Editorial: Intersections of health and human rights
Health and Human Rights 13/1
Published June 2011
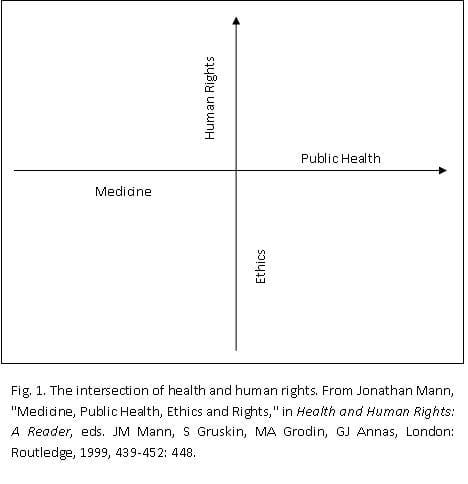
Shortly before his death, Jonathan Mann, the founding editor of this journal, imagined its major fields of inquiry as two perpendicular axes describing different dimensions of human well-being. The horizontal axis ranged from medicine, with its focus on individual suffering and intervention, to public health, with its focus on populations. The vertical axis began with ethics, concerned with treatment and behavior of individuals, and ended with human rights, “a historic effort to identify and agree upon what governments should not do to people and what they should assure to all.”
In an age when discussions of global or national health policy too often devolve into feckless technocratic sidebars or the crass rhetoric of horse-race politics, Dr. Mann’s vision gives us a sense of agency—and urgency. The “p values of biostatistics,” he insisted, are no substitute for values themselves. Just as any narrow epidemiology that identifies ‘risk behaviors’ of individuals in isolation from their social context threatens to distort our knowledge, understanding, and the collective decisions we make on their basis, so too the impulse to imprison health in a biomedical straitjacket does violence to its potential as a nexus of moral, and therefore political, action. There are two dimensions of well-being, and only one is statistical or physical. To Dr. Mann, the human rights framework offered “coherence and clarity required for public health to identify and work with conscious attention to its roles and responsibilities. At that point, an ethics of public health … can emerge.”
This issue of HHR addresses settings of natural disaster where the nation-states that structure both public health and human rights have been shaken. On the axis of means and ends, it inhabits the lower left-hand quadrant; in post-disaster settings, individuals are easier to locate and engage with than groups, making pursuit of human rights and public health a symmetrical challenge.
In some cases, the challenge is met. Arbour and colleagues describe a rights-based policy framework that offered considerable advantages to Chilean authorities recovering from the 2010 earthquake as they attempted to protect highly vulnerable children. Klasing and Satterthwaite, by contrast, present survey data illustrating the challenges of implementing rights-based approaches in settings like Haiti, where the weak central state was unable to enforce conceptual, strategic, and regulatory consistency.
The intersection between health and human rights occurs in three configurations: (1) where protection of rights leads to promotion and protection of health; (2) where public health policies, programs, and practices are a burden on human rights; and (3) where human rights violations implicate health. The remaining three articles in this issue touch on the last of these configurations. Baldwin and colleagues report on victims of forced labor and sex trafficking in Los Angeles, using qualitative research methods to characterize the interactions of trafficked women with health providers. They find that health professionals often encounter human trafficking victims without knowing they have done so; by increasing awareness and providing more opportunities for disclosure, we can therefore make it much easier to identify victims. Davis and Bookey describe the toll of sexual violence in post-earthquake Haiti, a country long ruled by dictatorships and juntas that used rape systematically as a method of control. After the January 2010 quake, the historical legacy of state-sponsored human rights abuses was a sharp increase in rapes due to weakness in policing and other official institutions. The authors tie sexual violence against women in present-day Haiti to the failure to include women in the planning process. Finally, the review by Malik assesses the relationship between violations of foundational civil liberties and of the human right to health in Pakistan after the catastrophic floods of 2010. Embodying Dr. Mann’s call to better understand “the impacts of violations of dignity on physical, mental and social well-being,” Malik shows how broadly discriminatory legislation against the Ahmadiyya sect of Islam created an environment where international flood relief could be denied with impunity to many Ahmadi families despite a nominal state commitment to equal access. Without specific attention to the broad sweep of human rights legislation in post-disaster settings, humanitarian agencies can unwittingly ratify entrenched discrimination with serious implications for the health of vulnerable populations.
For the last several volumes, Health and Human Rights has pursued intersections between its two main fields of inquiry and key themes in health and medicine. Like the focus on natural disasters in the present issue, these cross-cutting research streams feed a model of human well-being that is defined in dynamic, multidimensional, real-world terms and not by reference to bureaucratic or disciplinary categories. Beginning in issue 13(2), we will pursue the intersections of health and rights with a rolling set of topics chosen for their centrality to well-being as understood by individuals, states, and other contemporary institutions. HHR invites articles that explore these thematic linkages between values and realities of healing.
Aaron Shakow, Editor