HIV/AIDS in Cuba: A rights-based analysis
Tim Anderson
Health and Human Rights 11/1
Published June 2009
Abstract
The common assertion that Cuba’s achievements in HIV/AIDS control have come at a cost in human rights is reinforced by US hostility toward its small neighbor. Nevertheless, a rights-based analysis may be one useful way of examining the actual Cuban experience. By reference to the United Nation’s Guidelines on HIV/AIDS and Human Rights, this paper examines the Cuban experience as it relates to the themes of quarantine and personal freedom; privacy in testing and tracing; education, participation, and non-discrimination; and the availability of AIDS treatment. The paper concludes that Cuba’s quarantine period was unnecessarily prolonged in the late 1980s but that this prolonged quarantine did not target men who have sex with men. Testing and tracing procedures in Cuba follow a standard protocol, but they are more thorough than elsewhere. Cuba has strengthened participation in education programs, and treatment is now the best in the Caribbean region. The human rights implications of HIV programs must be considered in an integrated way. Selective criticisms of the Cuban program have not improved international understanding of HIV/AIDS treatment in Cuba.
Introduction
Cuba has achieved the lowest rate of HIV infection and the highest level of AIDS treatment in the Caribbean region.1 Yet the Cuban HIV program — part of its famous health system — has been subjected to many criticisms, usually linked to the themes of “freedom” and “rights.” These criticisms must be seen in the broader context of demands for economic “freedoms” in Cuba and in the context of US demands for the dismantling of Cuban socialism and for widespread privatization, including privatization of the public health system. Outside understandings of the Cuban health system are further undermined by the US economic blockade of Cuba, roundly condemned each year by the United Nations General Assembly, which prevents normal scientific and cultural exchange between the US and Cuba.
In view of the global search for lessons on best practices for containing the HIV/AIDS pandemic, particular criticisms of the Cuban HIV program deserve closer attention. A rights-based analysis could be one useful way of examining the Cuban experience. Such an approach might address some of the criticisms directed at Cuba, whether through a selective focus on particular rights issues or through general, utilitarian notions that Cuba has forced “trade offs” between personal liberties and the protection of public health.2
This paper introduces the Cuban experience with HIV/AIDS by reference to historical developments and recent Cuban perspectives. It draws on data from interviews with a number of Cuban peer educators and HIV professionals in 2005–2006. Following discussion of these interviews, the paper then uses the United Nations International Guidelines on HIV/AIDS and Human Rights to apply a rights-based analysis to several themes in the way Cuba approaches HIV/AIDS treatment: quarantine and personal freedom; privacy in testing and tracing; education, participation, and non-discrimination; and the availability of AIDS treatment. It concludes with a rights-based assessment of the Cuban program.
Achievements and criticism
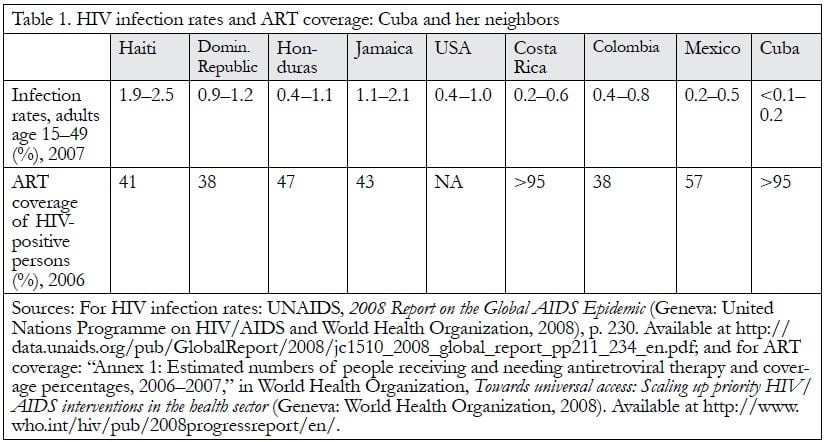
UNAIDS notes that “Cuba’s epidemic remains the smallest in the [Caribbean] region,” with a sexually active adult infection rate of around 0.1%.3 Table 1 shows infection rates and antiretroviral therapy (ART) coverage rates for Cuba and many of its closest neighbors. The Caribbean region has the second highest HIV infection rate in the world, and Cuba, often advertised in tourism literature as a “sexually permissive” society, appears particularly exposed to risk as it has been receiving more than two million tourists per year since 2004.4 Although there has been a steady increase in newly reported HIV infections since the late 1990s, mostly in men who have sex with men (MSM), Cuba’s epidemic remains relatively small.
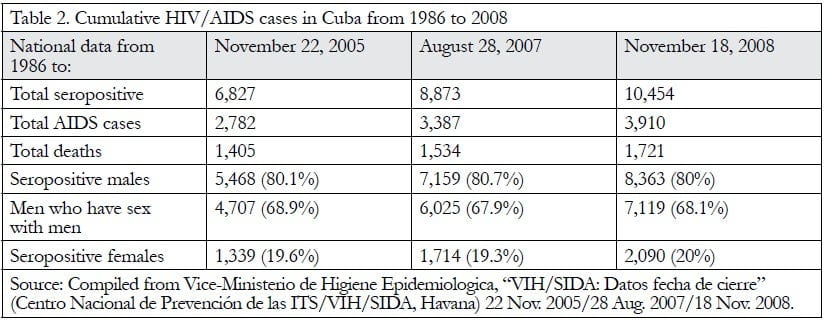
Nevertheless, by late 2008, Cuba’s infection rate had risen (see Table 2) and may now approach 0.15% of sexually active adults. This is still a significantly lower rate than that of Cuba’s neighbors, but it represents an ongoing challenge. After universal and free coverage of patients with antiretroviral treatment began in 2001, the death rate fell markedly.5 The HIV infection prevalence is slowly rising, but AIDS is being controlled.
In the face of these achievements, there has been a series of predominantly US-based criticisms of the Cuban methods, mostly in the popular media but reinforced by some academic material. The first criticism was over the 1986–1989 use of a mandatory quarantine period in health resorts (called sanatorios, or sanatoria) for the first persons infected with HIV. A Los Angeles Times report from 1988 noted that a US delegation visiting a sanatorium described it as “pleasant but frightening.”6 The following year, a US medical report noted wide-scale testing but claimed that “Cuba has not made education the key focus of its anti-AIDS strategy.”7 Such criticisms were not always well-informed. Education has been central to the Cuban HIV/AIDS programs from the beginning, though the emphases of education efforts have changed (discussed further below).
Programs similar to Cuba’s experiment with quarantine were also proposed in many parts of the US in the 1980s. Between 1987 and 1990, for example, “more than a dozen states” brought AIDS within the scope of state quarantine statutes.8 However, modernization of these laws generally included provisions for “the least restrictive alternative.”9 In Cuba’s case, patients began to come and go from sanatoria in 1989. In 1993, an alternate non-sanatoria-based day care program was introduced.10 Some US medical reports took the Cuban approach seriously, studied it in some detail, and noted the phasing-out of quarantine in the late 1980s.11 Nevertheless, attacks in the popular media continued long after the removal of quarantine, even though advances in HIV education were also noted.12
These attacks have used examples — from individual cases and from the testing regime as a whole — in their efforts to reinforce the theme that Cuban patients with HIV/AIDS were being deprived of their freedom as a way to explain Cuba’s relative success. Some Cuban professionals, however, do not consider the early quarantine period to have been a significant part of their program’s success.13 One 2003 medical report, for example, noting that Cuba had an HIV infection rate “nearly eleven times lower than [that of] the United States,” suggested that this could be due to Cuba being “politically and socially isolated,” to Cubans being less susceptible to risk factors such as poverty and social inequality, and to “aggressive HIV screening and subsequent contact tracing of infected individuals.”14 Yet “aggressive” seems an inappropriate word and “isolated” improbable since, by the time of the report, there had been nearly a decade of mass tourism to Cuba.
A rights-based analysis
In view of the polemics over Cuba and their extension into discussions of the Cuban HIV program, it seems useful to complete a more systematic rights-based analysis of the Cuban program in historical perspective.15 This can be done by reference to the UN’s human rights guidelines, which call on states “to implement an effective, rights-based response” to the HIV pandemic.16 I will do this by addressing the major relevant themes of quarantine and personal freedom; privacy through the testing and tracing regimes; the rights of education, participation and non-discrimination; and finally the right to access AIDS treatment.
Quarantine and personal freedom
The quarantine period that was enforced as a standard procedure for HIV/AIDS treatment in Cuba between 1986 and 1989 is probably the most controversial practice associated with Cuban health care. As it relates to human rights, the issue here is the personal freedom of movement, a cost borne by every person subject to any quarantine regime; such a denial of freedom may also have discriminatory implications.17 However, two misunderstandings persist about the Cuban quarantine period. First, it is sometimes suggested that the practice persisted into the 1990s, when the virus and its treatment were better understood.18 Second, it has been suggested that quarantine predominantly targeted men who have sex with men (MSM).19 In response to these criticisms on quarantine, Cuban authors argue that it was an emergency response that took place when little was known about the disease and that the practice has since changed.20 Cuban respondents also argue that the initial (quarantine) period gave health care workers a useful “space” to prepare a more considered response.21 Nancy Scheper-Hughes was told that the early use of sanatoria was not about quarantine but rather “aggressive medical treatment, research, testing of new drugs and epidemiological vigilance”; Scheper-Hughes concluded that she was left with “contradictory impressions” but mostly admiration for the achievements of the Cuban program.22 Most visitors to the sanatoria have commented favorably on their environment, food, and general conditions. A smaller group of patients remains in sanatoria voluntarily, to this day, because of the favorable conditions and support or because of problems at home. Yet some relationship between the initial quarantine and issues of stigmatization and fear of the disease has also been acknowledged.23
A National AIDS Commission was set up in Cuba in 1983 with the aim of developing a complete prevention and treatment program. In that same year, Fidel Castro charged the Instituto Pedro Kourí with the responsibility of ensuring that this epidemic “does not constitute a health problem for Cuba.”24 The first Cuban AIDS case was not diagnosed until 1985, and the first death occurred in 1986; the decision to proceed with sanatoria was based on a 1982 law set up to allow for the isolation of those carrying an infectious disease that might be a danger to the public.25 The first sanatorium was in Havana Province; soon others on the island followed. Cuba has more recently used quarantine to prevent dengue fever victims from infecting the broader population.26
The Cuban quarantine of HIV-positive persons has raised concerns about the likelihood of unjust discrimination against gay and bisexual men in light of Cuba’s traditionally “macho” culture and the emerging trend of the 1980s to associate HIV/AIDS with MSM. In the 1980s, Cuban analysts recognized that the groups most at risk for HIV infection in Western countries were MSM, intravenous drug users, and those receiving blood transfusions. Yet the association of HIV infection with gay and bisexual men was not a global tendency, since those at risk in Africa were young sexually active heterosexuals, children, sex workers, and those receiving blood transfusions.27 Cuba in the 1980s was strongly linked to Africa through various aid missions, particularly through its deployment of thousands of troops in Angola. AIDS in Africa was and remains a disease primarily affecting heterosexual persons, with almost equal numbers of HIV-positive women and men. Initial evidence suggested that Cuba had a pattern of HIV infection similar to that of Africa, though there were signs of an emerging hybrid infection pattern toward the Western one of a largely MSM epidemic. By 1988, Cuba had 190 HIV-positive cases and seven deaths. By the late 1980s, MSM were substantially over-represented in the HIV-positive population in Cuba but were still a minority of cases (39 cases or 21%); these numbers were identical to those for infected women.28 MSM were thus a minority of those quarantined for HIV/AIDS. This may suggest that the stigmas associated with HIV infection and against homosexuality (in a culture with significant homophobia) did not necessarily coincide. The initial quarantine measure therefore did not suggest a regime of discrimination against gay and bisexual men, since they did not constitute a majority of infected persons until later in the mid-1990s.
From 1989 onward, patients could come and go from the sanatoria, and at the end of 1993, the day care program (sistema de atención ambulatoria or SAA) was opened for all those who did not want to live in a sanatorium. However, all newly infected patients were (and are) required to attend a course called “Living with HIV.” Those in the SAA program live at home but attend clinics daily. They receive the same treatment as those at the sanatoria, including a diet supplemented with milk, fiber, and vegetables.29 After the first few months of close observation at the sanatoria, patients are monitored as outpatients by their family doctor.30 In January 1998, the “Hospital for a Day” system was opened. This provided morning sessions in the sanatoria as part of an eight-week program.31 Some of these programs were later taken over by support teams, and since the year 2000, many newly-diagnosed patients do not use sanatoria at all, opting instead to participate in the “Living with HIV” program. This program is directed and operated by peer educators (who are often also HIV-positive) in a community-based “Line of Support” for those living with HIV/AIDS.32
By the mid-2000s, those voluntarily in the sanatoria appeared to be a shrinking minority; in Plaza Municipality, for example, seven times more HIV-positive individuals were in day care than in sanatoria.33 Nevertheless, the expansion in day care seems to have resulted in sanatoria populations composed of a disproportionately high percentage of socially marginalized individuals. In 2002–2003, for example, 80% of the 267 patients at Los Cocos had some family dysfunction, 66% had been unemployed, over 40% had some type of psychiatric disturbance, and over 50% had received only basic secondary schooling (a low level for Cubans).34 These statistics have been cited in Cuba as evidence of the need to further develop integrated systems of social support to prevent isolation of marginalized people.35
Social integration rather than isolation remains a strong priority of the Cuban system. A specialist nurse with nine years of experience in Cuba’s HIV/AIDS programs puts it this way:
From the time a person is diagnosed, it is the responsibility of the state to put that person back in society to resume their normal life. So public health, workplaces, mass organizations, all have a role in the well-being of the patient, so that they don’t feel rejected, so they know this is a person living with a virus, or an illness, but that this is nothing to be ashamed of.36
An important structural part of this policy of social inclusion is that by law all HIV-positive patients maintain their job entitlements and 100% of their salary when they have to be absent from work for programs or treatment.37 Despite this law, some Cuban employers have tried to remove HIV-positive people from their jobs. In a survey of 80 patients who had left Los Cocos sanatorium for ambulatory care, 16 had faced attempts to exclude them from their work. For 12 patients who had permanent jobs, these attempts failed, except in the case of one individual who became discouraged and abandoned his appeal. However, four individuals who had been on temporary contracts lost their jobs, even though they had been considered good workers. Some health workers have also faced pressures, for example, to move their place of work to an HIV patient care facility, such as a sanatorium. This had led to calls for greater clarity in anti-discrimination procedures and for more social support consistent with “the principles of solidarity of Cuban society.”38
Although the early quarantine practice was a result of a strong directive to protect public health, it seems that fear of the disease, including fear among some professionals, may have led to the prolonging of the quarantine period.39 This extension was an unreasonable deprivation of liberty, but there is no evidence that the early quarantine period was directed at gay and bisexual men — or more broadly, MSM — who formed a minority of the HIV-positive population at that time.
Privacy: Testing and tracing
The second main theme of the rights-based criticism of the Cuban quarantine system for HIV/AIDS relates to privacy concerns over the regimes for testing and contact tracing. The UN has called for law and practice to “ensure privacy and confidentiality” of HIV-infected people and their families.40 Here criticism of Cuba has been anecdotal and weak. While the Cuban practice of testing and contact tracing is thorough, its basic principles appear similar to those of many other countries with effective testing regimes. Scheper-Hughes described early Cuban testing as part of “the classical public health tradition — routine testing with contact tracing and partner notification,” yet also as “the most comprehensive . . . of any nation.”41 Testing is neither universal nor aggressive but is targeted at high-risk groups. Patient consent is required for any personal procedure, such as a blood test, and privacy laws to protect patient confidentiality are said to be taken seriously.42
Testing began in 1986, and by the following year, testing included vulnerable groups such as pregnant women, health workers, blood donors, and those who had traveled to areas with a high incidence of the disease.43 By February 1988, around 25% of the sexually active Cuban population had been tested. There was mandatory testing of blood donors, pregnant women, those with other sexually transmitted diseases (STDs), all hospital admissions, and the sexual contacts of those already infected. Some critics of the Cuban system complained about its sexual contact tracing and requests for testing.44 However, this practice is hardly unique to Cuba. Some invasion of the privacy of the contact group would seem to be justified on public health grounds; indeed measured breaches of privacy occur in most forms of epidemiological surveillance. In 1988, there were positive results in almost 4% of contact trace testing in Cuba, a far higher level than any of the other groups (pregnant women, and so forth) undergoing targeted testing.45
By 2003, there were approximately 1.5 to 1.6 million tests per year.46 While MSM came to be the largest infected group in the mid-1990s, women still constitute 21% of infected Cubans, and they are the fastest growing HIV-positive group.47 All testing is done through the family doctor or anonymously through a Policlinic (Cuban treatment centers that carry out most procedures and lie between the basic community health centers and the hospital system). Blood tests require patient consent, a fundamental element of Cuban medical practice.48 Sexual contacts are traced with some sensitivity but also with thoroughness. There is a fair degree of moral persuasion in the Cuban system, generally, but our interviews suggested that there is also a respect for rights in the professional procedure. When there is a positive HIV finding, for example, the person is asked, as part of a structured interview, for all of their sexual contacts in recent years. These contacts are followed up with privately by the family doctor and often assisted by a nurse.49 HIV cases and some other listed diseases (such as leprosy) are confidentially registered with the National Center for Epidemiology. This information is protected by law, with penalties for breaches of the privacy of patients’ records.50
The November 2005 data for Plaza Municipality (which, by Cuban standards, has a high rate of infection), covering 1985–2005, gives a more detailed picture of the Cuban HIV-positive population and the testing system. Over the previous twenty years in Plaza Municipality, 57 HIV-positive individuals died, and the remaining 223 of the 280 HIV-positive persons were classified as “people living with HIV.” Of these, 187 were day care patients, 25 were in a sanatorium, 19 had gone overseas, and several were in a specialist hospital or under private care.51 The major methods of discovery of the 280 infections were by normal family doctor consultations (74), tracing the sexual contacts of infected persons after an interview (55), hospital in-patient tests (43), STD tests (36), self-reports (31), blood donor tests (29), and prisoner tests (9). A little over 15% of the group members were female and 75% were MSM. This proportion varies only slightly from the national average (see Table 2 on page 95).52
These findings seem to suggest that Cuba’s privacy and confidentiality practices in testing and tracing are standard in that laws provide penalties for breaches of the privacy rules. Cuba is distinct, however, for the moral persuasion that puts particular pressure on individual choices across a range of issues in Cuban society. Because of this moral persuasion, patients requested to disclose sexual contacts might feel a stronger sense of obligation to do so. But a strong sense of obligation to certain behaviors does not, in our view, in and of itself constitute a breach of the United Nations standards as they relate to HIV/AIDS and human rights.
Education, participation, and non-discrimination
Education on rights (to medical care and social treatment) and participation in HIV programs are important principles stressed by the UN’s human rights guidelines.53 These principles must in turn be linked to the basic right to non-discrimination. Cuba’s social policy has always stressed education and popular involvement, but the structure of the HIV program, including the education and participation components, has undergone several changes.
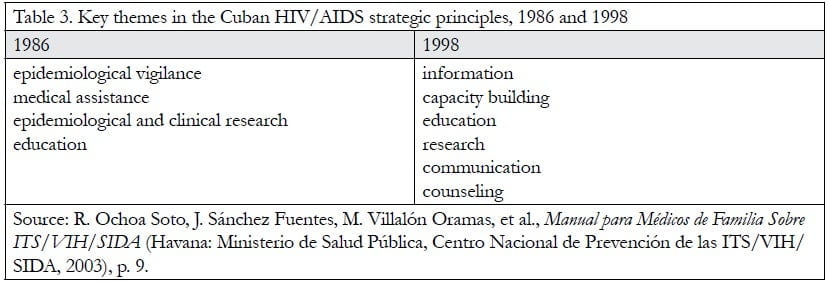
The National Program for the Prevention and Control of STDs and HIV/AIDS was established in Cuba in 1986, with the primary aim of “ensuring that the process of infection-illness does not become an important health problem for the Cuban population.”54 This preventive approach was very soon challenged by the international shift to a focus on health promotion. Committed to developing and prioritizing their health system, Cuba took seriously the discussions at the 1986 First International Health Promotion Conference in Ottawa, Canada, and began to elevate the notion of “health as a source of the richness of life,” regarding programs of prevention as “doors of entry” to health promotion.55 This principle was well established by the time Cuba revised their policy on AIDS in 1998, which was issued by the newly formed National Center for the Prevention of STDs/HIV/AIDS. This revised policy put into place a stronger emphasis on social support and participation, and this shift in emphasis is reflected in Table 3 on page 99.
Several booklets provide a foundation for patient education in the new policy. The educational text “Living with HIV” covers clinical information, HIV and the social environment, information on mutual help, nutrition and hygiene, sexuality, and some legal considerations.56 It explains the details of drug therapy, the development of mutual aid groups and self help strategies, and the rights and duties of HIV-positive persons, as well as work, social security, health, and confidentiality law. A second booklet, “Living together with HIV” is designed for the families of HIV-positive individuals; this booklet discusses topics such as the social, familial, and work implications of HIV/AIDS in addition to discussing HIV/AIDS treatment and HIV/AIDS-related concerns as they pertain to biosecurity, nutrition and hygiene, death, pregnancy, children, and where to get help.57 It explains infection and the disease, treatment regimes, and how to support family members living with the disease. When Dr. Byron Barksdale told the American Association for the Advancement of Science that the US could learn lessons from Cuba, he pointed in particular to Cuba’s six-week “Living with AIDS” program, noting that six weeks “is certainly a longer time than is given to people in the US who receive such a diagnosis. They may get about 5 minutes worth of education.”58 Indeed, the “Living with AIDS” program appears to meet several of the UN’s educational and rights requirements.59 A family doctor manual on HIV and STDs, another educational resource available in Cuba, provides parallel, detailed information to local health workers.60
Since the 1990s, when the Cuban HIV epidemic became one characterized as being most prevalent among MSM, the question of public education — in particular dealing with the compound issue of homophobia in a macho Latino culture and of public stigmatization of and discrimination against HIV patients — has required greater focus. Campaigns in support of sexual diversity, considered a part of the “social inclusion” policy, are first introduced to children through the school system, which begins sex education (including sexual diversity education) at grade five. The national program, including a TV soap opera with gay and lesbian individuals as well as characters who are HIV-positive, is led by the National Center for Sex Education (CENESEX). The Federation of Cuban Women (FMC) began sex education programs in the early 1970s and set up CENESEX in 1989. Led by Mariela Castro (daughter of Raul Castro and the late Vilma Espín, a founder of the FMC), CENESEX stresses acceptance of sexual diversity and has attracted international attention in recent years for its campaigns for the rights of transgender persons, including the recognition of an individual’s gender identity, regardless of birth sex, and provision of state-funded sexual reassignment surgery.61
Cuba’s National Center for the Prevention of STDs and HIV/AIDS, with international support (for example, from the United Nations Development Programme [UNDP]), hosts training programs, assessment, and research in-person and helpline telephone counseling, networking, condom distribution, help for mutual support groups, nutrition education, and support for vulnerable groups. An “Afroache” program trains educators and develops specially focused educational materials for addressing the issues from that religious perspective as it is practiced in Cuba.62 Although churches appear to have no great influence on the educational campaign or the use of condoms, some of the material developed by the National Center includes the basic information that safe sex includes abstinence and that this is the only form of safe sex endorsed by the Catholic Church. Nevertheless, most materials provide an overwhelming emphasis on the use of condoms, which are distributed freely, in the millions, through the National Center.
Education programs must be periodically reviewed. The manual for groups working in HIV/AIDS prevention refers to a method developed by US academic Dr. David Kolb. This method is a teaching and learning process that emphasizes a circular relationship among concrete experience, observation and reflection, conceptualization, and practice.63 Long-term cooperation was also developed with some international agencies, in particular the World Health Organization and the UNDP. The National Center for the Prevention of STDs and HIV/AIDS, for example, was created in 1998 with support from the UNDP and Doctors without Borders (Holland) to help expand HIV education.64
Many of the health promotion pamphlets that this author observed in use during 2005–2006 were aimed at the general population, with some material aimed more directly at men who have sex with men (for example, “Siempre conmigo/Always with me” and “Hablando entre nosotros/Speaking amongst ourselves”) or addressing the male responsibility for condom use (for example, “Los hombres marcan la diferencia/Men make the difference”). Another national pamphlet addressed cultural attitudes, urging, “Judge your friends by their qualities, not by their sexual orientation,” and stressing acceptance of sexual diversity to counter prejudices and stigmas. This pamphlet states that lesbian, gay, bisexual, and transgender identities are all valid forms of sexuality and gender identity and that “understanding and accepting people as they are, will make you grow as a better person” (for example, a pamphlet titled, “He is also one of us”). Local music stars have been enlisted to help promote safe sex, for example in the national HIV magazine Lazo Adentro.65
International polemic has sometimes argued that homophobia in Cuba is a matter of official policy. Some outside commentators argue that homophobia was “institutionalized,” at least prior to the 1980s.66 Nevertheless, Cuban activists for sexual diversity seem to regard homophobia these days as mostly a cultural problem.67 One activist who is transgender rejects the idea that violence against people for their sexual orientation or gender identity exists in Cuba, as it does in some other parts of Latin America.68 Fidel Castro accepts that “homosexuals were victims of discrimination” in Cuba in the past but adds that “in the more cultured sectors there was less prejudice against homosexuals. . . . [D]iscrimination and machismo are today inversely proportional to the level of culture and knowledge. . . . I would like to think that discrimination against homosexuals is a problem that is being overcome.”69
Participation of HIV-positive persons in HIV/AIDS programs, less evident in the early phase when programs were led by professionals, has increased since the 1998 reforms. Following the growth of the post-1993 day care program, a community-based “Line of Support” for people living with HIV/AIDS has been developed, and this program has been increasingly populated by HIV-positive peer educators. This changing trend in program leadership has also helped to separate much of the “Living with AIDS” program from its earlier association with the sanatoria.70 The peer educators/health promoters are volunteers, with paid time out from their employment. The number of HIV-positive educators/health promoters is not disclosed for privacy reasons, but HIV-positive workers can disclose their own status. After pressure from “Line of Support” groups, the government began to pay many of the municipal coordinators full-time salaries. Health promoters have created pressure for more resources to support the expansion of the day care program, but they have been told that this allocation of resources had to compete in the health budget with, for example, programs for children with cancer or those with diabetes.71 Both the National Center and the Line of Support have been fostering mutual support groups, some of which are very small and want to remain anonymous. Another more recent shift in health promotion campaigns has been to redirect some attention to the 25+ age group, where there have been higher than average infection rates.72
Cuba has thus taken some significant steps toward developing levels of participation in its HIV programs, as well as cooperating effectively with international agencies, as is urged by the UN guidelines.73 In the two decades since the creation of CENESEX in 1989, Cuba has made some significant advances in popular education on sexual diversity. In the HIV/AIDS program, the expanded role of peer educators in the 2000s is noteworthy, when considering the right to education and participatory programs.
AIDS treatment
With full treatment coverage of patients, Cuba’s commitment to equal and universal access to treatment is arguably ahead of the “widespread availability” of treatment measures suggested by the UN.74 However, full treatment coverage took time to implement. Drugs for antiretroviral treatment were in short supply in the 1990s, but, since 2001, 100% of Cuba’s HIV-positive patients have had access to a relatively full cocktail of ART drugs, free of charge. As a result, the death rate from HIV/AIDS has been falling rapidly, and most HIV-positive Cubans are able to avoid secondary infections. Treatment for those with opportunistic infections associated with HIV/AIDS has been coordinated through the Instituto Pedro Kourí, which specializes in tropical medicine.75
The use of immune system-boosting drugs was recommended in Cuba from 1986 onward. In 1987, zidovudine (ZDV) was recommended for all those who developed AIDS. With limited drugs available, Cuban experts stressed the need for an “intense educational campaign” designed to lower the risk of infection, emphasizing reduced “sexual promiscuity” and promoting stable relationships.76 Later literature would caution against pejorative use of the term “promiscuous.”77 In 1996, after the Worlds AIDS conference and the recommendation of highly active antiretroviral treatment (HAART), Cuba bought ART drugs for all children with AIDS and their mothers, at a cost of US$14,000 per person per year. This was a strain on resources, especially as this occurred just after Cuba’s deep economic crisis in the mid-1990s. At the same time, between 1998 and 2001, 100 Cuban AIDS patients were treated with ART drugs donated by NGOs.78 Because of these serious resource constraints, not every patient who needed it received treatment in the 1990s.
However, from 1998, with economic recovery and the gradually growing number of HIV cases, generic drugs began to be developed. Cuba was well-placed for this due to its biomedicine industry.79 The first drug produced was zidovudine. Then in 2001, lamivudine (3TC), stavudine (D4T), zalcitabine (DDC), didanosine (DDI), and indinavir (IDV) were produced. Bioequivalence was assessed and those drugs were registered for use. Production of nevirapine (NVP), abacavir (ABC), efavirenz (EFV), and nelfinavir (NFV) was then assessed. The full “cocktail” was made available to all Cubans, and after 2001 there was no further foreign assistance to purchase any HIV treatment drugs or materials except for the purchase of Western blot test materials, which supplement the Cuban ELISA test materials.80
With removal of the economic constraints and the widespread availability of ART drugs, Cuba’s treatment regime has become “pre-emptive,” unlike some health systems where initiating treatment requires an immune system below a certain level plus an opportunistic infection. Indeed, in the first years of treatment, Cuba required a CD4 cell count below 350, a viral load above 55,000 copies per milliliter, and an opportunistic infection before HAART treatment was begun.81 However, a health promoter involved in monitoring adherence to treatment programs reports that, as of late 2005, the practice had shifted to administering treatment when the cell count was low, without an additional infection required.82 This treatment plan might indeed produce better results through earlier treatment regimes. The nutritional supplements provided to HIV-positive patients most likely also assist recovery.
Final comments: HIV/AIDS and rights in Cuba
This paper has sought to apply a rights-based analysis, in light of the UN’s International Guidelines on HIV/AIDS and Human Rights, to several themes in Cuba’s approach to HIV/AIDS: quarantine and personal freedom; privacy, testing, and tracing; education, participation and non-discrimination; and AIDS treatment.
Under the Cuban constitution, the state guarantees “that every sick person will have medical attention” and that “[a]ll have the right to attention and protection of their health . . . [including] free medical and hospital attention.”83 The Cuban system appears to have made substantial steps to deliver on this promise to HIV/AIDS patients. It has also taken important steps in law and in practice consistent with the UN’s human rights guidelines, in particular on freedom of movement, privacy, and education.
The early quarantine practice followed a strong political directive to protect public health and was the result of uncertainty over the nature of the disease. However, it seems that fear of the disease, including among professionals, may have unnecessarily prolonged this quarantine period.84 This extension was an unreasonable deprivation of liberty. However, the early period and its privations do not appear to have been directed at gay and bisexual men, who formed a minority of the HIV-positive cohort at that time.
Outside suggestions that the early quarantine period traded personal liberties for public health achievements have little support in Cuba. Cuban health professionals suggest that the concerted and “intersectoral” approach to health problems, combined with strong epidemiological vigilance, extensive education campaigns, a free public health system, and social solidarity are central to the relative success of the Cuban program. The quarantine system of the 1980s is not thought to have been an important factor.85
Cuba’s privacy and confidentiality practices in testing and tracing appear to follow routine practices, though they are more thorough than in other countries, and there are penalties for breaches of privacy. Target groups have been tested from the beginning of the epidemic, and normal patient consent is required for tests. The moral persuasion that is common in Cuban culture might generate a stronger sense of obligation for patients to disclose sexual contacts, but this is not in itself a breach of UN standards.
From the 1990s onward, Cuba took significant steps toward developing participation and non-discrimination. Since this time, the country has actively promoted respect for sexual diversity. In the late 1990s, Cuba developed and backed an important peer educator campaign. There were problems in providing access to antiretroviral treatment in the 1990s, aggravated by the economic crisis and by the US economic blockade. However, the extension of full treatment to all HIV-positive patients in 2001 puts Cuba ahead of the entire region with respect to widespread availability of treatment.
It is important to consider human rights in an HIV/AIDS program in an integrated way. Selective attacks on and caricatures of the Cuban program have not helped understanding and have deprived others of the lessons that can be learned from the Cuban experience. The Cuban system has made mistakes, developed its own practices, learned from the international experience, and effectively built its capacity to meet the needs and the rights of patients, families, and the community.
Tim Anderson, BA, PhD, is Senior Lecturer in Political Economy at the University of Sydney.
Please address correspondence to the author at the Department of Political Economy, University of Sydney, NSW, 2006, Australia, email: t.anderson@usyd.edu.au.
References
1. Joint United Nations Programme on HIV/AIDS (UNAIDS), Caribbean: AIDS epidemic update, Regional Summary (Geneva: Joint United Nations Programme on HIV/AIDS and World Health Organization, 2008), p. 8. Available at http://data.unaids.org/pub/Report/2008/jc1528_epibriefs_caribbean_en.pdf.
2. See, for example, E. Michelson, “Individual freedom or collective welfare? An analysis of quarantine as a response to global infectious disease,” in M. Selgelid, M. Battin, and C. Smith (eds), Ethics and Infectious Disease (Blackwell: Melbourne, 2006), pp. 53–69.
3. UNAIDS (see note 1), p. 8.
4. UNAIDS (see note 1), pp. 215, 230; Oficina Nacional de Estadisticas, Anuario Estadistico de Cuba 2008: 15.2 Visitantes por mes (Havana, 2008). Available at http://www.one.cu/aec2008/esp/15_tabla_cuadro.htm.
5. J. Pérez, SIDA: Confesiones a un Médico (Havana: Centro Nacional de Prevención de las ITS/VIH/SIDA, 2006).
6. V. Zonana, “Cuba’s AIDS quarantine center called ‘frightening,’” Los Angeles Times (November 4, 1988), p. 1, col 5.
7. R. Bayer and C. Healton, “Controlling AIDS in Cuba: The logic of quarantine,” New England Journal of Medicine 320/15 (1989), pp. 1022-1024.
8. Pérez (see note 5).
9. R. Bayer, “AIDS, public health, and civil liberties: Consensus and conflict in policy,” in F. G. Reamer (ed), AIDS and Ethics (New York: Colombia University Press, 1991), pp. 26–49.
10. Pérez (see note 5).
11. R. Granich, B. Jacobs, J. Mermin, and A. Pont, “Cuba’s national AIDS program: The first decade,” Western Journal of Medicine, 163/2 (1995), pp. 139–144.
12. For attacks in the media, see, for example, V. Bauza and T. Collie, “HIV-positive Cubans get care but live in quarantine,” South Florida Sun-Sentinel (July 7, 2001), p. A4; For advances in HIV education that were noted at this time, see, for example, E. Pérez-Stable, “Cuba’s response to the HIV epidemic,” American Journal of Public Health 81/5 (1991), pp. 563–567.
13. T. Vilacha (Vice-director of epidemiology at La Rampa Policlinic, Havana), interview with the author, Havana, December 21, 2005; and C. Segredo (specialist nurse in HIV treatment centers, previously at Los Cocos Sanatorium and in 2006 at the Instituto Pedro Kourí), interview with the author, Havana, January 3, 2006.
14. H. Hansen and N. Groce, “Human immunodeficiency virus and quarantine in Cuba,” Journal of the American Medical Association 290 (2003), p. 2875.
15. Hansen and Groce (see note 14).
16. UNAIDS, International Guidelines on HIV/AIDS and Human Rights, 2006 Consolidated Version (Geneva: UNAIDS, 2006), p. 17. Available at http://data.unaids.org/Publications/IRC-pub07/jc1252-internguidelines_en.pdf.
17. UNAIDS, International Guidelines (see note 16), pp. 17, 19, guidelines 3, 5, and 11.
18. A. Yera (Coordinator of the People Living with HIV/AIDS Program in the Plaza Municipality), interview with the author, Vedado, Havana, December 22, 2005.
19. D. W. Johnston, “Cuba’s quarantine of AIDS victims: A violation of human rights,” Boston College International and Comparative Law Review, 15 (1992), p. 189, citation 12.
20. Yera (see note 18).
21. L. Oliva, “Modelos de salud en Cuba,” Temas 47 (2006), pp. 35–43 (interview with Dr. Francisco Rojas Ochoa on p. 39).
22. N. Scheper-Hughes, “AIDS, public health and human rights in Cuba,” Lancet, 342 (1993), p. 966.
23. Pérez (see note 5).
24. Pérez (see note 5), p. 12.
25. A. R. Socarrás, “Derechos de las personas que viven con VIH en Cuba: Legalidad y perjuicios sociales” (paper presented at El Foro en VIH/SIDA/ITS de América Latina y el Caribe 2003, Havana, Cuba, April 7–8, 2003). Available at http://www.foro2003.sld.cu/recursos/ver.php/Rosabal%20Socarrás?id=349.
26. Oliva (see note 21), p. 38.
27. E. García, N. de Quesada Ramírez, and A. Cádiz Lahens, Programa de entrenamiento sobre el SIDA 3: Epidemiología (Havana: Editorial Ciencias Medicas, 1989), p. 18.
28. García et al. (see note 27), p. 51.
29. Yera (see note 18).
30. J. Pérez, D. Pérez, I. Gonzalez, et al., “Approaches to the management of HIV/AIDS in Cuba: Case study, Perspectives and Practice in Antiretroviral Treatment” (Geneva: World Health Organization, 2004), p. 3. Available at http://www.who.int/hiv/amds/case1.pdf.
31. Socarrás (see note 25).
32. Yera (see note 18).
33. Centro de Higiénico y Epidemiología, Personas infectadas en Municipio Plaza: 1986–2005, (Municipio Plaza, Vedado: Centro de Higiénico y Epidemiología, November 2005).
34. Socarrás (see note 25).
35. Ibid.
36. Segredo (see note 13).
37. Socarrás (see note 25); Yera (see note 18).
38. Socarrás (see note 25).
39. Pérez (see note 5), pp. 21–32.
40. UNAIDS (see note 16), pp. 17–18, guideline 5.
41. Scheper-Hughes (see note 22), p. 965.
42. Vilacha (see note 13); Segredo (see note 13).
43. Pérez et al. (see note 30), p. 2.
44. Bayer and Healton (see note 7); A. C. d’Adesky, “Cuba fights AIDS its own way,” (New York: The Foundation for AIDS Research [AMFAR], 2003). Available at http://www.thebody.com/amfar/cuba_aids.html.
45. García et al. (see note 27), pp. 49–50.
46. Pérez et al. (see note 30), p. 2.
47. Yera (see note 18); Pérez et al. (see note 30), p. 1.
48. Vilacha (see note 13).
49. Ibid.
50. Segredo (see note 13).
51. Centro de Higiénico y Epidemiología (see note 33).
52. Ibid.
53. UNAIDS (see note 16), pp. 17–19, guidelines 1, 2, 5, 7, 8, 9, and 12.
54. R. Soto, J. Fuentes, M. Oramas, et al., Manual para médicos de familia sobre ITS/VIH/SIDA, (Havana: Ministerio de Salud Pública, Centro Nacional de Prevención de las ITS/VIH/SIDA, 2003), p. 9.
55. Soto et al. (see note 54), pp. 13–15.
56. A. González, M. Oramas, G. González, et al., Viviendo con VIH: Manual para las personas que viven con VIH/SIDA en Cuba, second edition (Havana: Centro Nacional de Prevención de ITS/VIH/SIDA, Havana, 2004).
57. A. de la Torre, O. Carro, and I. Carro, “Conviviendo con VIH: Manual dirigido a las familias de las personas que viven con VIH/SIDA en Cuba (Havana: Centro Nacional de Prevención de ITS/VIH/SIDA, 2003).
58. T. Fawthrop, “Cuba: Is it a model in HIV-AIDS battle?” (New York: Global Policy Forum, December 2003). Available at http://www.globalpolicy.org/component/content/article/211/44946.html.
59. See, for example, UNAIDS (see note 16), pp. 17–19, guidelines 5, 7, 8, and 9.
60. Soto et al. (see note 54).
61. M. Castro (Director of Cuba’s CENESEX), Presentation on sexual diversity and inclusion in Cuba, World Social Forum, Caracas, Venezuela (January 28, 2006).
62. Ministerio de Salud Pública, “Centro Nacional de Prevención de las ITS/HIV/SIDA” (brochure) (Havana: Ministerio de Salud Pública, 2005).
63. R. Soto, I. Santana, M. Fernández, et al., Manual metologo: trabajo de prevención de la ITS/VIH/SIDA (Havana: Ministerio de Salud Pública, Centro Nacional de Prevención de las ITS/VIH/SIDA, 2004).
64. Ministerio de Salud Pública (see note 62).
65. English translations of pamphlet titles and messages by the author.
66. See, for example, I. Lumsden, Machos, maricones and gays: Cuba and homosexuality (Philadelphia: Temple University Press, 1996).
67. Yera (see note 18).
68. Presentation on sexual diversity and inclusion in Cuba by Daniela, Cuban transgender spokesperson to the World Social Forum, Caracas, Venezuela (January 28, 2006).
69. I. Ramonet, Cien Horas con Fidel: Conversaciones con Ignacio Ramonet, 2nd edition (Havana: Oficina de Publicaciones del Consejo de Estado, 2006), pp. 253–256.
70. Yera (see note 18).
71. R. Cruz (Coordinator Provincial of the Line of Support for HIV/AIDS in Vedado, Havana), interview with the author, Havana, Cuba, (January 4, 2006).
72. Yera (see note 18).
73. UNAIDS (see note 16), pp. 17–19, guidelines 1, 8, 9, and 12.
74. Ibid., pp. 17–19, guideline 6.
75. Of note, the Policlinics (Vilacha, see note 13) do not deal with HIV or with diseases (such as malaria, for example) that are considered to no longer exist in the country.
76. García et al. (see note 27), p. 60.
77. Soto et al. (see note 54), pp. 27–48.
78. Pérez et al. (see note 30), pp. 3–6.
79. Ibid., p. 3.
80. No further foreign assistance: Ibid., p. 2; Western blot tests: Segredo (see note 13).
81. Pérez et al. (see note 30), p. 4.
82. Yera (see note 18).
83. Constitución de la República de Cuba (1976) (Havana: Editora Política, 2005), Art. 9b, Art. 50, translation by the author.
84. Pérez (see note 5), pp. 21–32.
85. Granich et al. (see note 11); Vilacha (see note 13); Segredo (see note 13).