International obligations through collective rights: Moving from foreign health assistance to global health governance
Benjamin Mason Meier and Ashley M. Fox
Health and Human Rights 12/1
Published June 2010
Abstract
This article analyzes the growing chasm between international power and state responsibility in health rights, proposing an international legal framework for collective rights — rights that can reform international institutions and empower developing states to realize the determinants of health structured by global forces. With longstanding recognition that many developing state governments cannot realize the health of their peoples without international cooperation, scholars have increasingly sought to codify international obligations under the purview of an evolving human right to health, applying this rights-based approach as a foundational framework for reducing global health inequalities through foreign assistance. Yet the inherent limitations of the individual human rights framework stymie the right to health in impacting the global institutions that are most crucial for realizing underlying determinants of health through the strengthening of primary health care systems. Whereas the right to health has been advanced as an individual right to be realized by a state duty-bearer, the authors find that this limited, atomized right has proven insufficient to create accountability for international obligations in global health policy, enabling the deterioration of primary health care systems that lack the ability to address an expanding set of public health claims. For rights scholars to advance disease protection and health promotion through national primary health care systems — creating the international legal obligations necessary to spur development supportive of the public’s health — the authors conclude that scholars must look beyond the individual right to health to create collective international legal obligations commensurate with a public health-centered approach to primary health care. Through the development and implementation of these collective health rights, states can address interconnected determinants of health within and across countries, obligating the international community to scale-up primary health care systems in the developing world and thereby reduce public health inequities through global health governance.
Introduction
The human right to health is thought to have evolved from an individual right of persons against a single governmental duty-bearer to a collective right of peoples against myriad duty-bearers throughout the world. Yet in spite of this rights-based recognition of globalized determinants of health, these evolving human rights claims remain imprecise in creating international legal obligations to meet global health priorities. With advocates challenging all manner of powerful actors — public and private, domestic and foreign, institutional and individual — these inchoate claims have been unable to achieve the global health policies necessary to realize public health improvements in developing countries through primary health care systems.
To the extent that the developed world has assumed any responsibility for global health, this responsibility has been asserted through political commitments that lack enforceability and sustainability. With these fleeting political initiatives funneled largely through foreign assistance programs, such policies have been crafted through rhetorical pleas for charity rather than binding obligations of law. As a result, developing states have faced inconsistent commitments that have impeded the functioning of national primary health care systems — commitments that have become increasingly precarious as the global economic crisis has deepened.
With ethicists positing moral obligations between developed and developing countries — conceptualizing international development aid not as a voluntary, altruistic gesture, but rather as a form of redistributive justice to rectify past and ongoing structural harms — an imperative has arisen to ground these non-binding ethical frameworks in international law. To reassert the authoritative legal frameworks of human rights in global health governance, it is necessary that these frameworks incorporate collective rights, complementing an individual right to health with collective international obligations for public health.
Foreign assistance for global health
Given the persistence of entrenched poverty, developing countries continue to experience high rates of infectious disease, shortened lifespan, and diminished quality of life for large portions of their populations, generating wide epidemiologic rifts between rich and poor countries. At the end of the 20th century, 14% of the world remained undernourished, 16% lacked access to safe drinking water, and 40% lacked basic sanitation — with these wanting masses overwhelmingly congregated in the developing world.1 While health trends have continuously improved at the global level, health gains in many regions have stagnated in step with the increasing immiseration occasioned by international development policy during the 1980s and 1990s, an era of structural adjustment that was characterized by health policy prescriptions for privatization and deregulation.2
Recent attention to these global health inequalities, precipitated by a worldwide movement for HIV treatment access, has resulted in unprecedented increases in health-related foreign assistance to developing countries. To this end, Official Development Assistance (ODA) — government financing for the economic development and welfare of developing countries — nearly doubled between 2001 and 2007, with health-related foreign aid growing by US$14.9 billion.3 In addition, so-called megaphilanthropists and their foundations have begun investing unprecedented billions into global health programs and novel governance systems (for example, public-private partnerships) to develop health technologies for the neglected diseases of the developing world.4 Turning from what many view as their tarnished past, international financial institutions have taken a renewed interest in health-related development financing through such programs as the World Bank’s Health, Nutrition, and Population initiative and its Multi-Country HIV/AIDS Program.5
However, current global health policy, while a vast improvement over the tradition of neglect that has long plagued the world’s poor, has tended to take programmatic form in vertical interventions directed at select diseases — often to the detriment of horizontal primary health care systems directed at underlying determinants of the public’s health (such as potable water, improved sanitation, and basic health infrastructures).6 Given that funding priorities are driven by the strategic interests of donors, the conditionalities attached to these inherently unsustainable foreign assistance programs have proven to be barriers to the effective implementation of global health policy through the strengthening of primary health care systems.7 Further, a substantial portion of this new global health funding has gone toward the development of expensive and technically sophisticated biomedical interventions for a fortunate few, overshadowing the obtainable public health strategies needed to meet basic survival needs for the common good.8
As research has uncovered the harms of these vertical and biomedical approaches to health policy, advocate attention has shifted back to horizontal systems to strengthen primary health care, addressing underlying determinants of health through the provision of public goods, such as water and sanitation systems.9 However, despite growing calls for sector-wide health support under the mantle of “new” or “smart” aid, foreign assistance and international lending continue to bypass the state, with aid given directly to NGOs or channeled through the privatized provision of public goods.10 This uncoordinated response has the potential to undermine the developing state, disadvantaging the national primary health care systems necessary for disease prevention and health promotion.11 As a result, there are growing concerns about how best to “improve the coordination necessary to avoid waste, inefficiency and turf wars” while maintaining the enthusiasm for global health generated by disease-specific political mobilization.12 While foreign assistance remains an important source of needed revenue for health, the current framework cannot realize the public health needs of developing countries without increasing international cooperation and support for national primary health care systems.
Limited evolution of the right to health in codifying international obligations
In reducing global health inequalities through this foreign assistance framework, scholars and advocates have looked increasingly to the authoritative obligations of international human rights law.13 Recognizing that many developing state governments cannot realize the health of their peoples without foreign resources, advocates have increasingly sought to codify international obligations under the purview of the human right to health, using this rights-based approach as a foundation for foreign health assistance. As this right to health has evolved to encompass international obligations, however, it has faced scholarly criticism for exceeding the bounds of international law and has encountered policy limitations in influencing foreign assistance.
This trend toward international obligations began as early as the 1948 Universal Declaration of Human Rights (UDHR), which established, through the United Nations (UN), “a common standard of achievement for all peoples and all nations.”14 The UDHR elaborated a right to health — drawn from negotiations for the 1948 Constitution of the World Health Organization (WHO) — by which the state would seek to realize for each person “a standard of living adequate for the health and well-being of himself and of his family, including food, clothing, housing and medical care and necessary social services.” To achieve this end through global action, a promise set forth in the 1945 UN Charter, the UDHR acknowledged the need for international cooperation in realizing human rights, holding that “[e]veryone is entitled to a social and international order in which the rights and freedoms set forth in this Declaration can be fully realized.”15
Drawing on this international order, the UN’s 1966 International Covenant on Economic, Social and Cultural Rights (ICESCR) extended these international legal obligations for achieving health rights. To realize the ICESCR’s right to health, defined as a “right of everyone to the enjoyment of the highest attainable standard of physical and mental health,” the ICESCR committed states “to take steps individually and through international assistance and cooperation, especially economic and technical, to the maximum of its available resources.”16 With an understanding that such international obligations were necessary for the full realization of human rights, the UN’s specialized agencies took the lead in directing this economic and technical cooperation within their respective areas of competence.17
In moving forward from the ICESCR under this UN mandate, WHO’s “Health for All” strategy provided an institutional framework for global efforts to expand the normative development of the right to health, accommodating international health obligations through the 1978 Declaration of Alma-Ata. In order to realize human rights to health and development through international health assistance and cooperation, WHO and UNICEF brought together representatives from 134 state governments for an international conference on primary health care. Under the Declaration’s rights-based goal of “health for all by the year 2000,” representatives sought international cooperation to reduce inequalities in health status between developed and developing countries, encouraging governments to work toward establishing a “New International Economic Order” that would prioritize disadvantaged groups through national primary health care systems.18
With the advent of economic structural adjustment policy in the 1980s, however, the Declaration of Alma-Ata failed to achieve its goals for primary health care, leading WHO to postpone its “Health for All” mission, remove the language of “by the Year 2000” from its “Health for All” campaign, and rename its delayed vision of health justice “Health for All in the 21st Century.”19 Despite efforts to reach consensus on international cooperation in the 1986 UN Declaration on the Right to Development and the 1993 Vienna Declaration and Programme of Action, these proclamations of a new world order did not translate into international health obligations.20 At this nadir in global health governance, WHO’s leadership under the right to health was displaced by the expanding influence of international financial institutions, with WHO’s authority for global health policy dispersed among other international organizations.21 Rather than addressing global health threats through the world’s premier public health organization, states sidelined WHO through the creation of The Joint United Nations Programme on HIV/AIDS (UNAIDS) and The Global Fund to Fight AIDS, Tuberculosis and Malaria (The Global Fund) as parallel programs to coordinate vertical interventions for high-profile diseases. Even as the harmful ramifications of the structural adjustment paradigm compelled a return to WHO’s “Health for All” strategy, weaknesses in the international legal framework for health enabled the dismantling of national health systems through economic austerity programs, exacerbating health inequalities within and between countries with little regard for the human rights consequences.22
In response to these weaknesses in the rights-based approach to health, public health advocates rallied around non-obligatory political commitments through the 2000 Millennium Development Goals (MDGs), which were designed to serve as a moral framework for a large-scale global campaign to advance human development through eight goals to be achieved by 2015. Introducing the MDGs, states recognized that “in addition to our separate responsibilities to our individual societies, we have a collective responsibility to uphold the principles of human dignity, equality and equity at the global level.”23 Given this proclaimed “duty to all the world’s people, especially the most vulnerable,” four of the eight MDGs invoke commitments to global health — including the reduction of maternal and infant mortality, prevention of HIV infection, and eradication of hunger — with the final goal calling for the creation of “a global partnership for development.” Yet, although the MDGs provide hortatory indicators in global health — delineating aspects of international partnerships necessary for development — they do so in a way that is focused on foreign assistance, untethered to human rights, and wanting for legal obligations.24 As a result, the MDGs have failed to develop legal accountability for health obligations on international duty-bearers.25 Without unprecedented coordination in health investments from developed states — a commitment not even broached by the international community — it is highly unlikely that any substantial number of developing states will meet their public health goals.
A belated attempt to revitalize the rights-based approach to primary health care was made in 2000, when the UN Committee on Economic, Social and Cultural Rights (CESCR) took up the evolving definition of a right to health in its 14th General Comment on the ICESCR. Drawing on previously elaborated obligations of “international assistance and cooperation,” General Comment 14 reinterpreted these obligations for application to the right to health, furthering the consensus of the Declaration of Alma-Ata to highlight the international obligations of developed countries to “facilitate access to essential health facilities, goods, and services in other countries, whenever possible, and provide the necessary aid when required.”26 In reiterating the international obligations of the ICESCR, the CESCR stated that:
For the avoidance of any doubt, the Committee wishes to emphasize that it is particularly incumbent on States parties and other actors in a position to assist, to provide ‘international assistance and cooperation, especially economic and technical’ which enable developing countries to fulfill their core and other obligations.27
Extending this reasoning to international financial institutions, the CESCR advised that “[s]tates parties which are members of international financial institutions, notably the International Monetary Fund, the World Bank, and regional development banks, should pay greater attention to the protection of the right to health in influencing the lending policies, credit agreements and international measures of these institutions.”28 Advocates have pushed forward in advancing these international health obligations despite criticisms that 1) extraterritorial obligations do not exist under the ICESCR, 2) the CESCR has limited “international assistance and cooperation” in health to “facilities, goods, and services” rather than underlying determinants of health, and 3) General Comment 14 “go[es] far beyond what the treaty [ICESCR] itself provides and what the states parties believe to be the obligation they have accepted.”29 The advocacy to advance these obligations has accelerated even as developed states have neglected rights-based approaches to foreign assistance and developing states have faced hobbling budgetary uncertainties in their progressive realization of health goals.
With growing recognition of the rights-based impact of globalized forces on primary health care systems in the developing world, there has been increasing analysis of international health obligations following the 2002 appointment of the first UN Special Rapporteur on the right to the highest attainable standard of health, who sought to “give practical guidance about the application of the human rights responsibility of international assistance and cooperation in health.”30 Under his mandate to recommend measures to promote and protect the right to health, the Special Rapporteur found that:
[s]tates are obliged to respect the enjoyment of the right to health in other jurisdictions, to ensure that no international agreement or policy adversely impacts upon the right to health, and that their representatives in international organizations take due account of the right to health, as well as the obligation of international assistance and cooperation, in all policy-making matters.31
Although the first Special Rapporteur enumerated general principles to guide states in the financial allocations and global policies necessary to realize international health assistance and cooperation, both he and the second Special Rapporteur have faced difficulties in applying these expansive international obligations to developed states and international organizations.32
Collective rights as a means to international obligations
Despite this normative evolution of the right to health, the inherent limitations of the individual human rights framework stymie the right to health in impacting the development processes that are most crucial for realizing underlying determinants of health through primary health care.33 Because the right to health has been advanced as an individual right, one to be realized by a state duty-bearer, this limited, atomized right has proven insufficient to create accountability for international obligations in global health policy, leaving in its wake deteriorating national health systems that lack the capacity to address an expanding set of public health claims.34
Although individuals have found success against their own governments in select claims for a right of access to essential medicines, this national litigation model has little salience to underlying determinants of health, many of which are structured by actors and forces beyond the sovereignty of the state.35 As recognized by legal analysts:
International human rights law, caught within its framework of state responsibility for human rights violations, is unable to deal fully with the changes to state sovereignty accelerated by the process of globalization. Where the violator of human rights law is not a state or its agent but a globalized economic institution or a transnational corporation, international human rights law finds it difficult to provide any redress to the victim.36
As such, national enforcement of the right to health has been limited in challenging the global institutional arrangements that structure the ability of states to realize public health through primary health care systems.37 With large proportions of health-related funding flowing through foreign assistance programs, a growing chasm is evident between international power and domestic responsibility in health rights. This chasm highlights the utility of collective health rights — rights of states and peoples that can reform international institutions to account for international obligations to realize underlying determinants of health through primary health care.
Collective rights to realize global public goods
Collective rights can give meaning to underlying determinants of health in the human rights system, and through the scaling up of primary health care systems, provide for the realization of public health. It has long been recognized by public health scholars that “public health and safety are not simply the aggregate of each private individual’s interest in health and safety … . Public health and safety are community or group interests.”38 As a result, public health — based upon its non-rivalrous and non-excludable properties — is a public good that, by its very nature, has meaning only at a collective level.39 Working as a shared public good, a collective whole that is greater than the sum of its parts, primary health care systems can lead to positive externalities — in this case, health for all. Where this public good “benefits all of mankind,” its realization becomes the “collective responsibility of all nations.”40 With global health determinants implicating such international responsibility for primary health care, collective rights become necessary to address these international obligations for global public goods.
The rise of collective rights to challenge global institutions
Although human rights were initially conceived following the Second World War solely as individual rights — with an individual rights-bearer left to make claims against a national duty-bearer (and provide external restraint against a presumably tyrannical sovereign) — the rise of developing states and development debates has forced a re-examination of this individualistic conception of human rights.41 Viewing traditional human rights frameworks as an extension of imperialist domination, developing states advanced collective rights as a means of freeing their peoples from the neocolonial binds of international relations and establishing a “New International Economic Order.”42 Following the supremacy of individual rights in early UN treaties, collective rights received their first explicit recognition in regional human rights systems, wherein developing states advanced economic development rights in the 1972 UN Conference for Trade and Development (UNCTAD III) and African states memorialized communal rights in the 1976 Universal Declaration of the Rights of Peoples.43 Since that time, scholars and advocates have put forward arguments for collective rights to, inter alia, development, environmental protection, humanitarian assistance, peace, common heritage, and public health.44
Often referred to as “third-generation” rights, a rhetorical remnant of Cold War typologies, collective rights operate at an international level to assure public goods that can only be enjoyed in common with similarly-situated individuals and thus cannot be realized through individual rights claims against the state.45 Rather than restraining the state — a woefully inadequate obligation for states struggling to provide for their peoples in a globalizing world — these collective rights seek to empower the state to realize rights outside of its control. Despite the inherent conceptual weaknesses attendant to such nascent rights frameworks, collective rights claims have shown themselves effective in responding to national changes brought about by insalubrious development, shifting the balance of power in international relations and creating widely recognized, if not always realized, entitlements within the international community.46
Employing collective rights for global health governance
Collective rights offer an extant legal framework by which to restructure international institutions to meet global justice imperatives for public health. Through a vector of rights and duties, collective rights can address interconnected determinants of health within and between countries, obligating states and the international community to scale up primary health care systems in the developing world and thereby reduce inequities in global health. Reflecting sovereign inequalities, international dependencies, and cooperation imperatives, the developing state can be reconceptualized as both duty-bearer and rights-holder.47 While developing states would still bear a duty to realize individual health rights, they would also hold collective health rights — where they are unable to realize public health alone — to call on the international community for cooperation and assistance. By providing a framework for a national rights-holder in a globalized world, collective rights can be invoked to alter the global forces that structure the developmental and distributive policies underlying the public’s health.48 As such, collective rights in public health can complement the individual right to health, examining systemic problems engendered by global development processes and working alongside the right to health to mobilize national and international resources for primary health care.
In framing these international obligations, the duty-bearer for such collective rights would be the international community — including individual states, international organizations, and public-private partnerships. It was once thought that such obligations on the international community could not exist because state sovereignty obviated transnational rights violations. As Louis Henkin noted in The Age of Rights,
The failure of the international human rights movement to address the responsibility of a state for human rights of persons in other states may reflect only the realities of the state system. States are not ordinarily in a position either to violate or to support the rights of persons in other states.49
Globalization has laid bare such hermetic conceptions of sovereignty. While such international obligations undeniably impinge upon both the developing and developed state’s sovereignty, these tensions pose little conflict where developing nations are incapable of realizing the health rights of their peoples alone, and developed nations need not shoulder these transnational obligations individually.
At the international level, developing states could operationalize these collective rights to enforce global health commitments, channel foreign assistance toward primary health care, and ensure cooperation in global health policy. Since the ability of states to realize their human rights obligations at the domestic level is constrained by the actions and institutional arrangements of the international community, the realization of collective rights will require a restructuring of international institutions and national foreign assistance programs, allowing developing states to enter public health debates not merely with a plea for charity, but with a right to assistance and cooperation.
Developing human rights claims against the international community: Respect, protect, and fulfill
Based upon General Comment 14’s delineation of state obligations pursuant to the right to health — drawn from the CESCR’s approach to “respect, protect, and fulfill” all economic, social and cultural rights — it is possible to extend these dimensions of health obligation from the domestic to the international sphere.50
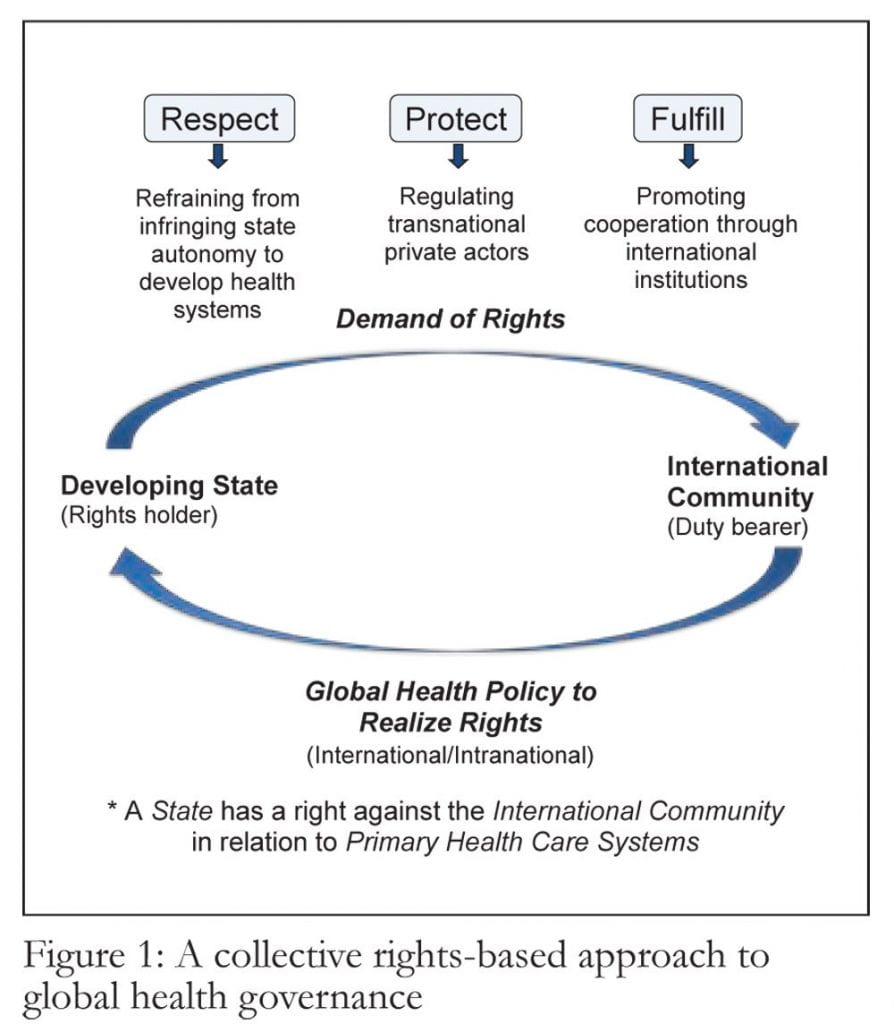
Under this analogous tripartite framework, the international community has an obligation to respect the rights of developing states by not infringing upon these states’ autonomy to develop functioning primary health care systems. This would place legal responsibility on developed states and international financial institutions to refrain from such actions as enforcing trade regimes with inequitable subsidies, preventing parallel importation of essential medicines, and privatizing services in ways detrimental to sustainable health systems.51 In this sense, collective rights can be viewed as restoring sovereignty to developing states to meet the basic public health needs of their peoples without interference, thereby creating an enabling environment for states to realize their domestic obligations for economic, social, and cultural rights, including the right to health.
Similarly, the international community has an obligation to protect developing states through the regulation of transnational private actors that undermine state governance in public health. In particular, transnational corporations (TNCs) — whose pursuit of increasingly flexible labor markets and deregulated policy environments has resulted in a “race to the bottom” in national regulations — have limited states’ ability to govern in the absence of global coordination.52 Further impeding national health care administration, pharmaceutical TNCs have prevented developing states from directing finite resources to the procurement of affordable essential medicines and health services.53 To protect states from these deregulatory and monopolistic practices that harm the public’s health, the international community can promulgate international public health standards, creating global public health frameworks to prevent TNCs from seeking safe haven for harm in any country.54
Finally, as the realization of collective rights in a globalized world requires cooperation across the international community, WHO can be viewed as a natural institutional mechanism to fulfill the obligations of the international community for global public health. WHO, as the leading authority in global health policy and “the only organization with the political credibility to compel cooperative thinking” on public health, can serve a dual role in fulfilling international obligations pursuant to collective rights — promoting international cooperation to support global public goods (such as preventing the transnational spread of infectious disease) and coordinating funding efforts to strengthen national primary health care systems (such as developing research agendas for the chronic and neglected diseases of developing countries).55 Where such leadership necessitates the incorporation of collective public health obligations in treaty law, WHO — drawing on its constitutional mandate for health and human rights — can reestablish its rights-based legitimacy in global health policy by codifying such obligations through the recently-proposed Framework Convention on Global Health — galvanizing engagement across the global health architecture to overcome collective threats to global health, heralding global consensus on primary health care, and creating a lasting legacy of public health in international law.56
Implementing human rights claims through international organizations: International and intranational institutional reforms
Yet even among those who advocate international human rights obligations for health, there remain doubts as to the implementation mechanisms that would be necessary to operationalize these obligations under international law.57 Where individual human rights have long relied on goodwill and shaming to effectuate national policy change, collective health rights provide a set of legal claims and accountability mechanisms that can be institutionalized through international organizations. In implementing this collective rights framework through the international community, collective health rights may be implemented through both international and intranational means.
Internationally, collective rights can be implemented to restructure existing international institutions by incorporating human rights clauses into the international legal structure of these institutions and by developing multilateral governance institutions to ensure reciprocal conditionalities as obligations of the international community.58 Rather than allowing states to hide behind the veil of international institutions to absolve themselves of human rights obligations, states would bear duties through their membership in these organizations. For example, within the WTO — a forum for state negotiation and adjudication of free-trade principles, often to the detriment of public health — collective rights could be asserted by developing states to incorporate health rights into trade negotiations or dispute resolution mechanisms; thus, collective rights could harmonize regulations to protect the public’s health and reverse the burden of proof to show that trade agreements are not violating health standards.59 In addition, given an obligation of states to provide foreign assistance through international organizations, collective health rights could be invoked 1) against idle members to meet their unfulfilled commitments to global health and 2) on behalf of developing state members to heighten their participation in these organizations. To ensure that such health assistance is channeled into projects that strengthen primary health care, international assistance could be coordinated through a central body such as WHO — as discussed above, under obligations of the international community to fulfill collective rights — thereby reducing inefficiency and redundancy in contribution efforts in a manner similar to that of The Global Fund but cutting more broadly across health conditions and their determinants.60
Intranationally, to address developing country sources of global health inequalities — that is, inequalities in structural capacity that reinforce the dependence of developing states on ODA for vertical health programs — collective rights can be implemented to ensure that both bilateral and multilateral assistance is channeled through general budgetary support and sector-wide approaches to national primary health care systems.61 Whereas current health assistance tends to “crowd out” the public sector while creating funding distortions in national health policy, general budgetary support would overcome these bottlenecks in donor-driven priority setting by providing developing states with greater autonomy to address national public health priorities through official needs assessments. Realizing the collective health rights of states in such country-led development assistance, sector-wide approaches (SWAps) could overcome the tendency toward verticalization of health programs and create integration across sectors that underlie health.62 Through this channeling of assistance via general budget support, SWAps may be reformulated to cut across determinants of health (for example, education, infrastructure, environment, water and sanitation systems, and social insurance), strengthening state capacity for providing public goods by way of primary health care. As a result, primary health care could then be assured domestically, through individual rights claims against the state, and internationally, through human rights assessments of foreign assistance.
Thus, collective rights would provide a legal framework for states to seek or provide international assistance and cooperation in accordance with their respective capabilities.63 With the massive influx of funds invested in health and health-related development projects, it is critical that global health partnerships — including intergovernmental, governmental, and nongovernmental organizations — coordinate this health assistance to meet international public health goals and strengthen national primary health care systems. As interpretations of global social justice increasingly recognize imperatives to address power imbalances that give rise to an unjust social order, rather than merely increase assistance to offset the harms generated by global institutional arrangements, collective rights can be leveraged to bolster global institutions at the international level and channel development aid at the national level.64 By assuring that health assistance is directed toward efficient cross-sectoral channels through primary health care systems, collective rights could appreciate the pathways and synergies between development commitments and underlying determinants of health. To that end, states could employ collective health rights to institute a “development compact” in global health as a mechanism for “ensuring the recognition among all stakeholders of the ‘mutuality of the obligations’ so that the obligations of developing countries to carry out these rights-based programs are matched with reciprocal obligations of the international community to cooperate in order to enable the implementation of those programs.”65 Such a compact would offer a means for developing states to reshape the international community for health promotion, to raise public health obligations in economic development planning, and to increase national resources to realize primary health care for all.
Conclusion
So long as states can argue that their foreign assistance is elective, “health for all” will remain an elusive goal — one more regret upon the altar of failed political commitments. Realizing the rights-based promise of international obligations for global health will require sustainable international structures for facilitating coordination and cooperation across the international community. These structures can be created through the frameworks of collective human rights, developed and implemented through the structures outlined above and illustrated in Figure 1.
In this way, collective rights offer a framework for developing structures of global health governance. With human rights providing normative resonance to social mobilization and legal standards in global policy, the language and obligations of collective rights can prove instrumental in achieving the public health goals that have been incompletely realized under the aegis of the individual right to health. Through the complementary advancement of individual and collective health rights, states can create the optimum synergy of global efforts — at the national and international level — and give meaning to human rights as they address collective vulnerabilities to the realization of the public’s health.
Benjamin Mason Meier, JD, LLM, PhD, is Assistant Professor of Global Health Policy at the University of North Carolina at Chapel Hill.
Ashley M. Fox, MA, PhD, is a post-doctoral fellow in the Department of Global Health and Population at the Harvard School of Public Health.
Please address correspondence to the authors c/o Benjamin Mason Meier, Department of Public Policy, University of North Carolina, Chapel Hill, NC, 27599–3435, email: bmeier@unc.edu.
References
1. T. W. Pogge, “Human rights and global health: A research program,” Metaphilosophy 36 (2005), pp. 182–209.
2. As argued by J. Kim, J. Millen, J. Gershman, and A. Irwin (eds), Dying for growth: Global inequality and the health of the poor (Monroe, ME: Common Courage Press, 2000); and I. Kawachi and S. Wamala (eds), Globalization and health (Oxford/New York: Oxford University Press, 2006).
3. Kaiser Family Foundation, Donor funding for health in low-and middle-income countries, 2001–2007 (Washington, DC: The Kaiser Family Foundation, 2009), p. 1.
4. M. R. Reich (ed), Public-private partnerships for public health (Cambridge: Harvard University Press, 2002).
5. World Bank, World development report 1993: Investing in health (New York: Oxford University Press, 1993). Updated information is available at http://go.worldbank.org/FOL40VL5C0 (Health, Nutrition, and Population Initiative) and at http://go.worldbank.org/I3A0B15ZN0 (Multicountry HIV/AIDS Program). See also J. P. Ruger, “The changing role of the World Bank in global health,” American Journal of Public Health 95/1 (2005), pp. 60–70.
6. Institute of Medicine, US commitment to global health (Washington, DC: National Academy of Sciences, 2009), pp. 1–39; N. A. Szlezák, B. R. Bloom, D. T. Jamison, et al. “The global health system: Actors, norms, and expectations in transition.” PLoS Medicine 7/1 (2010), pp. 1–4, doi:10.1371/journal.pmed.1000183.
7. L. Garrett, “The challenge of global health,” Foreign Affairs 86/1 (2007), pp. 14–38.
8. T. R . Frieden and K. J. Henning, “Public health requirements for rapid progress in global health,” Global Public Health 4/4 (2009), pp. 323–337.
9. D. T. Halperin, “Putting a plague in perspective,” New York Times (January 1, 2008). Available at http://www.nytimes.com/2008/01/01/opinion/01halperin.html.
10. D. Kinley, Civilising globalisation: Human rights and the global economy (New York: Cambridge University Press, 2009).
11. R. G. Biesma, R. Brugha, A. Harmer, et al., “The effects of global health initiatives on country health systems: A review of the evidence from HIV/AIDS control,” Health Policy and Planning 24/4 (2009), pp. 239–252.
12. Szlezák et al. (see note 6), p. 2.
13. J. P. Ruger, “Ethics and governance of global health inequalities,” Journal of Epidemiology and Community Health 60 (2006), pp. 998–1002.
14. Universal Declaration of Human Rights (UDHR), G.A. Res. 217A (III) (1948), Preamble. Available at http://www.un.org/en/documents/udhr/.
15. Ibid., Arts. 25, 28 (emphasis added).
16. International Covenant on Economic, Social and Cultural Rights (ICESCR), G.A. Res. 2200A (XXI) (1966), Arts. 12, 2 (emphasis added). Available at http://www2.ohchr.org/english/law/cescr.htm.
17. S. F. Musungu, “Developing countries and the promotion of the right to health in multilateral institutions: A review of development in trade and health institutions,” in M. Robinson and A. Clapham (eds), Realizing the right to health (Zurich: Rüffer & Rub, 2009), pp. 368–378.
18. World Health Organization, Primary health care: Report of the international conference of primary health care Alma-Ata, USSR, September 6–12, 1978 (Geneva: WHO, 1978), para. 3. Available at http://www.who.int/hpr/NPH/docs/declaration_almaata.pdf.
19. World Health Assembly, Strengthening primary health care, Res. 41.34. 13 May 1988.
20. M. E. Salomon, Global responsibility for human rights: World poverty and the development of international law (New York: Oxford University Press, 2007).
21. G. Silver, “International health services need an interorganizational policy,” American Journal of Public Health 88/5 (1998), pp.727–729.
22. D. Tarantola, “A perspective on the history of health and human rights: From the Cold War to the gold war,” Journal of Public Health Policy 29/1 (2008), pp. 42–53. B. M. Meier and A. M. Fox, “Development as health: Employing the collective right to development to achieve the goals of the individual right to health,” Human Rights Quarterly 30 (2008), pp. 259–355.
23. United Nations, Millennium Development Goals (2000). Available at http://www.undp.org/mdg/basics.shtml.
24. S. Fukuda-Parr, “Millennium Development Goal 8: Indicators for international human rights obligations?” Human Rights Quarterly 28 (2006), pp. 966–997.
25. M. Robinson, “What rights can add to good development practice,” in P. Alston and M. Robinson (eds), Human rights and development: Towards mutual reinforcement (Oxford, New York: Oxford, 2005), pp. 25–44.
26. Committee on Economic, Social and Cultural Rights, General Comment No. 14, The Right to the Highest Attainable Standard of Health. UN Doc. E/C.12/2000/4 (2000), para. 39. Available at http://www.unhchr.ch/tbs/doc.nsf/0/40d009901358b0e2c1256915005090be?Opendocument (emphasis added).
27. Ibid., para. 45.
28. Ibid., para. 39.
29. On the three criticisms, see respectively R. Künnemann, “Extraterritorial application of the international covenant on economic, social and cultural rights,” in F. Coomans and M. T. Kamminga (eds), Extraterritorial application of human rights treaties (Antwerp: Intersentia, 2004); B. M. Meier and L. M. Mori, “The highest attainable standard: Advancing a collective human right to public health,” Columbia Human Rights Law Review 37 (2005), pp. 101–147; and K. Gorove, “Remarks at the ninety-eighth annual meeting of the American Society of International Law: Shifting norms in international health law,” American Society of International Law Proceedings 98 (2004), pp. 18–20.
30. Paul Hunt, UN Special Rapporteur on the right of everyone to the enjoyment of the highest attainable standard of physical and mental health, Report on Mission to the World Bank and the International Monetary Fund, Washington, DC, October 20, 2006, and Uganda, February 4–7, 2007, UN Doc. A/HRC/7/11/Add.2. (2008), para.15. Available at http://daccess-dds-ny.un.org/doc/UNDOC/GEN/G08/114/25/PDF/G0811425.pdf?OpenElement.
31. Paul Hunt, UN Special Rapporteur on the right of everyone to the enjoyment of the highest attainable standard of physical and mental health, The Right of Everyone to the Enjoyment of the Highest Attainable Standard of Physical and Mental Health, February 13, 2003, UN Doc. E/CN.4/2003/58, para. 28. Available at http://www.essex.ac.uk/human_rights_centre/research/rth/docs/CHR2003.pdf.
32. Paul Hunt, UN Special Rapporteur on the right of everyone to the enjoyment of the highest attainable standard of physical and mental health, Addendum: Mission to the World Trade Organization. UN Doc. E/CN.4/2004/49/Add.1. 2004. Available at http://www.unhchr.ch/Huridocda/Huridoca.nsf/e06a5300f90fa0238025668700518ca4/5860d7d863239d82c1256e660056432a/$FILE/G0411390.pdf.
33. P. Alston, “Ships passing in the night: The current state of the human rights and development debate as seen through the lens of the Millennium Development Goals,” Human Rights Quarterly 27 (2005), pp. 755–829.
34. M. Stuttaford, “Balancing collective and individual rights to health and health care,” Law, Social Justice and Global Development Journal 1 (2004). Available at http://www2.warwick.ac.uk/fac/soc/law/elj/lgd/2004_1/stuttaford/.
35. L. Forman, “‘Rights’ and wrongs: What utility for the right to health in reforming trade rules on medicines?” Health and Human Rights: An International Journal 10/2 (2008), pp. 37–52; A. E. Yamin, “Not just a tragedy: Access to medications as a right under international law,” Boston University International Law Journal 21 (2003), pp. 325–371; H. V. Hogerzeil, M. Samson, J. V. Casanovas, and L. Rahmani-Ocora, “Is access to essential medicines as part of the fulfillment of the right to health enforceable through the courts?” Lancet 368 (2006), pp. 305–311.
36. R. E. Mazur, “Realization or deprivation of the right to development under globalization? Debt, structural adjustment, and poverty reduction programs,” GeoJournal 60/1 (2004), p. 64.
37. P. Danchin, “A human right to water? The South African Constitutional Court’s decision in the Mazibuko case,” EJIL: Talk! Blog of the European Journal of International Law. Available at http://www.ejiltalk.org/a-human-right-to-water-the-south-african-constitutional-court%E2%80%99s-decision-in-the-mazibuko-case/.
38. D. Beauchamp, “Community: The neglected tradition of public health,” Hastings Center Report 15/6 (1985), pp. 28–36.
39. R. D. Smith, “Global public goods and health,” Bulletin of the World Health Organization 81/7 (2003), p. 475.
40. J. E. Stiglitz, “The theory of international public goods and the architecture of international organizations 2,” Background paper 7, United Nations, Department for economic and social information and policy analysis (Nov. 7, 1995).
41. J. Donnelly, Universal human rights in theory and practice (Ithaca, NY: Cornell University Press, 2003), pp. 1–260.
42. B. I. Hamm, “A human rights approach to development,” Human Rights Quarterly 23 (2001), pp. 1005–1031.
43. B. I. Hamm, “A human rights approach to development,” Human Rights Quarterly 23 (2001), pp. 1005–1031.
44. B. M. Meier, “Advancing health rights in a globalized world: Responding to globalization through a collective human right to public health,” Journal of Law, Medicine and Ethics 35/4 (2007), pp. 545–555.
45. P. R. Baehr and K. VanderWal, “Human rights as individual and as collective rights,” in J. Berting and P. Baehr (eds), Human rights in a pluralist world: Individuals and collectivities (Geneva: UNESCO, 1990), pp. 33–50.
46. D. G. Newman, “Collective interests and collective rights,” American Journal of Jurisprudence 49 (2004), pp. 127–163; L. A. Obiora, “Beyond the rhetoric of a right to development,” Law & Policy 18 (1996), pp. 355–368.
47. W. Vandenhole, “The limits of human rights law in human development,” in E. Claes, W. Devroe, and B. Keirsbilck (eds), Facing the limits of the law (Berlin: Springer-Verlag, 2009), pp. 355–374.
48. M. E. Salomon, A. Tostensen, and W. Vandenhole, Casting the net wider: Human rights, development and new duty-bearers (Antwerp: Intersentia, 2007).
49. L. Henkin, The age of rights (New York: Columbia University Press, 1990), p. 44.
50. S. I. Skogly, Beyond national borders: States’ human rights obligations in international cooperation (Antwerp: Intersentia, 2006).
51. Salomon (see note 20).
52. See especially J. V. Millen and T. H. Holtz, “Dying for growth, part 1: Transnational corporations and the health of the poor,” in Kim et al. (see note 2), pp. 177–223.
53. S. Burris and J. L. Dunoff, “Introduction to the Symposium on SARS, public health, and global governance,” Temple Law Review 77/1 (2004), pp. 143–148.
54. J. Donnelly, “Human rights, globalizing flows, and state power,” in A. Brysk (ed), Globalization and human rights (Los Angeles: University of California Press, 2002), pp. 226–241; N. Jägers, Corporate human rights obligations: In search of accountability (Antwerp: Intersentia, 2002).
55. L. Garrett (see note 7), p. 22.
56. L. O. Gostin, “Meeting basic survival needs of the world’s least healthy people: Toward a framework convention on global health,” Georgetown Law Journal 96 (2008), pp. 331–392.
57. L. O. Gostin and R. Archer, “The duty of states to assist other states in need: Ethics, human rights, and international law,” Journal of Law, Medicine & Ethics 35 (2007), pp. 526–533.
58. A. M. Fox and B. M. Meier, “Health as freedom: Addressing social determinants of global health inequities through the human right to development,” Bioethics 23 (2009), pp. 112–122; S. I. Skogly, The human rights obligations of the World Bank and the International Monetary Fund (London: Cavendish Publishing, 2001).
59. D. Fidler, “Constitutional outlines of public health’s ‘new world order,’” Temple Law Review 77 (2004), pp. 247–290.
60. P. Östlin, T. Schrecker, R. Sadana, et al., Priorities for research on equity and health: Implications for global and national priority setting and the role of WHO to take the health equity research agenda forward (Geneva: World Health Organization, 2009). Available at http://uottawa.academia.edu/TedSchrecker/Papers/109104/Priorities-for-research-on-equity-and-health.
61. A. Lawson, D. Booth, M. Msuya, et al., Does general budget support work? Evidence from Tanzania (London: Overseas Development Institute, 2005). Available at http://www.worldbank.org/ieg/nonie/docs/TanzaniaGBS.pdf.
62. A. Cassels and K. Janovsky, “Better health in developing countries: Are sector-wide approaches the way of the future?” Lancet 352 (1998), pp. 1777–1779; M. Foster, A. Brown, and T. Conway, Sector-wide approaches for health development: A review of experiences (Geneva: World Health Organization, 2000).
63. S. P. Marks, “Obligations to implement the right to development,” in B. A. Andreassen and S. P. Marks (eds), Development as a human right: Legal, political, and economic dimensions (Cambridge, MA: Harvard University Press, 2006), pp. 59–80.
64. T. W. Pogge, “Priorities of Global Justice,” in T. W. Pogge (ed.), Global Justice (Oxford: Blackwell Publishers, 2001), pp. 6–23.
65. A. Sengupta, Development cooperation and the right to development (Boston, MA: François-Xavier Bagnoud Center for Health and Human Rights, 2003), p. 8. Available at http://www.harvardfxbcenter.org/resources/working-papers/FXBC_WP12–Sengupta.pdf.