Growing Up Can be Hard to Do: Reimagining Structurally Supportive Pediatric-to-Adult Transitions of Care from a Rights-Based Perspective
Vol 25/1, 2023, pp. 51-65 PDF
Michelle Munyikwa, Charles K. Hammond, Leanne Langmaid, and Leah Ratner
Abstract
Extended life expectancies and shifting dynamics in chronic disease have changed the landscape of public health interventions worldwide, with an increasing emphasis on chronic care. As a result, transition from pediatric to adult care for medically complex adolescents and young adults is a growing area of intervention. Transition medicine is a nascent field whose current emphasis is on middle- and high-income countries, and thus far its methods and discourse have reflected those origins. Through several case-based examples, this paper aims to highlight the possibilities of an analytic approach grounded in structural competency for transforming transition medicine through a human rights-based framework, with an emphasis on imagining a more global framework for transition medicine. Our cases highlight the disparities between patients navigating pediatric to adult-based care, illuminating social stigma, stratification between public and private insurances, engagement in risk-taking behaviors, family conflict, and challenges with transition readiness. To reimagine transition medicine so that it is based on human rights, we must prioritize structural solutions that embrace multisectoral integration and holistic mental health support rather than oppress and marginalize these critical systemic adaptations. We aim to reconfigure this scaffolding to center structures that integrate holistic well-being and imagine alternate realities to healing. Our work contributes to the literature bringing structural competency to new spaces of clinical practice, contextualizing new frontiers for the exploration of chronic diseases across diverse clinical contexts worldwide.
Introduction
As extended life expectancies and shifting dynamics in chronic disease change the landscape of public health interventions worldwide, chronicity has become a growing area of study. Gains in life expectancy pose new challenges for ensuring the health of populations in diverse socioeconomic, political, and cultural contexts. Of particular interest to this paper, gains associated with “Western” biomedicine have enabled many with pediatric-onset diseases to live into adulthood. In the United States, Canada, Australia, and Western Europe, ensuring the safe transition from pediatric care to adult care has grown into a burgeoning clinical and research field organized under the framework of transition medicine.
Transition medicine is a nascent field that has traditionally been salient in high-income countries, with its methods and frameworks reflecting these origins. To the best of our knowledge, frameworks and structures around pediatric-to-adult transition have been shaped by the resources—both cultural and material—available in places like the United States, Canada, and the United Kingdom.[1] Though unique challenges present themselves depending on the overarching health system (e.g., US individualized health insurance versus the National Health Service in the UK), many common themes present across these geographically and culturally diverse situations.[2] Transition medicine is a diverse and vibrant field that has maintained close attention to the lived experiences of transitioning young adults and adolescents and centers its work and study around health care transition (HCT) for children and youth with special health care needs.[3] HCT is the formal model for standard of care utilized by those who practice transition medicine. This emphasis on HCT has generated frameworks, such as SMART, which allow for understanding transitioning youth (from pediatric to adult-based care) in context and for predicting and maximizing transition readiness.[4]
Adolescence is a critical developmental stage with important milestones, including increased desire for independence, self-discovery around sexuality, and emotional regulatory changes, particularly sadness and depression.[5] Without secure support through this transition, those already marginalized are at increased risk for further morbidity. Important to this work is the recognition that HCT could benefit from attention to structural oppression that unequally affects youth with chronic diseases and demonstrates the limits of existing systems in addressing these patients’ needs. Access to culturally responsive, situationally appropriate care is a priority for all youth but is particularly vital for those with chronic conditions or living with disability. While social-ecological frameworks have been integral in framing youth at the center of competing forces that affect readiness for and success in transition to adult care, greater attention to structural inequality would benefit the field as we imagine an expansion of its principles to diverse global contexts. An emphasis on structural competency in the design and evaluation of transition programs, as well as the framing of these resources as a right to be fought for, is key.[6] As advances in modern biomedicine have allowed for extended life expectancies, there is a need for a human rights-based approach to ensure the dignity and longevity of adolescents and young adults with chronic illness. It is, as we argue, our obligation to actively dismantle structures upholding and perpetuating inequity in this already vulnerable population.
The evolution of a rights-based model to transition
We ground our argument for HCT in an attentiveness to the right not only to health, but to the civic, political, and economic rights that enable youth to flourish in their communities.[7] This paper, an outgrowth of interdisciplinary and transnational collaboration in Ghana and the United States, is rooted in the conviction that transition support is an important site of intervention for ensuring the rights of adolescents and young adults living with chronic disease worldwide.[8]
While this paper is not the outcome of a formal qualitative research study, it is the product of over a decade of collaborative research between several authors of this paper. Thus, while this piece is not an ethnography, it is deeply ethnographic insofar as it draws on the ethos of deep participatory exploration, collaboration, and communication.[9] This collaboration is rooted in a long-standing working relationship between two of the authors (LR and CKH) through a variety of projects regarding transition-age youth. Their conversations, built from shared experience working on these issues in Ghana, formed the impetus to engage this topic. Another Boston-based collaborator, LL, has worked with LR in a transition clinic in Boston. Many of the challenges identified in transition medicine in the United States emerged from this working relationship. Recently, Philadelphia-based author MM began engaging with this team regarding challenges in transition medicine with a global lens rooted in structural competency, cultural humility, and anthropological thought and methods. Drawing on both her anthropological expertise and the other collaborators’ years of experience, our team started with a series of open-ended, though often case-based, discussions taking place over the course of several months, engaging in a constant comparative method akin to that which undergirds grounded theory.[10]
Early conversations took the shape of brainstorming about the challenges we face with transition-age youth in our clinical disciplines and locations.[11] Subsequently, we began organizing these freeform conversations into thematic buckets, refined until we reached collective agreement.[12] Our goal was twofold: more practically, we sought to problem-solve issues we had seen in all three locations; more globally, we sought to imagine a future for global transition medicine. Ultimately, the themes elucidated in this paper emerged from these conversations among the authors which highlighted challenges with HCT in our respective clinical practices. Through these conversations and experiences, we noted patterns that could be addressed most holistically by applying a rights-based approach. To further support the exploration of this framework, we engaged the transition medicine literature to understand if this had ever been done before; literature referenced was chosen for its salience to practitioners in transition medicine, with additional PubMed searches performed for resources regarding the HCT approach and its relationship to inequality and marginalization. Thus, the selection of our rights-based framework emerged from these collaborative conversations, our thematic exploration, and consensus after review of the literature, read against our collective clinical experiences. What emerged is a consensus view of these authors regarding challenges and opportunities embedded in existing transition frameworks.
Frameworks in transition medicine: Identifying existing challenges
As patients with pediatric-onset disease live increasingly into adulthood, transition medicine has become a growing field in many resource-rich settings. Optimal transition is not simply the transfer of providers but rather an integrated, systematic response to support the transfer of care from a pediatric to an adult medical home.[13] Systemic and structural support is important (e.g., transferring medical records, finding new sub-specialists), particularly at this time of developmental transition. We acknowledge that adolescence has salient representations across cultures, where it may be framed as a unique developmental period of major life transition, though noting that this period may be framed differently in different contexts.[14] While the social salience of adolescence varies, institutional structures related to pediatric versus adult care mean that this time is a significant period of transition. Adolescents and young adults with chronic medical conditions who may have grown up with their pediatric providers like family members must move on.
Moreover, in many contexts, this developmental period is marked by increased personal independence, often guided by adult role models. Medication and therapeutic adherence is most vulnerable during this transition given that adolescents and young adults can lose sight of self-management as their caregivers and providers give increasingly more autonomy.[15] This can be particularly at risk when these relationships are also in flux during this period.[16] Many innovators have sought to integrate skills-based learning to help these patients grow into their roles to self-navigate, self-advocate, and self-manage their chronic disease.[17] This is particularly important for those with multiply marginalized identities who must also navigate bias.
Though pediatric-to-adult transition medicine is still new, the commonly accepted methodology usually includes certain standard elements: (1) transition policy; (2) patient registries (tracking and monitoring); (3) readiness assessments; (4) planning; (5) transfer of care; and (6) transition completion with post-transition feedback.[18] Though these elements can serve as building blocks and integrate into existing health care infrastructure, they often center dominant identities. One example of these elements is the concept of transition registries. Rarely, if ever, do transition patient registries intentionally collect data to measure patient-facing equity indicators (e.g., self-identified gender, ethnoracial categories, or socioeconomic status), structural influences, or identities that may reflect how that patient interacts with the system and how the system then interacts or interferes with their ability to feel safe and cared for. Data typically collected on registries include name, date of birth, documentation of current and future providers, and readiness assessments. Gottransition.org, which has set the “gold standard” for these templates, has no mention of collecting ethnoracial data, gender identity, or socioeconomic or insurance status, undermining the critical importance that this type of data has on the patient’s and family’s ability to have a safe and successful transfer of care. As noted by Maria Diaz-Gonzalez de Ferris et al., without intentionally collecting data on types of insurance, primary language, or other ecological factors impacting care, certain communities are disproportionately marginalized.[19]
Transition-readiness assessments also often value a notion of self-advocacy within certain culturally bound developmental milestones that are framed as universal, failing to account for both cultural variation in the valorization of these traits and structural barriers to enacting these ideals where they are valued. Following Jonathan Metzl and Helena Hansen, we place greater emphasis on structural barriers and inequalities and are hesitant to fall back on cultural frameworks for understanding differences in transition readiness.[20] One question included in the Transition Readiness Assessment Questionnaire, a commonly used and validated readiness assessment, asks “Do you get financial help with school or work?” as an indicator of transition readiness. We are advocates for detailed social histories, which can provide valuable information for provider-driven resources.[21] Therefore, we recognize the importance and careful crafting of the Transition Readiness Assessment Questionnaire as an instrument, but can also imagine a scenario where this is being asked by a white provider in the United States to a young person of color who recently lost financial aid due to struggles with substance misuse. Or we might consider this being asked of a young adult who was not able to submit applications for assistance because they were recently incarcerated. We propose that these questions are important questions to answer not as a marker of readiness but as a point from which to strategize around structural barriers needed to overcome to provide rights-based and equitable transitions of care. These conversations could be integral to the process of “warm handoffs,” a recommended component of transition care in which providers discuss patients undergoing HCT.
The above examples reflect just a few existing challenges in transition medicine. Our observations of patterns in this work underscore the variations in rights and access to services across the geographic spaces in which we practice. In the United States, where many of our collaborators are based, steep hierarchies exist across racialized, classed, and gendered lines, making access to care and safe transition deeply variable.[22] In Ghana, based on our experience, similar but overlapping challenges exist, framed in colonial perceptions of care equity. Colonial notions promote the ideal of “Western” care as the gold standard. Without understanding the local context, these notions further create inequities in Ghana. In our work, we have observed the following patterns that have shaped our impetus to evolve and restructure how we practice transition medicine.
With a failure of empowerment, accountability, and participatory approaches, transition often flattens differences between patients and their desires for seeking care. People living at the intersections of multiple marginalized identities tend to suffer disproportionately, and transition programs, where they exist, intentionally allow for provider discretion in handling care to promote a patient-tailored response.[23] Though this can be extremely beneficial to patients’ unique needs, it leaves room for both implicit and explicit bias in the handling of the transfer of care. Additionally, diversity in clinical and healing perspectives is not often allowed for. Those seeking care with both “traditional” and biomedical practitioners of healing are often caught in the middle. The minimal integration of “traditional” and “Western” medicine often makes patients choose between the two, specifically in lower- and middle-income countries like Ghana. By doing this both within HCT and within the greater context of medical pluralistic hierarchies, we fail to recognize that our patients and their families have deep-seated beliefs in traditional practices.[24]
Patient “desirability” often shapes transition practices, and without legality and accountability embedded in health care structures, further marginalization is a result. As previous scholarship has demonstrated, the perception of the “difficult” patient is not equally applied to all populations.[25] This is no less true in transition medicine. In our collective experience, those with histories of substance misuse, or behavioral concerns that manifest themselves in anger or violence, are more often escorted to adult care.[26] Meanwhile, those who are well established with mental support are often kept in pediatric-based care. In the United States, patients from non-white backgrounds are disproportionately described as “difficult” or “angry,” as opposed to a recognition that, for example, “this family advocates for themselves well.” This further illustrates that not all advocacy is perceived the same, and sometimes this perpetuates inequity when it is transformed into a tailored transition experience.
The lack of nondiscrimination and equality structures promotes the recognition of those with chronic issues of childhood as a “special group”—a recognition that does not get applied equally. In the United States, where a robust system of tertiary and quaternary care exists, providers often face challenges with families and patients who are long convinced of their unique characteristics and who feel entitled to particular rights. In our transition clinic in Boston—where, in order to be referred to the clinic, patients must have at least five comorbid conditions or significant psychosocial vulnerability—we often find that those with privileged identities introduce as “the sickest patient or most unique patient” we have ever met. Typically, the patients who self-identify as especially vulnerable are often not those identified by providers as the most in need. The patients with the most vulnerability (both relative to structural determinants and chronic disease acuity) are usually more reticent to advocate for themselves or to self-identify in a way that suggests that they feel that the system is not supporting them.
These challenges, in addition to differences in ability to pay for care, access services, and navigate systems, permeate our experiences in transition medicine.
Toward a global transition medicine: Rights-based frameworks for adolescent and young adult care
Transforming transition medicine within a global lens requires an attunement to the unequal landscapes in which this field is practiced. Moreover, thinking about these practices and policies on a global stage, it is imperative that we also mention the role of colonialism in centering Eurocentric understandings of pediatric-to-adult transition medicine globally. We thus draw on work at the intersection of structural competency and human rights to ground our case analyses. Structural competency and related frameworks, with their interdisciplinary emphasis on health across sociopolitical contexts, offer the ability to ground our practice of transition medicine in the lived experiences of adolescents and young adults in diverse sociopolitical contexts, understanding that the needs of adolescents and young adults living with chronic disease vary depending on local communities, their resources, and their sites of struggle.[27] In this sense, successful HCT will not look the same in the United States as it does in Ghana.
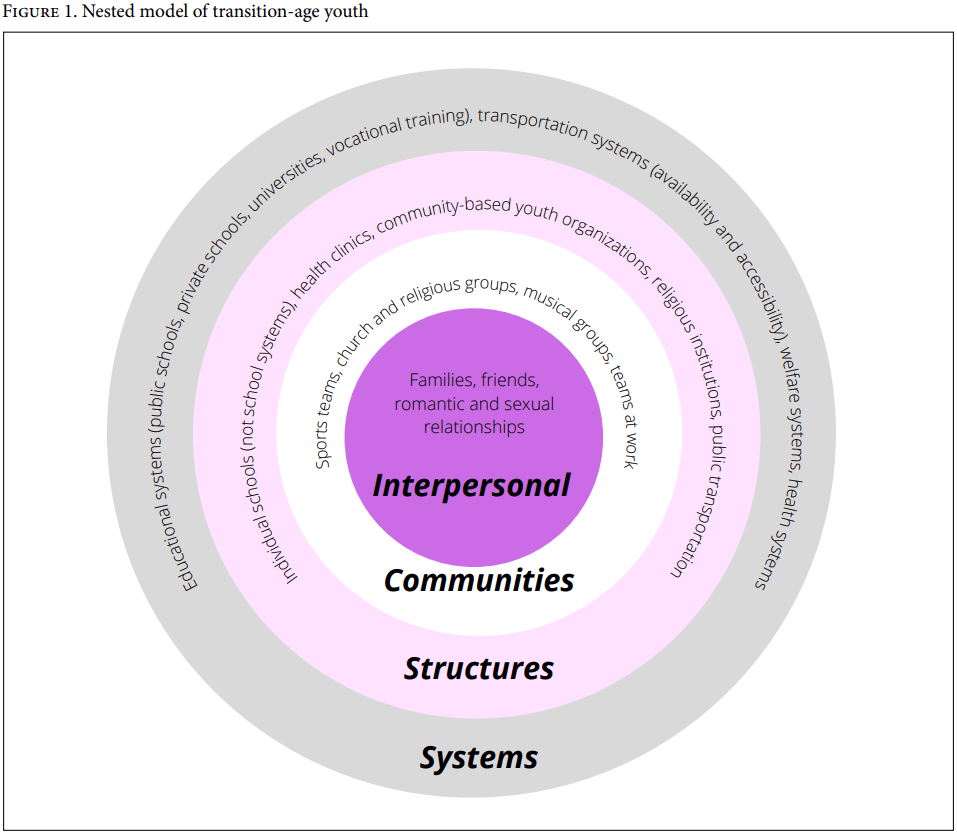
One model, the SMART model of transition—which elaborates 11 domains of transition medicine, from relationships to beliefs to skills and self-efficacy—focuses primarily on the individual or family unit undergoing HCT. Notably, the model includes one category, “pre-existing factors,” which are described as less amenable to change.[28] These include sociodemographic and cultural factors—“age, ethnic/racial identity, socio-economic status (SES), culture of family and community,” and gender and sexuality—that may impact HCT.[29] While these factors are bracketed in this model, we believe that they are essential to the understanding of how to build equitable HCT structures worldwide. We thus instead conceptualize the adolescents and young adults as existing at the center of multiple overlapping domains (see Figure 1)—their kin networks and local communities, the institutions (medical and otherwise) that they navigate in transition, the health care and educational infrastructure of their society, the cultural norms and ideologies that shape their identity, the way they navigate the world, and the global flows of information and power that shape the health care they have access to. As a result, we propose a structurally informed expansion of the socio-ecological SMART model informed by our transnational collaborations in HCT. Our fundamental argument is that a safe, structurally aware, and interpersonally supportive transition to adult services is a key component of the right to health for all people, particularly medically complex and vulnerable youth.
Pediatric-to-adult transition lends itself well to a rights-based approach. This has been imagined through the PANEL framework, which utilizes five main principles: participation, accountability, nondiscrimination, empowerment, and legality.[30] Participation refers to equity in participation for all stakeholders in decision-making. Accountability within a rights-based framework ascertains that “duty bearers” are held accountable to “rights holders.” It would be fair in this context to define rights holders as adolescents and young adults with pediatric-onset disease and duty bearers as the health system at large. Under the principle of nondiscrimination and equality, all rights holders are entitled to equal access to care. There should be no discrimination of care based on one’s ability to pay for transportation or communicate in common or colonial languages, for example. In terms of empowerment, many such adolescents and young adults are often part of many traditionally non-dominant communities, with common identities of neurodiversity or disability. It is critical that these communities and individuals have systems-level empowerment so they can adequately navigate the system and self-advocate for their care in equity with other individuals and communities from dominant societal groups. Finally, legality refers to the need for congruence in legal rights.
From personal to structural: Cases in transition medicine
The United States: Navigating generational trauma and systemic bias
Let us consider a 21-year-old second-generation Haitian American woman, Rose. Rose was born in Haiti but grew up in Boston and recently graduated from a four-year university with a bachelor’s in science. She is currently working at a tech start-up where she does not have employee-based health insurance. She carries a diagnosis of bipolar disorder and a more recent diagnosis of non-insulin-dependent diabetes. Given her age, Rose is no longer able to see her pediatrician for care, so she has gone without care for several years and is unsure where to go next in light of her insurance gap. She is working on applying for public insurance to find a new adult provider, a challenge that forces her to encounter the lack of availability and accessibility of services for those with public insurance, especially at transition age.
Rose’s mother has been somewhat skeptical of her seeking care, based on several traumatic events they both experienced while hospitalized upon first moving to the United States. Her mother often cries while telling stories of being stuck with needles and given medication while in the hospital without the use of an interpreter. The lack of participation in her own care has left her with traumatic memories. She shares that she felt terrified not knowing what she was given or why. After being given the medications in the hospital, she often woke up more tired, confused, and unsure of how to ask for help. She was never even told exactly what was wrong with her at the time or how to take care of herself after being discharged. Partially driven by these experiences, when our patient talks with her mom about her own feelings of depression, her mother often first suggests traditional Haitian models of care.
When Rose eventually obtains public insurance, she is automatically assigned to a primary care provider (PCP). Upon their first meeting, Rose reports to the new PCP that she thinks her mom carries similar symptoms of bipolar disorder, which seem to have worsened after she experienced a near-death event during an earthquake in Haiti. During this visit with the PCP, our patient becomes tearful when asked to follow up for routine age-appropriate screening. She reports that last year, while hospitalized for a flare-up of her bipolar disorder, she was forced to take new psychiatric medications without her consent that sedated her for several days. Traumatized from that experience and reflecting on her mother’s experience, she explains to the new PCP her mistrust in the system. She indicates her desire for the PCP to understand the cultural perspective from which she is coming. The PCP, a white woman, explains that the treatments she wants Rose to get are different and not sedating, but leaves the choice ultimately with our patient. The PCP is quick to cut Rose off and gets easily frustrated with her resistance. Rose eventually agrees, but becomes overwhelmed shortly after leaving the office. Unsure of what to do, she signs into her patient portal and reviews the medical encounter written by the PCP, which states, “Patient has been non-compliant and non-adherent to recommendations.” Rose is hurt and overwhelmed and decides not to follow up. Several months later, she has a syncopal episode at work and gets admitted to a different hospital for complications from her diabetes. Missing work for being hospitalized, she gets fired from her job and after discharge further struggles to follow up for primary care.
Case from Ghana: Neurodiversity and transition
Kofi, a 17-year-old Ghanaian boy with tuberous sclerosis complex (TSC) and epilepsy, presented to a transition clinic in Kumasi at a large academic teaching hospital. Kofi was diagnosed with epilepsy at the age of five and was referred to the pediatric neurology clinic of a teaching hospital at age 13 after many years of poor seizure control. He is the last of four children, with no family history of seizures or TSC. He started at a mainstream public school in rural Ghana at age four, where he entered preschool. He struggled with kindergarten, which he repeated twice, and was promoted to grade one at age seven. In the first grade, Kofi demonstrated severe difficulties in all aspects of learning due to complications from his illness; he repeated this grade twice, and then his parents withdrew him from school at age nine. Teachers’ reports from the five years that he was in the mainstream educational system indicate that he struggled with all aspects of learning. However, he did not receive any referral for assessment by either an educational or a clinical psychologist. He had, however, been seen by various traditional, religious, and herbal practitioners, with no improvement in seizure control or intellectual functioning. However, due to colonial notions of health care, and concern about bias, the family did not tell the neurologist that they were seeking care from community healers.
On referral to the pediatric neurology clinic at age 13, Kofi had overt cutaneous manifestations of TSC, as well as neurobehavioral challenges. He has since been seen by a clinical psychologist and diagnosed as having an intellectual disability. He has also undergone various tests, including an electroencephalogram, neuroimaging, an echocardiogram, and a renal ultrasound. His medications have been changed, and his seizures have now stabilized on two anti-seizure medications: carbamazepine, which is covered by the national health insurance scheme, and clobazam, which the family must pay for out of pocket. He occasionally has breakthrough seizures when he runs out of clobazam due to financial constraints. At age 15, Kofi was seen twice at a newly established pediatric-to-adult transition clinic and was transitioned to the adult neurology service but missed his appointment twice because his mom did not have money for transportation.
Case reflection
The literature suggests that individualized transition plans allow for unique attention to readiness as dictated by developmental milestones.[31] The above examples highlight subjects whose intersectional identities have consequential similarities and differences across systems and structures globally. Trauma was experienced in both cases at the personal, systemic, and structural level. Despite their geographic disparity, both cases also sit at the intersection of “Western” and traditional medicine, which ultimately promotes more fragmented than holistic care. The two cases also illustrate the need for multisectoral collaboration. In thinking about our adolescent with TSC, would his case have been different if the health sector and the education sector had been able to collaborate? Furthermore, while not specific to HCT, our case illuminates the failure of health systems to support chronic care. These are issues that are particularly integral to HCT but pose challenges across many domains of health. What if there were a direct referral system or collaboration between traditional and spiritual healers, on the one hand, and neurology or pediatrics, on the other? In our first case, how would the patient have benefited from a trauma-informed approach that embeds mental health care into the pediatric-to-adult transition process? What would have been different if Haitian healing practices had been invited to be discussed during her visits with her PCP? How could both cases have been different if the insurance schema in both countries recognized intersectional disparity and supported these patients specifically at these vulnerable life periods? Though both patients may have been included on transition registries and transitioned according to policy, and providers may have given “warm handoffs,” it is critical to recognize how without intentionally integrating anti-racist, anti-colonial, anti-oppressive care, the health system is built to increasingly marginalize those already on the periphery.
Reimagining structurally competent rights-based and humble care for transition-age youth
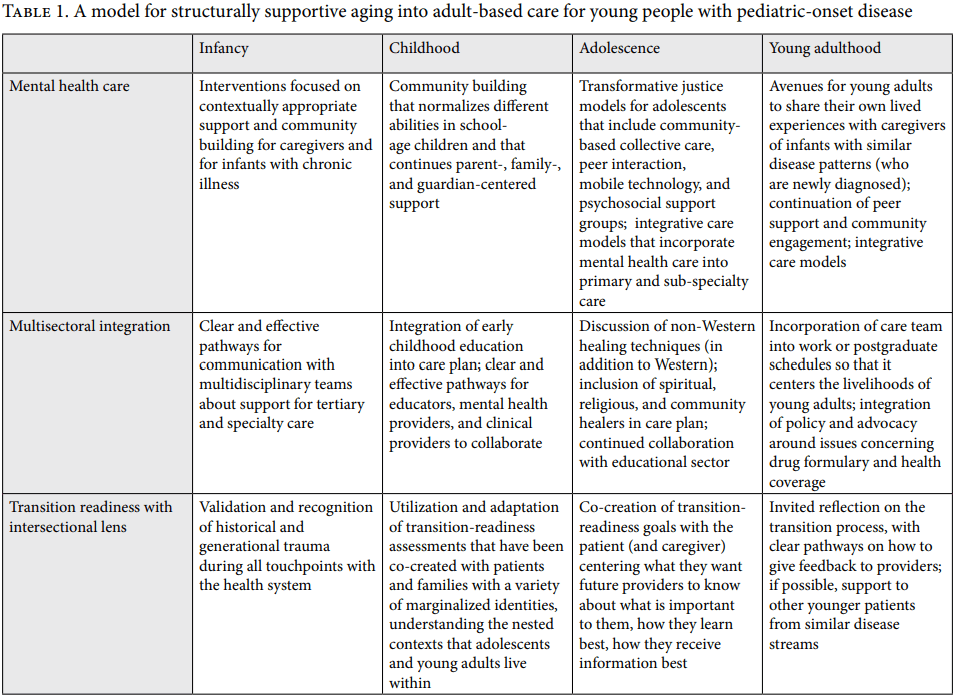
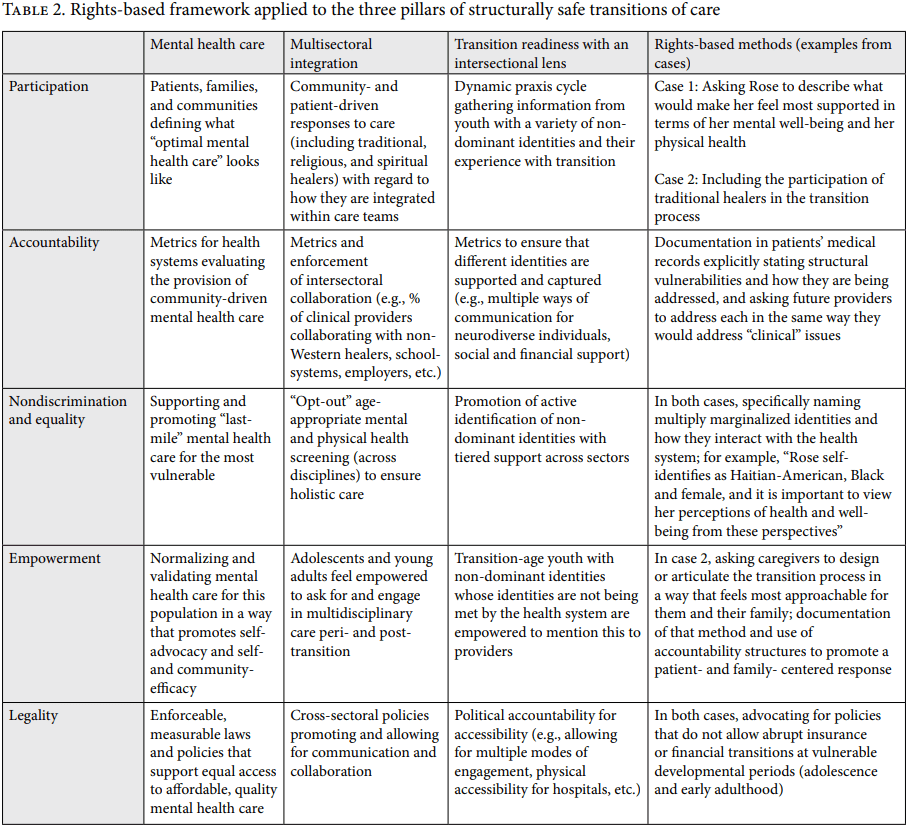
Children born with once rare pediatric-onset disease are now living into adulthood in striking numbers. But what does that mean if we have not created structurally safe health systems for them to age into? As a collective, we used themes generated from our conversations to create pillars of what we would imagine to be a structurally supportive system and explored those pillars by developmental period (see Table 1). We then applied the PANEL framework to these pillars utilizing examples from the cases discussed above (see Table 2). Our goal is not to impose Western visions on transition medicine through human rights practice but rather to engage in the effort to produce structurally equal transition medicine as one that asks of us “pragmatic solidarity.” Solidarity is not only a felt practice (empathy by HCT providers) but also a material one in which we contribute materially (where systems and structures are built to protect those most at the periphery during this process) what we can to common cause.[32] These practices would also be grounded in the understanding that the needs of patients vary greatly among contexts. These alternative structures would represent three pillars, as outlined in Table 1:
- Recognition of the importance of opt-out culturally and structurally humble mental health care, with a focus on healing justice and social capital. It is well known that adolescents are at increased risk of mental health morbidity and that those with ongoing chronic illness are at even higher risk. Supporting holistic well-being prophylactically by building community and enhancing sense of belonging can strengthen resiliency during this developmental period.
- Multisectoral integration, including non-health-related sectors, in which practitioners center individuals’ holistic developmental milestones, such as school, jobs, and relationships. This structure also recognizes and names the shame and strife that is inherent with being chronically ill, in pain, and feeling “left out” of adulting experiences.
- Transition readiness with an intersectional lens that supports championing at the individual and systemic level to overcome intersectional oppression. Validating this health-seeking behavior looks different in different settings, and therefore the health system must adapt to meet the patient where they are.
The PANEL framework highlights areas of further growth in transition medicine in the domains of participation, accountability, nondiscrimination and equity, empowerment, and legality.
Participation. Though not often the case in clinical medicine, transition medicine relies on iterative feedback from patients and families in process metrics. However, to further decolonize our practice, it is also critical that diverse providers—including traditional, religious, and spiritual healers—have input into transition processes. How can we create systems so patients, providers, and community members are able to actively participate in a way that works for them? How can this be done from a population perspective? In some contexts, virtual platforms for patient care have allowed for nimble and flexible care.[33] This enables the clinic to meet patients and families at their home, where providers can meet pets or family members or see their gardens or artwork, for example, all of which promotes human-centered care. Alternative learning styles can be honored utilizing different platforms within virtual features. However, with globally unequal access to digital technologies, these approaches can be limiting for patients and families who lack access to this technology. In other contexts, other proven interventions such as community health worker programs and regional clinics may be more helpful. Patient advisory committees also serve as a dynamic way to promote care that is responsive to adolescents and young adults, built with the understanding that these committees should demographically represent the communities that clinics serve.[34] Additionally, integrative approaches that accept various models of non-biomedical approaches to medicine juxtaposed with biomedicine are key. These could include patient co-referrals, collaborations between orthodox and traditional medical practitioners, and the creation of a unit for traditional medicine and healers in Westernized hospitals and clinics. Incorporating aspects of traditional healing in the training of health care practitioners and creating a space for knowledge sharing have also been proposed.[35] These strategies are not a silver bullet, given the asymmetries in access to material resources and institutional recognition, as well as the marginalization of Indigenous beliefs and practices, that often shape contemporary health care systems.[36] Assuming that many communities practice syncretic healing practices, how might transition programs—and all health programs—guarantee the right to pursue culturally concordant, structurally supported care? Ultimately, the point is that fostering participation must be done with intention.
Accountability. How do we create systems in which providers are accountable to their own bias? How do we promote self-reflection around the types of patients who often remain in pediatric-centered care versus the ones who are encouraged to transition because of divergent non-dominant identities? Part of the solution requires the implementation of enforceable, measurable, and consequential systems-based policy. Though transition policies are a commonly accepted methodology, what is often missed is the importance of accountable structures to promote equity (and stopgap inequity). Without this, these policies promote inequity. In Kumasi, Ghana, many successful transitions from pediatric to adult care employ the use of joint adult and pediatric clinics to assess these factors and address deficiencies that are identified.[37] This allows both adult and pediatric providers to physically attend to the patient at the same time, improving care coordination, rapport, and trust toward the new providers. It also allows for more meaningful good-byes to pediatric providers. This is a context-driven solution, as Ghana’s National Health Insurance Scheme allows for two providers to collaborate, whereas in the US system, that would make for a challenging billing paradigm. We could, however, imagine transforming the formal systems of payment to enable such care innovations.
Nondiscrimination and equality. Critical to enforcing this element of a rights-based framework is intentionality in the type and method of data collection. How are we creating transition registries? What data points about systemic bias and systemic oppression are being collected? When our patient with TSC in Ghana fails to transition, how are we capturing the financial burden of his antiepileptics that allowed him to begin to seize again? We recommend, in this vein, a registry with intentional equity indicators, attuned to the potential disparities in health care and access to care, not to mention lived experiences of care. It is important to build on existing structures while also recognizing the context within which they are practiced. Pediatric specialists should be encouraged to find transition-readiness assessments based on context-appropriate developmental readiness, disease stability, and sociocultural and economic factors.
Empowerment. Building social capital through community has been shown to support rights-based practice for healing. Christian Ntizimira refers to Ubuntu (umuntu ngumuntu ngabantu) as the African expression of “who we are” as a critical message for decolonizing end-of-life practice, through a shared community. Transition medicine benefits from similar decolonized ideals, where social capital can be pivotal to promote wellness, and community can be used as a resource for justice. We recommend youth-led psychosocial support groups that build community and help youth connect through shared experience.[38] Chronic disease can be isolating and stigmatizing in many settings, and coming together to share experiences can be empowering and build protective factors in promoting well-being.
Legality. It is critical to discuss the Convention on the Rights of Persons with Disabilities when thinking about the legality for structurally safe care for this population. This convention, signed by both Ghana and the United States (but which only Ghana has ratified), centers on the aim to “promote, protect and ensure the full and equal enjoyment of all human rights and fundamental freedoms by all persons with disabilities, and to promote respect for their inherent dignity.”[39] Using this as groundwork, it is imperative that there be legally binding policies that promote equity in access to care. Legal frameworks involving the voices of clinicians (both Western and non-Western) and patients must be advocated for before local, regional, and national governments. Important points for advocacy include supported decision-making, equity in medications on national formularies, and accessible health services for people with varying abilities.
Conclusion
Current definitions and accepted best practices of the health care transition from pediatric to adult care fail to intentionally recognize the diverse needs of adolescents and young adults with multiply marginalized identities and the overwhelming impact of racism and colonialism on HCT. In our experience, the current standard of care for practicing transition medicine promotes harm. We believe that the transition process should instead be viewed through three pillars—supportive peri-transitional mental health care, multisectoral collaboration, and transition readiness with an intersectional lens—in order to guide providers, systems, and structures toward equitable, safe, and holistic care for these populations. We hope that this model can promote the use of an actionable rights-based methodology in the field of transition medicine to facilitate more just and equitable HCT.
Acknowledgments
We wish to acknowledge our teams in the United States and Ghana. Specifically, we are grateful to Ahmet Uluer, director of the BRIDGES Adult Transition Program, for supporting us in prioritizing an equity-based approach to transition; Kessewea Gyan, Bernard Nkum, and Gustav Nettey for their dedication to the development of a rights-based transition process for youth in Ghana; and Angela Osei-Bonsu and Sheila Owusu for their dedication to mental health support groups for our neuro-diverse and chronically ill adolescents and young adults in Ghana, and for teaching us so much about prioritizing overall well-being in transitions of care.
Michelle Munyikwa, MD, PhD, is a resident physician in combined internal medicine and pediatrics at the University of Pennsylvania Health System and Children’s Hospital of Philadelphia, United States.
Charles K. Hammond, MBChB, MPhil, FWACP, FGCP, is a consultant pediatric neurologist at the Komfo Anokye Teaching Hospital and a senior lecturer at the School of Medicine and Dentistry, Kwame Nkrumah University of Science and Technology, Kumasi, Ghana.
Leanne Langmaid, MSN, RN, CPN, is a clinical coordinator within inpatient medicine at Boston Children’s Hospital, and a former nurse transition coordinator within the BRIDGES Adult Transition Program at Boston Children’s Hospital, United States.
Leah Ratner, MD, MS, DTM&H, is an instructor at Harvard Medical School and an attending physician at Boston Children’s Hospital and Brigham and Women’s Hospital, Boston, United States.
Please address correspondence to Michelle Munyikwa. Email: michelle.munyikwa@pennmedicine.upenn.edu.
Competing interests: None declared.
Copyright © 2023 Munyikwa, Hammond, Langmaid, Ratner. This is an open access article distributed under the terms of the Creative Commons Attribution Non-Commercial License (http://creativecommons.org/licenses/bync/4.0/), which permits non-commercial use, distribution, and reproduction in any medium, provided the original author and source are credited.
References
[1] P. White, A. Schmidt, J. Schorr, et al., “Six Core Elements of Health Care TransitionTM 3.0” (2020); CAPHC National Transitions Community of Practice, “A Guideline for Transition from Paediatric to Adult Health Care for Youth with Special Health Care Needs: A National Approach” (Canadian Association of Paediatric Health Centres, 2016); M. Kaufman, J. Pinzon, Canadian Paediatric Society, and Adolescent Health Committee, “Transition to Adult Care for Youth with Special Health Care Needs,” Paediatrics and Child Health 12/9 (2007); Care Quality Commission, “From the Pond into the Sea: Children’s Transition to Adult Health Services” (2014).
[2] N. P. Narla, L. Ratner, F. V. Bastos, et al., “Paediatric to Adult Healthcare Transition in Resource-Limited Settings: A Narrative Review,” BMJ Paediatrics Open 5/1 (2021).
[3] L. Li, M. Bird, N. Carter, et al., “Experiences of Youth with Medical Complexity and Their Families during the Transition to Adulthood: A Meta-Ethnography,” Journal of Transition Medicine 2/1 (2020); J. S. Porter, A. D. Lopez, K. M. Wesley, et al., “Using Qualitative Perspectives of Adolescents with Sickle Cell Disease and Caregivers to Develop Healthcare Transition Programming,” Clinical Practice in Pediatric Psychology 5/4 (2017); P. H. White, W. C. Cooley, Transitions Clinical Report Authoring Group, et al., “Supporting the Health Care Transition from Adolescence to Adulthood in the Medical Home,” Pediatrics 142/5 (2018).
[4] L. A. Schwartz, L. K. Tuchman, W. L. Hobbie, and J. P. Ginsberg, “A Social-Ecological Model of Readiness for Transition to Adult-Oriented Care for Adolescents and Young Adults with Chronic Health Conditions,” Child: Care, Health and Development 37/6 (2011); L. F. Zhang, J. S. Ho, and S. E. Kennedy, “A Systematic Review of the Psychometric Properties of Transition Readiness Assessment Tools in Adolescents with Chronic Disease,” BMC Pediatrics 14/1 (2014).
[5] Centers for Disease Control and Prevention, “Child Development: Adolescence (15–17 Years Old)” (2019), https://www.cdc.gov/ncbddd/childdevelopment/positiveparenting/adolescence2.html.
[6] J. M. Metzl and H. Hansen, “Structural Competency: Theorizing a New Medical Engagement with Stigma and Inequality,” Social Science and Medicine 103 (2014).
[7] P. Farmer, “Challenging Orthodoxies: The Road ahead for Health and Human Rights,” Health and Human Rights Journal 10/1 (2008).
[8] Narla et al. (see note 2).
[9] C. McGranahan, “Ethnography beyond Method: The Importance of an Ethnographic Sensibility,” Sites: A Journal of Social Anthropology and Cultural Studies 15/1 (2018).
[10] K. Charmaz, Constructing Grounded Theory (London: Sage Publications, 2006).
[11] H. Burgess, K. Jongbloed, A. Vorobyova, et al., “The ‘Sticky Notes’ Method: Adapting Interpretive Description Methodology for Team-Based Qualitative Analysis in Community-Based Participatory Research,” Qualitative Health Research 31/7 (2021).
[12] B. A. Israel (ed), Methods in Community-Based Participatory Research for Health, 1st edition (San Francisco: Jossey-Bass, 2005).
[13] M. A. McManus, L. R. Pollack, W. C. Cooley, et al., “Current Status of Transition Preparation among Youth with Special Needs in the United States,” Pediatrics 131/6 (2013).
[14] R. A. Sanders, “Adolescent Psychosocial, Social, and Cognitive Development,” Pediatrics in Review 34/8 (2013); R. F. Hill and J. Dennis Fortenberry, “Adolescence as a Culture-Bound Syndrome,” Social Science and Medicine 35/1 (1992); N. Lesko, “Denaturalizing Adolescence: The Politics of Contemporary Representations,” Youth and Society 28/2 (1996); J. E. Korbin and E. P. Anderson-Fye, “Adolescence Matters: Practice- and Policy-Relevant Research and Engagement in Psychological Anthropology,” Ethos 39/4 (2011); A. Schlegel and B. L. Hewlett, “Contributions of Anthropology to the Study of Adolescence,” Journal of Research on Adolescence 21/1 (2011).
[15] D. Taddeo, M. Egedy, and J.-Y. Frappier, “Adherence to Treatment in Adolescents,” Paediatrics and Child Health 13/1 (2008); D. A. Murphy, C. M. Wilson, S. J. Durako, et al., “Antiretroviral Medication Adherence among the REACH HIV-Infected Adolescent Cohort in the USA,” AIDS Care 13/1 (2001); E. Shemesh, B. L. Shneider, J. K. Savitzky, et al., “Medication Adherence in Pediatric and Adolescent Liver Transplant Recipients,” Pediatrics 113/4 (2004); I. M. Friedman, I. F. Litt, D. R. King, et al., “Compliance with Anticonvulsant Therapy by Epileptic Youth: Relationships to Psychosocial Aspects of Adolescent Development,” Journal of Adolescent Health Care 7/1 (1986).
[16] C. S. Kelly, C. A. Berg, M. A. Ramsey, et al., “Relationships and the Development of Transition Readiness Skills into Early Emerging Adulthood for Individuals with Type 1 Diabetes,” Children’s Health Care 47/3 (2018).
[17] J. S. Hess and D. M. Straub, “Brief Report: Preliminary Findings from a Pilot Health Care Transition Education Intervention for Adolescents and Young Adults with Special Health Care Needs,” Journal of Pediatric Psychology 36/2 (2011); M. E. Diaz-Gonzalez de Ferris, M. de L. Díaz-González de Martínez, A. M. Díaz-González de Velázquez, et al., “An Interdisciplinary Approach to Optimize the Care of Transitioning Adolescents and Young Adults with CKD,” Blood Purification 50/4–5 (2021).
[18] White et al. (2020, see note 1).
[19] Diaz-Gonzalez de Ferris et al. (see note 17).
[20] Metzl and Hansen (see note 6).
[21] H. L. Behforouz, P. K. Drain, and J. J. Rhatigan, “Rethinking the Social History,” New England Journal of Medicine 371/14 (2014); A. Premkumar, K. Raad, and M. H. Haidar, “Rethinking the Social History in the Era of Biolegitimacy: Global Health and Medical Education in the Care of Palestinian and Syrian Refugees in Beirut, Lebanon,” Anthropology and Medicine (2016); P. Bourgois, S. M. Holmes, K. Sue, and J. Quesada, “Structural Vulnerability: Operationalizing the Concept to Address Health Disparities in Clinical Care,” Academic Medicine 92/3 (2017); American Academy of Family Physicians, “Social Determinants of Health: A Guide to Social Needs Screening” (2019); R. D. Onie, R. Lavizzo-Mourey, T. H. Lee, et al., “Integrating Social Needs into Health Care: A Twenty-Year Case Study of Adaptation and Diffusion,” Health Affairs 37/2 (2018); B. J. Oldfield, M. Casey, A. DeCew, et al., “Screening for Social Determinants of Health among Children: Patients’ Preferences for Receiving Information to Meet Social Needs and a Comparison of Screening Instruments,” Population Health Management 24/1 (2021); M. W. Kreuter, T. Thompson, A. McQueen, and R. Garg, “Addressing Social Needs in Health Care Settings: Evidence, Challenges, and Opportunities for Public Health,” Annual Review of Public Health 42/1 (2021).
[22] K. E. Rea, G. K. Cushman, T. Santee, and L. Mee, “Biopsychosocial Factors related to Transition among Adolescents and Young Adults with Sickle Cell Disease: A Systematic Review,” Critical Reviews in Oncology/Hematology 167 (2021); K. Varshney, R. Iriowen, K. Morrell, et al., “Disparities and Outcomes of Patients Living with Down Syndrome Undergoing Healthcare Transitions from Pediatric to Adult Care: A Scoping Review,” American Journal of Medical Genetics Part A online ahead of print (2022).
[23] H. Marani, J. Fujioka, S. Tabatabavakili, and N. Bollegala, “Systematic Narrative Review of Pediatric-to-Adult Care Transition Models for Youth with Pediatric-Onset Chronic Conditions,” Children and Youth Services Review 118 (2020).
[24] I. Coulter, “Integration and Paradigm Clash: The Practical Difficulties of Integrative Medicine,” Mainstreaming Complementary and Alternative Medicine (New York: Routledge, 2003).
[25] D. Steinmetz and H. Tabenkin, “The ‘Difficult Patient’ as Perceived by Family Physicians,” Family Practice 18/5 (2001); R. C. Lorenzetti, C. H. M. Jacques, C. Donovan, et al., “Managing Difficult Encounters: Understanding Physician, Patient, and Situational Factors,” American Family Physician 87/6 (2013); A. Fiester, “The ‘Difficult’ Patient Reconceived: An Expanded Moral Mandate for Clinical Ethics,” American Journal of Bioethics 12/5 (2012).
[26] L. El-Hage, L. Ratner, S. Sridhar, et al., “Lessons Learned from the Pediatric Overflow Planning Contingency Response Network: A Transdisciplinary Virtual Collaboration Addressing Health System Fragmentation and Disparity during the COVID-19 Pandemic,” Journal of Hospital Medicine 16/9 (2021).
[27] J. T. Braslow and P. Bourgois, “Teaching Social Medicine as Collaborative Ethnographic Research and Advocacy on Homelessness and Serious Mental Illness,” in H. Hansen and J. M. Metzl (eds), Structural Competency in Mental Health and Medicine (Cham: Springer International Publishing, 2019); S. Stonington and D. Coffa, “Structural Iatrogenesis—A 43-Year-Old Man with ‘Opioid Misuse,’” New England Journal of Medicine 380/8 (2019); S. D. Stonington, S. M. Holmes, H. Hansen, et al., “Case Studies in Social Medicine—Attending to Structural Forces in Clinical Practice,” New England Journal of Medicine 379/20 (2018); S. M. Holmes, H. Hansen, A. Jenks, et al., “Misdiagnosis, Mistreatment, and Harm—When Medical Care Ignores Social Forces,” New England Journal of Medicine 382/12 (2020).
[28] Schwartz et al. (see note 4).
[29] Ibid., p. 886.
[30] Scottish Human Rights Commission, “A Human Rights Based Approach: An Introduction,” https://www.scottishhumanrights.com/media/1409/shrc_hrba_leaflet.pdf.
[31] A. M. Kelly, B. Kratz, M. Bielski, and P. M. Rinehart, “Implementing Transitions for Youth With Complex Chronic Conditions Using the Medical Home Model,” Pediatrics 110/Suppl 3 (2002); Institute of Medicine, The Future of Disability in America (Washington, DC: National Academies Press, 2007); A. Forbes, A. While, R. Ullman, et al., A Multi-method Review to Identify Components of Practice Which May Promote Continuity in the Transition from Child to Adult Care for Young People with Chronic Illness or Disability (National Coordinating Centre for the Service Delivery and Organisation, 2001).
[32] K. Muyskens, “Avoiding Cultural Imperialism in the Human Right to Health,” Asian Bioethics Review (2021); P. Farmer and N. Gastineau, “Rethinking Health and Human Rights: Time for a Paradigm Shift,” Journal of Law, Medicine and Ethics 30/4 (2002), p. 657.
[33] L. Langmaid, L. Ratner, C. Huysman, et al., “Supporting the Medically Fragile: Individualized Approach to Empowering Young Adults with Chronic Disease during the COVID-19 Pandemic,” Journal of Adolescent Health 67/3 (2020).
[34] C. L. Betz, M. L. Lobo, W. M. Nehring, and K. Bui, “Voices Not Heard: A Systematic Review of Adolescents’ and Emerging Adults’ Perspectives of Health Care Transition,” Nursing Outlook 61/5 (2013).
[35] A. Kwame, “Integrating Traditional Medicine and Healing into the Ghanaian Mainstream Health System: Voices from Within,” Qualitative Health Research 31/10 (2021).
[36] C. Piñones-Rivera, M. Mansilla, and R. Arancibia, “El imaginario de la horizontalidad como instrumento de subordinación: La política de salud pueblos indígenas en el multiculturalismo neoliberal chileno,” Saúde e Sociedade 26 (2017); C. Piñones-Rivera, N. Liberona, and B. Montecino, “La subordinación ideológica del saber médico andino en la salud intercultural chilena,” Polis 18/54 (2019).
[37] L. Gyan, L. Ratner, C. Dickens, et al., “Adulthood, Now What? A Pilot Transition Program in Kumasi, Ghana” (2022).
[38] S. A. Owusu, L. Ratner, Y. Woyome, et al., “Using Social Capital to Heal: Task Shifting Mental Health to Support Collective Care in Kumasi, Ghana” (2022); R. Sokol and E. Fisher, “Peer Support for the Hardly Reached: A Systematic Review,” American Journal of Public Health 106/7 (2016).
[39] European Network of National Human Rights Institutions CRPD Working Group and Mental Health Europe, “Implementing Supported Decision-Making: Developments across Europe and the Role of National Human Rights Institutions” (Saint Gilles: European Network of National Human Rights Institutions, 2020).

