A Global Review of Provisions on Emergency Care in National Constitutions
Volume 23/2, December 2021, pp. 187-200 | PDF
Taylor W. Burkholder, Madeline Ross, Lily Vartanyan, and Harveen Bergquist
Abstract
National constitutions are important tools for the realization of the right to health, and constitutional law linking health and human rights has been associated with improved access to health resources. Meanwhile, emergency care is a lifesaving service delivery platform with the potential to address much of the death and disability in low- and middle-income countries (LMICs). Yet even where services exist, access to emergency care may be systematically limited for vulnerable populations, except where laws explicitly protect the right to emergency care. We therefore sought to catalog and describe constitutional provisions related to emergency care. Through a comprehensive review of 195 national constitutions, we searched provisions for terms related to emergency care and performed qualitative framework analysis on these provisions. Eleven provisions met inclusion criteria, representing ten LMICs with constitutions written since 1996. While seven of the eleven provisions guarantee access to emergency care to all people, three narrow this guarantee to citizens only. Only three constitutions address the affordability of emergency care. While these constitutional provisions represent an important step toward the legal guarantee of access to emergency care for all people, further attention must be paid to the impact of such laws and regulation on the accessibility of emergency care and its related reduction of death and disability globally.
Introduction
Emergency medical conditions—including injuries, communicable and noncommunicable diseases, acute decompensation of chronic conditions, and complications of pregnancy—require timely, high-quality care to prevent death and permanent disability.1 These health conditions are estimated to represent over half of global deaths and up to 2.1 billion disability-adjusted life years annually.2 Whereas other parts of the health system may be incapable of the timely recognition and management of such conditions, emergency care is a service delivery platform intentionally oriented toward timely identification and management.3 The integration of emergency care systems into the overall health system therefore has potential to save lives, particularly in low- and middle-income countries (LMICs), where the burden of these conditions is highest and the outcomes are disproportionately worse.4
Access to emergency care is markedly limited in much of the world. Estimates in Africa, for example, suggest that only 71% of people live within two hours of a hospital that could potentially provide emergency care.5 Yet this method likely overestimates the true availability and accessibility of emergency care in these countries, since many hospitals do not have the trained personnel and resources capable of providing adequate emergency care.6 Additionally, there are many other barriers to accessing emergency care that are not included in this geospatial method of estimating access. Issues of affordability (financial accessibility), discrimination against vulnerable populations, and quality and acceptability of emergency care practices can also create barriers to accessing care during a health emergency.7 Barriers to accessing emergency care have been linked to delays in receiving care and to avoidable deaths.8
Reports of people being barred from hospitals due to the inability to levy upfront payments, or being required to purchase emergency medications and supplies before they can be administered, are not uncommon.9 These and other barriers to accessing emergency care not only result in otherwise avoidable death and disability but also represent systematic violations of human rights. As of the early 2000s, all nations had ratified at least one international treaty that enshrines the right to the highest attainable standard of health.10 According to the United Nations Committee on Economic, Social and Cultural Rights’ General Comment 14, the right to the highest attainable standard of health can be framed in terms of the AAAQ framework: availability, accessibility, acceptability, and quality. Special attention is paid to two dimensions of accessibility—nondiscrimination and affordability—to avoid the exclusion of vulnerable populations from health care programs.11 The time-dependent nature of emergency conditions leaves people vulnerable to undue financial demands from providers and facilities. The concept of a right to emergency care has recently entered the academic discourse, along with a call to include a rights-based approach to developing emergency care systems.12
Simultaneously, the global agenda on universal health coverage focuses on improving access to care, ensuring quality care, and protecting against financial risk.13 Recognizing this and the potential to save substantial lives, the 72nd World Health Assembly passed Resolution 72.16, titled “Emergency Care Systems for Universal Health Coverage: Ensuring Timely Care for the Acutely Ill and Injured,” in May 2019.14 The resolution signals a public commitment by United Nations member states to build and strengthen emergency care systems that will improve access to and the affordability of lifesaving care as an essential component of the overall health system.
As part of its guidance on the development of such health system frameworks, the World Health Organization (WHO) has described six “building blocks” fundamental to best practices in this process. The sixth building block, leadership and governance, is vital to achieving high levels of availability and accessibility of quality emergency care within the broader health system. The realization of good governance relies on the coordination of varying, yet overlapping, mechanisms to formalize intended health system frameworks among a wide spectrum of actors, including governments, nongovernmental organizations, private companies and corporations, medical practitioners, the general public, and others. These mechanisms span all levels of organization, including international treaties, national constitutional and statutory law, and national and local regulations, guidelines, and policies.
At the highest level, international treaties obligate the ratifying parties to fulfill legal stipulations in the agreement. A recent comprehensive review of United Nations treaties found that eight treaties included language directly addressing the need for emergency and essential surgical care and anesthesia.15 Given that emergency care systems are integral to the provision of emergency and essential surgical care and anesthesia, these treaty provisions can be applied to emergency care as a surrogate.
Although the enforcement of international treaties is challenging and often limited, these human rights laws have been used at the national level to substantiate legal claims around access to essential medications.16 The use of international treaties in such a way may obviate the need for domestic law in countries that have ratified one of these treaties if a judicial challenge rules that the treaty obligations apply to the provision of emergency care.
However, given the inconsistency with which international treaties are both upheld and applied on a country-by-country basis, constitutional law serves as a powerful mandate to guarantee the right to health at the national level. Despite how widely legal systems vary in structure around the world, constitutions can be readily appraised and comparatively analyzed given their inherent uniformity in existence.17 Constitutional law has previously been shown to produce tangible results. One study found that constitutional law was the most important contributor to expanding access to essential medications, as demonstrated by favorable judicial rulings when the right to access such medications was challenged in court.18 These laws can serve both as indicators of nations’ commitment toward health-related rights and as foundational directives in the creation of health policies and programs.19
Study objective
To date, there have been no formal studies regarding the existence or content of laws governing access to emergency care globally. Therefore, legislators and policy makers have a paucity of information on how to best draft and reform laws governing access to emergency care. Although we do not seek to develop a single “model text” for countries wishing to implement constitutional laws or amendments—owing to the complex nature of cultures, resource availability, and health care systems internationally—an analysis of common components of existing laws is likely to be useful for policy makers who are considering this approach to governing emergency care accessibility. In this study, we sought to (1) quantify and catalog constitutional provisions on emergency care worldwide and (2) qualitatively describe the characteristics of existing constitutional provisions on emergency care.
Methods
Comprehensive review
We conducted a comprehensive review of national constitutions from 195 countries as compiled by the Constitute Project (https://www.constituteproject.org). All constitutions were retrieved in their original English versions or English-language translations on January 26, 2019, and subsequently imported into ATLAS.ti to search for the terms “emergency,” “illness,” “injury,” “life threatening,” “life-threatening,” “medical care,” “medical treatment,” “healthcare,” “health-care,” and “health care.” Any constitutional provision (also known as clause or article) containing a search term was then compiled into Microsoft Excel for screening.
Two independent reviewers (MR and LV) screened each identified constitutional provision for inclusion if it was an original article or amendment that pertained to the delivery of emergency or acute care in any facility or pre-hospital setting for an individual experiencing a perceived health emergency. Provisions were excluded if they (1) addressed a state of national emergency or other non-health emergency law or regulation (e.g. armed conflict), (2) addressed a disaster or infectious epidemic rather than an everyday, individual health emergency, (3) addressed the health status of an elected or appointed official as it related to his/her ability to perform the duties of office, (4) addressed non-health emergencies (e.g. fire, hostage situation, legal damages), or (5) related to health care provision or protected health status but did NOT directly address emergency or acute care. The final exclusion criteria were selected in order to focus the review on constitutional law that directly and unmistakably guarantees access to emergency care. A senior reviewer (TB) resolved any discordant inclusion decisions and randomly re-screened an additional 10% of the provisions to ensure systematic agreement.
Data collection in MS Excel included verbatim text from the included provision(s) as well as the country name, year of ratification, and amendment status. Three reviewers (TB, MR, HB) then conducted a framework analysis using a mixed inductive and deductive qualitative approach. A mixed approach was selected in order to explore overlap with previously identified domains of the right to emergency care while also leaving space to discover unexpected components of existing constitutional provisions. Using a set of preliminary codes, the reviewers independently coded the constitutional texts according to pre-existing analytical frameworks, with new codes inductively added as deemed necessary by the reviewers. The code book was refined and texts were iteratively coded until consensus was reached by all reviewers and no new codes emerged. Thematic analysis of the codes was performed in ATLAS.ti followed by indexing according to framework analysis in MS Excel.
Analytical framework
This review employed the use of three existing frameworks for the right to the highest attainable standard of health (“right to health”) and constitutional laws pertaining to right to health issues (Box 1). The first two frameworks draw from international human rights standards outlined in General Comment 14. Provisions pertaining to the right to health can be categorized by the type of legal obligation and by the AAAQ framework. Legal obligations can be divided into responsibilities to respect, protect, and promote (or fulfill) the right to health, while the AAAQ framework classifies right to health issues according to availability, accessibility, acceptability, and quality.20 Legal obligations and the AAAQ framework are therefore clear, objective classifications of constitutional law that guarantee access to emergency care, and they have previously been used to analyze constitutional texts in other health system domains.21
The third framework used was derived from the Kinney-Clark typology of constitutional provisions on health.22 In this taxonomy, constitutional provisions can be divided into five categories based on the intent and function of the provision: statements of aspiration, statements of entitlement, statements of duty, programmatic statements, and referential statements (Box 1). Classifying provisions that pertain to access to emergency care according to this framework allows for a more objective assessment of the level of government commitment and potentially of the enforceability of the law.

Results
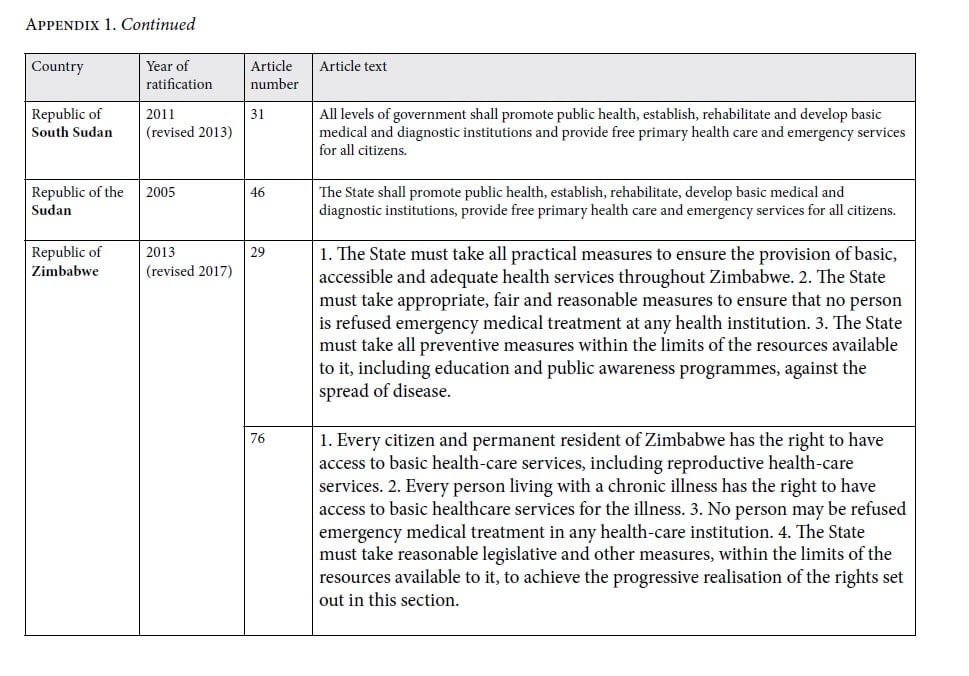
From the 195 constitutions compiled and searched, a total of 1,280 unique provisions were identified for screening, of which 1,269 were excluded based on predefined criteria. Eleven articles ultimately met inclusion, representing ten countries with constitutional laws containing provisions regarding emergency care (Appendix 1). Figure 1 shows the PRISMA flow diagram of screening results.
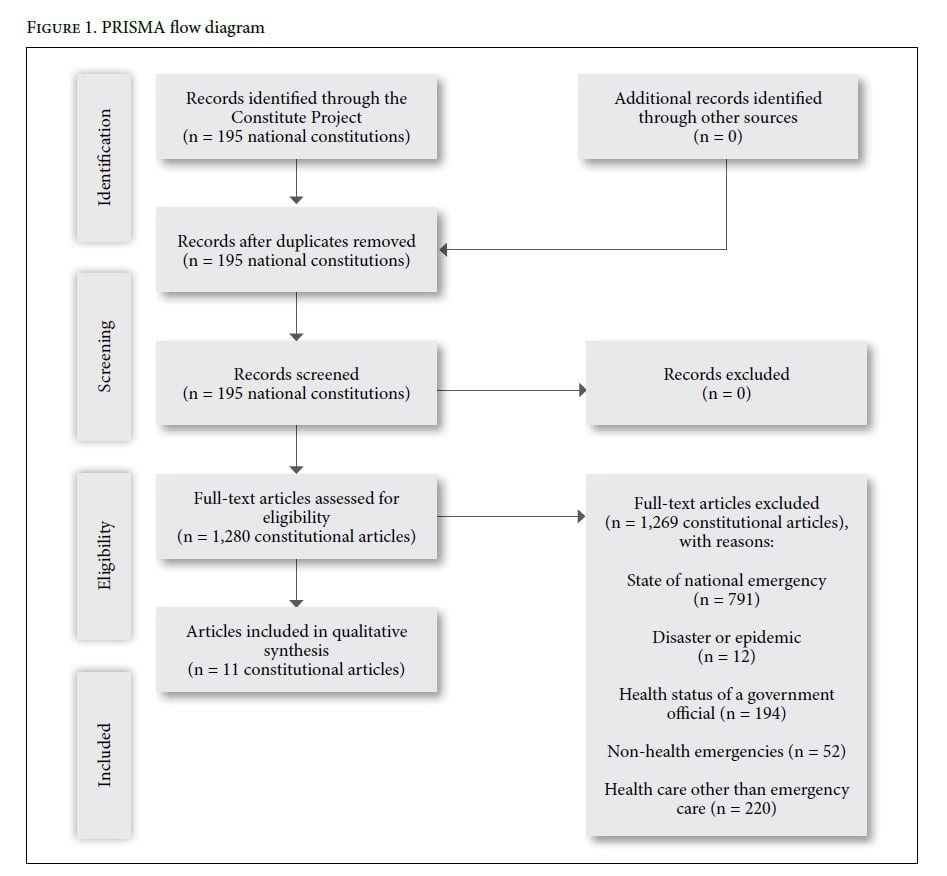
All ten countries are classified by WHO as low- or middle-income countries (three are classified as low income, four as lower-middle income, and three as upper-middle income). When mapped according to WHO regions, six of the ten countries are located in the African region. The remaining four countries are located in the Americas, the Eastern Mediterranean, the Western Pacific, and Southeast Asia. The earliest constitution to include a provision guaranteeing emergency care was passed in 1996.
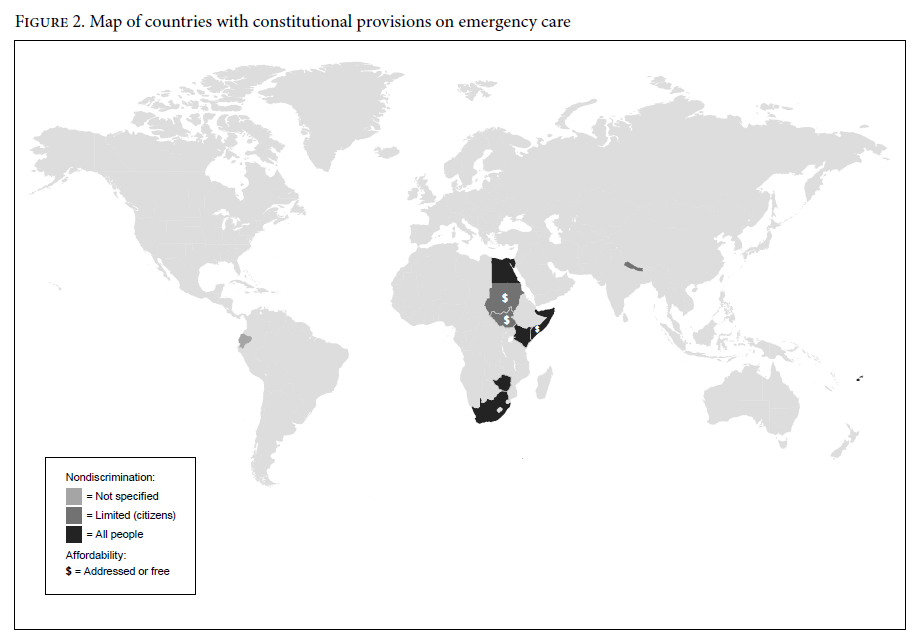
As classified by the AAAQ framework, none of the included constitutional provisions directly address the availability, acceptability, or quality of emergency care. However, accessibility is addressed by nine of the ten constitutions in two distinct ways: nondiscrimination and affordability. Six of the constitutions guarantee universal access to emergency care; three limit access to citizens only; and one implies (but does not directly specify) accessibility as it relates to nondiscrimination, stating that “for no reason” may a person be refused care. In terms of affordability, free emergency care is guaranteed in two of the ten constitutions (Sudan and South Sudan). Affordability is additionally addressed by one further constitution (Somalia), which states that access could not be limited by “economic capability.” Figure 2 maps countries with constitutional provisions on emergency care according to the AAAQ framework.
When analyzed under the obligations set forth by General Comment 14, the constitutional provisions were found to incorporate varying levels of commitment to the fulfillment of emergency care. One country (Zimbabwe) addresses all three levels of obligation: to respect, to protect, and to promote. However, the remaining nine countries are split, with five requiring respect for emergency care and four imposing protection of the right to emergency care.
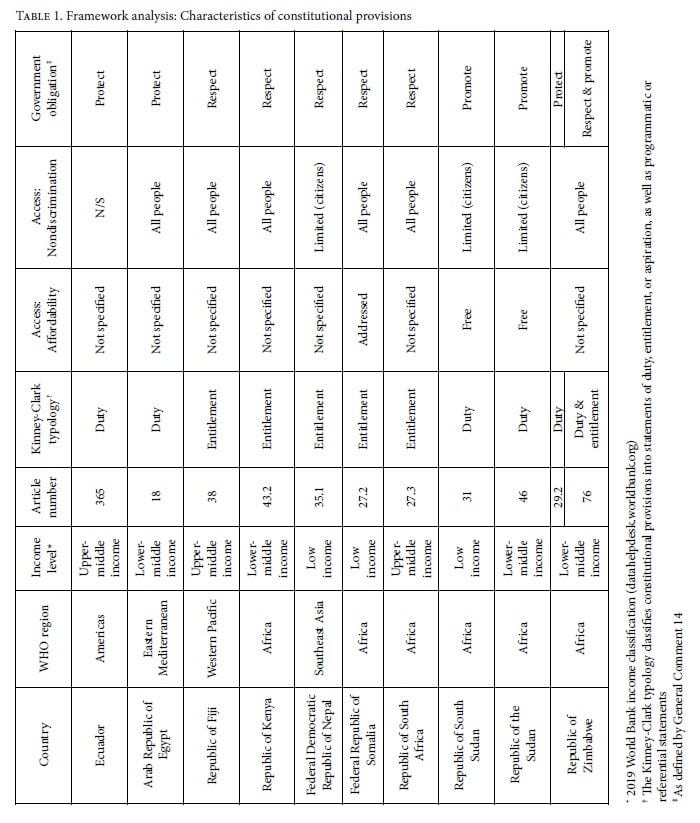
Finally, as coded by the Kinney-Clark typology, six constitutions include statements of entitlement and five include statements of duty (Zimbabwe included statements of both), all surpassing the most basic level of statement of aspiration, but none addressing programmatic or referential imperatives. The combined results of the framework analysis are reported in Table 1.
Discussion
Only 10 constitutions out of the 195 screened include provisions related to emergency care, demonstrating that a minority of countries have chosen to guarantee emergency care as a right in their most fundamental law. The reasons for this are likely multifactorial. The second half of the 20th century saw both a growth in the human rights movement, with an increase in the recognition of the right to health, and a surge in the adoption of constitutions containing more detailed rights, including not only civil and political rights but also economic, social, and cultural rights. All nations have now ratified at least one international agreement articulating the right to health. Since then, several studies have demonstrated an increasing number of nations incorporating variations of health-related provisions in their national constitutions.23
Emergency care, however, is a newer health system delivery innovation, only recently acknowledged in many health system frameworks. Constitutions adopted before the advent of emergency care in the mid to late 20th century, and much later for many countries, are not likely to reference this system. As a result, all 10 of the constitutions included in our study were written or revised after 1996, with South Africa representing the earliest incorporation of an emergency care provision into a constitution. We did not encounter any constitutional amendments that address a right to emergency care in those countries whose constitutions predate the advent of emergency care.
Countries with constitutional provisions meeting our inclusion criteria revealed an Afro-centric geographic distribution and a predominance of low- and middle-income levels. According to Jody Heymann et al., provisions addressing the overall right to health, defined as “constitutional references to physical or overall well-being, health protection, health security and/or a life free of illness or disease,” are most common in low-income countries.24 Not surprisingly, constitutions incorporating a right to emergency care as part of the right to health also demonstrate this predominance.
It may be more crucial for governments and policy makers in LMICs to support a constitutional right to emergency care, given that emergency care systems have been shown to address a wide range of illnesses and injuries that disproportionately lead to death and disability in LMIC populations.25 Others have theorized that the constitutional incorporation of economic, social, and cultural rights plays a different role in different types and stages of national systems. With regard to the right to health, Colleen Flood and Aeyal Gross recommend that nations transitioning to democracy, and thus toward equity in general, include health rights in their constitutions in an attempt to address societal inequities.26
Acknowledging the important role that national constitutions can play in fulfilling the right to health, we focused our framework analysis on the AAAQ framework from General Comment 14. The first essential element of the AAAQ framework is availability. Though the availability of emergency care may seem implicit in the discussion of accessibility of such services, none of the 10 constitutions referencing emergency care explicitly mandate that the care exist in sufficient quantity.
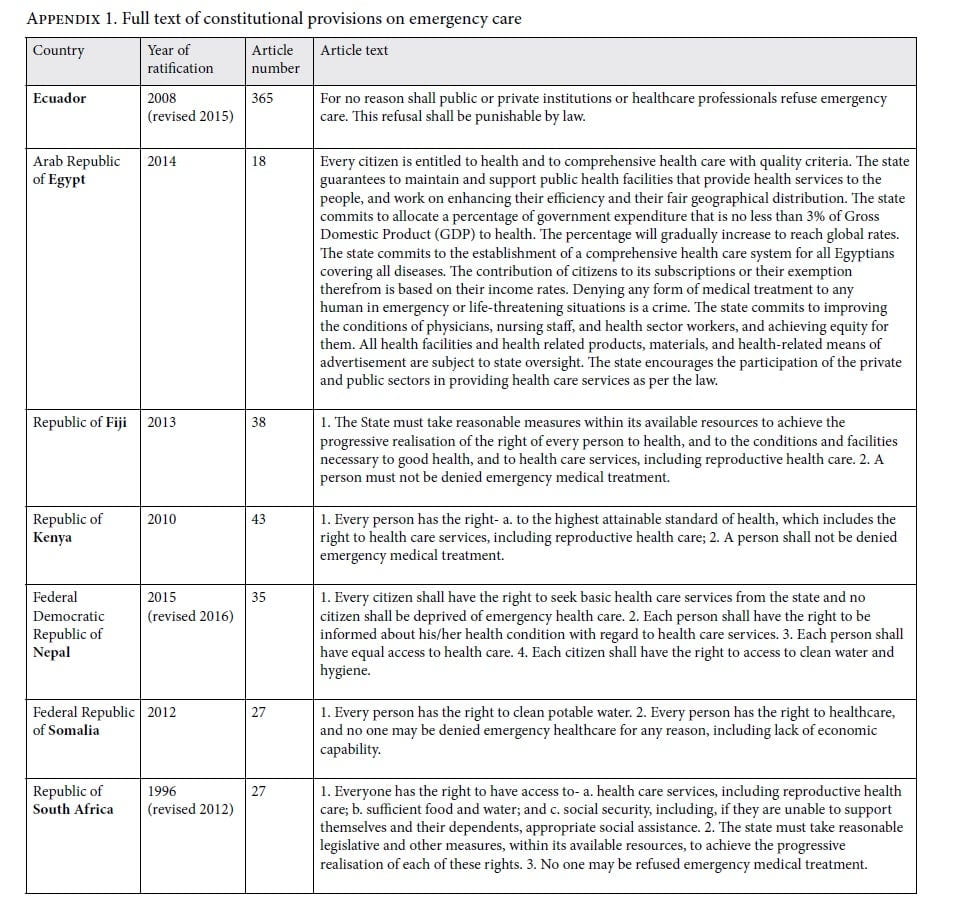
In contrast, accessibility is addressed in all 10 constitutions. In General Comment 14, accessibility is subdivided into the categories of nondiscrimination, physical accessibility, affordability, and information accessibility. Nondiscrimination in emergency care is best addressed by six of the ten constitutions. Kenya stipulates universal access by stating that “[a] person shall not be denied emergency medical treatment.”27 Meanwhile, South Africa decrees that “[n]o one may be refused emergency medical treatment.”28 In another example of nondiscrimination, Egypt states that “[d]enying any form of medical treatment to any human in emergency or life-threatening situations is a crime.”29 A seventh constitution implies this same universal access, as well as the accompanying enforcement, in its article 365, stating that “[f]or no reason shall public or private institutions or healthcare professionals refuse emergency care. This refusal shall be punishable by law.”30 The remaining three countries that address emergency care in constitutional provisions inherently limit access by using the term “citizen” in place of “person” or “human.” For example, Nepal specifies that “no citizen shall be deprived of emergency health care,” thereby excluding vulnerable and marginalized populations, such as migrants or refugees, and potentially violating principles of the right to health.31
Affordability, as a subclassification of accessibility, is addressed by only three constitutions, two of which are classified as low income and one as lower-middle income by the World Bank. Sudan and South Sudan both state that emergency care will be free. Somalia, meanwhile, states that “no one may be denied healthcare for any reason, including lack of economic capability.”32 In practice, these commitments will require substantial governmental funding or insurance schemes. It is important to note that seeking care has been linked to catastrophic health expenditures, further worsening the cycle of poverty and poor health.33 In the context of emergency conditions, this is likely even more important for LMICs that are saddled with a disproportionate burden of conditions amenable to emergency care.34 The two other categories of accessibility—physical and information accessibility—are not specifically addressed in any of the constitutions included in our study.
Likewise, the notion of acceptability—which encompasses cultural appropriateness and abidance by medical ethics—is not addressed by any of the 10 constitutions. Nor is quality, which refers to scientific or medical appropriateness. Without an emphasis on these attributes at the constitutional level, downstream policymaking may not yield focused guidance on these core components of comprehensive, effective emergency care delivery. Furthermore, any benefit that the availability and accessibility of emergency care affords may be negated if the care does not successfully manage the death and disability of emergent medical conditions through quality emergency care. As much as the human rights-based approach to health system development aims to develop the “capacity of duty bearers to meet their obligations,” it also serves to empower “rights-holders to effectively claim their health rights.”35 Without explicit attention to the acceptability or quality of emergency care systems in the law, it remains unclear if rights-holders will be able to demonstrate these rights as effectively in the judicial system.
When we applied the Kinney-Clark typology for health-related provisions in national constitutions, we classified the majority of articles as either statements of duty or statements of entitlement. For example, article 29 of the Constitution of Zimbabwe reads, “The State must take appropriate, fair and reasonable measures to ensure that no person is refused emergency medical treatment at any health institution,” representing a statement of duty on the part of the government.36 In contrast, article 38.2 of the Constitution of Fiji states, “A person must not be denied emergency medical treatment,” enshrining an entitlement of the people but not specifically addressing the role of the government.37 We found no constitutional provisions that could be classified as statements of aspiration, programmatic statements, or referential (to treaties or other statutes) statements. While programmatic statements would have been more detailed and prescriptive, it is not surprising that this level of detail is often omitted from constitutional provisions. However, the statements of duty and entitlement serve to prioritize a particular agenda and enable subsequent legislation, regulation, and judicial rulings that elaborate on the specifics of the guarantee of access to emergency care.
According to General Comment 14, governments must respect, protect, and promote (or fulfill) the right to health. Of the 11 provisions identified in our search, many contain language that suggest an obligation to respect or protect a right to emergency care, yet only three contain language that implies a duty to actively promote this right. Whereas the obligation to respect requires nations to refrain from interfering with the right to emergency care and the obligation to protect requires nations to prevent third parties from violating the right, an obligation to fulfill or promote would necessitate nations to “adopt appropriate legislative, administrative, budgetary, judicial, promotional and other measures toward the full realization of the right to health.”38
The overall significance of identifying 10 constitutions that address access to emergency care in LMICs is twofold. From a human rights perspective, these provisions establish a legal guarantee for access to a lifesaving service that, without such laws, could be afforded to some but denied to others based on factors such as ability to pay, national origin, or other discriminated status. From a public health perspective, these constitutional provisions—in conjunction with not-yet catalogued laws and regulations—are hypothesized determinants of increased access to quality emergency care. The aim of increasing access to quality emergency care is to reduce a substantial proportion of the global burden of disease that disproportionately affects LMICs. While there have been no studies demonstrating an association between constitutional laws and improved health emergency outcomes, anecdotal descriptions of post-ratification progress in countries such as Kenya and South Africa suggest that constitutional laws should not be ignored by policy makers. In fact, the increasing use of such constitutional provisions since their first appearance in 1996 could indicate a trend toward the adoption of constitutional guarantees of emergency care in more countries in the near future.
Limitations
Our study is limited to constitutional law, and as such, our results do not necessarily correlate with the prevalence or characteristics of other governance mechanisms for guaranteeing access to emergency care, such as statutory law (legislation), regulations, policies, and court rulings. For example, the United States, with a constitution long predating the advent of emergency care, has a statute protecting people’s right to access emergency care (called the Emergency Medical Treatment and Labor Act) but does not have a constitutional guarantee.39
The Constitute Project is a repository of national constitutions and includes English translations of documents originally published in other languages. There is thus the potential for subtle alterations in the meaning of articles that have been translated into English. Our search returned only 11 provisions from 10 national constitutions, and many of these provisions employ similar wording. The limited number of texts available for qualitative analysis and the homogeneity of their wording restricts the identification of other important themes for legislating access to emergency care. Finally, our study did not aim to correlate the presence of constitutional provisions on emergency care to any real-time markers of accessibility or emergency care system development.
Further studies are needed to understand the impact and effectiveness of constitutional provisions on emergency care. There remain questions regarding downstream legislation and regulation, as well as the judicial challenges that are made possible by such constitutional provisions. With a limited number of constitutions containing guarantees of emergency care accessibility, it is not currently feasible to correlate with health or human rights outcomes without a more detailed causal link analysis. However, countries such as Kenya have seen further codification of the right to emergency care since the passage of their constitutions, including through legislation and regulations that further detail and codify the right to emergency care.40 Future studies are needed to assess the degree to which these constitutional rights impact health and human rights outcomes. Such analysis could provide insights into the barriers that need to be overcome in order to truly guarantee access to emergency care. Additionally, there remains uncertainty regarding which components (e.g., scope of coverage, types of obligations, penalties, and enforcement) of emergency care legislation are necessary, which components can be practically and ethically modified to cultural context and resource availability, and which financing options are best suited to govern access to emergency care.
Conclusion
Constitutional law has the potential to empower governments to respect, protect, and promote the right to emergency care, an essential lifesaving health resource. As demonstrated by our review of national constitutions from 195 countries, constitutional guarantees of this right currently exist on a limited basis and are phrased as either statements of duty or statements of entitlement. They address nondiscrimination and affordability but do not address the acceptability or quality of emergency care. Despite the limited number of constitutions that guarantee access to emergency care, the presences of the 10 that were identified speaks to the potential to harness such governance tools to expand the right to emergency care where none previously existed. While consensus is still needed regarding the most essential components of these provisions, these findings demonstrate a recent movement to codify and guarantee emergency care in many of the countries that are most in need of strengthened emergency care systems. The international community is urged to consider how constitutional laws can best improve the availability, accessibility, acceptability, and quality of emergency care globally.
Taylor W. Burkholder, MD, MPH, is an assistant professor of emergency medicine at the Keck School of Medicine, University of Southern California, Los Angeles, USA.
Madeline Ross, MD, is a clinical instructor of emergency medicine and a fellow in global emergency medicine at the University of Colorado School of Medicine, Aurora, USA.
Lily Vartanyan, MD, is a resident physician in emergency medicine at the LAC+USC Medical Center, Los Angeles, USA.
Harveen Bergquist, MD, MSc, is an honorary senior lecturer in the Division of Emergency Medicine at the University of Cape Town, South Africa.
Please address correspondence to Taylor W. Burkholder. Email: taylor.burkholder@med.usc.edu.
Competing interests: None declared.
Copyright © 2021 Burkholder, Ross, Vartanyan, and Bergquist. This is an open access article distributed under the terms of the Creative Commons Attribution Non-Commercial License (http://creativecommons.org/licenses/by-nc/4.0/), which permits unrestricted noncommercial use, distribution, and reproduction.
References
- J. M. Hirshon, N. Risko, E. J. Calvello, et al., “Health systems and services: The role of acute care,” Bulletin of the World Health Organization 91/5 (2013), pp. 386–388; T. A. Reynolds, H. R. Sawe, A. M. Rubiano, et al., “Strengthening health systems to provide emergency care,” in Disease Control Priorities: Improving Health and Reducing Poverty (Washington, DC: World Bank, 2017), pp. 247–265.
- C. Y. Chang, S. Abujaber, T. A. Reynolds, et al., “Burden of emergency conditions and emergency care usage: New estimates from 40 countries,” Emergency Medicine Journal 33/11 (2016), pp. 794–800.
- L. C. Carlson, T. A. Reynolds, L. A. Wallis, et al., “Reconceptualizing the role of emergency care in the context of global healthcare delivery,” Health Policy and Planning 34/1 (2019), pp. 78–82.
- Reynolds et al. (see note 1); J. Razzak, M. F. Usmani, and Z. A. Bhutta, “Global, regional and national burden of emergency medical diseases using specific emergency disease indicators: Analysis of the 2015 Global Burden of Disease Study,” BMJ Global Health 4/2 (2019), p. e000733.
- P. O. Ouma, J. Maina, P. N. Thuranira, et al., “Access to emergency hospital care provided by the public sector in sub-Saharan Africa in 2015: A geocoded inventory and spatial analysis,” Lancet Global Health 6/3 (2018), pp. e342–e350.
- H. Geduld, E. J. C. Hynes, L. A. Wallis, et al., “Hospital proximity does not guarantee access to emergency care,” Lancet Global Health 6/7 (2018), p. e731 .
- L. Cannoodt, C. Mock, and M. Bucagu, “Identifying barriers to emergency care services,” International Journal of Health Planning and Management 27/2 (2012), pp. e104–e120.
- A. Fraser, J. Newberry Le Vay, P. Byass, et al., “Time-critical conditions: Assessment of burden and access to care using verbal autopsy in Agincourt, South Africa,” BMJ Global Health 5/4 (2020), p. e002289.
- C. N. Mock, D. nii-Amon-Kotei, and R. V. Maier, “Low utilization of formal medical services by injured persons in a developing nation: Health service data underestimate the importance of trauma,” Journal of Trauma: Injury, Infection, and Critical Care 42/3 (1997), pp. 504–513; E. Kilonzo, “Private hospital criticised for failing to admit crash victim,” Daily Nation (2015).
- G. Backman, P. Hunt, R. Khosla, et al., “Health systems and the right to health: An assessment of 194 countries,” Lancet 372/9655 (2008), pp. 2047–2085.
- Committee on Economic, Social and Cultural Rights, General Comment No. 14, The Right to the Highest Attainable Standard of Health, UN Doc. E/C.12/2000/4 (2000).
- T. W. Burkholder, K. Hill, and E. J. Calvello Hynes, “Developing emergency care systems: a human rights-based approach,” Bulletin of the World Health Organization 97/9 (2019), pp. 612–619.
- World Health Organization, Health systems governance for universal health coverage: Action plan (Geneva: World Health Organization, 2014).
- World Health Assembly, Resolution 72.16 (2019).
- K. S. Chawla, L. Rutkow, K. Garber, et al., “Beyond a moral obligation: A legal framework for emergency and essential surgical care and anesthesia,” World Journal of Surgery 41/5 (2017), pp. 1208–1217.
- H. V. Hogerzeil, M. Samson, J. V. Casanovas, et al., “Is access to essential medicines as part of the fulfilment of the right to health enforceable through the courts?,” Lancet 368/9532 (2006), pp. 305–311.
- M. M. Siems, “Varieties of legal systems: Towards a new global taxonomy,” Journal of Institutional Economics 12/3 (2016), pp. 579–602.
- Hogerzeil et al. (see note 16).
- K. Perehudoff, B. Toebes, and H. Hogerzeil, “Essential medicines in national constitutions: Progress since 2008,” Health and Human Rights Journal 18/1 (2016), pp. 141–156.
- Committee on Economic, Social and Cultural Rights (see note 11).
- Perehudoff et al. (see note 19).
- E. D. Kinney and B. A. Clark, “Provisions for health and health care in the constitutions of the countries of the world.,” Cornell International Law Journal (2004)
- J. Heymann, A. Cassola, A. Raub, et al., “Constitutional rights to health, public health and medical care: The status of health protections in 191 countries,” Global Public Health 8/6 (2013), pp. 639–653; C. Jung, R. Hirschl, and E. Rosevear, “Economic and social rights in national constitutions,” American Journal of Comparative Law 62/4 (2014), pp. 1043–1094.
- Heymann et al. (see note 23).
- Reynolds et al. (see note 1).
- C. Flood and A. Gross, “Litigating the right to health: What can we learn from a comparative law and health care systems approach,” Health and Human Rights Journal 16/2 (2014), pp. 62–72.
- Constitution of Kenya (2010). Available at https://www.constituteproject.org/constitution/Kenya_2010?lang=en.
- Constitution of the Republic of South Africa (1996). Available at http://www.justice.gov.za/legislation/constitution/SAConstitution-web-eng.pdf.
- Constitution of the Arab Republic of Egypt (2014). Available at https://www.constituteproject.org/search?lang=en&q=egypt&status=in_force&status=is_draft.
- Constitution of the Republic of Ecuador (2008). Available at https://www.constituteproject.org/constitution/Ecuador_2015?lang=en.
- Constitution of Nepal (2015). Available at https://www.constituteproject.org/constitution/Nepal_2015.pdf.
- Provisional Constitution of the Federal Republic of Somalia (2012). Available at https://www.constituteproject.org/constitution/Somalia_2012?lang=en.
- World Health Organization, A human rights-based approach to health (Geneva: World Health Organization, 2009); A. Leive, “Coping with out-of-pocket health payments: Empirical evidence from 15 African countries,” Bulletin of the World Health Organization 86/11 (2008), pp. 849–856.
- G. Bukhman, A. O. Mocumbi, R. Atun, et al., “The Lancet NCDI Poverty Commission: Bridging a gap in universal health coverage for the poorest billion,” Lancet 396/10256 (2020), pp. 991–1044.
- World Health Organization (see note 33).
- Constitution of Zimbabwe (2013). Available at https://www.constituteproject.org/constitution/Zimbabwe_2013.pdf.
- Constitution of the Republic of Fiji (2013). Available at https://www.constituteproject.org/constitution/Fiji_2013.pdf?lang=en.
- Committee on Economic, Social and Cultural Rights (see note 11).
- United States, Emergency Medical Treatment and Active Labor Act (1986).
- Republic of Kenya, The Health Act (No. 21) of 2017 (2017).

