Human Rights-Based Approaches to Mental Health: A Review of Programs
Sebastian Porsdam Mann, Valerie J. Bradley, and Barbara J. Sahakian
Health and Human Rights 18/1
Published June 2016
Abstract
The incidence of human rights violations in mental health care across nations has been described as a “global emergency” and an “unresolved global crisis.” The relationship between mental health and human rights is complex and bidirectional. Human rights violations can negatively impact mental health. Conversely, respecting human rights can improve mental health. This article reviews cases where an explicitly human rights-based approach was used in mental health care settings. Although the included studies did not exhibit a high level of methodological rigor, the qualitative information obtained was considered useful and informative for future studies. All studies reviewed suggest that human-rights based approaches can lead to clinical improvements at relatively low costs. Human rights-based approaches should be utilized for legal and moral reasons, since human rights are fundamental pillars of justice and civilization. The fact that such approaches can contribute to positive therapeutic outcomes and, potentially, cost savings, is additional reason for their implementation. However, the small sample size and lack of controlled, quantitative measures limit the strength of conclusions drawn from included studies. More objective, high quality research is needed to ascertain the true extent of benefits to service users and providers.
Introduction
The historical and current incidence of human rights violations in mental health care across nations has been variously described as a “global emergency” and an “unresolved global crisis,” evidenced by reports of physical and sexual abuse; discrimination and stigma; arbitrary detention; inability to access health care, vocational and residential resources; and denial of self-determination in financial and marital matters, among other rights deprivations.1 Mental illness affects nearly one in three individuals globally during their lifetime and nearly one in five in the past 12 months.2 Mental and substance abuse disorders were leading causes of disability and were responsible for 8.6 million years lost to premature death worldwide in 2010.3 The burden of these disorders increased by 37.6% from 1990 to 2010.4 The annual economic cost of mental illness globally has been estimated to be $2.5 trillion, with a projected increase to $6 trillion by 2030, more than half of the total costs for all non-communicable diseases.5 The World Health Organization defines mental health as a “state of well-being in which every individual realizes his or her own potential, can cope with the normal stresses of life, can work productively and fruitfully, and is able to make a contribution to her or his community.”6 This definition implies that mental health is reliant on the wide array of supports and resources that facilitate individual engagement at the highest level of gainful employment and in other community roles.7 These factors include, among others, health, the availability of adequate housing, just and favorable conditions for work, and freedom from discrimination, all of which are enshrined in international human rights law.8 There are thus significant connections between mental health and human rights.9
The relationship between mental health and human rights has at least three parts.10 First, human rights violations such as torture and displacement negatively affect mental health.11 Second, mental health practices, programs, and laws, such as coercive treatment practices, can impact human rights.12 Finally, the advancement of human rights benefits mental health synergistically.13 These benefits extend beyond mental health to the close connection between physical and mental health.14 There are thus clinical and economic reasons, as well as moral and legal obligations, to advance human rights in mental health care.
A human rights-based approach (HRBA) to mental health care capitalizes on these rich interconnections. An HRBA “is a conceptual framework…that is normatively based on international human rights standards and operationally directed to promoting and protecting human rights.”15 HRBAs have been successfully implemented in a variety of fields, including international development and HIV treatment.16 In the context of mental health care, an HRBA means placing emphasis not only on avoiding human rights violations but making sure that human rights principles are at the center of a service-providing organization.17
Human rights frameworks are increasingly being recognized as important contributors to health care. Recently, leaders in the fields of neuroscience and global mental health have called for:
a multilayered and multisectoral approach to prevention and treatment… including… provision of living and working conditions that enable healthy psychosocial development, promotion of positive interactions within and between social groups, social protection for the poor, anti-discrimination laws and campaigns, and promotion of the rights of those with mental disorders.18
Similarly, the Grand Challenges in Global Mental Health initiative has noted that:
[e]fforts to build mental capital—the cognitive and emotional resources that influence how well an individual is able to contribute to society and experience a high quality of life—could also mitigate the risk of disorders such as depression, substance-use disorders, bipolar disorder and dementia…. Thus, health-system-wide changes are crucial, together with attention to social exclusion and discrimination.19
However, “all care and treatment interventions—psychosocial or pharmacological, simple or complex—should have an evidence base to provide programme planners, clinicians and policy-makers with effective care packages.”20 HRBAs have the potential to fulfill these demands at relatively low costs. Their potential should be examined in order to provide the evidence called for above.
These frameworks have both normative and legal backing and have substantial overlap with medical ethics. Human rights set out universal, non-negotiable standards for all people, and can thus act as powerful catalysts for change in areas such as mental health care that have historically been marred by discrimination and, in some cases, disregard for the inherent worth and dignity of patients. Though there is little doubt that infringement of human rights has negative effects on mental welfare, few papers have sought to explore the converse part of this reciprocal relationship.
This paper aims to review instances where an explicitly HRBA to mental health care, including intellectual disability and dementia care, has been carried out by service providers. It does not aim to review the impact of rights-based litigation on mental health care.
Method
Literature search
An initial search of PubMed on March 22, 2015, with the search phrases “human rights based approach” and “mental” yielded 274 results, of which only one record met inclusion criteria. It was therefore decided to aggressively expand search criteria in the hopes of locating more records that would meet inclusion criteria.
A systematic search of PubMed (Medline), PsycInfo, PsycArticles, British Library, Library of Congress and Web of Science was carried out on March 22 and 23, 2015. Combinations of the phrases “human rights,” “mental health,” “mental,” “mental illness,” “mental disorder,” “human rights based approach,” “human rights-based approach,” “rights-based approach,” “rights based approach,” “human rights approach,” “intellectual disability,” “intellectual difficulty,” “intellectual difficulties,” “learning disorder,” “learning difficulty,” “learning difficulties,” “learning disability,” and “UNCRPD” constituted the search terms.
The publications and reports of the human rights commissions, health departments (where applicable), and mental health commissions (where applicable) of the United Kingdom, United States of America (Inter-American Commission), New Zealand, Australia, Scotland, Ireland, Canada, South Africa, Ontario, Germany, Denmark, European Union, United Nations, African Union, and Islamic Human Rights Council were hand searched.
The reports and publications of the organizations Amnesty International, Mind UK, National Disability Authority Ireland, BasicNeeds, Federation Global Initiative on Psychiatry, World Federation for Mental Health, Disability Rights International, International Disability Alliance, American Association of Community Psychiatrists, American College of Psychiatrists, National Institute of Mental Health, Samaritan Institute, Centre for Mental Health UK, Rethink Mental Illness, Royal College of Psychiatrists, SANE, United Response, Mental Health Europe, MindFreedom International, Mental Health Foundation UK, and Mental Health America were also hand searched.
In addition, 13 researchers as well as the above-mentioned human rights commissions and organizations were contacted in the hopes of locating additional sources.
The selection of organizations and commissions was based on size and the language competencies of the first author.
The first author performed the literature search and data abstraction.
Inclusion criteria
Studies were selected according to the following criteria:
- there was use of an explicitly HRBA to improve mental health outcomes;
- information was reported on the mental health outcomes or on measures immediately relevant to mental health outcomes;
- the report was in English; and
- the report was published.
Exclusion criteria
Studies were excluded according to the following criteria:
- the report referred to work that was reported more fully elsewhere;
- the report was in a language other than English; or
- the report was not published.
Studies that fulfilled all inclusion criteria and none of the exclusion criteria were included in the analysis. As a consequence, only studies that explicitly identified themselves as HRBA were included.
Results
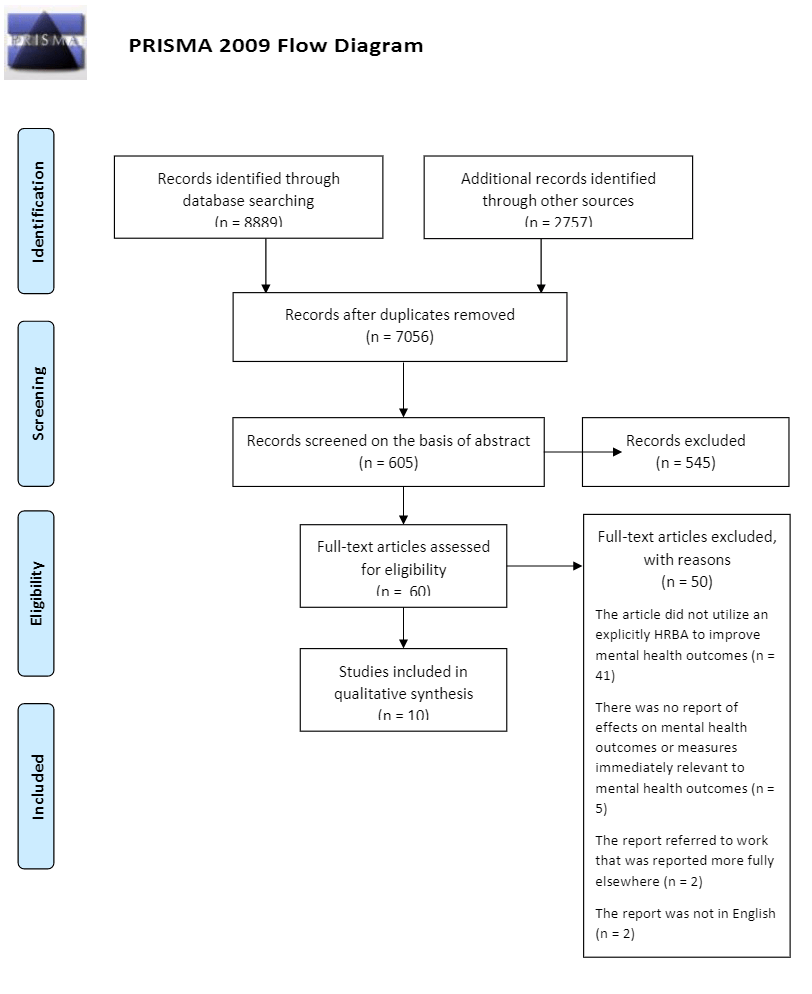
The database searches resulted in 8,889 hits. 2,757 records were identified through other sources, for a total of 11,646 records. 7,056 records remained after duplicates were removed. Of these, 615 were reviewed on the basis of their abstracts, and 60 were reviewed on the basis of the full text. Ten articles met inclusion criteria.
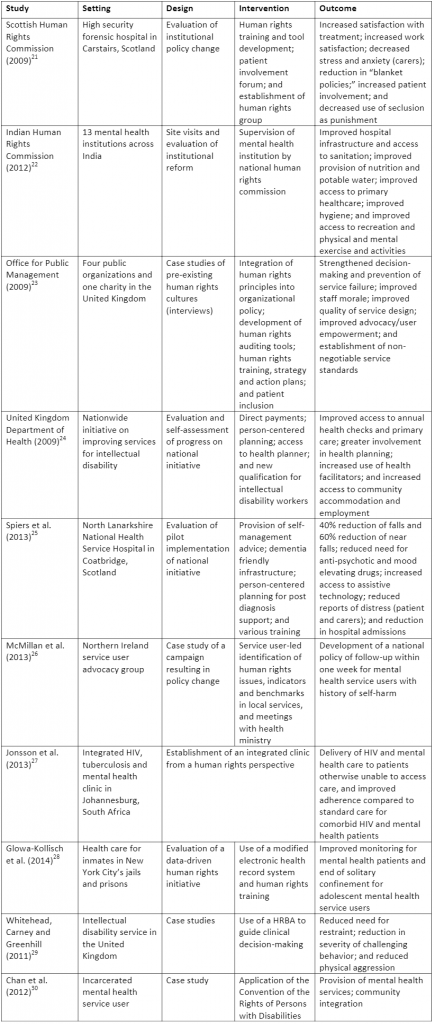
Figure 2. Characteristics of studies included.
Studies that met inclusion criteria ranged from a single case study to nationwide initiatives. Three studies were carried out by national human rights commissions and one by a national health department. Four studies reported on work performed by state hospitals. Of the remaining two studies, one reported a case study of an incarcerated mental health service user and the other reported on work done by a service user advocacy group. Five of the studies were evaluations of national or organizational policy initiatives and the remaining five reported case studies. The studies span across six countries. All 10 included studies reported positive outcomes.
The State Hospital, Carstairs, Scotland
The Scottish Human Rights Commission undertook an independent evaluation of an HRBA at The State Hospital (TSH) in Carstairs, Scotland.31 TSH is a high-security forensic hospital for compulsorily detained mental health patients. Following a critical report by the Mental Welfare Commission in 2000, the hospital decided to adopt an HRBA into its culture. A human rights working group was established and underwent extensive training under the purview of a human rights expert. In conjunction with the expert, the group interviewed approximately 100 staff and patients to identify human rights concerns. The working group proceeded to examine all hospital policies using a three-tiered “traffic light” assessment tool. Although no policies were given a “red light” (indicating that a policy was not compliant with human rights standards), several policies, such as those concerning the use of restraint and seclusion, were given an “amber light” rating. Amber light ratings were used to identify policies in need of development and consideration.
In addition, human rights training was provided for staff not involved in the working group and a patient and staff forum for involvement in the decision-making process was established. The human rights training was provided in the form of a series of workshops over two years, examining the reasons behind the implementation of the HRBA and using case studies to educate staff. Roughly 200 staff took part in these efforts. A “best practice guide” was developed to help staff make appropriate decisions in cases where human rights might be infringed. The guide included an index of hospital practices and policies where human rights problems might occur, with instructions on how to avoid breaches.
The Scottish Human Rights Commission’s evaluation included the review of internal documents as well as focus groups and interviews with management, staff, and patients. The Commission found that “the majority [of patients, caregivers, management, and external commentators] whole heartedly agree that a positive rights respecting culture, where the rights of staff, patients and carers are respected, was created at TSH as a result of the human rights-based approach.” The Commission found improvements in the care and treatment conditions of patients as well as a reduction in the use and severity of restraint. Staff reported improved working conditions and a reduction in anxiety. Both patients and caregivers reported a shift from blanket policies to more individualized, patient-centered approaches. These changes combined to effect improved working relations between caregivers and patients. Negative comments were limited to concerns about communications and involvement in discussions on working practices related to hospital rebuilding works among staff and patient concerns regarding proposed restrictions on diet choices and smoking.
Indian National Human Rights Commission
In a 1997 Indian Supreme Court decision, the National Human Rights Commission was given the mandate to monitor and supervise performance at the mental health institutions at Agra, Gwalior, and Ranchi “to ensure that [they function] in the manner as is expected for achieving the object for which [they were] set up.”32 Since then, this mandate has extended to all similar institutions in India. The Commission’s first steps were to analyze the existing status and shortcomings of 37 mental health institutions. The Commission then published a list of recommendations including abolition of cell admissions; restructuring of closed into open wards; construction of smaller capacity wards; ensuring adequate supply of potable water and access to sanitation; provision of nutritious food at 3,000 calories per day; ensuring compatibility of policies with the Mental Health Act (1987); provision of individual cots and mattresses; in-house training of staff; and occupational therapy for patients. A later set of recommendations included expanding patient access to public goods such as late-age pensions. In addition, the Commission established an advisory group with representatives from the Department of Health, the national legislature, and the Ministries for Social Justice and Women and Child Development; expanded data reporting requirements; engaged with the Indian Medical Council and Department of Health to expand mental health training and recruitment; and carried out regular site visits to monitor compliance.
A report of site visits at 13 institutions was prepared by the Commission’s Special Rapporteur, L. D. Mishra, in 2012.33 The rapporteur found improvements in hospital infrastructure, including the construction and improvement of outpatient departments and delivery of potable water, as well as improved use of technology, including electronic data collection. The inspections found improvements in integration of primary care and provision of nutritious food. In addition, patients were now able to access improved dining and recreational facilities and had better access to sanitation. Hygiene standards were improved, and some patients were offered occupational therapy as well as yoga and meditation opportunities. However, the report also highlighted the continuing dearth of mental health resources in the country, with an estimated shortfall of roughly 8,500 psychiatrists, 16,750 clinical psychologists and 22,600 psychiatric social workers. The report also noted the chronic lack of psychiatric beds as well as the dilapidated and archaic facilities, overcrowding of institutions, lack of modern tools, and persistence of practices such as unnecessary restraint and inadequate investigative facilities.
Mersey Care National Health Service Trust, England
The United Kingdom’s Equality and Human Rights Commission published a report on five organizations that had incorporated an HRBA into their culture.34 The five organizations were the Welsh Assembly Government, the National Policing Improvement Agency, Southwark Council, Mersey Care Trust, and Age Concern. Mersey Care Trust is of primary interest as it provides the full range of specialist mental health services as well as medium- and high-security forensic mental health services. Mersey Care adopted an HRBA to its service delivery in 2001. One of the first steps taken was the appointment of a director for user and caregiver involvement to the Trust board. Another was implementing performance monitoring of senior staff by caregivers and patients as well as caregiver and patient involvement in the recruitment and induction of new staff. In addition, each document passed to the board is required to feature a cover sheet identifying relevant human rights concerns. The trust worked with the British Institute of Human Rights to deliver human rights training to staff and caregivers as well as the board. The Institute’s training was tailored to the needs of the Trust and focused on the basic concepts involved. The training included case studies and highlighted the human rights issues most relevant for each group of participants. This resulted in the development of human rights benchmarks, assessment tools, and questionnaires for patients.
Eighty-nine percent of patients felt that involvement stemming from the HRBA had resulted in increased recovery and well-being. Patients reported increased access to skills training and vocational opportunities. In addition, the report found that newly hired staff were more likely to be empathetic and understanding due to patient and caregiver involvement in new hire screenings. Staff and management also reported positive effects on their work. The Trust reported that these benefits were achieved with an annual investment of less than £400,000.
United Kingdom Department of Health: Valuing People Now
In 2009, the United Kingdom’s Department of Health launched a nationwide initiative designed to improve care and services for people with intellectual disability. The initiative, Valuing People Now, was based on four key principles of rights, independence, choice, and inclusion.35 The initiative consisted of several recommendations and the establishment of funds for their implementation. The key priorities of the initiative were the modernization of day care facilities; provision of support for the transition to supported community accommodation; establishment of supported living arrangements for service users with older caregivers; development of local specialized services; provision of direct payments; and increased use of person-centered planning approaches.
The Department commissioned a self-evaluation of the project 18 months after roll-out.36 The report was based on progress reports from all 152 local institutions involved in the project. The report found that as a result of the initiative, more acute liaison nurses had been recruited and more annual health checks were being performed, though half of service users still failed to receive annual checks. The report also found increased access to employment opportunities and community accommodation. Institutions reported higher levels of service user involvement in health planning and greater access to person-centered planning approaches and health facilitators.
However, an independent review of Valuing People Now identified several areas of concern.37 The review found that although Valuing People Now had enhanced some areas of choice, participation, and quality of life for people with intellectual disabilities, it had only affected a minority of service users and may have disproportionately excluded people with the most severe disabilities. In addition, the review found little evidence that Valuing People Now had increased choice of public services for service users.
The Scottish Government’s National Dementia Strategy
The Scottish Government launched its first human-rights based nationwide dementia strategy in 2010.38 Three sites were chosen as demonstration sites. The North Lanarkshire site has published a report detailing the steps taken to ensure compliance with the human rights and outcome goals of the project.39 As part of this initiative, and in recognition of the terminal nature of dementia, the North Lanarkshire site placed a particular emphasis on reshaping institutional infrastructure and the local environment to become more dementia-friendly. A community outreach program was established, informing local business owners and community service providers of steps they could take to make their services more amenable to dementia patients. Several training programs for the demonstration site staff were conducted, including dementia awareness; post-diagnosis training; the use of assistive technology; best practice workshops; dealing with stress and distress; and palliative care. The training courses focused on improving awareness and understanding of the condition and the effects it can have on patients’ understanding of the world they live in. A post-diagnosis support program was developed and provision of day services was increased. Lastly, peer to peer support was encouraged through the establishment of “dementia cafes” for service users and caregivers.
The evaluation reported several beneficial outcomes. These included a 40% reduction in falls and a 60% reduction in near-falls resulting from dementia-friendly restructuring. The need for anti-psychotic and mood elevating pharmacotherapy was reduced and access to assistive technology was improved. In addition, fewer hospital admissions were reported. Both staff and patients reported lower levels of distress as a result of the program. Service providers received higher grades on their Care Inspectorate reports. Communication between caregivers and staff improved, resulting in greater treatment and work satisfaction.
The Public Initiative for the Prevention of Suicide—Greater Shankill Bereaved Families Rights Group
The Participation and Practice of Rights Project (PPR) is a service-user-led advocacy group based in Northern Ireland. As a result of political turmoil, Northern Ireland is facing much higher rates of mental health issues and suicide attempts than previously.40 In conjunction with another local organization, the Public Initiative for the Prevention of Suicide-Greater Shankill Bereaved Families (PIPS-GSBF) Rights Group, a human rights-based project with the aim of instituting a mandatory one-week follow-up system for patients with severe mental illness and a history of self-harm was conceived. The impetus behind this project was the fact that the majority of suicides happen within one week of discharge from services, yet only a minority of patients are assigned a follow-up appointment within one week.41 The group’s first steps were service-user-led research and identification and development of human rights issues, indicators, and benchmarks.
The group identified areas of local service provision which they considered problematic and compared them to international human rights standards. They then conducted focus group sessions and surveys of local service users to assess the extent to which these issues were pervasive in nearby communities. Next, the group presented their findings to an international panel of human rights and mental health experts. With the encouragement and support of the panel, the group conducted further research and an extensive campaign resulting in a meeting with the Minister of Health. As a consequence of the group’s campaign and meetings, the Minister of Health agreed to implement a nationwide policy of mandatory follow-up appointments within one week for service users with a history of self-harm.
Luthando HIV Clinic, Soweto, South Africa
In Soweto, South Africa, an HRBA was used to set up an integrated mental health, tuberculosis and HIV treatment clinic.42 Nearly two-thirds of all cases of HIV are located in southern Africa. An estimated 26.5% of all mental health service users in South Africa are thought to have co-morbid HIV.43 Though it is not an official policy, it is very difficult for mental health service users to access HIV or tuberculosis treatment due to limited resources and a widespread belief that they will not adhere to treatment. Using an HRBA, three local psychiatrists successfully argued that this constituted discrimination and were granted a small amount of resources to set up an integrated mental health and HIV clinic with tuberculosis care added subsequently. As a result of this program, integrated service has been provided to more than 600 individuals who would otherwise have faced severe obstacles to accessing care. In addition, the program delivers vocational and skills training.
New York City’s Bureau of Correctional Health Services
New York City’s Department of Health and Mental Hygiene’s Bureau of Correctional Health Services is responsible for the health care of jail and prison inmates. This setting can engender conflict between the medical and security missions, a situation known as “dual loyalty.” As a consequence of this, the Bureau adopted a health care policy in 2012 based on the three aims of patient safety, population health, and human rights.44 As part of the human rights element, a human rights forum and subcommittee were established and mandatory human rights and dual loyalty training for staff was implemented. This training focused on introducing and clarifying the basic concepts behind human rights. Case studies and examples of dual loyalty situations in correctional health were used in the training, which is mandatory for all health staff. In addition, the electronic health record system in use was modified with the aim of improving the monitoring and care of vulnerable inmates’ health.45 These modifications allowed the Bureau to track and analyze incidents of harm and self-harm among inmates who were also mental health service users. The analysis revealed that mental health problems and solitary confinement were very significant risk factors for self-harm.46 Due to concerns arising from the human rights viewpoint, these data were used to end solitary confinement practices for adolescents with serious mental illness.47
Individual patient case studies
The final two studies presented case studies of individual patients. Chan et al. applied the framework of the Convention on the Rights of Persons with Disabilities to the case of “Ned,” a man with co-morbid intellectual disability and mental health issues detained for most of his life in a high-security prison setting where he received little treatment beyond antipsychotic medication.48 Ned was being detained in prison despite having no records of violence, excepting verbal threats which were not followed through, during his roughly 40 years of detention. As a result, a number of Ned’s rights under the Convention were breached. Using an HRBA, a transfer to a community treatment setting was planned and executed over an extended period.
Whitehead, Carney, and Greenhill presented several case studies of an HRBA to positive risk assessment and support of people with a learning disability.49 The HRBA emphasized the use of proactive (preventive) instead of reactive strategies; the importance of using the least restrictive strategy; finding an appropriate balance between rights and risks; and service user involvement in health planning and advance directives. In addition, human rights risk screening and joint risk and human rights management tools were created. The team describes seven cases where complex treatment solutions have been reached as a result of the HRBA. The authors conclude that their approach “respects human rights, creates opportunities for growth and meaningful community participation, and empowers people with a learning disability and complex needs to access ‘a life like any other.’”50
Discussion
All 10 included studies reported beneficial effects of adopting an HRBA. Benefits ranged from subjective reports of a better work environment to the provision of previously unavailable services. The reports were consistently positive across the spectrum of studies included, from single-person case studies to national initiatives. Negative reports were much less frequent and generally concerned issues related to communication or inclusion.
The methodology used to assess impacts of the HRBAs was in many cases limited to interviews with patients, caregivers, and/or staff. Only three studies reported quantitative data related to the impact of their approaches on patients’ access to treatment, well-being, or mental health outcomes. Roughly half of the studies involved self-assessment rather than external evaluation. In addition, two external evaluations were carried out by national human rights bodies that may have had an interest in positive evaluations of HRBAs. None of the studies used experimental design and few used structured interview techniques for their evaluations. There is thus significant risk of bias.
The potential for bias can be seen in the contrast between the self-evaluation of the UK Department of Health’s Valuing People Now initiative and the independent review of the same project.51 Whereas the self-evaluation correctly identified several areas of improvements, it failed to mention that these were often limited and did not reach all of the intended recipients, as highlighted in the independent review. Nonetheless, it was clear that all projects were considered to have yielded significant benefits.
The cost of implementation was mentioned in one study only.52 Mersey Care Trust reported having spent roughly £400,000 on their HRBA, less than a quarter of 1% of their annual resources. Due to the nature of the interventions most frequently used, such as workshops, training, service user inclusion, and policy development, costs are likely to be modest compared to potential system-wide benefits. Administrators at Mersey Care argued that they had spent “less than a quarter of 1 per cent of their income to ensure they spend the other 99.75 per cent more effectively.”53
All studies were completed in 2009 to 2014. This may reflect the increased awareness of human rights issues in disability and mental health care due to the lead up to and ratification of the United Nations Convention on the Rights of Persons with Disabilities (CRPD), which came into effect in 2009.54 The CRPD places significant emphasis on the equality of persons with disability before the law and with respect to all other rights.55 One of the strengths of HRBAs is their grounding in international and some domestic law. This gives such approaches ethical and legal weight, with recourse to legal mechanisms should this be necessary.
Our survey is important in that it constitutes an early step towards the realization that human rights principles, beyond being ethically and legally obligatory, can also lead to beneficial outcomes in mental health. Furthermore, the experience of Mersey Care Trust indicates that HRBAs can be implemented at low cost and are likely to be cost-effective. We hope that calling attention to these features will galvanize stakeholders to pay more attention to human rights and their connection with mental health. Training mental health staff, advocacy groups, and other stakeholders in human rights has the potential to benefit all involved at little cost. This aspect of human rights has received little attention thus far, and may help as a practical incentive towards improved programs for vulnerable members of society with mental health problems.
The studies reviewed here can be seen as an indication that an HRBA can be successfully and beneficially applied in mental health contexts. However, the methodological shortcomings of the studies reviewed strongly suggest that more research is needed to confirm these benefits and to explore which types or features of HRBAs are most suitable. There were other limitations to our review. The literature and data extraction was performed by one author only. Only published studies in English utilizing an explicitly HRBA were included, and the grey literature was not searched. Consequently, our focus is restricted to an HRBA to mental health and does not cover other vulnerable populations, such as refugees, who are not represented in the included studies. The quantity of relevant articles and the extent of methodological rigor of the included studies limit the scope and strength of our analysis.
Objective, quantitative studies with appropriate control groups will be necessary in order to place HRBAs on a firm evidence base. Future studies ought to include clearly defined outcome measures such as effects on quality of life, use of medications, and use of mental health services. In addition, more cost-benefit analyses are required. Evidence of costs and benefits derived from well-conducted, controlled quantitative studies could be used to promote the wider introduction of HRBAs in mental health.
Conclusion
This paper aimed to review instances where explicit HRBAs were used to promote the mental well-being of service users. Although few such studies have been conducted or were available for analysis, and the quality of experimental design and data collection were generally not of a high standard, all noted widespread benefits of adopting human rights standards into service delivery. This was the case across both scale and nature of services, from single-case studies to nationwide initiatives, and from severe and persistent mental illness to dementia and intellectual disability services.
HRBAs ought to be in place for moral reasons, since human rights are fundamental pillars of justice and civilization.56 The fact that such approaches contribute to positive therapeutic outcomes and, potentially, cost savings, is an additional reason for their implementation. The HRBA thus offers a moral, political, legal, and empirical rationale for inclusion in mental health systems—at the national, state, and provider levels. Although more well-designed research is required to validate the extent of benefits to service users and providers, the information already available provides a strong argument for the adoption of HRBAs.
Acknowledgments
Barbara J. Sahakian receives funding from the Human Brain Project. She is President of the International Neuroethics Society and a Distinguished Research fellow at the University of Oxford Uehiro Centre for Practical Ethics. Sebastian Porsdam Mann wishes to acknowledge the International Neuroethics Society and the Carnegie Council for Ethics in International Affairs, where he is a Global Ethics Fellow for the Future.
Please address correspondence to the authors c/o Sebastian Porsdam Mann, Department of Psychiatry, Addenbrooke’s Hospital, University of Cambridge, Cambridge, UK CB2 0QQ. Email: sp564@cam.ac.uk.
Sebastian Porsdam Mann is a PhD student in the Department of Psychiatry, University of Cambridge, UK.
Valerie J. Bradley, MA, FAIDD, is President of the Human Services Research Institute, Cambridge, MA, USA.
Barbara J. Sahakian, PhD, DClinPsy, DSc, FMedSci, is Professor of Clinical Neuropsychology at the Department of Psychiatry and Medical Research Council/Wellcome Trust Behavioral and Clinical Neuroscience Institute, University of Cambridge, UK.
References
- World Health Organization, Mental Health, Human Rights & Legislation. Available at http://www.who.int/mental_health/policy/legislation/en/; N. Drew et al. ”Human rights violations of people with mental and psychosocial disabilities: An unresolved global crisis.” The Lancet 378 (2011), pp. 1664–1675.
2. Z. Steel et al. “The global prevalence of common mental disorders: a systematic review and meta-analysis 1980-2013.” International Journal of Epidemiology 43(2) (2014), pp. 476-493.
3. H. A. Whiteford et al. “Global burden of disease attributable to mental and substance use disorders: findings from the Global Burden of Disease Study 2010.” The Lancet 382(9904) (2013), pp. 1575-1586.
4. Ibid.
5. Bloom et al. The global economic burden of noncommunicable diseases (Geneva: World Economic Forum, 2011).
6. World Health Organization, Mental health: a state of well-being. (August 2014). Available at: http://http://www.who.int/features/factfiles/mental_health/en/
7. C. Watters, “Mental health and illness as human rights issues,” in M. Dudley, D. Silove, and F. Gale (eds), Mental health and human rights: Vision, praxis and courage (Oxford: Oxford University Press, 2012), pp. 69-79.
8. Universal Declaration of Human Rights (UDHR), G.A. Res. 217A (III) (1948), Art. 7, 23 and 25. Available at http://www.un.org/Overview/rights.html; International Covenant on Economic, Social and Cultural Rights (ICESCR), G.A. Res. 2200A (XXI), Art. 2, 6, 11 and 12. (1966). Available at http://www2.ohchr.org/english/law/cescr.htm
9. S. Rees and D. Silove, “Human rights in the real world: Exploring best practice research in a mental health context,” in M. Dudley, D. Silove and F. Gale (eds), Mental health and human rights: Vision, praxis and courage (Oxford: Oxford University Press, 2012), pp. 599-610.
10. J. M. Mann, “Introduction,” in J. M. Mann et al. (eds), Health and Human Rights, (New York: Routledge 1999) pp. 3-7.
11. Z. Steel et al. “Association of torture and other potentially traumatic events with mental health outcomes among populations exposed to mass conflict and displacement: A systematic review and meta-analysis.” JAMA 302(5) (2009) pp. 537-549.
12. L. O. Gostin and L. Gable, “The human rights of persons with mental disabilities: A global perspective on the application of human rights principles to mental health.” Maryland Law Review 63(20) (2009) pp. 20-121.
13. Ibid.; Mann (1999, see note 5.)
14. M. Prince et al. “No health without mental health.” The Lancet 370 (9590) (2007), pp. 859-877.
15. Office of the United Nations High Commissioner for Human Rights, Frequently asked questions on a human rights-based approach to development cooperation, (Geneva: OHCHR, 2006) pp. 15.
16. V. Gauri and S. Gloppen, Human rights based Approaches to development: Concepts, evidence and policy (Washington D. C.: World Bank, 2012); V. Paiva et al. ”Religious communities and HIV prevention: An intervention study using a human rights-based approach.” Global Public Health 5(3) (2010), pp. 280-294.
17. M. J. Curtice and T. Exworthy, “FREDA: A human rights-based approach to healthcare.” The Psychiatrist 34 (2010) pp. 150-156.
18. D. J. Stein et al. “Global mental health and neuroscience: potential synergies.” The Lancet Psychiatry 2(2) (2015), pp. 178-185.
19. P. Y. Collins et al. “Grand challenges in global mental health.” Nature 475(7354) (2011), pp. 27-30.
20. Ibid.
21. Scottish Human Rights Commission, Human rights in a healthcare setting: Making it work for everyone: An evaluation of a human rights-based approach at The State Hospital (Glasgow: Scottish Human Rights Commission 2009) pp. 5-6.
22. Indian Human Rights Commission, Care and treatment in mental health institutions: Some recent glimpses (New Delhi: Indian Human Rights Commission, 2012) pp. 7 & 146.
23. Office for Public Management, The impact of a human rights culture on public sector organizations: Lessons from practice (Manchester: Equality and Human Rights Commission, 2009) pp. 5-99.
24. United Kingdom Department of Health, Valuing people now: Summary report March 2009 – September 2010 (London: Department of Health, 2010), pp. 1-65.
25. K. Spiers et al., North Lanarkshire dementia demonstrator site evaluation report (North Lanarkshire: National Health Service North Lanarkshire, 2013), pp. 1-44.
26. F. V. McMillan et al. ”A card before you leave: participation and mental health in Northern Ireland.” Health and Human Rights 11(1) (2009), pp. 61-72.
27. G. Jonsson et al. “Human rights, mental illness and HIV: The Luthando neuropsychiatric HIV clinic in Soweto, South Africa.” Health and Human Rights 13(2) (2011), pp. 64-72.
28. S. Glowa-Kollisch et al. ”Data-driven human rights: Using the electronic health record to promote human rights in jail.” Health and Human Rights 16(1) (2014), pp. 157-165.
29. R. Whitehead, G. Carney and B. Greenhill, “Encouraging positive risk management: Supporting decisions by people with learning disabilities using a human rights-based approach.” In R. Whittington and C. Logan (eds), Self-harm and violence: Towards best practice in managing risk in mental health services, (Chichester: Wiley Publishing, 2011), pp. 215-236.
30. J. Chan et al. “Applying the CRPD to safeguard the rights of people with a disability in contact with the criminal justice system.” Psychiatry, Psychology and Law 19(4) (2012), pp. 558-565.
31. Scottish Human Rights Commission (2009, see note 21.)
32. Indian National Human Rights Commission (2012, see note 22.)
33. Ibid.
34. Office for Public Management (2009, see note 23.)
35. United Kingdom Department of Health, Valuing people: A new strategy for learning disability for the 21st century, (London: Department of Health, 2001), pp. 1-142.
36. United Kingdom Department of Health (2010, see note 24.)
37. S. Cumella, “New public management and public services for people with an intellectual disability: A review of the implementation of Valuing people in England. Journal of Policy and Practice in Intellectual Disabilities 5(3) (2008) pp. 178-186.
38. Scottish Government, Scotland’s national dementia strategy (Edinburgh: Scottish Government, 2010), pp. 1-62.
39. Spiers et al. (2010, see note 25.)
40. McMillan et al. (2009, see note 26.)
41. Ibid.
42. Jonsson (2011, see note 27)
43. Ibid.
44. R. Macdonald, A. Parsons, and H. Venters, “The triple aims of correctional health: Patient safety, population health, and human rights,” Journal of Health Care for the Poor and Underserved 24/3 (2013), pp. 1226-1234
45. Glowa-Kollisch et al. (2014, see note 28.)
46. F. Kaba et al. “Solitary confinement and risk of self-harm among jail inmates.” American Journal of Public Health 104(3) (2014), pp. 442-447.
47. H. Venters, personal communication 4/28/2015.
48. Chan et al. (2012, see note 30.)
49. Whitehead, Carney and Greenhill (2011, see note 29.)
50. Ibid.
51. United Kingdom Department of Health (2010, see note 24.); Cumella (2008, see note 37.)
52. Office for Public Management (2009, see note 23.)
53. Ibid.
54. Convention on the Rights of Persons with Disabilities, G.A. Res, 61/106 (2006). Available at http://www2.ohchr.org/english/bodies/ratification/15.htm.
55. Chan et al. (2012, see note 30.)
56. Universal Declaration of Human Rights (1948, see note 8.)
Copyright © 2016 Porsdam Mann, Bradley, and Sahakian. This is an open access article distributed under the terms of the Creative Commons Attribution Non-Commercial License (http://creativecommons.org/licenses/by-nc/3.0/), which permits unrestricted non-commercial use, distribution, and reproduction in any medium, provided the original author and source are credited.