Human Rights and the Confinement of People Living with Dementia in Care Homes
Volume 22/1, June 2020, pp 7 – 21
Linda Steele, Ray Carr, Kate Swaffer, Lyn Phillipson, and Richard Fleming
Abstract
This paper responds to growing concerns in human rights practice and scholarship about the confinement of people living with dementia in care homes. Moving beyond the existing focus in human rights scholarship on the role of restrictive practices in confinement, the paper broadens and nuances our understanding of confinement by exploring the daily facilitators of confinement in the lives of people with dementia. The paper draws on data from focus groups and interviews with people living with dementia, care partners, aged care workers, and lawyers and advocates about Australian care homes. It argues that microlevel interrelated and compounding factors contribute to human rights abuses of people living with dementia related to limits on freedom of movement and community access of people living with dementia, at times irrespective of the use of restrictive practices. These factors include immobilization and neglect of residents, limited and segregated recreational activities, concerns about duty of care and liability, apprehension of community exclusion, and pathologization and subversion of resistance. It is necessary to challenge the organizational, cultural, economic, and social dynamics that shape day-to-day, microlevel, routine, and compounding factors that remove the agency of people living with dementia and in turn facilitate entrenched and systematic human rights breaches in care homes.
Introduction
The Special Rapporteur on the right of everyone to the enjoyment of the highest attainable standard of physical and mental health has emphasized that confinement in health care settings can become a barrier to mental and physical health.[1] While the Special Rapporteur does not specifically mention care homes, his concerns align with growing awareness in human rights scholarship and practice of the impacts of confinement on the mental and physical well-being of people living with dementia in care homes. The Special Rapporteur on the rights of persons with disabilities has recently identified a range of human rights issues affecting people living with dementia, including “stigma and stereotypes,” the absence of rehabilitation services, being “assumed to possess weak or even no agency,” being at greater risk than other older people of “violence, abuse and neglect,” and a lack of building accessibility.[2] She emphasizes the particularly concerning conditions in care homes:
Many of these facilities are in fact segregated institutions, where staff exercise control over the person’s daily life and make decisions about the person’s care, including their placement in segregated locked wards, the administration of chemical restraints such as psychotropic drugs and the use of other physical restraints.[3]
An examination of confinement in care homes is timely because of growing international momentum to improve the human rights of people living with dementia. The United Nations Convention on the Rights of Persons with Disabilities (CRPD) enshrines the rights to non-discrimination and equality, including in relation to deprivation of liberty, the exercise of legal capacity, and consent to medical treatment.[4] People living with dementia and their organizations, such as Dementia Alliance International, are advocating for equal rights for people living with dementia in care homes.[5] Scholars and practitioners in public health and dementia care, traditionally focused on individual quality of care, are also now engaging with human rights.[6] International civil society is taking up this issue as well; for example, Human Rights Watch recently reported on chemical restraint in Australia and the United States.[7] The ongoing development of a Convention on the Rights of Older Persons promises enhanced recognition of the rights of people living with dementia.[8]
Turning to Australia, our focus, in 2016–17 there were 902 providers of aged care offering 200,689 residential places in 2,672 facilities, at a cost to the government of AUD11.9 billion.[9] Moreover, “[s]ince 2008–09, the proportion of people entering residential care with a diagnosis of dementia has been consistently between around 43 per cent and 45 per cent of all permanent residents entering care.”[10] These statistics alone indicate the increasing significance of care homes to the well-being and enjoyment of human rights of people living with dementia. However, a number of government reviews and inquiries have recently drawn attention to systemic shortcomings in the aged care system and have flagged their impact on human rights and people living with dementia (even if tangentially). Most notable in this respect is the current Royal Commission into Aged Care Quality and Safety (“Aged Care Royal Commission”), which states in its 2019 interim report that “[m]any people receiving aged care services have their basic human rights denied. Their dignity is not respected, and their identity is ignored. It most certainly is not a full life.”[11] It should be noted that Royal Commissions present a particularly significant opportunity to explore systems; in this way, they differ from most legal mechanisms, such as courts, which are focused on specific justiciable issues concerning a particular individual’s specific experience with a system. However, there is a long critique of government inaction on Royal Commission recommendations for systemic reform.[12] This is perhaps exacerbated in the context of aged care. While concepts such as “dignity” feature in Australia’s new Aged Care Quality Standards, possibly suggesting promising leanings toward human rights in aged care service delivery, there is a disappointing absence of reference in these standards to individuals’ access to avenues for enforcement or redress for breach.[13] In the Aged Care Royal Commission’s terms of reference and interim report, there is a similar absence of mention of—let alone in-depth consideration and commitment to action on—matters of enforceable legal or human rights and recourse to redress. Despite the possibly limited impact of the Aged Care Royal Commission on human rights reforms to aged care policy and practice, the evidence coming out of the inquiry confirms the urgency of increased engagement by human rights scholars and practitioners with care homes as a site of widespread and profound human rights violations.
We begin this paper by discussing some of the existing literature on the confinement of people living with dementia in care homes. Next, we introduce methods and present key findings from focus groups and interviews, identifying a series of interrelated factors that contribute to human rights breaches pertaining to confinement. We then reflect on the findings in the context of human rights and offer some recommendations for human rights scholars and practitioners. Our reflections are also relevant and of benefit to aged care and health policy workers who might very well have more capacity to affect the legal, policy, and service delivery frameworks that directly shape the conditions in aged care.
The confinement of people living with dementia in care homes
People living with dementia have explicitly expressed the desire not to be confined in care homes. Drawing on results from interviews and online focus groups with people living with dementia, a recent book by Kate Swaffer (a dementia human rights advocate living with dementia) and Lee-Fay Low explains what people living with dementia want in residential care. They want non-institutionalized settings, no segregation or locked dementia units, and the absence of apparent barriers or walls. They also want ample space inside and outside, as well as access to outdoor recreational areas for walking, bird watching, and enjoying natural environments. Swaffer and Low explain that people living with dementia want re-ablement, rehabilitation, exercise, and recreational activities; the ability for the outside community to come in; the opportunity to have visitors stay overnight; and strategies to enable independence.[14] However, as documented by the literature on aged care, care homes commonly employ a wide range of physical and environmental barriers to movement, including locked doors, lap sashes and belts, bed rails, and segregated wards.[15] Having a secured perimeter is often taken for granted as necessary for a care home where people living with dementia reside. While there is ample evidence that obvious “safety” features such as high fences can increase depression and agitation and provoke attempts to escape, staff and families continue to defend their use as being necessary to provide protection from the perils of access to the outside of the care home and getting lost. In addition, medications are overused in care homes, sometimes as a means of restraining people with dementia without consent.[16]
Human rights scholars’ and practitioners’ exploration of the confinement of people living with dementia in care homes has focused largely on the deprivation of or restriction on liberty through the use of restrictive practices such as those described above. However, a more nuanced examination of the dynamics within aged care settings resonates with the observation made by the Special Rapporteur on health (in the context of the right to health) that “[a] structural assessment … of the ‘climate’ of prison, detention and confinement, that is, how people experience life and survive once inside, how power is structured and organized and the structural factors that enable practices and institutions to persist, would help to broaden such responses.”[17] He elaborates on the systemic cultures that shape spaces of confinement:
Centres of … confinement often concentrate people from the most vulnerable situations, including those who are medically vulnerable. The centres are often characterized by inhumane physical and psychosocial environments and unequal structures of power frequently rooted within racist and violent pasts. The unpopularity and powerlessness of those deprived of liberty and confined leave them with no voice and few defenders to advocate for their dignity. These factors shape an ecology of deprivation that significantly compromises the ethical and effective organization and delivery of health care.[18]
In the course of grappling with the ethical, legal, and practical challenges to providing high-quality care to people living with dementia in care homes, health sciences research implicitly points to some less tangible means through which confinement occurs.[19] This research indicates that some of the most common forms of indirect restriction are seating a person in a deep chair that they cannot get out of, placing a table in front of their chair, leaning a wheelchair back, and otherwise ensuring that the person is “parked.”[20] As with fences, these techniques are frequently defended as necessary to protect the safety of residents and to enable daily care tasks to be performed.[21] Yet sociological scholarship emphasizes the socially constructed nature of risk, in particular the riskiness of people with dementia “wandering.”[22] Several scholars have argued that the extent to which doors are locked and the movement of people living with dementia is restricted, particularly with regard to outside spaces and beyond care home perimeters, varies depending on an institution’s philosophy, approach to risk, and understanding of dementia.[23] Frances Tufford et al. point out that the prevalent prioritization of risk management over residents’ choice and well-being indicates a cultural attitude of devaluing older people.[24]
Mark Skinner et al. argue that the social inclusion of people with dementia requires “supporting the rights for full participation with resources and services in relationships and activities across economic, social and cultural spheres,” including for those people living in institutional settings.[25] The health sciences literature, however, documents decisions made by care homes not to include people living with dementia in social and recreational activities. Research on residents’ access to community beyond the perimeter of a care home suggests that facilities often provide only very limited opportunities.[26] Underlying the lack of provision of such opportunities, Sherry L. Dupuis et al. identify resource limitations, as well as staff concerns about the suitability of the community for residents, and vice versa.[27] People with dementia in residential care are accordingly less likely to have opportunities for community access. Restrictions on movement into care homes of family and friends also contribute to the sense of confinement experienced by residents. Jessica E. Thomas et al.’s research shows that a care home’s environment and location can be a barrier to family and friends visiting.[28] Unsurprisingly, a lack of continuity with the broader community is associated with depression among residents.[29]
Methods
This paper reports on the findings of an Australian project that involved interviews and focus groups with people living with dementia, care partners, care home workers, and lawyers and advocates. Taking insights from health sciences literature and observations of the Special Rapporteur on the right to health as a point of departure, this paper aims to deepen human rights scholars’ and practitioners’ understanding of the drivers and facilitators of confinement in care homes, with the ultimate aim of enhancing the human rights of people living with dementia.
The project researchers constitute an interdisciplinary team traversing law, public health, dementia design, psychology, and science and technology studies, and include a leading international advocate on the rights of persons living with dementia who herself has younger onset dementia (Kate Swaffer). Our project was guided by an advisory group that included people living with dementia, care partners, care home professionals, and lawyers and advocates for people living with dementia.
Recruitment
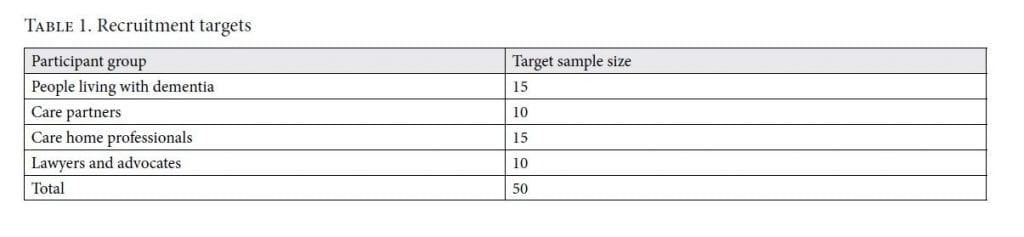
We recruited a convenience sample of participants by promoting our research to organizations whose members or staff identify with the relevant participant groups (people living with dementia, care partners, care home professionals, and lawyers and advocates). Promotion occurred via email, websites, Facebook, and Twitter. All those who responded were provided with the participant information statement and consent form and were required to provide written consent to participate. Our recruitment targets are outlined in Table 1.
Following extensive recruitment efforts, our final sample of participants consisted of 5 people living with dementia, 19 care partners, 12 care home professionals, and 9 lawyers and advocates. Overall, this was consistent with our targets, with the exception of the low numbers of participants living with dementia. We were unable to recruit any aged care regulatory officials.
Data collection
We gave respondents the choice of participating in an individual interview (via Zoom or phone) or an in-person focus group. Participants were asked questions about their current awareness and experiences of community access and freedom of movement in relation to care homes (commonly referred to in Australia as “aged care facilities”), as well as questions about their views on human rights (the latter is reported in a separate paper).[30] Questions about current awareness and experiences of community access and freedom of movement included the following:
- Do you know if people living with dementia in aged care facilities have access to the community? How does community access occur?
- Do you know if people living with dementia in aged care facilities have access to the full range of recreational and social spaces and activities in the aged care facility?
- Do you know of anyone who has been restricted in their ability to move around or beyond an aged care facility through the built environment? How did this occur?
Interviews ran for approximately 40–60 minutes, and focus groups ran for 1.5–2 hours. To maximize participants’ comfort and freedom, the two focus groups with a mixture of participant groups were conducted in two stages. The first stage, on current practice, separated participants with dementia and care partners from those who were care home professionals. For the second stage, all participants came together to discuss human rights.
Analysis
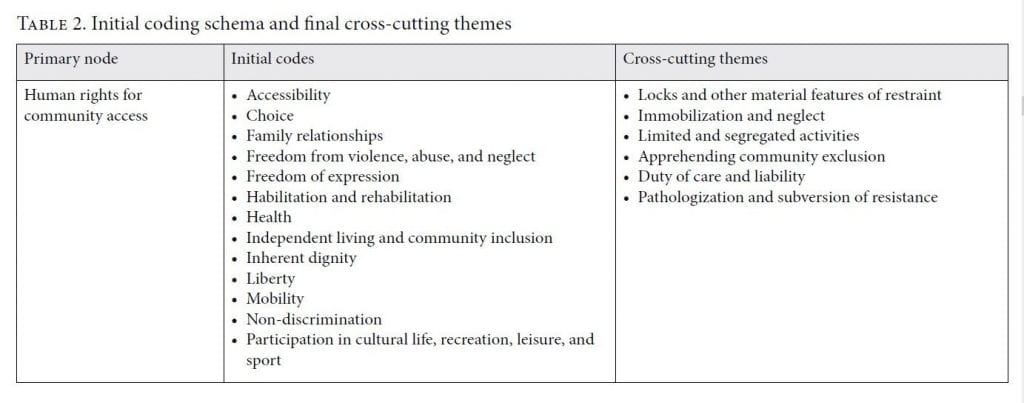
The data was thematically analyzed. Initial coding was undertaken manually by three of the authors. Each engaged in iterative coding of a small sample of transcripts. Following a discussion of emerging themes, a coding schema was applied to identify barriers to a wide range of CRPD rights relevant to freedom of movement and community access. This approach was taken in order to ensure that the analysis drew out the human rights implications of the data (with particular attention to the material, legal, and cultural dynamics affecting day-to-day experiences of restricted movement and community access). The broad range of rights utilized in coding enabled a more nuanced understanding of the dynamics of confinement, notably a shift away from a focus on the deprivation of liberty toward one that includes rights related to various facets of the care home experience whose breach can indirectly give rise to confinement. For example, attention to the right to participation in cultural life, recreation, leisure, and sport highlighted the impact that segregated bus trips have on confinement (a point we elaborate on below)—a finding that would not have emerged if we had concentrated only on the use of locks, lap belts, and so forth as the focus of the right to liberty and security of the person. Transcripts were uploaded into NVivo 12 to support systematic coding by one of the authors. Another author then identified themes emerging from and cutting across the codes for discussion in this paper, choosing those themes that were particularly relevant to enhancing human rights scholars’ and practitioners’ engagement with confinement in care homes.
Findings
Interestingly, while participants mentioned physical and environment restrictions on liberty (predominantly locked doors and gates) and ways in which people living with dementia had limited or no access to community activities or spaces, they generally did not perceive these as forms of confinement or restrictions on liberty or, indeed, even as problematic or unusual. As an overarching observation, this suggests that those involved in the day-to-day support and advocacy of people living with dementia are largely oblivious to significant human rights violations. We now turn to draw out some of the dynamics that contribute to restricted freedom of movement and limited community access and, we argue, systemic, day-to-day practices of confinement in care homes.
Locks and other material features of restraint
Many of the participants identified material features of restraint that restrict the movement of people living with dementia in care homes. However, participants generally mentioned these features only after being specifically asked about them by the interviewer, suggesting that they are unquestioned aspects of care home culture. One care home professional described these circumstances and attributed them to safety:
Across all of our sites where we have dementia units, they’re behind an access-control door. But it’s always done because of the residents’ safety, so they don’t wander out onto the street, so they don’t go … It’s for their safety. (focus group 2, care home professional)
Locked doors can also affect the ability of people living with dementia to receive visitors, as described by one care partner who has a friend in a dementia care unit (DCU) “cottage”:
All the cottages are locked so there’s, the facility, itself, just has a white picket fence but it’s double locked everywhere. Each cottage has its own little back yard and that’s got high bars et cetera … So, it really is—this particular friend is really going through psychological distress. Feeling locked in … So, if I go to visit him, I have to call ahead to the cottage and tell them that I’m coming and then I get to the cottage and knock or ring. And then I say who am I coming to see and then they open the door. (focus group 1, care partner)
Participants also observed forms of physical restraint. One person living with dementia who had visited care homes noted:
I’ve seen them sat with the tray tables and they were still sitting there hours later with the tray table in front of them. (interview 5, person with dementia)
As we discuss further below in relation to the subversion of resistance, some care partner participants had knowledge of chemical restraint in relation to their spouses or parents with dementia. These findings illustrate that restrictive practices are used in care homes and clearly affect mental well-being. However, as we now turn to show, the picture of confinement in care homes is much more complex and can occur in more subtle or unexpected ways.
Immobilization and neglect
The most commonly mentioned factor affecting freedom of movement was the removal of means of mobility. This includes not providing mobility aids, opportunities for physical exercise, or meaningful activities to prevent decline and distress.
The first thing they do with people with walking frames is take the walking frame away from them and put them in a wheelchair because they don’t have the staff to support them while they’re walking. And they sat in the wheelchair, and then they just … they’re parked. (focus group 1, care partner)
Several participants mentioned people being seated (“parked”) in front of televisions:
They’re parked … No, I’m not talking about them being restrained. I’m talking about them being put in an area like the common area, where the TV’s on, and, essentially, just left there. And they’re supposed to occupy themselves, I suppose, by looking at the TV for endless hours. Or, alternatively, they’re left in their room, perhaps in their bed or in their chair, but with no real way of them getting up and being able to move about and interact. (interview 3, lawyer)
These indirect means of restricting people’s movement can have profound impacts on people’s physical and mental well-being. They not only prevent immediate movement by residents with dementia but may reduce their capacity for mobility over time, in some instances physically disabling them.
Limited and segregated activities
While some care partners spoke positively about the opportunities for family and friends to enter the care home to visit residents with dementia and opportunities for the broader community to frequent cafes operating commercially on the care home site, many participants mentioned the limited opportunities for people living with dementia to move freely and spontaneously in the community, instead being restricted to excursions in groups that generally involved pre-determined activities and destinations. A common example offered was a bus trip:
Well, actually, where the sister is, they do occasionally have external activities, bus trips to places. (focus group 2, person with dementia)
My experience is … that the bus trips go out, but the residents don’t get off the bus. They maybe go for an ice-cream or view of the coastline. (focus group 1, care home professional)
A participant living with dementia who lives in a care home (but not in a DCU) elaborated on the bus trip they regularly participate in:
Yes, so there are outings and then there’s a bus that goes on a Friday … It’s only three quarters of an hour, but it just goes for a tour around the area and you see, you know, interesting points, history in the area because there’s lots … Being in the gold fields, there’s lots and lots of history in the area, you know. So I know I enjoy going out on that … we just sit in the bus because it’s only about three quarters of an hour, that one. (interview 10, person with dementia)
While some care partners spoke positively of the recreational and social opportunities available to residents with dementia within the care home, some participants noted that people living with dementia were not always included in the full range of external activities on offer to other residents. One participant living with dementia (focus group 2) said that people in the DCU were taken out on separate bus trips and these trips were “far rarer” and “more limited.” This was corroborated by another professional:
They don’t really have the full range of the activities that the other residents in the main nursing home have. (focus group 1, care home professional)
Individualized community access (in the dual sense of going out by oneself and choosing the timing and activities) was rare and contingent on staff availability and access to transportation. Given the limited resourcing of care homes, it thus depended on individuals’ access to family or friends who could help them.
Some people are denied access to the full range of social and recreational opportunities, being restricted to specific sections of the care home designated for people living with dementia. These areas are not always of the same quality as other areas:
They have opportunities to do activities in a certain area, a communal area where they would have music or people to visit them, community visitors and whatnot … that isn’t like the dementia unit … the rest of the facility have more open plan areas, gardens they can go and sit at. Although there are little gardens in the dementia unit but it’s not as—what’s the word?—fancy versus the other non-dementia unit areas. (interview 12, advocate)
A care partner similarly described the lack of stimulating activities and spaces in the DCU where her husband had lived:
There was a very, very basic garden around the cottage with a little path that walked round the perimeter of the cottage. And there were 14 residents in each cottage. So, some of them seemed to get into a habitual behaviour of walking round and round on this path around the perimeter of the cottage, which had a high fence around it. So, my husband eventually joined the walk. Which they do on their own volition, just going round in circles on this pathway. (interview 6, care partner)
Thus, people living with dementia can come to be confined through exclusion from opportunities to venture outside of the care home or to even traverse the care home itself, and through reduced opportunities for social interaction and meaningful activities. These means of confinement are striking in their segregating and discriminatory character, yet the majority of participants, across all groups, took these as normal or at least inevitable and unchangeable.
Apprehending community exclusion
Many care home professionals and care partners noted that the lack of understanding of dementia in members of the community caused fear, which can lead to residents with dementia being prevented from having access to the community:
Somebody has got a disability and he’s got a wheelchair; the public is aware that this one, we can help them in this way. But with dementia, there’s lack of awareness on how they present and the help that they need. (focus group 2, care home professional)
Participants also noted that public spaces outside of the care home might not be physically accessible for people living with dementia.
In this way, people living with dementia are effectively fenced in by both the stigma around dementia and the staff perception that negative community experiences are too difficult to manage. Yet, at the same time, the segregation of people with dementia cuts off opportunities for the whole community to develop a better understanding of living with dementia, thus reinforcing the “need” for confinement.
Duty of care, risk, and liability
Perceptions of duty of care play a significant role in shaping care home staff’s decisions about where in the care home people with dementia live, the circumstances in which they live, and whether they are included in excursions. Staff in some care homes quickly classified these residents’ riskiness, as noted by this care partner:
In terms of restriction or access to community services, the only one that was accessed … in the normal community … was to the local bowling club … In the minibus, which was once a week under supervision. For a small group of suitable residents. My husband participated in that on one occasion not long after he went there but was deemed to be a person who would be at risk after that one outing. That he was always looking at the horizon as though how he might escape, was their view, so he was banned from all future outings. (interview 6, care partner)
Lawyer and advocate participants, as well as some care partner participants, thought that duty of care toward residents with dementia was interpreted narrowly and arbitrarily by some care home staff as the physical safety of the individual. There was little consideration of the extent to which the duty of care pertained to emotional well-being or a duty to protect people’s rights and freedoms and to recognize personhood. Moreover, comments by some participants suggested that it is potentially directed toward concerns about protecting the care home from liability, rather than concern about the well-being of residents with dementia. For example, lawyers and advocates noted that fear of litigation may press care homes into risk-averse restrictions:
Now, when you run a nursing home you want to keep the people who live there safe because you have a duty of care, and also, you could be sued if you don’t do that. So, to really make sure people are safe and not in any danger, you completely remove risk, but when you do that you remove people’s rights and the quality of their lives. (interview 14, lawyer)
The lawyer explained how physical confinement and chemical restraint are central practices to the pursuit of this so-called duty:
To minimise that liability and have that duty of care, what a lot of aged care facilities do, will they heavily medicate the older person. That’s a form of restraint. They’ve got them drugged up all day. Then their behaviours are not going to come out, they’re not going to do much. You’re not going to have staff who have to, kind of, chase after them. (interview 14, lawyer)
Some care home staff noted the role played by family members in asserting a stringent focus on duty of care as physical safety. They highlighted the need for community education to teach people that being diagnosed with dementia should not automatically equate with people having their choices taken away from them:
And we’re seeing … that shift … in terms of litigation in response, as a sector… to “Mum fell” or that “Mum breaks her hip and dies.” Well, actually … they have a duty of care so Mum shouldn’t fall. But, in actual [fact], Mum’s choice was to actually get up and move and want to be free and not restricted. So I think there’s that whole balance there.
It’s really about educating the broader community around a diagnosis that doesn’t mean to say you don’t have the same rights as any other human being … I think it’s just about people understanding that just because Mum or Dad or Aunt or Uncle have a diagnosis of dementia doesn’t mean that they can’t make decisions about some things. (interview 16, care home professional)
These findings illuminate both misconceptions about the legal content of duty of care and a fear of liability for breach of duty in which considerations of the well-being and agency of the resident are largely absent. However, one care home professional (interview 18, care home professional) did recognize that “behaviors” of dementia that resulted in confinement for one’s purported safety were most likely the care home’s failure of its duty to provide residents with dementia with more stimulation.
The dominance of liability considerations in the choices made by care home staff about the movement and living circumstances of people living with dementia might inform the use of restrictive practices and, if an individual is not locked up or restrained, hinder individuals’ ability to practically realize their freedom of movement (for example, by receiving practical support from staff in order to be able to leave the care home or even leave their bed).
Pathologization and subversion of resistance
Some lawyers, advocates, care partners, and care home professionals expressed assumptions that people living with dementia cannot know and express their own views and needs. Such assumptions supported care homes denying people living with dementia the opportunities to make their own choices, rather than recognizing a basic desire for freedom. One person living with dementia stated:
So it was just a matter of, you know, there’s reasons that people go walking, if you know the history that they were up at dawn and they walked for five kilometres as the sun was coming up, well, that’s what they’re going to do. And so, you need to look at it with a, from outside of the square, why is this person doing this, why. (interview 5, person with dementia)
These assumptions also meant that attempts by people living with dementia to leave the care home were framed as subversive acts of escape or absconding. It is striking that behaviors that might be viewed as resistance or distress in response to the living circumstances of residents with dementia were pathologized as challenging or a clinical symptom of dementia, thus legitimating these individuals’ being locked away or excluded from community access.
I think the really telling thing is the number of people who are restrained because they object to the way they’re being treated. And, in fact, in many cases people don’t get the chance to say what they would like, they’re told what they’re supposed to do and then their reaction is, no. And so, if you react with no, it’s BPSD [behavioral and psychological symptoms of dementia], give you a shot, sit you in a chair, lap belt, whatever. Shut up and behave. (focus group 1, care partner)
Attempts to express distress and resistance in relation to one’s circumstances can simply sustain and legitimate the continuation of those circumstances. This was reflected in one care partner’s experiences in relation to her husband:
He wasn’t as well placed as he would’ve been in the past to discuss, explain, comment on how he was feeling about, for example, being confined to the cottage. So, you had to go by his behaviour, his expressions. And he subsequently made a few attempts to escape over the fence at different times in the following months. And was, of course, eventually caught and brought back … He did subsequently decline because they put him on anti-psychotics and that had a terrible effect on his capacities and, I think, just really accelerated his decline, rather rapidly from there … it certainly wasn’t discussed with me what the side effects were likely to be, and I don’t know whether people even knew or cared, perhaps, you know? It wasn’t ‘til sometime afterwards that I realised the decline we were seeing in him, both physically and mentally, was attributed to the anti-psychotics. (interview 6, care partner)
This participant’s husband was then moved to a locked cottage, which she noted she had not authorized:
They didn’t consult with me before doing that. The incident of him scaling the fence and trying to escape and he was caught. So, they brought him back and immediately transferred him and notified me afterwards. So, they seemed to consider … it was within their rights for the safety of the patient and for the safety of staff. (interview 6, care partner)
The pathologizing and subversion of resistance is a deeply concerning dynamic of confinement because it effectively prevents individuals from challenging the power relations within care homes.
To conclude our discussion of the findings, restrictive practices might be integral to the confinement of people living with dementia, yet they are just the “tip of the iceberg” of confinement, with multiple, less visible, and more diffuse dynamics at play. These dynamics could very well be present in relation to an individual or an entire care home free of restrictive practices. Indeed, our findings highlight indirect factors of restriction of liberty that are interrelated and compound one another in a negative spiral. The cultural understandings of dementia and people living with dementia is what threads together or interlocks the various facilitators of restriction, informing day-to-day choices made by care home staff and family members. If we envisage these compounding factors in terms of concentric circles, then at the very core sit profoundly troubling views about the ontology and epistemology of people living with dementia—who they are and can be, and what they can know and want. Our findings also reveal an aged care sector that is, at its heart, risk averse and procedural in nature. It is a sector that sustains a culture committed to minimizing risk, which is viewed through a narrow lens, at the expense of residents with dementia enjoying equality, autonomy, dignity, freedom, and other aspects integral to their physical and mental well-being.
Implications for human rights scholars and practitioners
Human rights scholars and practitioners have demonstrated increasing interest in the rights of people living with dementia, and the recent Aged Care Royal Commission has provided a forum through which to draw attention to these issues in the Australian context. The findings discussed in this paper suggest how the work of scholars and practitioners advocating for the human rights of people living with dementia can be broadened and enriched. The points we make here are also relevant to aged care and health policy makers, particularly because of their engagement with recommendations of the Aged Care Royal Commission. We conclude by identifying four key implications.
First, human rights scholars and practitioners can supplement their focus on restrictive practices and other legally ordered or regulated modes of deprivation of liberty with more microlevel dynamics affecting movement and agency in order to counter multifarious practices of confinement of people living with dementia. Restrictions occurring in the mundane, day-to-day provision of care can arise irrespective of formal restrictive practices and might not be associated with the kinds of decisions that care homes require from substituted decision makers. These issues might continue even if legal frameworks for restrictive practices are reformed. Confinement in care homes can so easily and systematically occur irrespective of the presence of legal authority or physical restraint (as compared to prisons, immigration detention facilities, or mental health facilities, where there are clearer legal and physical boundaries to confinement). One particular step that human rights practitioners and scholars can take is to argue for care homes to be classified as “places of detention” for the purpose of monitoring for torture under the Optional Protocol to the Convention against Torture. Australia has recently ratified this optional protocol, although it has yet to deem care homes (or locked units within them) as “primary places of detention” for monitoring, as advocated by civil society and legal scholars.[31] In Australia’s neighboring jurisdiction, New Zealand, locked dementia wards have been deemed places of detention and are now subject to the same scrutiny as jails.[32]
Second, human rights scholars and practitioners can advocate on issues relating to community access, social and recreational inclusion within care homes, and physical mobility. Lawyers and advocates providing support to people living with dementia in care homes should consider the extent to which existing laws and policies that might directly or indirectly pertain to these issues can be creatively utilized to challenge confinement.
Third, human rights scholars and practitioners should challenge the current interpretations and misappropriations of duty of care in relation to people living with dementia, and advocate for legal reforms that re-center people living with dementia as subjects of duty of care and see “duty of care” as requiring care homes to uphold freedom of movement and a full range of human rights. It would also be useful for all lawyers who work in elder and disability law to be made aware of the problems with the current narrow (mis)understandings of duty of care and to consider how they can shift community attitudes through their legal advice and advocacy.
Fourth, while it is important for human rights scholars and practitioners to advocate, in accordance with article 19 of the CRPD, for improved circumstances of those living inside care homes, there is a bigger, more long-term aim that requires their attention: deinstitutionalization, desegregation, and a transformation of the fundamental ways in which we provide housing and support to people living with dementia. For an increasing number of people with dementia, even current initiatives such as Dementia Friendly Communities and dementia villages run the risk of reinforcing ideas of dementia as “different” and of supporting inequality and, in turn, segregation and confinement. Indeed, the UN Special Rapporteur on the rights of persons with disabilities has noted this, stating, “Of particular concern is the emergence of dementia villages in developed countries, which represent a systemic form of disability-based segregation and isolation.”[33] While deinstitutionalization of the aged care system might seem an impossible and incomprehensible task, the child welfare and disability communities provide examples of the closure of large-scale institutions and movement of individuals into smaller-scale residences in the community. While these have not necessarily been wholly successful in addressing cultural, social, political, and legal drivers of oppression, they show that change is possible and provide case studies from which we might learn about how to garner policy and community momentum toward change (and the possible unintended consequences and risks we need to be alert to along the way).[34]
Ultimately, human rights scholars and practitioners (and aged care and health policy makers), mindful of principles of equality and personhood for all, should challenge the cultural logics around dementia that sustain confinement. One of these logics is that dementia is feared and needs to be hidden from the community. Another logic is that people living with dementia lack their own subjectivity and ability to articulate their needs and experiences. All of these logics speak to a profound tolerance of the inequality and dehumanization of people living with dementia. It is vital to foreground the voices and experiences of people living with dementia in human rights scholarship and advocacy, support and amplify the work of consumer-led organizations such as Dementia Alliance International, and challenge the pathologization and subversion of their acts of resistance into further bases for confinement.
Acknowledgments
We thank members of the project advisory group for their insights, guidance, and support. This paper is part of the “Safe and Just Futures for People Living with Dementia in Residential Aged Care” project funded by the Dementia Australia Research Foundation – Victoria.
Ethics approval
This study was approved by the University of Technology Sydney Human Research Ethics Committee (approval no. ETH18-2508).
Linda Steele, BA, LLB, GDipLegPrac, MPIL, PhD, is Senior Lecturer in the Faculty of Law, University of Technology Sydney, Australia, and Honorary Senior Fellow in the Faculty of Law, Humanities and the Arts, University of Wollongong, Australia.
Ray Carr, BA/BSc, PhD, is a research assistant in the Faculty of Law, University of Technology Sydney, Australia.
Kate Swaffer, BPsych, BA, MSc (Dementia), Grad Dip Grief Counselling, is Honorary Associate Fellow in the Faculty of Science, Medicine and Health, University of Wollongong, Australia.
Lyn Phillipson, BAppSc (Phys), MPH, PhD, is Associate Professor in the School of Health and Society, Faculty of Social Sciences, University of Wollongong, Australia.
Richard Fleming, BTech, Dip Clin Psy (BPS), PhD, is Honorary Professorial Fellow in the Faculty of Science, Medicine and Health, University of Wollongong, Australia.
Please address correspondence to Linda Steele. Email: linda.steele@uts.edu.au.
Competing interests: None declared.
Copyright © 2020 Steele, Carr, Swaffer, Phillipson, and Fleming. This is an open access article distributed under the terms of the Creative Commons Attribution Non-Commercial License (http://creativecommons.org/licenses/by-nc/4.0/), which permits unrestricted non-commercial use, distribution, and reproduction in any medium, provided the original author and source are credited.
References
[1] D. Pūras, Report of the Special Rapporteur on the Right of Everyone to the Enjoyment of the Highest Attainable Standard of Physical and Mental Health, UN Doc. A/HRC/38/36 (2018). See also D. Pūras, Report of the Special Rapporteur on the Right of Everyone to the Enjoyment of the Highest Attainable Standard of Physical and Mental Health, UN Doc. A/HRC/35/21 (2017).
[2] C. Devandas-Aguilar, Report of the Special Rapporteur on the Rights of Persons with Disabilities, UN Doc. A/74/186 (2019).
[3] Ibid., paras. 32–33.
[4] Convention on the Rights of Persons with Disabilities, G.A. Res. 61/106 (2006).
[5] See, for example, Dementia Alliance International, The human rights of people living with dementia: From rhetoric to reality, 2nd edition (DAI, 2016).
[6] S. Cahill, Dementia and human rights (Bristol: British Policy Press, 2018); S. Dreyfus, L. Phillipson, and R. Fleming, “Staff and family attitudes to fences as a means of detaining people with dementia in residential aged care settings: The tension between physical and emotional safety,” Australian Journal of Social Issues 53/2 (2018), pp. 107–122; L. Low, “Why Australia urgently needs post-diagnostic support and treatment for dementia,” Australian Journal of Dementia Care 8/6 (2019), pp. 30–32.
[7] Human Rights Watch, Fading away: How aged care facilities in Australia chemically restrain older people with dementia (New York: Human Rights Watch, 2019); Human Rights Watch, “They want docile”: How nursing homes in the United States overmedicate people with dementia (New York: Human Rights Watch, 2018).
[8] See, for example, Office of the United Nations High Commissioner for Human Rights, UN Human Rights Chief offers her support for a new Convention on the rights of older persons (April 8, 2014). Available at https://www.ohchr.org/EN/NewsEvents/Pages/RightsOfOlderPersons.aspx.
[9] Aged Care Financing Authority, Sixth report on the funding and financing of the aged care sector (July 2018), p. xvii.
[10] Ibid., p. 50.
[11] Royal Commission into Aged Care Quality and Safety, Interim report: Neglect (2019), p. 12. See also Royal Commission into Aged Care Quality and Safety. Available at https://agedcare.royalcommission.gov.au/Pages/default.aspx; Australian Law Reform Commission, Elder abuse—A national legal response (final report) (Sydney: Australian Law Reform Commission, 2017).
[12] J. R. Cadwallader, C. Spivakovsky, L. Steele, and D. Wadiwel, “Institutional violence against people with disability: Recent legal and political developments,” Current Issues in Criminal Justice 29/3 (2018), pp. 261, 267.
[13] See Australian Government Department of Health, Delivering quality aged care standards (2019). Available at https://agedcare.health.gov.au/quality/aged-care-quality-standards.
[15] See, for example, E. M. Bourret, L. G. Bernick, C. A. Cott, and P. C. Kontos, “The meaning of mobility for residents and staff in long-term care facilities,” Journal of Advanced Nursing 37/4 (2002), pp. 338–345; K. Moore and B. Haralambous, “Barriers to reducing the use of restraints in residential elder care facilities,” Journal of Advanced Nursing 58/6 (2007), pp. 532–540; R. Nay and S. Koch, “Overcoming restraint use: Examining barriers in Australian aged care facilities,” Journal of Gerontological Nursing 32/1 (2006), pp. 33–38; C. Øye, F. F. Jacobsen, and T. E. Mekki, “Do organisational constraints explain the use of restraint? A comparative ethnographic study from three nursing homes in Norway,” Journal of Clinical Nursing 26/13–14 (2017), pp. 1906–1916; F. Tufford, R. Lowndes, J. Struthers, and S. Chivers, ‘“Call security’: Locks, risk, privacy and autonomy in long-term residential care,” Ageing International 43/1 (2018), pp. 34–52; M. E. Graham, “The securitisation of dementia: Socialities of securitisation on secure dementia care units,” Ageing and Society (2019), pp. 1–17.
[16] Human Rights Watch (see note 7).
[17] Pūras (2018, see note 1).
[18] Ibid., para. 35.
[19] See, for example, Bourret et al. (see note 15); Moore and Haralambous (see note 15); Nay and Koch (see note 15); Øye et al. (see note 15); Tufford et al. (see note 15); Graham (see note 15).
[20] C. Øye and F. F. Jacobsen, “Informal use of restraint in nursing homes: A threat to human rights or necessary care to preserve residents’ dignity?” Health (2018), pp. 1–16.
[21] Ibid.
[22] J. M. Wigg, “Liberating the wanderers: Using technology to unlock doors for those living with dementia’ Sociology of Health and Illness 32/2 (2010), pp. 288–303; Graham (see note 15).
[23] Graham (see note 15); Tufford et al. (see note 15); Wigg (see note 22).
[24] Tufford et al. (see note 15).
[25] M. W. Skinner, R. V. Herron, R. J. Bar, et al., “Improving social inclusion for people with dementia and carers through sharing dance: A qualitative sequential continuum of care pilot study protocol,” BMJ Open 8/11 (2018).
[26] H. Walker and P. Paliadelis, “Older peoples’ experiences of living in a residential aged care facility in Australia,” Australasian Journal on Ageing 35/3 (2016), pp. E6–E10; G. H. Train, S. A. Nurock, M. Manela, et al., “A qualitative study of the experiences of long-term care for residents with dementia, their relatives and staff,” Aging and Mental Health 9/2 (2005), pp. 119–128.
[27] S. L. Dupuis, B. Smale, and E. Wiersma, “Creating open environments in long-term care settings: An examination of influencing factors,” Therapeutic Recreation Journal, Urbana 39/4 (2005), pp. 277–298.
[28] J. E. Thomas, B. O’Connell, and C. J. Gaskin, “Residents’ perceptions and experiences of social interaction and participation in leisure activities in residential aged care,” Contemporary Nurse 45/2 (2013), pp. 244–254.
[29] N. G. Choi, S. Ransom, and R. J. Wyllie, “Depression in older nursing home residents: The influence of nursing home environmental stressors, coping, and acceptance of group and individual therapy,” Aging and Mental Health 12/5 (2008), pp. 536–547.
[30] L. Steele, K. Swaffer, R. Carr, et al., “Ending confinement and segregation: Barriers to realising human rights in the everyday lives of people living with dementia in residential aged care,” Australian Journal of Human Rights (forthcoming).
[31] See, for example, L. Grenfell, “Aged care, detention and OPCAT,” Australian Journal of Human Rights 25/2 (2019), pp. 248–262.
[32] Ombudsman, Aged care monitoring. Available at http://www.ombudsman.parliament.nz/what-we-can-help/aged-care-monitoring.
[33] Devandas-Aguilar (see note 2).
[34] See, for example, L. Ben-Moshe, C. Chapman, and A. C. Carey (eds), Disability incarcerated: Imprisonment and disability in the United States and Canada (New York: Palgrave Macmillan, 2014); C. Spivakovsky, L. Steele, and P. Weller (eds), The legacies of institutionalisation: Disability, law and policy in the “deinstitutionalised” community (Oxford: Hart, forthcoming).