Essential surgery: Integral to the right to health
K. A. Kelly McQueen, Doruk Ozgediz, Robert Riviello, Renee Hsia, Sudha Jayaraman, Stephen R. Sullivan, John Meara
Health and Human Rights 12/1
Published June 2010
Abstract
In a rights-based approach to health, the provision of essential surgical services is not a luxury, but a critical component of the “highest attainable standard of health.” Yet while access to select basic health care interventions has increasingly been discussed as part of the human right to health, essential surgical services have generally not been part of this discussion. This is despite the substantial global burden of surgical conditions in low and middle-income countries, extreme global disparities in access to surgical care, and the fact that relatively simple, cost-effective, and curative surgical procedures can avert disability and premature death from many life-threatening emergencies and other conditions. Many barriers, both supply and demand-related, such as constraints in human resources, infrastructure, and access to care, have limited the ability of health systems to deliver surgical services. In this paper, the authors share their experience — as a group of surgeons, anesthesiologists, emergency physicians, and public health experts working with colleagues in varied resource-constrained settings to provide basic surgical care — in addressing the challenge of realizing the right to surgery in resource-poor settings. We argue that essential surgical care should be included in the basic human right to health, and that the current emphasis on “vertical” disease-specific models of health service delivery should be broadened to include systems needed to provide surgical services. We outline the global burden of surgical conditions, discuss the public health importance of surgery, identify the most significant global disparities in access to surgical care, and provide economic arguments for surgical delivery.
Introduction
The right to health care ranks among the most basic human rights supported by The Universal Declaration of Human Rights (UDHR).1 Since the UDHR was ratified in 1949, additions have expanded the general language of the declaration, as, for example, the “right to the highest attainable standard of health” as expressed in Article 12 of the International Covenant on Economic, Social, and Cultural Rights.2 The rights to essential medicines, safe childbirth, and preventive strategies to improve baseline health (for example, clean water, nutrition, and vaccination) have been major areas of focus. Further prioritization of the right to basic health care has been proposed by leading scientists, humanitarians, and others committed to global health.3 Many agree that this right is among the most basic health care interventions that should be provided to all human beings — regardless of resources or context. More recent work argues that a commitment to delivery of such basic health care packages must go beyond moral rhetoric and humanitarian idealism to legal obligation and health policy. By these means, health systems can increase their capacity to deliver essential health care.4
Although the rights-based approach to health care is a progressive movement, access to essential surgical services has yet to be included as part of the basic human right to health. While international health experts frequently acknowledge the right to safe childbirth and the role of surgical care as essential components of emergency obstetric care, the global health community has been reluctant to acknowledge the important and increasing role of other surgical services to public health in low- and middle-income countries. For example, the basic package of health services included in the Commission on Macroeconomics and Health considers emergency obstetric care as its only surgical input, and leading funding organizations have specifically and preferentially targeted investment in infectious diseases.5 This is despite increasing evidence that charts the vast global burden of surgical conditions and the fact that relatively simple, cost-effective and curative surgical procedures can avert disability and premature death from many life-threatening emergencies and other conditions.6 Furthermore, substantial global disparities in access to surgical care and many supply- and demand-related barriers have limited the ability of health systems to deliver surgical services. Nevertheless, the crucial role of surgery in meeting the Millennium Development Goals is becoming more apparent, most obviously in addressing maternal and child health.7
In this paper we argue that essential surgical care should be considered an essential component of the basic human right to health, and that this right should extend beyond the current emphasis on “vertical” disease-specific models of health service delivery to include surgical services. In the surgical arena, a rights-based approach has been explored primarily in relation to emergency obstetric care, but must be expanded to consider surgical services more broadly.8 As a group of surgeons, anesthesiologists, emergency physicians, and public health experts working with colleagues in varied resource-constrained settings to provide basic surgical care, we will begin by outlining the global burden of surgical conditions and the role of surgery in public health. Next, we will summarize global disparities in surgical access and consider a rights-based approach to the problem, citing the specific example of expanded access to treatment for HIV-AIDS in low-income countries. Finally, we will discuss economic aspects of surgical delivery, ultimately arguing that the provision of essential surgical services is not a luxury, but rather a critical component of “the highest attainable standard of health.”
Essential surgery as a right in light of the ICESCR
The International Covenant on Economic, Social, and Cultural Rights (ICESCR) requires States to provide the “highest attainable standard of physical and mental health” for its citizens.9 The ICESCR also acknowledges that the level of this standard is constrained by both an “individual’s biological and socio-economic preconditions and a state’s available resources.”10 However, states have “a core obligation to ensure the satisfaction of, at the very least, minimum essential levels of each of the rights enunciated in the Covenant.”11 Two alternative arguments can be made for considering access to essential surgery within the right to health. First, several types of essential surgical care are located within the existing core obligations of State as laid out by the Committee on Economic, Social and Cultural Rights (CESCR) but have not yet become part of the discourse on the right to health. Second, because essential surgical care is a cost-effective means of preventing mortality and unnecessary morbidity, it should be addressed as an important strategy for achieving a state’s highest attainable standard of health.
Essential surgical care related to the treatment of obstetric emergencies, disease, and accidents should be considered within the existing core obligations of a state. The ICESCR identifies the minimum core obligations that a state must achieve, regardless of resource constraints.12 These core obligations include a woman’s right to maternal care, and specifically, emergency obstetric services.13 In addition, the ICESCR states that individuals have a right to the treatment of “epidemic, endemic, occupational and other diseases,” which is regarded as necessary for the full realization of an individual’s right to health.14 Because treatment for some diseases requires surgery, such surgical care falls within the core obligation of states. Furthermore, the ICESCR states that “[t]he right to treatment includes the creation of a system of urgent medical care in cases of accidents.”15 Therefore, surgeries necessary for emergency obstetric care, treatment of disease, and urgent care for accidents are all part of the recognized core obligations of states, and failure to comply with these obligations cannot be justified under any circumstance.
In the alternative argument, states are obliged to provide the highest attainable standard of health, and essential surgical care is an underutilized means of achieving this standard. Moreover, four essential elements must be satisfied in order for a state to fulfill the right to health: availability, accessibility, acceptability, and quality.16 As the ICESCR acknowledges, the highest attainable standard of health and the practical application of these four elements depend on the conditions of the state. Within the context of resource constraints, states must make decisions about how to use existing resources for the greatest benefit, and surgical care is viewed as competing with other types of treatment and prevention for limited resources. Traditionally, surgical care has been regarded as a highly expensive approach to reducing mortality and morbidity, particularly in comparison with preventive measures like immunization and sanitation. However, the World Health Organization (WHO) and the Bellagio group have begun to identify essential surgeries that significantly reduce the burden of disease at relatively low cost. Furthermore, in the context of human resources shortages, low-resource countries have demonstrated some success in training non-physician providers to perform selected types of surgical care. Thus, providing for the availability and accessibility of quality, essential surgical care in resource-constrained settings is more feasible than has been traditionally regarded. Based on the criteria of cost-effectiveness, certain types of surgery that can prevent significant morbidity and mortality at low cost should also be included within the framework of public health services necessary for the achievement of the highest attainable standard of health.
Global burden of surgical conditions and public health importance of surgery
The capacity of surgical interventions to reduce the global burden of disease has not been formally evaluated.17 Initial work focused on primarily hospital-based estimates of “surgical output” with comparisons to higher income countries; more recent models based on limited available data have provided initial estimates of global surgical output and disparities.18 In addition, the most recent estimate suggests that 11% of the “global burden of disease” (GBD) can be treated with surgery. This 11% total consists of injuries (38%), malignancies (19%), congenital anomalies (9%), complications of pregnancy (6%), cataracts (5%) and perinatal conditions (4%).19 While laudable, these estimates do not include key surgical conditions, such as surgical infections and acute abdominal emergencies, and the statistics are additionally limited by available data. They also do not include the potential impact that recent randomized controlled trials siggest circumcision may have on HIV.20 Burden of disease metrics have focused on quantifying conditions rather than interventions, such as surgery, population-level morbidity, and mortality. Several groups of researchers have attempted to support such efforts by further refining the basic definition of “surgical conditions” and “surgical interventions.”21
Specifically, future projections suggest a rapid rise in injuries, especially road traffic crashes and non-communicable diseases such as diabetes and neoplasms. A larger share of these conditions, many of which are amenable to surgery, will only increase the proportion of surgical conditions contributing to the burden of disease and magnify the importance of including surgery in the delivery of health care services.22
Recent data from WHO and the World Bank suggests that significant morbidity and mortality may be averted at low cost by the provision of surgery in many low-income and middle-income countries (LMICs) where access to and delivery of surgical care is limited or non-existent.23 Efforts within the global health and humanitarian communities are ongoing to more thoroughly evaluate the contribution of surgical conditions and the impact of surgical intervention on the burden of disease.24 Specific calls for improved data collection for injuries — for which data in low-income countries often must be integrated from various local sources, as well as calls for the integration of surgical conditions and services in prospective population-based surveys (such as the IN-DEPTH network) — will hopefully improve efforts to quantify “unmet need” for surgical care.25 In the meantime, the few estimates that are available are being analyzed and expanded to advocate for the support of surgical access, delivery, and evaluation in LMICs.26
Surgery has recently been referred to as the “neglected stepchild of global health” and as a “forgotten grand challenge of global public health.”27 The reasons for this perception and a lack of emphasis on access to surgical services in LMICs are the result of a shared responsibility between the public health and surgical communities. Historically, the public health commitment to population health has not included surgical care due to the primary (albeit incorrect) perception of excessive expense in a resource-constrained environment; moreover, its exclusion has been due to fear that support of surgical programs will shift resources away from more cost-effective population-based programs to less cost-effective individual-based interventions. For example, in Uganda, which has comparably higher levels of foreign assistance for global health, in a recent two-year period of 111 projects totaling over US$300 million, only two projects supported regional hospital services.28 The commitment of surgical providers to the individual patient has often reinforced these perceptions, especially in resource-rich settings where surgical intervention spans the continuum from caesarian sections to liver transplants, and where resource constraints are rarely discussed, both on the individual and population levels. Efforts to unite these communities and build consensus between disciplines have been entertained for more than a decade, but have only recently gained traction among both communities.29
There is little doubt that surgery has a role in public health based on burden of disease estimates, even if only emergency procedures for obstructed labor and trauma are considered. Existing data suggests that many surgical interventions would decrease burden at low cost.30 Recent efforts prioritize surgical interventions, and efforts by WHO provide guidelines for essential and emergency surgery, increasing surgical safety and evaluating surgical outcomes.31 Preliminary lists of the highest surgical priorities — mainly emergencies — that should be made available to all individuals, regardless of context or resources, have been put forth by WHO and other groups, such as the Bellagio Essential Surgery Group.32 Unfortunately, studies also suggest that the majority of health facilities in many low-income countries currently do not have the capacity to deliver even the most basic surgical services.33
Essential surgical interventions
Few argue the impact of access to emergency cesarean section on maternal health. Most experts and advocates agree that emergency surgical interventions, such as cesarean section, should be included as a global health priority; however, the debate on the inclusion of cost effective, essential surgical interventions has only recently been internationally acknowledged. Recent work on prioritizing surgical procedures, which provide the most benefit with the fewest resources, was undertaken by several independent groups.34 These efforts, combined with health indicators revealing continued high maternal mortality rates in most low-income countries, as well as the impact of trauma, suggest that specific surgical interventions — such as cesarean sections, surgical treatment for acute abdomen, and limb saving procedures from trauma — are essential to the health of all populations. Furthermore, basic low-cost context appropriate interventions, such as the training of lay first responders for injuries (US$0.12 per capita) and the provision of hospital-based trauma training, have been shown to have a significant impact at low-cost.35 For example, a district-based program to improve emergency obstetric care in Uganda cost only US$0.85/capita/year over five years.36 More recently, data suggesting that circumcision can prevent HIV transmission has prompted high HIV-incidence countries to consider infrastructure for surgical services more broadly.37
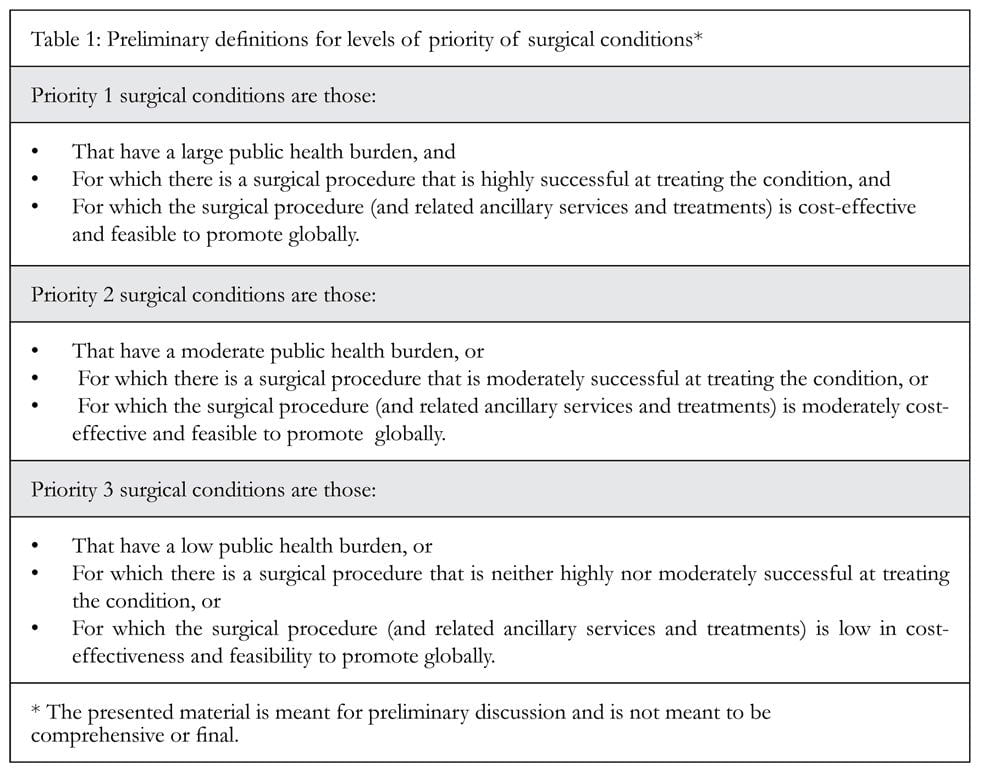
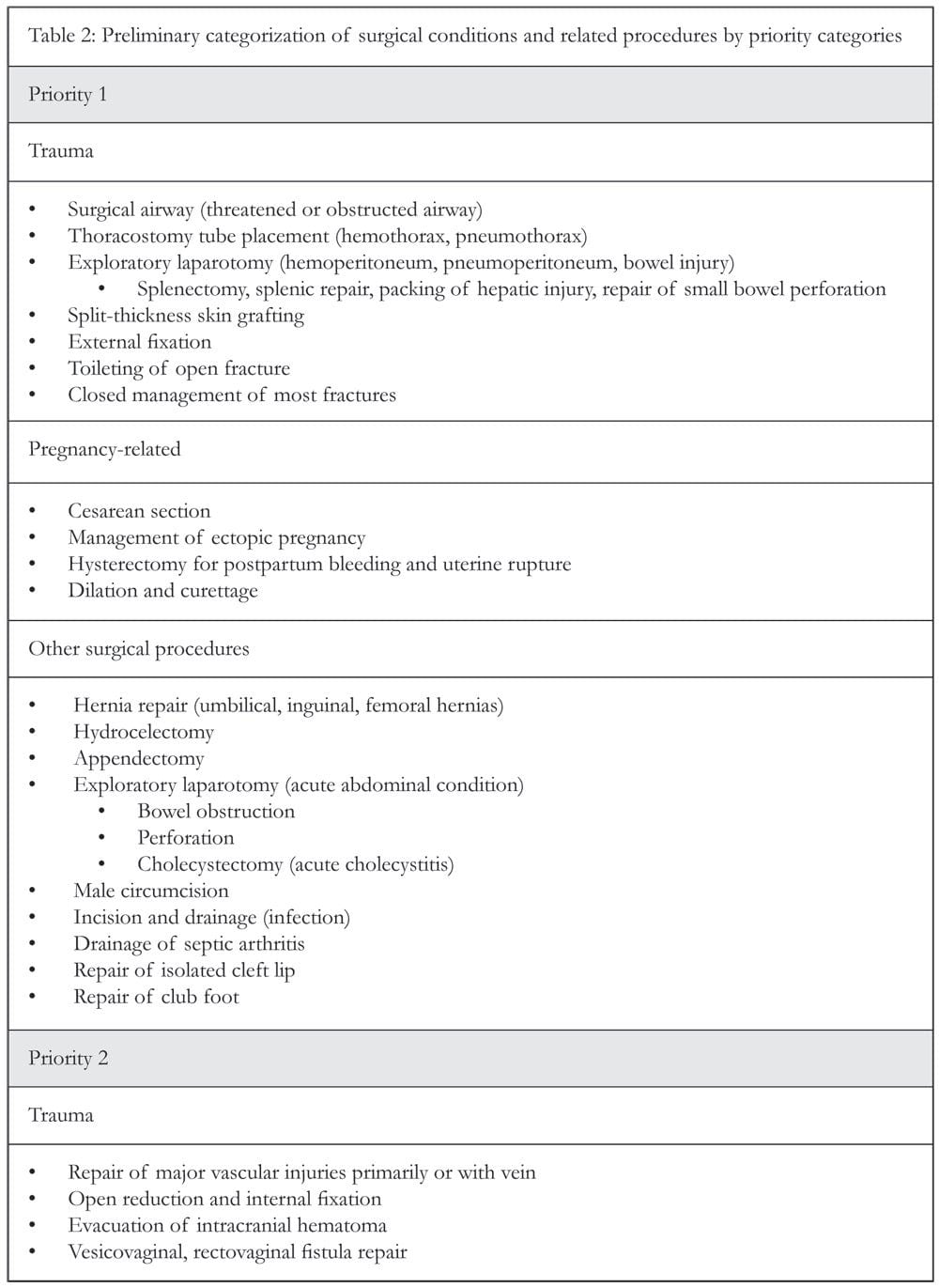
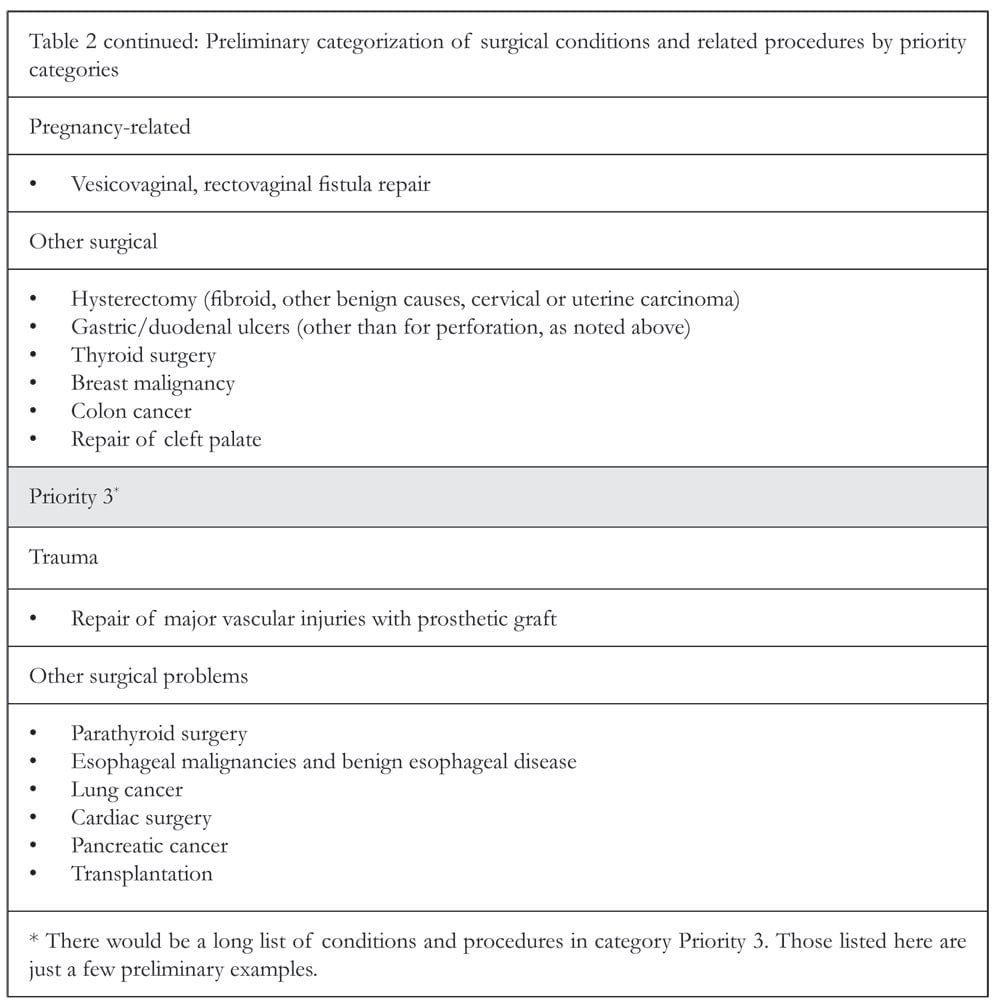
Thus, WHO and the Bellagio group, among others, have worked to better define the details of what accounts for essential surgery. However, while consensus has been reached on a majority of surgical interventions, a few outliers exist and have prevented publication of a definitive list. In the March 2010 World Journal of Surgery, Charles Mock et al. suggested a practical approach for prioritizing surgical interventions and proposed that surgical interventions be ranked Priority 1, 2 or 3 based on the burden of the specific disease, the success of the surgical intervention and the cost-effectiveness of the procedure to rank interventions (see Tables 1 and 2). Priority 1 conditions included emergencies and common surgical conditions with cost-effective interventions and significant impact of disability, such as hernia repair, male circumcision and club foot repair. Mock’s approach suggests that a list of essential surgery can be reached by application of a list of objective considerations, and that essential surgical interventions should be recognized and applied to global health much in the same way as essential medicines have been embraced.38 With this in mind, from an ethical standpoint, the right to emergency and essential surgical interventions must be considered as integral to health care, as essential medicines are to treatment of communicable diseases and HIV.
The right to surgery
ICESCR Comment 14, Article 12, calls for government obligations to provide prevention and treatment for diseases and also states that “health facilities, services, and goods must be available in sufficient quantity, accessible, (including affordable), culturally, acceptable … and of good quality.”39 Although rights-based language, which originated in the realm of civil and political rights, is now familiar in the context of economic and social rights, there has been little movement on the part of governments to enact laws and ensure the realization of this latter set of rights.
The UN Committee on Economic Social and Cultural Rights states that “availability” is one criteria by which to evaluate a right to health, which includes access to “functioning public health and health-care facilities, goods and services, as well as programs … in sufficient quantity.”40 While specific services are not listed in these definitions, public health institutions have generally interpreted this to mean that services that provide a large benefit to the population with low cost — such as vaccinations and tuberculosis treatment — should be made more widely available. Based on these utilitarian criteria, certain types of surgery that prevent significant morbidity and mortality at low cost should also be included within this framework of public health services.
Several examples exist in LMICs, suggesting that an ethical approach to the global surgical crisis is mandatory, and that considering essential and emergency surgery as a human right is a reasonable position. First, recent discussions on the Neglected Tropical Diseases (NTD) suggest that a large burden of disease, along with demonstrable strategies for success, should be considered as part of Millennium Development Goal 6, which refers to recognition of diseases beyond HIV, tuberculosis, and malaria. Second, the recent recognition of antiretroviral drugs as essential medicines has changed the approach to even this high cost intervention, which has in turn altered the HIV/AIDS pandemic.
The NTDs have been displaced within the global health agenda in a manner comparable to the lack of recognition of surgical diseases as an important contributor to premature death and disability. Ozdegiz and Riviello make a robust argument that compares NTDs with the provision of emergency and essential surgery.41 They suggest that recent attention to the NTDs are appropriate and provide substantive support for treating these diseases and addressing other cost-effective interventions, such as essential surgery.42
Once the role of antiretroviral therapy in treating the global HIV/AIDS pandemic was universally recognized as a human right, as were the barriers to access these medications, significant strides were made to improve access to antiretroviral drugs in LMICs and subsequently reduce mortality in the most impoverished and affected countries. However, implementation of the UN resolution on access to medication in the context of pandemics, such as HIV/AIDS, was met with difficulty, and strategies for beginning antiretroviral drugs in resource-limited settings have not only needed individual country considerations, but also ongoing revision.43
Similarly, barriers to providing surgical care that make it “impossible” to treat those in greatest need must also be considered. Based on the HIV/AIDS experience, many LMICs are clearly at a stage of development to offer essential surgical services if they were perceived as basic health care needs.
Economics of surgical services
Several studies at the level of district hospitals have supported the cost-effectiveness of basic surgical services, with estimates on a par with vaccination programs.44 Even studies that focused on trauma care alone showed similar cost-effectiveness.45 These results are particularly significant, as the perception of excessive cost of care is one of the primary reasons that surgery has not generally been included in discussions of essential health services.
In addition, many surgical services, particularly emergency care, fall outside of the “market” for health care, resulting in poor provision by the private sector. Such services meet criteria of “global public goods for health” based on their potential for social and sector-wide impact and should be funded as such.46 Specific accounts of effective provision of such services through public-private partnerships exist in the literature, and their usefulness in provision of surgical care could also be considered.47
These results may illustrate potential methods in addressing the market failure inherent in surgical care, especially in emergency situations. In addition, the recent call to improve health systems overall and focus on greater “horizontal” interventions across levels of the health system, rather than disease-specific interventions, provides momentum to synergize the resources required to advance surgical delivery with those needed for primary care.48
Conditions that require surgery also preferentially affect the young working population and impoverished patients and families through lost days of work and out-of-pocket health expenditures.49 While there have been few studies in this area beyond emergency obstetric care, the collective experience of the authors suggests that the economic impact of surgical conditions is profound. The inexpensive and technically simple surgical interventions most often provided that have an impact on disability and premature death include orthopedic interventions following motor vehicle and land mine trauma, cataract surgery, and surgery for congenital anomalies (for example, club feet and cleft lips and palates). Having an equally significant impact, but technically and logistically more complicated, are interventions for neoplasms that now plague low-income countries and lead to significant disability and premature death. These include cervical cancer, breast cancer, and many intra-abdominal neoplasms; while many neoplasms may be cured by surgery if diagnosed at an early stage, later diagnosis limits the possibility of surgical cure alone and often extends the surgical intervention and the likelihood of complications.50
One need only visit a typical rural (and sometimes, urban) hospital in a resource-limited setting to detect a few trends; these include high acuity patients who present at a relatively advanced level of disease; families living in the hospital to provide essential bedside care, advocate for their family members and face difficult daily decisions about the economic impact on their livelihoods; and on the other hand, local health providers often stretched thin and working with limited resources. In both short term specialty surgical missions in the provision of surgery in war and post-conflict zones and within long term academic partnerships dedicated to teaching providers to provide surgery and safe anesthesia, we have witnessed the preservation of human life and the restoration of hope. Large organizations, such as the International Committee for the Red Cross and Doctors Without Borders/Médecins Sans Frontières (MSF), provide a significant number of surgical procedures in LMICs. In the zones of war, post-conflict, and disaster where they serve, their mission is to predominately treat the war wounded. Their annual reports, however, reveal that in reality in these desperate settings they provide more non-conflict related procedures — including obstetrical care, caesarian sections, abdominal emergencies, and even repair of congenital anomalies such as cleft lip and palate, club feet, and removal of disfiguring tumors.51
While anecdotal reports of the successes of surgical intervention by international teams or short term missions are inspiring and contribute to the recognition of the abundance of unmet surgical need, these anecdotes are only the tip of the iceberg. As many epidemiologists are quick to point out, without outcome measures and follow up, little can be concluded accurately beyond the personal stories and photos of physically changed children. Therefore, more research is needed to identify specific indicators to study the effectiveness and impact of surgical interventions.52
Notwithstanding the favorable economics of essential surgical care, many patients in low-income countries suffer from eminently treatable conditions and have a right to appropriate treatment. In resource-constrained settings where these services are not currently provided, a human-rights based approach signifies a legal obligation to improving services along with establishing indicators to monitor progress.53
Global disparities in access to surgical care
Current global health disparities in surgical care are staggering. For example, a comparison between high and low-income countries suggests an estimated 1-2 million avertable injury deaths/year in severely injured patients alone and that 90% of those injury deaths occur in low-income countries.54 However, only a third of injured patients in rural low-income countries are able to obtain care.55 In many LMIC settings, there is a lack of functional prehospital and other emergency care systems to provide care.56 Meanwhile, 99% of maternal deaths, at least partially avertable through access to emergency obstetric care inclusive of caesarian section, occur in low-income countries.57 Nevertheless, interim evaluation suggests that the Millennium Development Goal to reduce maternal mortality is unlikely to be met.58 Additionally, estimates of surgical output, albeit with limited available data, show that only 3% of operations occur in poor and low-health-expenditure countries (defined as US$100 or less per capita spent on health per year) and that 75% of operations occur in higher-health-expenditure countries (more than US$400 per capita on health per year).59 In general, patients present at a much more advanced stage of disease in LMICs, limiting the potential for cure or even palliation of otherwise curable conditions.60
These disparities suggest a tremendous unmet need for surgical care in low-income countries. This may be largely due to the state of health systems, access barriers for the population, inadequate human resources for health, and poor functionality of health facilities. Recently, emphasis has been placed on the link between rights and the functions of health systems, although — with the exception of emergency obstetric care — the indicators used to evaluate health systems do not generally include the capacity to deliver surgical services.61 While surgical care overlaps with other “vertical” programs, such as maternal health, child health, infectious disease initiatives, cancer care, and injuries, there has been minimal effort to comprehensively integrate efforts to improve care in these areas.
Barriers in access to surgical care
Supply-side barriers
Access to surgical care is complicated by the number of variables that contribute to limited service provision, such as inadequate infrastructure and unsustained financial and human resources. Health facility evaluations in these settings often show deficiencies in the most essential infrastructure, equipment, and supplies to provide services.62 The lack of human resources often provides the greatest challenge, as the simple provision of funding and equipment will not begin to address the critical shortage of healthcare providers from nursing to surgery and anesthesia. The surgical workforce shortage in the lowest-income countries is profound, though the precise numbers are unknown. Africa may have less than 1% of the surgical workforce of the United States despite a significantly greater share of the burden of disease.63 The world’s anesthesia and nursing workforce shortage is even more extreme, severely compromising the safety and quality of perioperative care.64 This fact is reflected in basic data showing high perioperative morbidity and mortality rates in some resource-constrained settings.65
With a shortage of specialists, selected countries have depended on training non-physician providers in essential surgical care, such as caesarian sections, hernia repairs, basic surgical infections, wound and burn care, fracture and club foot management, and selected abdominal emergencies.66 Evidence suggests that this approach may provide effective quality care especially for rural district hospitals that disproportionately serve indigent populations.67 This limited workforce also often works with insufficient material and resources in adverse circumstances to care for patients, often at their own risk of occupational exposure to infectious diseases.68 However, the resilience and rights of these health workers are often not included in rights-based discussions.
Demand-side barriers
Access to care cannot be improved without also considering the many demand-side barriers, such as lack of information about the availability and efficacy of health care options; direct and indirect costs such as poverty, transportation, and opportunity expenses; as well as socio-cultural, gender and educational obstacles.69 The role of “iatrogenic poverty” has been well described in limiting access to health care.70 Poor referral systems, costs of transportation to higher level facilities, as well as the public perception of quality of care and the opportunity cost of seeking care contribute to disparities in care available to rural populations. Examples of social barriers abound in the maternal health literature where women are reluctant or limited by cultural norms to seek care outside the home.71 Of course, positive methods that alter these barriers and successful delivery of surgery have impacted the lives of many.
With these complex issues, it is unlikely that one approach will address all barriers or that one solution package will work in each LMIC. International organizations have spearheaded efforts to address the challenges outlined above through the development of guidelines and initiatives — for example, in trauma care, obstetric care, and essential surgery, and in selected surgical conditions such as obstetric fistula.72 Furthermore, to improve surgical care for vulnerable populations in low-income countries, many humanitarian international organizations, nongovernmental organizations, and faith-based organizations have provided surgical services for decades. These services have been provided in a wide range of settings — from conflict and disaster to a sustained presence in resource-constrained health systems. Some organizations have been more service-based, while others have worked to build greater local capacity. A recent survey of over 100 such organizations reveals that these organizations provide a significant volume of critical surgical interventions in many low-income countries, providing emergency and essential services as well as subspecialty procedures, which would otherwise be unavailable in most of the regions where these organizations provide care.73
Civil society organizations have used various approaches to meet the need for essential health services, and some have integrated a rights-based approach to their planning and evaluation. Much can be learned from the practical applications implemented by these organizations to meet the right to surgical care. The training of non-physicians in resource-constrained environments in surgical and anesthetic skills, as previously discussed, provides a possible model.74 In addition, academic and other organizations have documented their success stories in surgical training, even in these environments. It is important, however, to consider that many of these “success stories” have not been reported by groups faced with limited resources and a necessarily greater emphasison service provision over evaluation and dissemination.75
Conclusions
Essential and emergency surgery is not a luxury. Essential surgical interventions are increasingly important to public health and must be included in contemporary discussions on health and human rights. The large burden of disease with surgical interventions known to avert disability and death, along with cost effectiveness of the intervention, are evidence that some surgical procedures should be prioritized for delivery in all countries, and that the status of these specific procedures must be elevated from important to an essential element of the right to health. The current disparities in global surgical care are unacceptable. This is supported by available facility and population-based data, and also, by the authors’ personal experiences of the ground-reality in resource-constrained settings. Unequivocally, rights-based discussions must inform concrete short- and long-term plans to improve access to surgical care in these environments. As a starting point, this includes critical appraisal and action in areas of the world’s surgical workforce, integration of surgical services in ongoing health policy initiatives, and agreement on indicators that can be used to measure progress.
Health personnel involved in delivery of surgical services have much to learn from the practical applications of human rights principles and the essential role they must fulfill in research and advocacy to improve availability for surgical care globally.76 Similar to other medical interventions once thought to be too expensive or complicated to deliver, support and success of surgical programs rely upon the commitment of the global health community. Further, the basic right to health care demands the delivery of essential surgical services; its demonstrated cost effectiveness argues that delivery is feasible; and the benefit to entire health systems from building surgical infrastructure makes neglecting these needs unacceptable. Ultimately, investing in surgical services would benefit all sectors.
K. A. Kelly McQueen, MD, MPH, is a Fellow at the Harvard Humanitarian Initiative in Boston, Massachusetts and a partner at Valley Anesthesiologist Consultants, Phoenix, Arizona.
Doruk Ozgediz, MD, MSc, is a Fellow in Pediatric Surgery at the Hospital for Sick Children at the University of Toronto, Canada.
Robert Riviello, MD, MPH, is a Fellow in Acute Care and Burn Surgery at Brigham and Women’s Hospital in Boston.
Renee Hsia, MD, MSc, is Clinical Instructor in Emergency Medicine in the Department of Emergency Medicine at the University of California, San Francisco.
Sudha Jayaraman, MD, MSc, is a Resident Physician in the Department of Surgery and a Fellow in Global Health Sciences at the University of California, San Francisco.
Stephen R. Sullivan, MD, MPH, is a plastic surgeon in Craniofacial Surgery at Children’s Hospital Boston.
John G. Meara, MD, DMD, MBA, is Plastic Surgeon-in-Chief at Children’s Hospital Boston.
Please address correspondence to the authors c/o Dr. K. A. McQueen, 4134 North 49th Place, Phoenix, AZ 85018, email: kamcqueen@gmail.com.
References
1. D. M. Kent, D. M. Mwamburi, M. L. Bennish et al., “Clinical trials in sub-Saharan Africa and established standards of care: A systematic review of HIV, tuberculosis, and malaria trials [comment],” Journal of the American Medical Association 292/2 (2004), pp. 237–242.
2. G. Backman, P. Hunt, R. Khosla et al., “Health systems and the right to health: An assessment of 194 countries,” Lancet 372/9655 (2008), pp. 2047–2085; S. Gruskin, E. J. Mills, and D. Tarantola, “History, principles, and practice of health and human rights,” Lancet 370/9585 (2007), p. 449–455.
3. The World Health Organization and Office of the United Nations Commissioner for Human Rights, The right to health, Fact Sheet No. 31 (July 1, 2008). Available at http://www.ohchr.org/Documents/Publications/Factsheet31.pdf; J. M. Mann, “Health and human rights.” British Medical Journal 312/7036 (1996), pp. 924–925; N. Pillay, “Right to health and the Universal Declaration of Human Rights,” Lancet 372/9655 (2008), pp. 2005–2006; S. R. Benatar, “Global disparities in health and human rights: a critical commentary,” American Journal of Public Health 88/2 (1998), pp. 295–300.
4. A. Sen, “Why and how is health a human right?” Lancet 372/9655 (2008), p. 2010; Ibid., “The right to health: From rhetoric to reality,” p. 2001.
5. J. D. Sachs, Macroeconomics and health: Investing in health for economic development. The report of the Commission on Macroeconomics and Health (Geneva, Switzerland: World Health Organization, 2001); H. Varmus, R. Klausner, E. Zerhouni et al., “Public health: Grand challenges in global health,” Science 302/5644 (2003), pp. 398–399; A. S. Daar, P. A. Singer, D. L. Persad et al., “Grand challenges in chronic non-communicable diseases,” Nature 450/7169 (2007), p. 494–496.
6. H. T. Debas, R. Gosselin, C. McCord et al., “Surgery,” in D. T. Jamison, J. G. Breman, A. R. Measham et al. (eds), Disease control priorities in developing countries (New York: Oxford University Press, 2006), pp. 1245–1260.
7. “A crucial role for surgery in reaching the UN Millennium Development Goals” [Editorial], PLoS Medicine 5/8 (2008), pp. 1165–1167.
8. R. J. Cook, B. M. Dickens, and S. Syed, “Obstetric fistula: The challenge to human rights,” International Journal of Gynaecology Obstetrics 87/1 (2004), pp. 72–77; R. J. Cook and M.B. Galli Bevilacqua, “Invoking human rights to reduce maternal deaths,” 363/9402 Lancet (2004), p. 73; S. Gruskin, J. Cottingham, A. M. Hilber et al., “Using human rights to improve maternal and neonatal health: History, connections and a proposed practical approach.” Bulletin of the World Health Organization 86/8 (2008), pp. 589–593.
9. International Covenant on Economic, Social and Cultural Rights (ICESCR), G.A. Res. 2200A (XXI), Art. 12.1. (1966). Available at http://www2.ohchr.org/english/law/cescr.htm. Available at http://www2.ohchr.org/english/law/cescr.htm.
10. Ibid., General Comment No. 14, para. 9
11. Ibid., para. 43.
12. Ibid., para 47: “It should be stressed, however, that a State party cannot, under any circumstances whatsoever, justify its non-compliance with the core obligations set out in paragraph 43 above, which are non-derogable.”
13. Ibid., Art. 12.2a. See also, Comment 14, para 14.
14. Ibid., Art. 12.2c.
15. Ibid., General Comment 14, para. 16.
16. B. Taira, K. McQueen, and F. Burkle, “Burden of surgical disease: Does the literature reflect the scope of the international crisis?” World Journal of Surgery 33/5 (2009), pp. 893–898.
17. S. Holmberg and E. Nordberg, “Surgical rates in Africa: Variations and their possible explanations.” Tropical and Geographical Medicine 42/4 (1990), pp. 352–358; T. G. Weiser, S. E. Regenbogen, K. D. Thompson et al., “An estimation of the global volume of surgery: A modelling strategy based on available data,” Lancet 372/9633 (2008), p. 139–144.
18. T. Vos, “Improving the quantitative basis of the surgical burden in low-income countries,” PLoS Medicine 6/9 (2009), p. e1000149.
19. Debas (see note 6).
20. Vos (see note 18); S. Bickler, D. Ozgedis, R. Gosselin et al., “Key concepts for estimating the burden of surgical conditions and the unmet need for surgical care,” World Journal Surgery 34/3 (2009), pp. 374–380.
21. Daar et al. (see note 5); K. Hofman, A. Primack, G. Keusch et al., “Addressing the growing burden of trauma and injury in low- and middle-income countries,” American Journal of Public Health 95/1 (2005), pp. 13–17.
22. Debas et al. (see note 6).
23. S. W. Bickler and D. A. Spiegel, “Global surgery — Defining a research agenda,” Lancet 372/9633 (2008), pp. 90–92.
24. K. Bhalla, J. Harrison, J. Abraham et al., “Data sources for improving estimates of the global burden of injuries: Call for contributors,” PLoS Medicine 6/1 (2009); C. J. Murray and J. Frenk, “Health metrics and evaluation: Strengthening the science,” Lancet 371/9619 (2008), pp. 1191–1199.
25. D. Ozgediz, R. Hsia, T. Weiser et al., “Population health metrics for surgery: Effective coverage of surgical services in low-income and middle-income countries,” World Journal of Surgery 33/1 (2009), pp. 1–5; Global Burden of Surgical Disease Working Group, “Conference on increasing access to surgical services in resource-constrained settings in sub-Saharan Africa” (2007). Available at http://globalhealthsciences.ucsf.edu/bellagio/docs/bellagio_report.pdf; T. G. Weiser, M. A. Makary, A. B. Haynes et al., “Standardised metrics for global surgical surveillance.” Lancet 374/9695 (2009), pp. 1113–1117.
26. D. Ozgediz, D. Jamison, M. Cherian, and K. McQueen, “The burden of surgical conditions and access to surgical care in low- and middle-income countries,” Bulletin of the World Health Organization 86/8 (2008), pp. 646–647; P. E. Farmer and J. Y. Kim, “Surgery and global health: A view from beyond the OR,” World Journal of Surgery 32/4 (2008), pp. 533–536.
27. D. Angemi, J. Oyugi, I. Aziz et al., “The money flows, the boy dies,” International Herald Tribune (April 25, 2007).
28. Disease Control Priorities Project, “Promoting essential surgery in low-income countries: A hidden cost-effective treasure” (2008). Available at http://www.dcp2.org/file/155/dcpp-referralhospitals.pdf; The World Health Organization, “Surgical care at the district hospital” (2003). Available at http://www.who.int/surgery; D. Ozgediz, P. Dunbar, C. Mock et al., “Bridging the gap between public health and surgery: Access to surgical care in low- and middle-income countries,” Bulletin of the American College of Surgeons 94/5 (2009), pp. 14–20.
29. R. A. Gosselin and M. Heitto, “Cost-effectiveness of a district trauma hospital in Battambang, Cambodia,” World Journal of Surgery 32/11 (2008), pp. 2450–2453.
30. C. Mock, M. Cherian, C. Juillard, et al, “Developing priorities for addressing surgical conditions globally: Furthering the link between surgery and public health policy,” World Journal of Surgery 34/3 (2010), pp. 381–385.
31. Debas et al. (see note 6); S. Ansart, L. Perez, O. Vergely et al., “Illnesses in travelers returning from the tropics: A prospective study of 622 patients,” Journal of Travel Medicine 12/6 (2005), pp. 312–318; A. B. Haynes, T. G. Weiser, W. R. Berry et al., “A surgical safety checklist to reduce morbidity and mortality in a global population,” New England Journal of Medicine 360/5 (2009), pp. 491–499.
32. Global Burden of Surgical Disease Working Group (see note 25); Ansar et al. (see note 30); G. Benagiano and B. Thomas, “Safe motherhood: The FIGO initiative,” International Journal of Gynaecology and Obstetrics 82/3 (2003), p. 263–274; C. Mock, J. D. Lormand, J. Goosen et al., Guidelines for essential trauma care (Geneva, Switzerland: World Health Organization, 2004); Mock et al. (see note 30); S. Luboga, S. B. Macfarlane, J. von Schreeb et al., “Increasing access to surgical services in sub-Saharan Africa: Priorities for national and international agencies recommended by the Bellagio Essential Surgery Group,” PLoS Medicine 6/12 (2009), p. e1000200.
33. C. Mock, S. Nguyen, R. Quansah et al., “Evaluation of trauma care capabilities in four countries using the WHO-IATSIC guidelines for essential trauma care,” World Journal of Surgery 30/6 (2006), pp. 946–956; L. Pearson and R. Shoo, “Availability and use of emergency obstetric services: Kenya, Rwanda, Sudan, and Uganda,” International Journal of Gynegology and Obstetrics 88/2 (2005), pp. 208–215; S. C. Hodges, C. Mijumbi, M. Okello et al., “Anesthesia services in developing countries: Defining the problems,” Anesthesia 62 (2007), pp. 4–11; T. P. Kingham, T. B. Kamara, N. M. Cherian et al., “Quantifying surgical capacity in Sierra Leone: A guide for improving surgical care,” Archives of Surgery 144/2 (2009), pp. 122–128.
34. Mock et al. (see note 30); J. Cohen, “Asia and Africa: On different trajectories?” Science 304/5679 (2004), pp. 1932–1938.
35. S. Jayaraman, J. R. Mabweiiano, M. S. Lipinick et al., “First things first: Effectiveness and scalability of a basic prehospital trauma care program for lay first-responders in Kampala, Uganda.” PLoS ONE 4/9 (2009), p. e6955; H. Husum, M. Gilbert, T. Wisborg et al., “Rural prehospital trauma systems improve trauma outcome in low-income countries: A prospective study from North Iraq and Cambodia,” The Journal of Trauma 54/6 (2003), pp. 1188–1196; M. A. Tiska, M. A. Adu-Ampofo, G. Boakye et al., “A model of prehospital trauma training for lay persons devised in Africa,” Emergency Medicine Journal 21/2 (2004), pp. 237–239; J. Ali, R. Adam, A. K. Butler et al., “Trauma outcome improves following the advanced trauma life support program in a developing country,” The Journal of Trauma 34/6 (1993), pp. 890–899.
36. A. B. Lalonde, P. Okong, A. Mugasa et al., “The FIGO save the mothers initiative: The Uganda–Canada collaboration,” International Journal of Gynaecology and Obstetetrics 80/2 (2003), pp. 204–212.
37. B. G. Williams, J. O. Lloyd-Smith, E. Gouws et al., “The potential impact of male circumcision on HIV in sub-Saharan Africa,” PLoS Medicine 3/7 (2007), pp. 1032–1040; S. Pincock, “Workforce biggest barrier to roll-out of male circumcision,” Lancet 370 (2007), pp. 1817–1818.
38. Mock et al. (see note 30); for the categorization of essential medicines in global health, see The World Health Organization, “WHO essential medicines” (2010). Available at http://www.who.int/topics/essential_medicines/en.
39. Backman et al. (see note 2).
40. H. Nygren-Krug, “Integrating human rights in health: Human rights in the context of public health,” Bulletin of Medicus Mundi Switzerland 96 (2005), pp. 6–11.
41. D. Ozgediz and R. Riviello, “The ‘other’ neglected diseases in global public health: Surgical conditions in sub-Saharan Africa,” PLoS Medicine 5/6 (2008), p. e121.
42. J. O. Gyapong, M. Gyapong, N. Yellu et al., “Integration of control of neglected tropical diseases into health-care systems: Challenges and opportunities,” Lancet 375/9709, pp. 160–165.
43. N. Ford, A. Calmy, and S. Hurst, “When to start antiretroviral therapy in resource-limited settings: A human rights analysis,” BioMed Central International Health and Human Rights 10/6 (2010), p. 6.
44. R. Laxminarayan, A. J. Mills, J. G. Breman et al., “Advancement of global health: Key messages from the Disease Control Priorities Project,” Lancet 367/9517 (2006), pp. 1193–1208; C. McCord and Q. Chowdhury, “A cost effective small hospital in Bangladesh: What it can mean for emergency obstetric care,” International Journal Gynaecology and Obstetetrics 81/1 (2003), pp. 83–92.
45. R. A. Gosselin and M. Heitto, “Cost-effectiveness of a district trauma hospital in Battambang, Cambodia,” World Journal of Surgery 32/11 (2008), pp. 2450–2453.
46. R. D. Smith and L. Mackellar, “Global public goods and the global health agenda: Problems, priorities and potential,” Global Health 3/9 (2007), p. 9.
47. L. C. Ivers, E. S. Garfein, J. Augustin et al., “Increasing access to surgical services for the poor in rural Haiti: Surgery as a public good for public health,” World Journal of Surgery 32/4 (2008), pp. 537–542; K. Hanson, L. Gilson, C. Goodman et al., “Is private health care the answer to the health problems of the world’s poor?” PLoS Medicine 5/11 (2008), p. e233.
48. V. Oliveira-Cruz, C. Kurowski, and A. Mills, “Delivery of priority health services: Searching for synergies within the vertical versus horizontal debate,” Journal of International Development 15/1 (2003), pp. 67–86; M. R. Reich, K. Takemi, M. J. Roberts et al., “Global action on health systems: A proposal for the Tokyo G8 summit,” Lancet 371/9615 (2008), pp. 865–869; D. Yu, Y. Souteyrand, M. A. Banda et al., “Investment in HIV/AIDS programs: Does it help strengthen health systems in developing countries?” Global Health 4/1 (2008), p. 8.
49. C. N. Mock, E. Boland, F. Acheampong et al., “Long-term injury related disability in Ghana,” Disability and Rehabilitation 25/13 (2003), pp. 732–741; B. Meessen, Z. Zhenzhong, W. Van Damme et al., “Iatrogenic poverty,” Tropical Medicine and International Health 8/7 (2003), pp. 581–584.
50. B. O. Anderson and R. Jakesz, “Breast cancer issues in developing countries: An overview of the Breast Health Global Initiative,” World Journal of Surgery 32/12 (2008), pp. 2578–2585.
51. International Committee of the Red Cross, Annual Report 2007. Available at http://www.icrc.org/Web/Eng/siteeng0.nsf/htmlall/section_annual_report_2007?OpenDocument; M. Alary and C. M. Lowndes, “The central role of clients of female sex workers in the dynamics of heterosexual HIV transmission in sub-Saharan Africa,”AIDS 18/6 (2004), pp. 945–947; T. Ensor and S. Cooper, “Overcoming barriers to health service access: Influencing the demand side,” Health Policy Plan 19/2 (2004), pp. 69–79; M. Ranson, K. Hanson, V. Oliveira-Cruz et al., “Constraints to expanding access to health interventions: An empirical analysis and country typology,” Journal of International Development 15/1 (2003), pp. 15–39.
52. K. A. McQueen, J. A. Hyder, B. R. Taira et al., “The provision of surgical care by international organizations in developing countries: A preliminary report,” World Journal of Surgery 34/3 (2009), pp. 397–402; J. Maki, M. Qualls, B. White et al., “Health impact assessment and short-term medical missions: A methods study to evaluate quality of care,” BioMed Central Health Services Research 8 (2008), p. 121.
53. Backman et al. (see note 39).
54. C. N. Mock, G. J. Jurkovich, D. nii-Amon-Kotei et al., “Trauma mortality patterns in three nations at different economic levels: Implications for global trauma system development,” The Journal of Trauma 44/5 (1998), pp. 804–814.
55. C. N. Mock, D. nii-Amon-Kotei, and R.V. Maier, “Low utilization of formal medical services by injured persons in a developing nation: Health service data underestimate the importance of trauma,” The Journal of Trauma 32/3 (1997), pp. 504–513.
56. Mock et al. (see note 30).
57. C. Ronsmans and W. J. Graham, “Maternal mortality: Who, when, where, and why,” Lancet 368/9542 (2006), pp. 1189–1200.
58. Ronsmans et al. (see note 57).
59. T. G. Weiser, S. E. Regenbogen, K. D. Thompson et al., “An estimation of the global volume of surgery: A modelling strategy based on available data,” Lancet 372/9633 (2008), pp. 139–144.
60. A. Gakwaya, J. B. Kigula-Mugambe, A. Kavuma et al., “Cancer of the breast: 5-year survival in a tertiary hospital in Uganda,” British Journal of Cancer 99/1 (2008), pp. 63–67.
61. Backman et al. (see note 39).
62. Hodges et al. (see note 33); Mock et al. (see note 33).
63. A. E. Wasunna, “Surgical manpower in Africa,” Bulletin of the American College of Surgeons 72/6 (1987), pp. 18–19.
64. I. A. Walker and I. H. Wilson, “Anaesthesia in developing countries — a risk for patients,” Lancet 371/ 9617 (2008), pp. 968–969; G. Dubowitz, S. Detlefs, and K. A. McQueen, “Global anesthesia workforce crisis: A preliminary survey revealing shortages contributing to undesirable outcomes and unsafe practices,” World Journal of Surgery 34/3 (2009), pp. 439–444.
65. I. A. Walker and N. S. Morton, “Pediatric healthcare — the role for anesthesia and critical care services in the developing world,” Paediatric Anaesthesia 19/1 (2009), pp. 1–4; P. M. Fenton, C. J. Whitty, and F. Reynolds, “Caesarean section in Malawi: Prospective study of early maternal and perinatal mortality,” The British Medical Journal 327/7415 (2003), p. 587; A. F. Ouro-Bang’na Maman, K. Tomta, S. Ahouangbevi et al., “Deaths associated with anaesthesia in Togo, West Africa,” Tropical Doctor 35/4 (2005), pp. 220–222.
66. M. E. Kruk, C. Pereira, F. Vaz et al., “Economic evaluation of surgically trained assistant medical officers in performing major obstetric surgery in Mozambique,” BJOG:An International Journal of Obstetrics and Gynaecology 114/10 (2007), pp. 1253–1260; S. Bergstrom, “Who will do the caesareans when there is no doctor? Finding creative solutions to the human resource crisis,” BJOG: An International Journal of Obstetrics and Gynaecology 112/9 (2005), pp. 1168–1169; A. Loutfi, A. P. McLean, and J. Pickering, “Training general practitioners in surgical and obstetrical emergencies in Ethiopia,” Tropical Doctor 25 Suppl 1 (1995), pp. 22–26; S. Contini and R. A. Gosselin, “Rural surgery in southern Sudan,” World Journal of Surgery 31/3 (2007), pp. 613–614; A. J. Tindall, A. Gul, S. Sambandam et al., “Results of manipulation of idiopathic clubfoot deformity in Malawi by orthopaedic clinical officers using the Ponseti method: A realistic alternative for the developing world?” Journal of Pediatric Orthopaedics 25/5 (2005), pp. 627–629; N. Semer, Practical plastic surgery for nonsurgeons (New York/ Lincoln/ Shanghai: Authors Choice Press, 2007); A. O. Longombe, “Surgical training of nurses for rural areas: necessity or aberration?” East and Central African Journal of Surgery 3/1 (1997), pp. 43–47.
67. Kruk et al. (see note 66); K. Chu, P. Rosseel, P. Gielis, and N. Ford, “Surgical task shifting in sub-Saharan Africa,” PLoS Medicine 6/5 (2009), p. e1000078.
68. J. Jagger, A. E. Gomaa, and E. K. Phillips, “Safety of surgical personnel: A global concern,” Lancet 372/9644 (2008), p. 1149.
69. Sachs (see note 5); T. Ensor and S. Cooper, “Overcoming barriers to health service access: Influencing the demand side,” Health Policy Plan 19/2 (2004), p. 69–79; M. Ranson, K. Hanson, V. Oliveira-Cruz et al., “Constraints to expanding access to health interventions: An empirical analysis and country typology,” Journal of International Development 15/1 (2003), pp. 15–39; A. Onuminya, “The role of the traditional bone-setter in primary fracture care in Nigeria,” South African Medical Journal 94/8 (2004), pp. 652–658.
70. B. Meessen, Z. Zhenzhong, W. Van Damme et al., “Iatrogenic poverty,” Tropical Medicine and International Health 8/7 (2003), p. 581–584.
71. S. Thaddeus and D. Maine, “Too far to walk: Maternal mortality in context,” Social Science and Medicine 38/8 (1994), pp. 1091–1110.
72. Ansart et al. (see note 31); Benagiano et al. (see note 32); M. Muleta, “Obstetric fistula in developing countries: A review article,” Journal of Obstetrics and Gynaecology Canada 28/11 (2006), pp. 962–966.
73. K. A. K. McQueen, J. A. Hyder, B. R. Taira, et al. “The provision of surgical care by international organizations in developing countries: A preliminary report,” World Journal of Surgery 34 (2010), pp. 397–402.
74. Chu et al. (see note 67); R. Jacob, “Pro: Anesthesia for children in the developing world should be delivered by medical anesthetists,” Paediatric Anaesthesia 19/1 (2009), pp. 35–38.
75. Contini et al. (see note 66); N. Sohier, L. Frejacques, and R. Gagnayre, “Design and implementation of a training programme for general practitioners in emergency surgery and obstetrics in precarious situations in Ethiopia,” Annals of the Royal College of Surgeons of England 81/6 (199), pp. 367–375.
76. J. M. Mann, “Medicine and public health, ethics and human rights,” The Hastings Center Report 27/3 (1997), pp. 6–13.