Effective access to justice against state and non-state actors in the Framework Convention on Global Health: A proposal
Martín Hevia, Carlos Herrera Vacaflor
Health and Human Rights 15/1
Published June 2013
Abstract
A Framework Convention on Global Health (FCGH) seeks to have a profound, effective, and broad impact: bringing access to health rights to the largest global community possible. One of the main issues the FCGH will address is how to make the right to health justiciable. An FCGH must articulate functional remedies for violations of the right to health by state or non-state actors. This paper analyzes one approach to ensuring the recognition of the rights defended in a future FCGH. Following the incremental development approach inspired by the architecture of other successful framework convention protocols, we propose the inclusion of access to health justice guidelines in an FCGH. This proposal is based on the amparo remedy, a figure already extant in the legislation of several Latin American countries; since its incorporation, these countries have witnessed a significant increase in litigation defending health rights. This is only one of many important advantages to broadly adopting guidelines based on the amparo remedy. The proposed guidelines would serve as a basic agreement on broad principles on access to health justice.
Introduction
A Framework Convention on Global Health (FCGH) seeks to have a profound, effective, and broad impact: bringing access to health rights to the largest global community possible.1 An FCGH would be a global health governance scheme aimed at constructing global pillars of progress on the right to health, and to dramatically reducing health inequities.2 It would establish a post-Millennium Development Goals global health agenda rooted in right to health principles such as equality, accountability, and empowerment. An FCGH would also make right to health responsibilities clearer by setting concrete objectives for establishing progressive realization obligations and maximum available resource obligations.3
One of the main issues the FCGH will address is how to make the right to health justiciable. Although litigation is not the only way to promote the right to health, as cases from South Africa, India, and Latin America show, it has been a useful tool for advancing the health of the population.4 Most Latin American and some European countries already recognize the right to health as a fundamental constitutional right, and thereby justiciable in their national courts.5 Many countries whose constitutions may or may not explicitly include specific provisions on health may be parties to a self-executing international convention that recognizes the right to health.6 Even so, the positive legal recognition of the right to health does not guarantee its enforceability: people may not have access to effective and expeditious judicial remedies for enforcing this right. Moreover, although we know that the actions of non-state actors such as local or transnational corporations can have a significant impact on the health of a population, it is frequently the case that states are the only actionable parties. Moreover, several studies suggest that the cumulative effect of individual lawsuits—even successful ones—may have unintended effects on health equity, and that there are risks involved in the fact that relatively wealthy claimants are better able to litigate right to health claims.7
In order to remedy such pathological results in health rights litigation, an FCGH must articulate functional remedies for violations of the right to health by state or non-state actors. This paper analyzes one approach to ensuring the recognition of the rights defended in a future FCGH. Following the incremental development approach inspired by the architecture of other successful framework convention protocols, we propose the inclusion of access to health justice guidelines in an FCGH.8 This proposal is based on the amparo remedy, a figure already extant in the legislation of several Latin American countries. There are many advantages to broadly incorporated guidelines based on the amparo remedy, and Latin American countries that have incorporated it into law have already seen a great increase in the amount of litigation in defense of health rights. The proposed guidelines would serve as a basic agreement on broad principles on access to health justice. Then, at later stages, specific protocols would be developed for each of the basic principles originally set forth, including substantive and procedural legal norms and processes.9 Doing so would advance realistic access to justice for victims of health rights abuses, a clear priority for the FCGH, and begin to ensure that those responsible for the abuses answer for their actions, essential steps in framing global health rights within a contemporary paradigm designed to meet the challenges of the new millennium.
The right to health and effective access to justice guidelines: A sketch
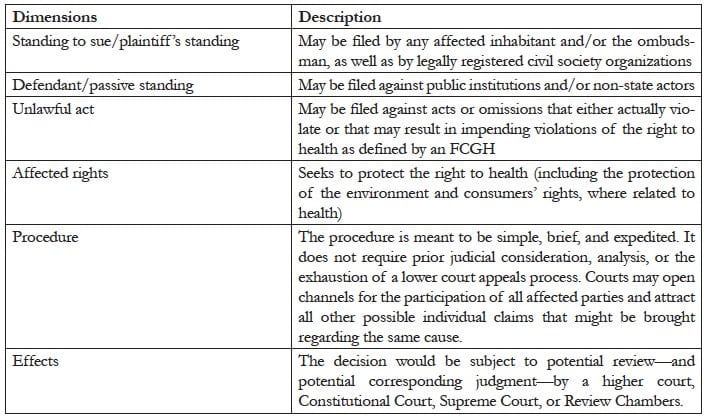
Our proposed guidelines are based on the writ of amparo, a brief and summary judicial action. Unlike the familiar habeas corpus, which protects physical liberty, amparo actions seek judicial protection as a shield for fundamental constitutional rights and liberties. Many jurisdictions already contemplate the amparo or equivalent remedies in their legal systems, but our proposal would have distinctive features. The following table outlines the different dimensions of the proposed guidelines.
Table 1: Guidelines for individual [collective] judicial procedure
While each feature of the guidelines deserves special attention, the issues of standing are the most salient. With regard to standing to sue, we propose that both individual and collective claims be admissible. As we will explain in the next section, the possibility of filing collective claims addresses the objection that under the current law of many jurisdictions, the least advantaged individuals lack effective access to justice. Our guidelines propose mechanisms for seeking the protection of the right to health of the least advantaged; institutional figures like the ombudsman or public defender are viable options through which the least advantaged may voice their claims. Regarding the defendant’s standing, we take into account that in jurisdictions such as Mexico, Germany, and many other potential signatories to an FCGH, the version of amparo—or legal equivalent— currently in force can only be filed against the state or state representatives.10 In light of that, we propose to expand passive standing so that actions may also be filed against non-state actors, such as transnational corporations, for actions or omissions that constitute actual or impending violations of the right to health.
Standing to sue and defendant’s standing in right to health litigation
In this section, we address the reason why FCGH guidelines on effective access to justice should include a collective remedy. We also consider why this would be a useful legal mechanism for advancing the right to health and health equity, and the ground that would be gained by allowing for claims against state and non-state actors.
First, violations of the right to health that appear to affect only particular individuals may expand into collective conflicts. Violations of an individual right do not only result in individual conflict. Multiple violations to individual rights could easily add up to a collective conflict, despite the fact that technically, various similar violations of the same right have occurred. Even though this right should be characterized as individual, as it is when considered from the standpoint of the judicial system, the resulting conflict is collective.11
Second, multiple violations of the right to health of several persons usually require that the judiciary resolve issues that deeply impact the social, economic, or political spheres of the state. For instance, successful health litigation may improve access to health services to particular litigants or groups, but that may not translate to improved access to health services for the general population.12 Such situations demand that the judiciary listen to all affected parties to ensure that wholly informed decisions are reached, for example, by ordering public hearings that enable robust debate with the parties. If reduced to the interest of a single claimant, a future decision that has strong repercussions may lack broader legitimacy because it fails to consider all affected parties.
Third, as previously mentioned, an FCGH that fosters guidelines contemplating collective claims can help overcome the negative impact that right to health litigation has on the least advantaged victims. Indeed, experience in some countries has shown that the individual amparo—that is an individual action—as a legal mechanism for enforcing the right to health led to inequality for those that lack the necessary resources to access justice. Such evidence can be explained by the failure to draft robust regulation that permits the proposed proceeding for collective amparo and simultaneously institute mechanisms that increase access to justice for the least advantaged. In light of this, we argue for the inclusion of “institutional voices” like the Ombuds Office (civil society organizations or health actions groups may also be appropriate and successful for this end). In Colombia, for example, the Ombuds Office can file an amparo on behalf of “any person who requests it or that is under distress and helplessness.”13 Where right to health conflict is collective, the Ombuds Office may attract all individual claims, including those of the least advantaged, thereby transforming an unheard individual voice into an institutional one. Such regulation in practice would mean that the often disempowered lone voice (whose power and resources for litigation are limited compared to those of the defendant) is removed from the particular circumstances of an individual claimant and becomes representative of a broader social claim. Furthermore, because of its status as mouthpiece for the people, the Ombuds Office as a plaintiff in a collective conflict has a special and profound impact in suing a non-state actor compared with the impact an individual plaintiff has on a non-state actor and the judiciary. This has occurred with great success in Bolivia and Venezuela, where, seeking justice, the Ombuds Office was able to guarantee medical treatment specifically and access to the right to health in general.14
Fourth, we propose that the FCGH guidelines include the possibility of filing simple, brief, and expedited claims against non-state actors. This may involve a change of paradigm in right to health responsibilities. In most jurisdictions, the state is nominally and legally the principal potential protector or violator of norms and human rights duties. This traditional configuration known as the “vertical account” of human rights norms is one in which the hierarchy between the state and the individual reflects an assumption of responsibility.15 Nevertheless, this paradigm no longer accurately describes current distributions of rights and obligations in the modern globalized world. In a contemporary context in which private actors are potentially as powerful as states in the context of human rights violations, the “vertical account of human rights” must be reconsidered. Contemplating private actors as human rights guardians and violators—with responsibilities on parity with those traditionally held by the state—is known as the “horizontal effect” of human rights norms.16 Here, the status of the private party in relation to the state is not taken into account, and the state’s involvement, or lack thereof, has no bearing on the question of liability. Those who attempt to obscure the responsibility of private actors could concede that business and non-state actors do incur right-to-health related duties (they have “responsibilities regarding the realization of the right to health”); objectors may also recognize that business and non-state actors have been found complicit in human rights violations in the scope of tort law. However, they may object that at present the international human rights system does not recognize non-state actors as subjects of international responsibility for human rights violations.17 According to this position, the framework convention would be “illegitimately” expanding the scope of current human rights if it were to add this recognition. However, immunity from international courts does not necessarily imply absolute impunity; local legislation may establish liability or sanctions to non-state actors for human rights violations; some jurisdictions even penalize national corporations for human rights violations outside their home countries.18 In other words, an FCGH could potentially extend current the right to health-related duties of non-state actors, such as those recognized by the “Ruggie Principles,” and transform them into binding obligations. This would advance a horizontal account of human rights by adopting a different strategy, such as including guidelines for signatory states to further enact effective legal remedies through which individuals can enforce their right to health.19
Finally, our proposed guidelines would also impact cost-effective judicial workload. Choosing which particular case to review among similar individual claims that stem from a homogenous conflict is too costly for the courts, so they have a strong external incentive to resolve similar claims as a single collective one and thereby avoid future similar claims.20
There are several examples from Latin American right to health case law that illustrate our points, including a major piece of Colombian right to health litigation. A 2008 report by the Colombian Human Rights Ombuds Office showed that a staggering 674,612 petitions for the protection of constitutional rights related to health issues were filed in the courts between 1999 and 2008.21 The Constitutional Court has accepted more than 1,000 health-related cases since its formation in 1991.22 The Colombian Constitutional Court had to confront the failings of the judicial system when it became clear that the inflexible infrastructure of the courts was incapable of meeting the demands of victims defending their constitutional right to health. Courts were collapsing under the sheer volume of individual injunctions, or tutelas as amparo is known in Colombia, filed. To address this problem, the Court issued judgment T-760/08 in 2008, which deemed that most of the individual cases shared one cause: insufficient access to health services. Consequently, the Court grouped all the individual cases into one collective conflict that became the clarion call for Colombian health care system reform. The judgment “examined systemic failures in the regulation of the health system, re-asserted the justiciability of the right to health, and called for significant restructuring of the health system based on rights principles.”23 In addition, the Court also stated that the consolidation of individual claims into a single comprehensive suit is possible “whenever it is not appropriate for the individual rights-holder to act independently [en forma exclusiva].”24 This shows how quantitative issues, such as the volume of individual cases that comprise a collective conflict, can shed light on the qualitative issues that may be systematically violating people’s right to health, thus shifting the discussion from an individual complaint into a collective issue.25
In the case of Colombia, judicial activism was largely responsible for the shift from multiple individual claims to collective litigation. The judicial solution to a practical problem resulted in the innovative creation of an informal collective amparo, a concept that Colombian legislators had not previously considered. Notwithstanding the Colombia Constitutional Court´s intervention, which demonstrated an awareness of and commitment to health equity, the guidelines we suggest call for regulation that would allow claimants to organize themselves and file claims collectively. Thus, the proactive role of the courts—to advance the right to health through deliberation—would shift to the claimants. Judicial review would only have to address the issue of compliance to the procedure or upon a violation of due process, drafted according to these guidelines, and intervene when collective discussion or the participation of all affected parties had not been guaranteed.26
In contrast to the drawbacks of the individual amparo as it originally appeared in Colombian law, the writ of amparo in Argentina’s Constitution offers an appealing, flexible framework for bringing the acts or omissions of state and non-state actors to justice. We propose that the guidelines be based on a similar framework. The Argentinean collective amparo enables plaintiffs to challenge acts or omissions from state and non-state actors that result in discrimination or threaten or harm rights that protect the environment, fair competition, the consumer, and collective rights. The collective amparo is not regulated by a specific law, but is extrapolated from the ideas enshrined in a single article of Argentina’s Constitution.27 Article 43 broadens the concept of standing to sue so that the affected individual is no longer the only interested party who may file an amparo. A similar interpretation was elaborated by the Constitutional Court of Colombia regarding the tutela.28 Accordingly, the benefit of the collective amparo is that victims of indirect harm can also file it.29 Therefore, civil society organizations whose object is compatible with the claim under review may also file an amparo, as can the Ombuds Office.30 Interpreting this clause in the 1997 case Asociación Benghalensis y otros c. Estado Nacional, the Argentine Supreme Court famously held that civil societies that can demonstrate an interest in the suit have standing to sue under the constitutional right to the writ of amparo.31 The court found that Asociación Benghalensis, an organization dedicated to fighting HIV/AIDS, had standing to sue the state for omissions in advancing access to health treatments for people living with HIV/AIDS.32
Regarding situations where the state is the defendant, our guidelines propose that the collective remedy may be filed against both state and non-state actors. Recent case law, including a landmark 1998 right to health case in Argentina, Mariela Viceconte v. Ministry of Health and Social Welfare, illustrates the benefits of this possibility.33 Representing several community groups, the plaintiff sought to require the state to provide a vaccine against the Argentine hemorrhagic fever that threatened the lives of 3.5 million people. Most of the at-risk population did not have access to preventive medical services. The plaintiff´s argument invoked the state’s obligation to prevent, treat, and control endemic and epidemic diseases recognized in Article 12.2c of the International Covenant on Economic, Social and Cultural Rights (ICESCR). The Federal Administrative Court of Appeals ordered the government to designate funds for completing the vaccination campaign and ensuring the production of the vaccine. Remarkably, the Court also put a follow-up framework in place to oversee compliance with its ruling. Additionally, the Court established a deadline for the state to meet the requirements. The Court’s ruling was based on regional and international standards defined by international human rights instruments of constitutional rank in Argentina: the American Declaration on the Rights and Duties of Man, the Universal Declaration of Human Rights, and perhaps more importantly, Article 12 of ICESCR.
The case has often been referred to as an example of how difficult it is for courts to decide cases where important state financial commitments are at stake; it took ten years to overcome the budgetary obstacles to implementing the vaccine. Nevertheless, in spite of these difficulties, the case set an important precedent in many ways. First, it showed that ordinary citizens, such as the plaintiff Viceconte, can utilize the amparo and gain access to the courts to challenge state action or inaction. Second, the case is an example of how local courts can directly invoke international human rights doctrine to mandate the fulfillment of states´ human rights duties. Third, by imposing a deadline, the Court affirmed the importance of the state as the main guardian of the right to health. The case is also an example of how courts can take part in the political process by impacting how administrative and political authorities set priorities and allocate budgets.34
In situations where the collective right to health amparo is brought against non-state actors for violating fundamental rights, Venezuelan case law offers a paradigmatic example. In Defensora del Pueblo de la República Bolivariana de Venezuela et al. v. Galaxia Médica C.A., a group of women filed a collective amparo against a number of corporations and the state for marketing toxic breast implants as safe.35 In granting the case’s admissibility, the Supreme Tribunal invoked the “horizontal effect” of human rights duties, under which non-state actors—in this case corporations—are also bound to respect human rights, including the right to health. Additionally, the Supreme Tribunal established some of the procedural rules we suggest as guidelines to ensure effective access to justice. This includes opening channels for the participation of all affected parties and legal mechanisms to attract other possible individual claims that might be brought regarding the same cause.
From these Latin American right to health litigation experiences, we can conclude that collective procedures had a greater impact on the judiciary and the defendants because they communicated the needs, desires, and anxieties of a large group. Collective procedures transformed the complaints from isolated individual occurrences to broader societal issues. In this way, the collective writ of amparo strengthens community, equalizes the playing field in access to justice, and augments the force and effect—on both the judiciary and the defendant—of health litigation.
Some scholars criticize the central role that courts have played in protecting the right to health and the broad interpretations they have made. According to these critiques, such decisions ultimately benefit the more advantaged parties to the detriment of the disadvantaged victims of health rights violations. Several studies also demonstrate that judicial decisions on policies and budgets introduce judicial power into the sphere of executive power.36 Notwithstanding these issues, our proposed guidelines for collective remedies and participatory frameworks address these potential problems. The conceptual framework of guidelines advocates a different understanding of judicial review. From our standpoint, the judiciary´s role in the process would require its intervention to secure the participation of all possible affected parties and call for public hearings to promote open discussion about the proper solution to right to health conflicts.37 The court´s institutional objective would be to ensure that the health policies impacting society are the result of collective and inclusive debate. Sentence T-760/08 from Colombia is a good example of what we have in mind: the Constitutional Court of Colombia showed commitment to collective debate by holding public sessions exhorting the authorities to provide reports on the system of public health care coverage and its challenges, and information to those affected by the healthcare system’s failings. Colombian society was heard when the Court struck down structural aspects of Colombia´s public health system. In turn, in the Venezuelan case, the affected parties were gathered in public audiences to inform the Court about the claims under the suit. Additionally, the Supreme Tribunal urged the ombudsman to establish methods for all affected parties to participate in the public session online. All in all, these examples demonstrate the amparo’s usefulness as an effective remedy and its compatibility with participatory and robust notions of the role of courts. This disproves the objections that have been made about the illegitimacy of decisions affecting social policies or the dysfunction of state institutions.
Conclusion
We believe an FCGH should include guidelines on effective access to the judicial system in cases involving the right to health. The proposed guidelines would be the initial codification of normative parameters on access to justice. The proposed guidelines would prevent current pathological results in health rights litigation. We also argue for a robust conception of standing to sue. On the one hand, by allowing for collective claims, the guidelines offer mechanisms to promote the right to health of the most disadvantaged. On the other hand, the guidelines allow for the participation of juridical actors like the ombudsman for “institutionalizing” the health issues that are a priority for the most disadvantaged. In the absence of these procedures, as we have seen, individual claims cannot be channeled into a collective claim and the failures of the justice system become immediately apparent. In addition, the guidelines suggest that state parties to an FCGH should allow for simple, brief, and expedited claims not only against the state, but also against non-state actors. If an FCGH adopted these guidelines, it would set the stage for further, more detailed global agreements about how each country should internally design and tailor its procedural rules so that litigation can be as effective, efficient, and as socially beneficial as possible for everyone.
Acknowledgements
The authors would like to thank Marinka Yossiffon-Halpern, who meticulously edited this paper and challenged us on many points. Eric Friedman’s comments were also much appreciated. We are grateful to the two anonymous referees and to the editors of this special issue for their helpful comments.
Martín Hevia, SJD, is the Director of the LL.B. Program and an Assistant Professor at the Escuela de Derecho, Universidad Torcuato Di Tella in Buenos Aires, Argentina.
Carlos Herrera Vacaflor, JD, is a lawyer who graduated from the Escuela de Derecho, Universidad Torcuato Di Tella in Buenos Aires, Argentina.
Please address correspondence to the authors c/o Martín Hevia, Universidad Torcuato Di Tella School of Law, Avenida Figueroa Alcorta 7530 (C1428BCW) Buenos Aires, Argentina, email: mhevia@utdt.edu.
References
1. Joint Action and Learning Initiative for National and Global Responsibilities for Health, JALIHEART.COM. Available at http://www.jalihealth.org/; See also L. O. Gostin, “A framework convention on global health: Health for all, justice for all,” JAMA 307/19 (2012), pp. 2087-2092. Available at http://jama.jamanetwork.com/article.aspx?articleid=1157495; E. A. Friedman and L. O. Gostin, “Pillars for progress on the right to health: Harnessing the potential of human rights through a global convention on global health,” Health and Human Rights: An International Journal 14/1 (2012). Available at http://www.hhrjournal.org/index.php/hhr/article/view/483/751.
2. Ibid., p. 2.
3. Ibid.
4. Minister of Health & Others v. Treatment Action Campaign & Others (July 5, 2002), CCT 8/02 (Constitutional Court of South Africa). Available at http://www.saflii.org/za/cases/ZACC/2002/15.html; State of Punjab & Others. v. Mohinder Singh Chawla (December 17, 1996), SC 1225/97 (Supreme Court of India). Available at http://indiankanoon.org/doc/1569214/; Cruz del Valle Bermúdez & Others. v. Ministerio de Sanidad y Asistencia Social (Supreme Court of Justice of Venezuela, Case No. 15.789, Decision No. 916, July 15, 1999). Available at: http://www.law.georgetown.edu/oneillinstitute/global-health-law/who-hhr/caselaw-detail.cfm?id=1292&b=1; Sandra Clemencia Perez Calderon & Others (Constitutional Court of Colombia, Case No. T-140800, Decision SU-225/98, May 20, 1998). Available at http://www.corteconstitucional.gov.co/relatoria/1998/SU225-98.htm.
5. See, for example, Article 4 of the 1857 Constitution of Mexico; Article 9 of the 1980 Constitution of Chile; Article 19 of the 1987 Constitution of Haiti; Article 20 of the 2012 Constitution of Hungary; Article 42 of the 1994 Constitution of Argentina; Article 83 of the Constitution of Venezuela; Article 18 of the Constitution of the Plurinational State of Bolivia; Article 43 of the Constitution of Spain; Article 64 of the 1976 Constitution of Portugal; Article 23(2) of the Constitution of Belgium. All available at http://www.constitution.org/cons/natlcons.htm.
6. Constitution of Colombia (1991), Art. 93. Available at http://confinder.richmond.edu/admin/docs/colombia_const2.pdf; Constitution of Argentina (1994), Art. 75(22). Available at http://www.senado.gov.ar/web/interes/constitucion/english.php; Constitution of Costa Rica (1949), Art. 105. Available at http://www.costaricalaw.com/legalnet/constitutional_law/constitenglish.html; Constitution of Switzerland (1999), Art. 121. Available at http://www.admin.ch/ch/e/rs/1/101.en.pdf; Constitution of the Republic of India (2007), Art. 52(c). Available at http://lawmin.nic.in/coi/coiason29july08.pdf, are some examples.
7. See, for example, L. M. Ferraz, “The right to health in the courts of Brazil: Worsening health inequities?” Health and Human Rights: An International Journal 11/2 (2009), p. 40. Available at http://www.hhrjournal.org/index.php/hhr/article/view/172/25. See also A.Yamin and S. Gloppen (eds.), Litigating health rights: Can courts bring more justice to health? (Cambridge, MA: Harvard University Press, 2011).
8. See, for example, WHO Framework Convention on Tobacco Control, World Health Assembly Res. 56.1 (2003). Available at http://whqlibdoc.who.int/publications/2003/9241591013.pdf.; Vienna Convention for the Protection of the Ozone Layer, UNEP Governing Council TIAS No. 11,097 (1987). Available at http://untreaty.un.org/cod/avl/ha/vcpol/vcpol.html; and the United Nations Framework Convention on Climate Change, FCCC/INFORMAL/84 (1992). Available at http://unfccc.int/2860.php.
9. Ibid.
10. See, for example, German Constitution (2009), Art. 93(1). Available at http://www.servat.unibe.ch/icl/gm00000_.html; Spanish Constitution (1978), Art. 41(2). Available at http://www.congreso.es/portal/page/portal/Congreso/Congreso/Hist_Normas/Norm/const_espa_texto_ingles_0.pdf; Constitution of Hungary (2011), Art. 64. Available at http://www.kormany.hu/download/4/c3/30000/THE%20FUNDAMENTAL%20LAW%20OF%20HUNGARY.pdf; Article 144 of the BVerfG do not prescribe effective legal remedies against non-state actors. Available at http://www.gesetze-im-internet.de/gg/BJNR000010949.html.
11. F. Verbic, Procesos colectivos (Buenos Aires: Ed. Astrea, 2007), pp. 34-36.
12. See, for example, Recurso Extraordinario (November 24, 2000) STF 271.286-8 D.J. (Federal Supreme Court of Brazil) or Caja Costarricense de Seguro Social (September 23, 1997) SC Res. 5934-97 (IV Constitutional Chamber of the Supreme Court).
13. Colombia´s executive decree 2591/1991, Art. 46. [unofficial translation]. See César Gaviria, Executive Order 2591: Acción de Tutela [Legal Protection Writ], November 19, 1991 (Colombia).
14. See Defensora del Pueblo de la República Bolivariana de Venezuela et al. v. Galaxia Médica C.A (June 6, 2012) TSJ Sentence No. 790 (Supreme Tribunal of Justice of Venezuela); Defensora del Pueblo v. Minister of Health et al. (access to medical treatment) (July 14, 2000) CCB N° 687-200-R (Constitutional Court of Bolivia).
15. L. M. Zanitelli, “Corporations and human rights: The debate between voluntarists and obligationists and the undermining effects of sanctions,” SUR International Journal on Human Rights 8/15 (2011), p. 36.
16. Ibid, pp. 35-55.
17. Para. 42 of CESCR General Comment 14 can also be understood in that light. See http://www1.umn.edu/humanrts/gencomm/escgencom14.htm).
On non-state actors and human rights violations, see S. Michalowski and J. P. Bohoslavsky, “Jus cogens, transitional justice and other trends of the debate on odious debts—A response to the World Bank discussion paper on odious debts,” Columbia Journal of Transnational Law 48/61 (2010); J. P. Bohoslavsky and V. Opgenhaffen, “The past and present of corporate complicity: Financing the Argentinean dictatorship,” Harvard Human Rights Journal 23 (2010), pp. 157-223.
18. Special Rapporteur´s Guidelines for Pharmaceutical Companies in Relation to Access to Medicines, available at http://www.who.int/medicines/areas/human_rights/A63_263.pdf.
19. The “Ruggie Principles,” UN Guidelining Principles on Business and Human Rights. See http://www.business-humanrights.org/SpecialRepPortal/Home/Protect-Respect-Remedy-Framework/GuidingPrinciples with summary at http://www.humanrights.gov/2012/12/03/un-guiding-principles-on-business-and-human-rights/.
20. Verbic, p. 52. See note 11.
21. Defensoría del Pueblo (Ombuds Office’s Office of Colombia), La tutela y el derecho a la salud. Periodo 2003-2005 (2007), pp. 77-79; Defensoría del Pueblo, La Tutela y el Derecho a la Salud. Periodo 2006-2008 (2009), p. 30 [hereinafter Defensora del Pueblo 2006-08].
22. Luz Mary Osorio Palacio & Others. v. SaludCoop & Others (July 31, 2008) CCC Judgment T-760/08 (Constitutional Court of Colombia, Second Panel of Review), sec. 3. Available at http://www.corteconstitucional.gov.co/relatoria/2008/T-760-08.htm. See also A.Yamin and O. Parra-Vera, “Judicial protection of the right to health in Colombia: From social demands to individual claims to public debates,” Hastings International and Comparative Law Review 33/432 (2010).
23. Ibid.
24. Ibid.
25. Verbic, p. 35. See note 11.
26. On judicial intervention in this sense, see, J. H. Ely, Democracy and distrust: A theory of judicial review (Cambridge, MA: Harvard University Press, 1980).
27. Constitution of Argentina (1994), supra note 5, Art. 43, para. 2. Available at: http://www.senado.gov.ar/web/interes/constitucion/english.php.
28. See, for example, C. Botero, La acción de tutela en el ordenamiento constitucional colombiano (Bogotá: Escuela Judicial Rodrigo Lara Bonilla, Consejo Superior de la Judicatura, 2006), pp. 85-88.
29. A. M. Morello and C. A. Vallefín, El amparo: Régimen procesal (La Plata: Librería Editora Platense, 2004), p. 286.
30. There is literature that makes the argument for including the Public Office (public defenders included) as an interested party that may file an amparo to advance the protection of the right to health. See, for example, Verbic, note 11, p. 76; O. L. Motta-Ferraz and D. W. Liang Wang, “Can public attorneys improve health equity through right to health litigation? A case study of the city of Sao Pablo” (unpublished manuscript). Available at www.raison-publique.fr/…/WangFerr.; the regulation of the tutela in Colombia explicitly allows the Ombuds Office to file a tutela writ indistinctively of what the affected party decides. See note 28, Botero, pp. 89-91.
31. Asociación Benghalensis v. Ministerio de Salud y Accion Social-Estado Nacional (National Supreme Court of Justice of Argentina, A. 186, XXXIV, June 1, 2000). Available at http://www.law.georgetown.edu/oneillinstitute/global-health-law/who-hhr/caselaw-detail.cfm?id=1464&b=1.
32. Idem, cited in A. M. Morello & C. A. Vallefin, supra footnote 29, p. 290. Case law of the Constitutional Court of Colombia also acknowledges civil society organizations and groups standing to sue. See, C.C.C., Judgment T-411/92, in Botero, supra footnote 28, p. 87.
33. Mariela Viceconte v. Ministry of Health and Social Welfare (June 2, 1998) FACA Exp. 31 777/96 (Federal Administrative Court of Appeals of Argentina, Fourth Chamber). See also, V. Abramovich, Argentina: The Right to Medicines’ in Litigating Economic, Social and Cultural Rights: Achievements, Challenges and Strategies (COHRE 2003).; V. Abramovich & L. Pautassi, “Judicial Activism in the Argentine Health System: Recent Trends,” Health and Human Rights: An International Journal 10/2 (2008), pp. 57-58.
34. Mariela Viceconte v. Ministry of Health and Social Welfare. See note 31.
35. Defensora del Pueblo de la República Bolivariana de Venezuela et al. v. Galaxia Médica C.A. See note 14.
36. O. L. Motta Ferraz, “Harming the poor through social rights litigation: Lessons from Brazil,” Texas Law Review 89/1643 (2011); C. Rodríguez-Garavito, “Beyond the courtroom: The impact of judicial activism on socioeconomic rights in Latin America,” Texas Law Review 89/1669 (2011).
37. R. Gargarella, “Dialogic justice in the enforcement of social rights,” in A.Yamin and S. Gloppen (eds.), Litigating the Right to Health: Can courts bring more justice to health systems? (Cambridge, MA: Harvard University Press, 2011).