbell-Lendrum, et al., “Human health: Impacts, adaptation, and co-benefits,” in C. B. Field, V. R. Barros, M. D. Mastrandrea, K. J. Mach, et al. (eds), Climate change 2014: Impacts, adaptation and vulnerability. Contribution of Working Group II to the Fifth Assessment Report of the Intergovernmental Panel on Climate Change (Cambridge: IPCC, 2014). Available at http://ipcc-wg2.gov/AR5/images/uploads/WGIIAR5-Chap11_FGDall.pdf.
2. M. Ezzati, A.D. Lopez, A. Rodgers et al. (eds), Comparative quantification of health risks: The global and regional burden of disease attributable to selected major risk factors (Geneva: World Health Organization, 2004); DARA International and the Climate Vulnerable Forum, Climate vulnerability monitor, 2nd edition: A guide to the cold calculus of a hot planet (DARA International and the Climate Vulnerable Forum, 2012). Available at http://daraint.org/climate-vulnerability-monitor/climate-vulnerability-monitor-2012/report/.
3. McMichael (2013, see note 1); Butler et al. (2010, see note 1); Costello et al. (2009, see note 1); Smith et al. (2014, see note 1); New Zealand College of Public Health Medicine (NZCPHM), Substantive policy statement on climate change 2013 (NZCPHM, 2013). Available at http://www.nzcphm.org.nz/media/67575/2013_11_6_climate_change_substantive_policy__final-corrected_.pdf
4. Smith et al. (2014, see note 1).
5. World Health Organization and World Meterological Association, Atlas of health and climate (Geneva: WHO, 2012). Available at http://www.who.int/globalchange/publications/atlas/en/index.html; DARA International (2012, see note 2); J. Hosking, R. Jones, T. Percival, N. Turner, and S. Ameratunga, “Climate change: The implications for child health in Australasia,” Journal of Paediatrics and Child Health 47/8 (2011), pp. 493-96. Available at http://onlinelibrary.wiley.com/doi/10.1111/j.1440-1754.2010.01699.x/full; S. Friel, M. Marmot, A.J. McMichael et al., “Global health equity and climate stabilisation: A common agenda,” Lancet 372 (2008), pp.1677-1683. Available at http://www.sciencedirect.com/science/article/pii/S014067360861692X.
6. United Nations Department of Economic and Social Affairs, State of the world’s indigenous peoples (New York: UNESA, 2009), p. 119. Available at http://www.un.org/esa/socdev/unpfii/documents/SOWIP_web.pdf
7. Statistics New Zealand, 2013 Census QuickStats about Māori (Wellington: Statistics New Zealand, 2013). Available at http://www.stats.govt.nz.
8. M. Durie, Whaiora: Māori health development, 2nd ed. (Auckland: Oxford University Press, 1998); R.J. Walker, Ka Whawhai Tonu Matou, revised ed. (Auckland: Penguin, 2004).
9. P. Reid and B. Robson (eds), Hauora Māori standards of health IV (Wellington: Te Rōpū Rangahau Hauora A Eru Pōmare, 2007). Available at http://www.fmhs.auckland.ac.nz/faculty/tkhm/tumuaki/_docs/hauora.pdf; Ministry of Health, The health of Māori adults and children (Wellington: Ministry of Health, 2013). Available at http://www.health.govt.nz/publication/health-maori-adults-and-children; Ministry of Health, Tatau kahukura: Māori health chartbook 2010, 2nd ed (Wellington: Ministry of Health, 2010). Available at http://www.health.govt.nz/publication/tatau-kahukura-maori-health-chart-book-2010-2nd-edition; Ministry of Health, Health loss in New Zealand: A report from the New Zealand Burden of Diseases, Injuries and Risk Factors Study 2006–2016, Statistical Annexe Maori/Non-Maori DALY rate ratio by condition (Wellington: Ministry of Health, 2013). Available at http://www.health.govt.nz/system/files/documents/publications/workbook-3-nzbd-inequalities-2006.xlsx; P. Davis, R. Lay-Yee, L. Dyall L et al., “Quality of hospital care for Māori patients in New Zealand: Retrospective cross-sectional assessment,” Lancet 367 (2006), pp.1920-1925; B. Robson, G. Purdie and D. Cormack, Unequal impact: Māori and non-Māori cancer statistics 1996-2001 (Wellington: Ministry of Health, 2006). Available at http://www.health.govt.nz/publication/unequal-impact-maori-and-non-maori-cancer-statistics-1996-2001; C. Tukuitonga and A. Bindman, “Ethnic and gender differences in the use of coronary artery revascularisation procedures in New Zealand,” New Zealand Medical Journal 115/1152 (2002), pp.179-182. Available at https://researchspace.auckland.ac.nz/bitstream/handle/2292/4506/12044000.pdf?sequence=1; S. Hill, D. Sarfati, T. Blakely, et al., “Ethnicity and management of colon cancer in New Zealand: Do indigenous patients get a worse deal?” Cancer 116 (2010), pp. 3205-3214. Available at http://www.ncbi.nlm.nih.gov/pubmed/20564634; S. Crengle, E. Robinson, C. Grant et al., “Pharmacological management of children’s asthma in general practice: Findings from a community-based cross-sectional survey in Auckland, New Zealand,” New Zealand Medical Journal 124 (2011), pp. 44–56. Available at http://journal.nzma.org.nz/journal/124-1346/4969/content.pdf; T.Gillies, A.Tomlin, S. Dovey et al., “Ethnic disparities in asthma treatment and outcomes in children aged under 15 years in New Zealand: Analysis of national databases,” Primary Care Respiratory Journal 22 (2013), pp. 312–318. Available at http://www.thepcrj.org/journ/view_article.php?article_id=1051.
10. A. Haines, P. Wilkinson, C. Tonne et al., “Aligning climate change and public health policies,” Lancet 374/9707 (2009), pp.2035-8. Available at http://www.thelancet.com/journals/lancet/article/PIIS0140-6736(09)61667-6/fulltext; D. Campbell-Lendrum, R. Bertollini, M. Neira et al., “Health and climate change: A roadmap for applied research’” Lancet 373/9676 (2009), pp. 1663-1665. Available at http://www.thelancet.com/journals/lancet/article/PIIS0140-6736(09)60926-0/fulltext.
11. Editorial, “Intersection 1: Rights and responsibilities amid climate change and environmental degradation,” Health and Human Rights 13/1 (2011), pp. 4-6.
12. UN Committee on the Rights of the Child, General Comment No. 15 (2013). Available at http://www.crin.org/docs/CRC-C-GC-15_en-1.pdf.
13. Durie (1998, see note 7); M. Durie, “Te Pae Mahutonga: a model for Māori health promotion” (Health Promotion Forum of New Zealand newsletter 49, 1999).
14. United Nations Development Group (UNDG), “Guidelines on indigenous peoples’ issues” (Geneva: United Nations, 2008). Available at http://www.undg.org/index.cfm?P=270.
15. D.N. King, G. Penny, and S. Severne, “The climate change matrix facing Māori society” in R. A. Nottage, D. S. Wratt, J. F Bornman, et al., (eds), Climate change adaption in New Zealand: Future scenarios and some sectoral perspectives (Wellington: New Zealand Climate Change Centre, 2010). Available at http://www.nzclimatechangecentre.org/sites/nzclimatechangecentre.org/files/images/research/
Climate%20Change%20Adaptation%20in%20New%20Zealand%20(NZCCC)%20high%207.pdf
16. NZCPHM (2013, see note 3).
17. NZCPHM (2013, see note 3); S. Hales, T. Blakely, and A. Woodward, “Air pollution and mortality in New Zealand: Cohort study,” Journal of Epidemiology and Community Health 66/5 (2012), pp. 468-73.
18. King et al (2010, see note 14); A. Reisinger, B. Mullan, and M. Manning, “Global and local climate change scenarios to support adaption in New Zealand,” in: R. A. Nottage, D. S. Wratt, J. F. Bornman et al., (eds), Climate change adaptation in New Zealand: Future scenarios and some sectoral perspectives (see note 15), pp. 26-43; Howden-Chapman, R. Chapman, S. Hales et al., “Climate change and human health: Impact and adaptation issues for New Zealand,” in R. A. Nottage, D. S. Wratt, J. F. Bornman et al., (eds), Climate change adaptation in New Zealand: Future scenarios and some sectoral perspectives (see note 15), pp. 112-121.
19. M. Tobias, T. Blakely, D. Matheson, K. Rasanathan and J. Atkinson, “Changing trends in indigenous inequalities in mortality: lessons from New Zealand,” International Journal of Epidemiology 38 (2009), pp. 1711-1722.
20. Durie (1999, see note 13).
21. Committee on Indigenous Health, The Geneva Declaration on the Health and Survival of Indigenous Peoples (Geneva: World Health Organization, 1999).
22. King et al. (2010, see note 15); Reisinger et al. (2010, see note 18); Office of the Prime Minister’s Chief Science Advisor, New Zealand’s changing climate and oceans: the impacts of human activity and implications for the future (Wellington: PMCSA, 2013). Available at http://www.pmcsa.org.nz/wp-content/uploads/New-Zealands-Changing-Climate-and-Oceans-report.pdf
23. D. Dhar, A. Macmillan, G. Lindsay et al., “Carbon pricing in New Zealand: Implications for public health,” New Zealand Medical Journal 122/1290 (2009), pp.105-115. Available at http://journal.nzma.org.nz/journal/122-1290/3483/
24. M. Chan, “Cutting carbon, improving health,” Lancet 374/9705 (2009), pp. 1870-1871. Available at http://www.thelancet.com/journals/lancet/article/PIIS0140-6736%2809%2961759-1/fulltext; A. Haines, A.J. McMichael, K.R. Smith et al., “Public health benefits of strategies to reduce greenhouse-gas emissions: overview and implications for policy makers,” Lancet 374/9707 (2009), pp. 2104-2114. Available at http://www.thelancet.com/journals/lancet/article/PIIS0140-6736(09)61759-1/fulltext; J.J. West, S.J. Smith, R.A. Silva et al., “Co-benefits of mitigating global greenhouse gas emissions for future air quality and human health,” Nature Climate Change 3 (2013), pp. 885–889. Available at http://www.nature.com/nclimate/journal/v3/n10/full/nclimate2009.htm; A. Haines, P. Wilkinson, C. Tonne, and I. Roberts, “Aligning climate change and public health policies,” Lancet 374/9707 (2009), pp. 2035-2038. Available at http://www.thelancet.com/journals/lancet/article/PIIS0140-6736(09)61667-6/fulltext; J. Woodcock, P. Edwards, C. Tonne et al., “Public health benefits of strategies to reduce greenhouse-gas emissions: urban land transport,” Lancet 374/9705 (2009), pp. 1930-1943. Available at http://www.thelancet.com/journals/lancet/article/PIIS0140-6736%2809%2961714-1/fulltext; S. Friel, A.D. Dangour, T. Garnett et al, “Public health benefits of strategies to reduce greenhouse-gas emissions: food and agriculture,” Lancet 374/9706 (2009), pp. 2016-2025. Available at http://www.thelancet.com/journals/lancet/article/PIIS0140-6736(09)61753-0/fulltext; P. Wilkinson, K.R. Smith, M. Davies et al., “Public health benefits of strategies to reduce greenhouse-gas emissions: household energy,” Lancet 374/9705 (2009), pp. 1917-1929. Available at http://www.thelancet.com/journals/lancet/article/PIIS0140-6736%2809%2961713-X/fulltext.
25. P. Hunt, G. Backman et al., “The right to the highest attainable standard of health,” in R. Detels, R. Beaglehole, M. A. Lansang, and M. Gulliford (eds), Oxford Textbook of Public Health (Oxford: Oxford University Press, 2009).
26. Ibid
27. Te Tiriti O Waitangi (The Treaty of Waitangi). Available at http://www.waitangi-tribunal.govt.nz/treaty/kawharutranslation.asp; The New Zealand Public Health and Disability Act 2000, New Zealand Legislation. Available at: http://www.legislation.govt.nz/act/public/2000/0091/latest/DLM80051.html.
28. Convention on the Rights of the Child (CRC), G.A. Res. 44/25 (1989). Available at http://www2.ohchr.org/english/law/crc.htm; International Covenant on Economic, Social and Cultural Rights (ICESCR), G.A. Res. 2200A (XXI), (1966). Available at http://www.ohchr.org/EN/ProfessionalInterest/Pages/CESCR.aspx; United Nations Declaration on the Rights of Indigenous Peoples (UNDRIP), G.A. Res. 61/295 (2007). Available at http://www.un.org/esa/socdev/unpfii/documents/DRIPS_en.pdf; International Labour Organization (ILO), “Indigenous and Tribal Peoples Convention”, Convention No. 169, (1989). Available at http://www.ilo.org/indigenous/Conventions/no169/lang–en/index.htm
29. NZPHDA (2000, see note 27); The Health and Disability Commissioner Act 1994, New Zealand Legislation. Available at http://www.legislation.govt.nz/act/public/1993/0082/latest/DLM304212.html; The Health Act 1956, New Zealand Legislation. Available at http://www.legislation.govt.nz/act/public/1956/0065/latest/DLM305840.html; The New Zealand Bill of Rights Act 1990, New Zealand Legislation. Available at http://www.legislation.govt.nz/act/public/1990/0109/latest/DLM224792.html; The Human Rights Act 1993, New Zealand Legislation. Available at http://www.legislation.govt.nz/act/public/1993/0082/latest/DLM304212.html.
30. United Nations, United Nations Framework Convention on Climate Change (Rio de Janeiro: United Nations, 1992). Available at http://unfccc.int/essential_background/convention/items/6036.php
31. International Covenant on Economic, Social and Cultural Rights (ICESCR), G.A. Res. 2200A (XXI), Art. 12. (1966). Available at http://www.ohchr.org/EN/ProfessionalInterest/Pages/CESCR.aspx
32. UNDRIP (2007, see note 28).
33. P. Hunt and R. Khosla,“Climate change and the right to the highest attainable standard of health,” in S. Humphreys, Human rights and climate change (Cambridge: Cambridge University Press, 2009), pp. 238-256.
34. Parliamentary Commissioner for the Environment, Submission on the Climate Change (Emissions Trading and Other Matters) Amendment Bill (Wellington: Parliamentary Commissioner for the Environment, 2012). Available at http://www.pce.parliament.nz/assets/Uploads/PCE-Submission-on-the-Climate-Change-Amendment-Bill.pdf; N. Wilson, R. Chapman, and P. Howden-Chapman, “End of term review of the New Zealand government’s response to climate change: A public health perspective,” New Zealand Medical Journal 124/1345 (2011), pp. 90-95. Available at http://journal.nzma.org.nz/journal/124-1345/4949/
35. Hunt et al (2009, see note 25).
36. King et al (2010, see note 15).
37. United Nations Declaration on the Rights of Indigenous Peoples (UNDRIP), G.A. Res. 61/295 (2007), Art. 3. Available at http://www.un.org/esa/socdev/unpfii/documents/DRIPS_en.pdf
38. United Nations Declaration on the Rights of Indigenous Peoples (UNDRIP), G.A. Res. 61/295 (2007), Art. 18. Available at http://www.un.org/esa/socdev/unpfii/documents/DRIPS_en.pdf; United Nations Declaration on the Rights of Indigenous Peoples (UNDRIP), G.A. Res. 61/295 (2007), Art. 20. Available at http://www.un.org/esa/socdev/unpfii/documents/DRIPS_en.pdf
39. United Nations Declaration on the Rights of Indigenous Peoples (UNDRIP), G.A. Res. 61/295 (2007), Art. 25. Available at http://www.un.org/esa/socdev/unpfii/documents/DRIPS_en.pdf; United Nations Declaration on the Rights of Indigenous Peoples (UNDRIP), G.A. Res. 61/295 (2007), Art. 29.
40. NHS Sustainable Development Unit, Save Money by Saving Carbon: Decision Making in the NHS Using Marginal Abatement Cost Curves (NHS SDU, 2010). Available at http://www.sduhealth.org.uk/documents/publications/1279123659_ljvk_save_money_by_saving_carbon.pdf; S. Kaplan, B. Sadler, K. Little et al, Can sustainable hospitals help bend the health care cost curve? (Commonwealth Fund Issue Brief, 2012). Available at http://www.commonwealthfund.org/~/media/Files/Publications/Issue%20Brief/2012/Nov/
1641_Kaplan_can_sustainable_hosps_bend_cost_curve_ib.pdf
41. Dhar et al (2009, see note 23).
42. Ministry for the Environment, Consultation with Māori on climate change: Hui report (Wellington: Ministry for the Environment, 2007). Available at http://www.mfe.govt.nz/publications/climate/consultation-maori-hui-report-nov07/consultation-maori-hui-report-nov07.pdf
43. Ministry for the Environment, New Zealand’s greenhouse gas inventory and net position report 1990-2011, snapshot April 2013 (Wellington: Ministry for the Environment,2013). Available at http://www.mfe.govt.nz/publications/climate/greenhouse-gas-inventory-2013/index.html; Hon. Tim Groser, New Zealand commits to 2020 climate change target (Wellington: 16 August, 2013). Available at http://beehive.govt.nz/release/new-zealand-commits-2020-climate-change-target; The Sustainability Council of New Zealand, The carbon budget deficit (Wellington: The Sustainability Council, 2012). Available at http://www.sustainabilitynz.org/wp-content/uploads/2013/02/TheCarbonBudgetDeficit.pdf; Te Puni Kokiri, Kei tua i te 2020: Te taupori Māori. Beyond 2020: Population projections for Māori (Wellington: Te Puni Kokiri, 2010). Available at http://www.tpk.govt.nz/en/in-print/our-publications/fact-sheets/beyond-2020-population-projections-for-maori/download/tpk-beyond-2020-population-projections-2010-en.pdf
44. Dhar et al (2009, see note 23).
45. P. Howden-Chapman, A. Matheson, H. Viggers et al., “Retrofitting houses with insulation to reduce health inequalities: results of a clustered, randomised trial in a community setting,” British Medical Journal 334 (2007), pp.460-464. Available at http://www.bmj.com/content/334/7591/460.
46. Ministry for the Environment (2007, see note 42).
47. Ibid
48. Ministry for the Environment (2013, see note 43).
49. Oxfam International, Hang together or separately? How global co-operation is key to a fair and adequate climate deal at Copenhagen (Oxfam: Briefing Paper 128, 2009). Available at http://www.oxfam.org/en/policy/fair-climate-deal-copenhagen, http://policy-practice.oxfam.org.uk/publications/hang-together-or-separately-how-global-cooperation-is-key-to-a-fair-and-adequat-114525; R. Stott, “Contraction and convergence: the best possible solution to the twin problems of climate change and inequity,” British Medical Journal 344/e1765 (2012), doi: 10.1136/bmj.e1765. Available at http://www.bmj.com/content/344/bmj.e1765.
50. N. Mimura, L. Nurse, R.F. McLean et al., “Small islands,” in M.L. Parry, O.F. Canziani, J.P. Palutikof, P.J. van der Linden, and C.E. Hanson (eds), Climate Change 2007: Impacts, Adaptation and Vulnerability. Contribution of Working Group II to the Fourth Assessment Report of the Intergovernmental Panel on Climate Change (Cambridge: IPCC, 2007); 687-716.
51. UNDRIP (2007, see note 28).
52. Hunt and Khosla (2009, see note 33).
53. NZCPHM (2013, see note 3).
54. UNESA (2009, see note 6).